Review Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Assessment Genetic Mutations in gene TYMP in indicate Mitochondrial Neuro-Gastro-Intestinal Encephalopathy Syndrome
*Corresponding author: Shahin Asadi, Department of Medical Genetics, Harvard University of Medical Sciences, Massachusetts, USA.
Received: January 17, 2019; Published: January 22, 2019
DOI: 10.34297/AJBSR.2019.01.000510
Abstract
MNGIE syndrome is a genetic disorder that affects several parts of the body, in particular the digestive system and the nervous system. Almost all people with MNGIE syndrome have gastrointestinal disorder in which gastrointestinal muscles and nerves do not move food efficiently. MNGIE syndrome is caused by the mutation of the TYMP gene, which is based on the long arm of chromosome 22, based on 22q13.33.
Keywords: MNGIE Syndrome; TYMP Gene; Mitochondrial Disorder; Encephalopathy
Generalizations of MNGIE syndrome
MNGIE syndrome is a genetic disorder that affects several parts of the body, in particular the digestive system and the nervous system. Major features of the MNGIE disease can be created at any time from birth to adulthood, but symptoms and symptoms often start at the age of 20. The medical problems associated with this disorder become worse with time [1].
Clinical Signs of MNGIE Syndrome
Gastrointestinal disorders are one of the most common and severe symptoms of MNGIE. Almost all people with MNGIE syndrome have gastrointestinal disorder in which gastrointestinal muscles and nerves do not move food efficiently. Digestive problems in the syndrome include feeling sick after eating only with small amounts, difficulty swallowing (dysphagia), postnatal nausea and vomiting, abdominal pain, diarrhoea, and bowel obstruction. These problems in the gastrointestinal tract lead to severe cramping and cachexia [1].
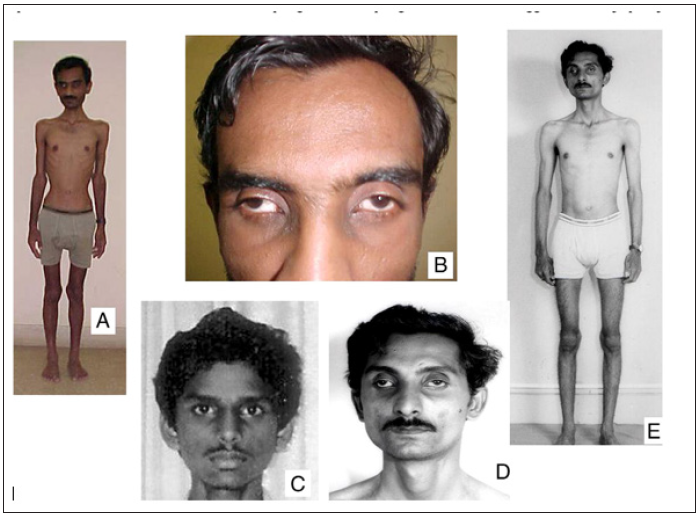
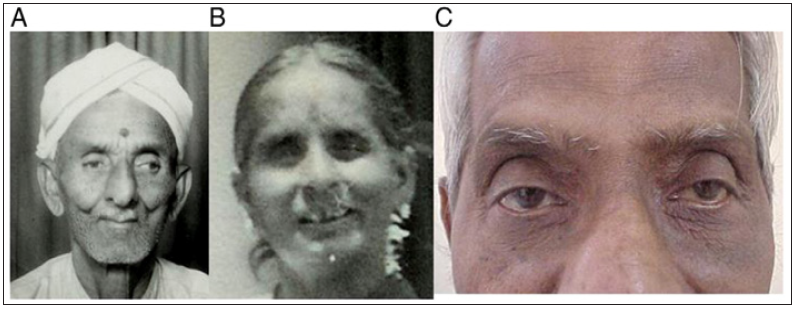
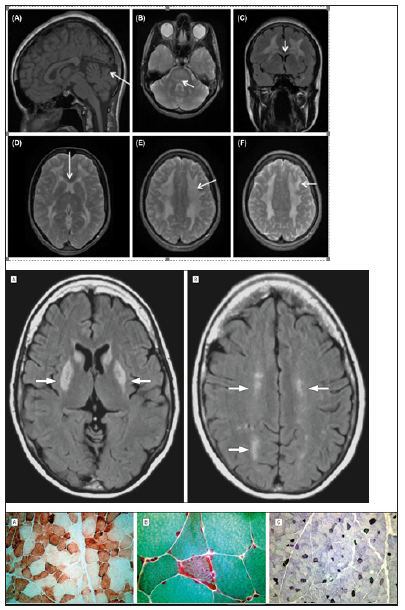
MNGIE disease is also characterized by disorders of the nervous system, although these tend to be less likely than gastrointestinal problems. Affected people have a tingling sensation in the skin, numbness and weakness in their limbs (peripheral neuropathy), especially in the hands and feet. Additional nerve symptoms include drooping eyelids (ptosis), muscle weakness that controls eye movements (optomoplegia), and hearing loss. Leukoencephalopathy, which is the breakdown of white matter from the fat in the brain tissue called myelin, is also a symptom of MNGIE disease. These changes in the brain can be seen with magnetic resonance imaging (MRI), although they usually do not cause symptoms in people with this disorder [2] (Figure 1).
Etiology of MNGIE Syndrome
MNGIE syndrome is caused by the mutation of the TYMP gene, which is based on the long arm of chromosome 22, based on 22q13.33. The gene provides instructions for the synthesis of enzymes called thymidine phosphorylase. Thymidine is a molecule known as a nucleoside, which (after biochemical modification) is used as a building block of DNA. The thymidine phosphorylase enzyme decomposes thymidine into smaller molecules, which helps regulate the amount of nucleosides in the cells [3].
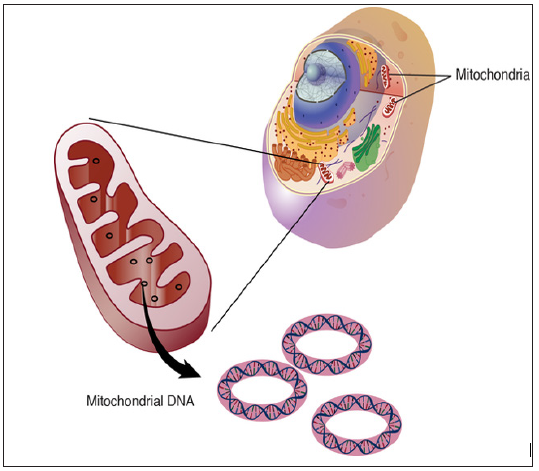
TYMP gene mutations severely reduce the activity or production of thymidine phosphorylase. The deficiency of this enzyme allows timed in to be produced at a very high level in the body. Researchers believe that excessive increase in this molecule can also damage mitochondrial DNA or mtDNA. Mitochondria are cellular structures that convert energy from food to other forms that cells can use (ATP). Although the highest amount of DNA is packaged in the chromosomes inside the nucleus, the mitochondria also have a small amount of their own DNA [3] (Figure 2).
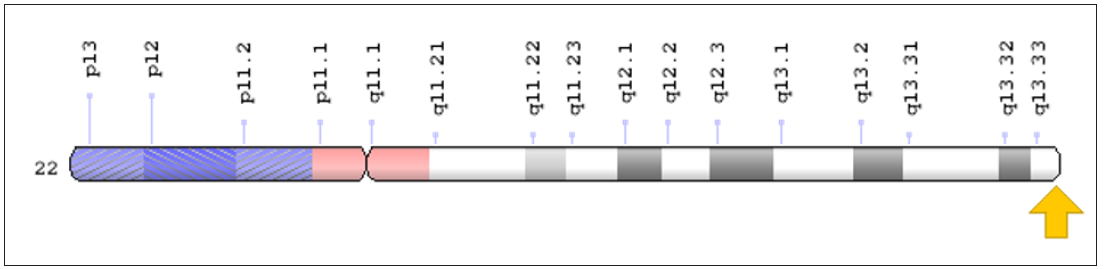
Figure 2. Schematic view of chromosome number 22, in which the TYMP gene is located in he long arm of this chromosome as 22q13.33.
The mitochondria use nucleosides, including thymidine, to create new molecules of mtDNA. The loss of activity of the enzyme thymidine phosphorylase and the increase of thymidine impair the normal maintenance of mtDNA. As a result, mutations can create mithrodine in mtDNA and cause mitochondrial DNA instability. In addition, the proliferation of the thymidine molecule in the mitochondria may reduce the amount of mtDNA below the standard (mtDNA). These genetic changes can cause mitochondrial dysfunction. Although mtDNA abnormalities produce digestive and neurological problems that are characteristic of MNGIE disease, it is still unclear how the defect in mitochondria causes the specific characteristics of the disorder [4].
MNGIE syndrome follows an autosomal recessive hereditary pattern. Therefore, in order to produce this syndrome, two copies of the mutated gene of TYMP (one parent and one of the mothers) are needed, and the chance of having a child with this syndrome in an autosomal recessive state is 25% for each pregnancy [5].
Frequency of MNGIE syndrome
MNGIE syndrome is a genetic disorder whose frequency is not known in the world. So far, about 70 cases of this syndrome have been reported in medical literature from around the world [6] (Figure 3).
Diagnosis of MNGIE Syndrome
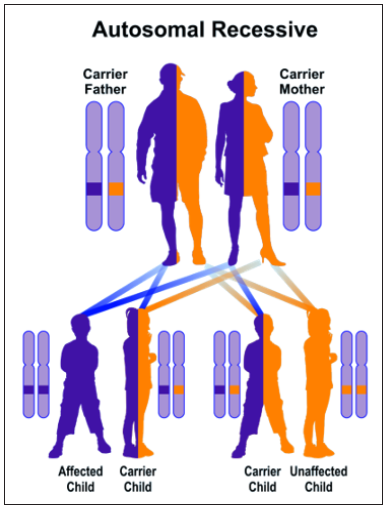
Figure 5. Schematic view of the autosomal recessive hereditary pattern that follows the MNGIE syndrome.
MNGIE syndrome is diagnosed based on the clinical and physical findings of the patients and some pathological tests. The most accurate method for diagnosing this syndrome is the molecular genetic testing of the TYMP gene to investigate the presence of possible mutations [7] ( Figure 4 & 5)
Treatment Routes for MNGIE syndrome
The MNGIE syndrome treatment and management strategy is symptomatic and supportive. Treatment may be done by a team of experts, including orthopedics, eye specialist, neurologist, dietitian, gastroenterologist and other healthcare professionals. There is no valid treatment for this syndrome, and all clinical measures are needed to reduce the suffering of the sufferers. Genetic counseling is also important for all parents who want a healthy baby [8] (Figure 6).
Discussion and Conclusion
MNGIE syndrome is a genetic disorder that affects several parts of the body, in particular the digestive system and the nervous system. Almost all people with MNGIE syndrome have gastrointestinal disorder in which gastrointestinal muscles and nerves do not move food efficiently. MNGIE syndrome is caused by the mutation of the TYMP gene, which is based on the long arm of chromosome 22, based on 22q13.33. There is no valid treatment for this syndrome, and all clinical measures are needed to reduce the suffering of the sufferers.
References
- Hirano M, Martí R, Spinazzola A, Nishino I, Nishigaki Y (2004) Thymidine phosphorylase deficiency causes MNGIE: an autosomal recessive mitochondrial disorder. Nucleosides Nucleotides Nucleic Acids 23(8-9): 1217-1225.
- Hirano M, Silvestri G, Blake DM, Lombes A, Minetti C, et al. (1994) Mitochondrial neurogastrointestinal encephalomyopathy (MNGIE): clinical, biochemical, and genetic features of an autosomal recessive mitochondrial disorder. Neurology 44(4): 721-727.
- Hirano M (2005) Mitochondrial Neurogastrointestinal Encephalopathy Disease. In: Pagon RA et al. (Eds), Gene Reviews®, Seattle, University of Washington, Seattle, USA.
- Lara MC, Valentino ML, Torres-Torronteras J, Hirano M, Martí R (2007) Mitochondrial neurogastrointestinal encephalomyopathy (MNGIE): biochemical features and therapeutic approaches. Biosci Rep 27(1-3): 151-163.
- Marti R, Spinazzola A, Nishino I, Andreu AL, Naini A, et al. (2002) Mitochondrial neurogastrointestinal encephalomyopathy and thymidine metabolism. results and hypotheses. Mitochondrion 2(1-2): 143-147.
- Nishino I, Spinazzola A, Hirano M (2001) MNGIE: from nuclear DNA to mitochondrial DNA. Neuromuscul Disord 11(1): 7-10.
- Nishino I, Spinazzola A, Papadimitriou A, Hammans S, Steiner I, Hahn CD, et al. (2000) Mitochondrial neurogastrointestinal encephalomyopathy: an autosomal recessive disorder due to thymidine phosphorylase mutations. Ann Neurol 47(6): 792-800.
- Teitelbaum JE, Berde CB, Nurko S, Buonomo C, Perez-Atayde AR, et al. (2002) Diagnosis and management of MNGIE syndrome in children: case report and review of the literature. J Pediatr Gastroenterol Nutr 35(3): 377-83.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.