Mini Review 
 Creative Commons, CC-BY
Creative Commons, CC-BY
The First Reported COVID 19 Infection in a Patient with Cardiovascular Disease in Sudan; Case Report
*Corresponding author: Mohd Ahmar Rauf, Barbara Ann Karmanos Cancer Institute, School of Medicine, Wayne State University, Detroit, Michigan, USA.
Received: June 22, 2020; Published: September 15, 2020
DOI: 10.34297/AJBSR.2020.10.001504
Abstract
The Corona virus disease 2019, caused by severe acute respiratory syndrome coronavirus 2, and has become the furthermost popular clinical entity since the beginning of the year 2020, as a viral infection spread rapidly and has significant mortality rate. The aim of this study is to report the first case of COVID 19 in Sudan. Here we are report a 26-year-old female, presented with generalized edema, cough, fever, shortness of breath and one-month history of left side hemiplegia. Clinical examination and lab investigation show the diagnosis of anemic heart failure, echocardiography revealed a severe mitral stenosis. Eight days after receiving the treatment patient markedly improved in spite of raising temperature, Chest computer tomography (CT), real time PT-PCR nasopharyngeal swab and sputum for COVID 19 Confirmed the diagnosis. Five days later patient passed away after developed massive pleural effusion.
Keywords: COVID 19; Mitral stenosis; Sudan; Young female
Introduction
A serious of unexplained cases with pneumonia have been reported in Wuhan, china. The disease has a very similar clinical manifestation of viral pneumonia. After multiple sequences analysis of respiratory tract samples, a novel strain of coronavirus was isolated, and has been named Coronavirus Disease 2019 (COVID19) [1]. Common symptoms include cough, fever, fatigue and myalgia [2].
Complications include acute cardiac injury, acute respiratory distress syndrome and secondary infections [3], however data regarding cardiovascular involvement due to COVID 19 are less described. here we describe the first reported case of COVID 19 infection in Sudan complicated by mitral valve lesion.
Case Report
We are presenting 26 years old female, postpartum delivered two months ago by normal vaginal delivery at hospital, presented with generalized body swelling, cough and shortness of breath (SOB) two weeks prior to admission. Three days prior to her admission patient condition deteriorated, she developed SOB even at rest associated with severe continuous cough, productive of blood-stained sputum and mild grade fever. Then she was brought to hospital at 4 of April 2020. Regarding her past medical history, the patient had mild hemoptysis started one year ago, mild, on and off, she sought medical advice, tuberculosis was excluded, and the etiology remained unknown.
Also, there is history of left sided weakness and mouth deviation one months prior to presentation, but the patient was alert, and conscious, she did not attend to hospital.
No other significant past history, no history of recent travel, and no family history of similar condition. On examination, she was vitally stable, conscious, oriented, edematous and severely dyspneic, severely pale, had irregular pulse and raised JVP.
Examination of chest and pericardium revealed: normal air entery, loud first heart sound, mid diastolic murmur, gallop rhythm, sinus tachycardia 130 beat/minute, pan-systolic murmur at tricuspid area and fine basal crepitation. There was also tender hepatomegaly, massive lower limb oedema, and left sided weakness with power grade zero.
Her investigations showed: hemoglobin level: 5,7 ( normal ref: 12-16g/dl), total white blood cells 9.2 ( normal: 4-10), platelet count 186 ( normal ref: 150-450), her renal function test shows normal creatinine level 0.6 (normal ref: 0,5-0.9), urea: 59 (normal ref: 10-50), serum sodium: 134 ( normal ref: 135-145mmol/L), serum potassium: 3.7 (normal ref: 3.5-4.5mmol/L). Echocardiography shows severe mitral stenosis, severe pulmonary hypertension, severe tricuspid regurgitation, Multiple Left atrium thrombi (Figure 1). Patient diagnosed as: Anaemic heart failure, multiple valvular lesions which lead to atrial fibrillation and ischemic stroke. Patient admitted to cardiac care unite and received optimal treatment including blood transfusion, anticoagulants, and diuretics. 8 days later after receiving the treatment patient showed marked improvement, she was out of anemic heart failure, Lung was clear on auscultation, lower limb edema subsided ,her condition was stable apart of mild fever which was increasing from 38.5 c on day 8 to 40 c after two days and cough persisted.
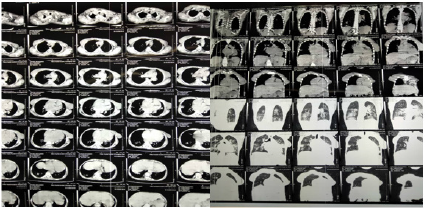
Full septic screening was done with no isolated organism, urine culture showed no growth, three-time negative blood culture and negative gene Xpert for tuberculosis. Erythrocyte sedimentation rate (ESR): 70 mm/hr (normal ref 1–20 mm/hr), C reactive protein: 22 mg/L (Normal ref: below 3.0 mg/L).Hemoglobin level: 11.7 ( normal ref: 12-16 g/dl), total white blood cells 4.3 ( normal: 4-10). CT Chest was done which showed bilateral ground glass opacity (Figure 2). And a diagnosis of COVID 19 was highly suspicious, Sputum and nasopharyngeal swab collected on day 14 after admission.
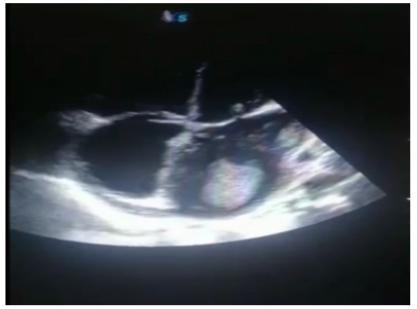
Figure 1: shows severe mitral stenosis, severe pulmonary hypertension, severe tricuspid regurgitation.
The real time PT-PCR result was conclusive to the diagnosis. patient transfer to the isolation center with stable condition, five days later she passed away after developed massive pleural effusion.
Discussion
On 13 March 2020, Sudan federal Ministry of health reported the first case of COVID 19 for an elderly male came from United Arab Emirates a week before he died on 12 March 2020. A week later, precisely on 20, March 2020 the second case has been reported for a foreign young man came to the country a week before after been reported. Today on 2 of May 2020 the accumulative number of all patients been reported by Sudan Ministry of health is 5173 confirmed case.
Mitral valve lesion can occur due to multiple factors such as rheumatic fever (RF) and Infections [4], however the valvular lesion in the reported case is newly discovered after admission although her medical history may indicate she may suffer from underlying heart disease for long duration as she was complaining of hemoptysis for one year duration which is mainly due to cardiovascular causes and can be sign of pulmonary hypertension, other cause of hemoptysis like tuberculosis has been excluded many times by sputum culture and gene Xpert test. pulmonary hypertension itself can be a complication to mitral valve lesion [5], the patient also presented with anemic heart failure and she was pregnant which are both contribute in aggravate the conditions [6].
She also presented with one month history of left sided hemiplegia, they sought medical advice but no further investigations such as brain imaging were done as they were finically unaffordable, after echocardiography was done revealed left atrial thrombus and multiple small thrombi, those were mainly the underlying causes of the patient’s neurological deficit.
Most of the reports indicate clearly multiple comorbidities including cardiac, neurological conditions and recent history of delivery being risk factors of adverse outcomes from COVID 19 [7], however coronaviruses infection itself has been reported to participate in developing sever cardiac complications [8], either directly through the virus replication in the myocardium or indirectly via the immune response caused by the virus or the systemic response to respiratory failure [9]. For instance, SAR-CoV infection can causes myocardial injury due to down regulation of the ACE2 system, and this may lead to adverse cardiac outcome [9].
Cardiac patients with COVID 19 are prone to multiple complications such as arrhythmias, Myocarditis, hypotension and sudden cardiac death [10,11], So early detection and management of this viral infection is important to avoid kind of complications, most of the cardiac patients during COVID 19 outbreak revealed electrocardiographic abnormalities raised troponin level and subclinical left ventricular (LV) diastolic impairment [11], and hence it’s important to pay attention to the cardiac biomarkers level as most studies indicate almost all hospitalized COVID 19 patients have elevated levels of lactate dehydrogenase (LDH) and serum creatine kinase (CK) [12-14], other considerations beside echocardiography which may show regional or global myocardial systolic dysfunction with or without a pericardial effusion and the opposite, Troponin to identify patients with silent myocardial injury and assessment for the patients who may be requiring ICU, D-dimer and Ferritin may for poor outcome [10]. Regarding the treatment strategies and antiviral therapies for Cardiac patient with COVID 19, careful consideration should be taken about the interaction and toxicities with cardiovascular medications. well recognition and early isolation for cardiovascular patients with high suspicion of COVID 19 is important as they are vulnerable group and can be potentially infected. patients also should be vaccinated against pneumonia as secondary bacterial infection can worsen the outcomes of COVID 19 [15].
In the event of cardiac arrest, health care workers are at high risk as cardiopulmonary resuscitation (CPR) can causing aerosolized pathogens leading to viral particles dissemination to clinicians, so protective a measure such as using external mechanical compression devices can lower direct contact with patients. Specific protocols regarding diagnosing, triaging, isolation and management should be developed among health care providers when dealing with COVID 19 patients with cardiovascular complications or cardiovascular patients with COVID 19 to guarantee good outcomes.
In this reported case the patient has no history of travel to or from any area with COVID 19 outbreak or contact with confirmed patient, and hence she acquired the virus from the community and she was been presented to the hospital after three weeks from the first reported COVID 19 case in Sudan. And in both ways either her comorbidities predispose the risk of the infection or the opposite where the virus itself aggravated her conditions.
Conclusion
This is not the first announced case of COVID 19 in Sudan but is the first reported case of COVID 19 to the scientific community. The reported case is young patient with neurological and cardiac comorbidities, tested positive with COVID 19. The report highlights the importance of laboratory testing and clinical surveillance in patients with recent symptoms of acute illness to guarantee appropriate identification and early isolation to individual at risk of COVID 19.
Acknowledgments
This study is been done as collaborative project Between Medical and Cancer Research Institute (MCRI), Nyala, Sudan. And Institute of molecular biology.
Financial Support
None
Conflicts of Interest
All authors declare there are no conflicts of interest
References
- Zheng R, Xu Y, Wang W, Ning G, Bi Y (2020) Spatial transmission of COVID-19 via public and private transportation in China. Travel medicine and infectious disease 34:101626.
- Lei Z, Cao H, Jie Y, Huang Z, Guo X, et al. (2020) A cross-sectional comparison of epidemiological and clinical features of patients with coronavirus disease (COVID-19) in Wuhan and outside Wuhan, China. Travel medicine and infectious disease 35:101664.
- Ribas RM, Campos PA, Brito CS, Gontijo-Filho PP (2020) Coronavirus Disease 2019 (COVID-19) and healthcare-associated infections: Emerging and future challenges for public health in Brazil. Travel medicine and infectious disease 101675.
- Adam MEAE, Osman SME, Abdalrasoul DIA, Yagoup IAO, Hussein MMA, et al. (2020) Echocardiography Effectiveness in Improving Diagnosis of Rheumatic Heart Disease in North Darfur: A Hospital-based Study. Exploratory Research and Hypothesis in Medicine 5(1): 11-18.
- Song X, Zhang C, Chen X, Chen Y, Shi Q, et al. (2015) An excellent result of surgical treatment in patients with severe pulmonary arterial hypertension following mitral valve disease. Journal of cardiothoracic surgery 10(1): 70.
- Tsiaras S, Poppas A (2009) Mitral valve disease in pregnancy: outcomes and management. Obstetric medicine 2(1): 6-10.
- Chung CJ, Nazif TM, Wolbinski M, Hakemi E, Lebehn M, et al. (2020) Restructuring of Structural Heart Disease Practice During the Covid-19 Pandemic. Journal of the American College of Cardiology 75(23): 2974-2983.
- Shah PB, Welt FGP, Mahmud E, Phillips A, Kleiman NS, et al. (2020) Triage Considerations for Patients Referred for Structural Heart Disease Intervention During the Coronavirus Disease 2019 (COVID-19) Pandemic: An ACC /SCAI Consensus Statement. journal of the Society for Cardiac Angiography & Interventions 13(12):1484-1488.
- Oudit GY, Kassiri Z, Jiang C, Liu PP, Poutanen SM, et al. (2009) SARS-coronavirus modulation of myocardial ACE2 expression and inflammation in patients with SARS. European journal of clinical investigation 39(7): 618-625.
- Guzik TJ, Mohiddin SA, Dimarco A, Patel V, Savvatis K, et al. (2020) COVID-19 and the cardiovascular system: implications for risk assessment, diagnosis, and treatment options. Cardiovascular research 116(10): 1666-1687.
- Xiong TY, Redwood S, Prendergast B, Chen M (2020) Coronaviruses and the cardiovascular system: acute and long-term implications. European heart journal 41(19): 1798-1800.
- Huang C, Wang Y, Li X, Ren L, Zhao J, et al. (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395(10223): 497-506.
- Liu PP, Blet A, Smyth D, Li H (2020) The Science Underlying COVID-19: Implications for the Cardiovascular System. Circulation 142(1): 68-78.
- Lippi G, Lavie CJ, Sanchis-Gomar F (2020) Cardiac troponin I in patients with coronavirus disease 2019 (COVID-19): Evidence from a meta-analysis. Progress in cardiovascular diseases 63(3): 390-391.
- Chen C, Qi F, Shi K, Li Y, Li J, et al. (2020) Thalidomide combined with low-dose glucocorticoid in the treatment of COVID-19 pneumonia.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.