Opinion 
 Creative Commons, CC-BY
Creative Commons, CC-BY
COVID-19 hospital admission appropriateness analysis
*Corresponding author: Abelardo Fernández Chávez, Preventive Medicine, Ramón y Cajal University Hospital, Preventive Medicine, M-607, km. 9, 100, 28034 Madrid, Spain.
Received: October 31, 2020; Published: December 03, 2020
DOI: 10.34297/AJBSR.2020.11.001599
Introduction
Inconsistencies in clinical practice, coupled with uncertainty, are constants across all scenarios and throughout all time. In countries with better-developed healthcare models, overuse is far more problematic than underuse, hence the appearance of methods for assessing hospital inadequacy at the end of the 20th century [1]. During the COVID-19 pandemic, hospital admission criteria have been questioned based on the alleged inconsistency between hospitals [2,3]. Several studies put the proportion of inappropriate visits to hospital emergency services at between 20% and 80% of the total [4,5]. However, these studies date to the pre-SARS-CoV-2 pandemic period.
Purpose
This study was to compare hospital admission criteria applied to COVID-19 patients in the emergency department of the Ramón y Cajal University Hospital (HURyC) and their alignment with the AEP (Appropriateness Evaluation Protocol) and PSI (Pneumonia Severity Index).
Methodology
The HURyC is an extremely complex hospital with approximately 720 beds. Between 14 September and 5 October 2020, 501 patients diagnosed with SARS-CoV-2 were admitted to the hospital through the HURyC emergency department. We selected a random sample of 40 of these patients from a list of patients arranged in date order. The first patient was selected from the admissions on 14 September, and subsequent patients were selected at fixed intervals of 12 patients to a total of 40 patients.
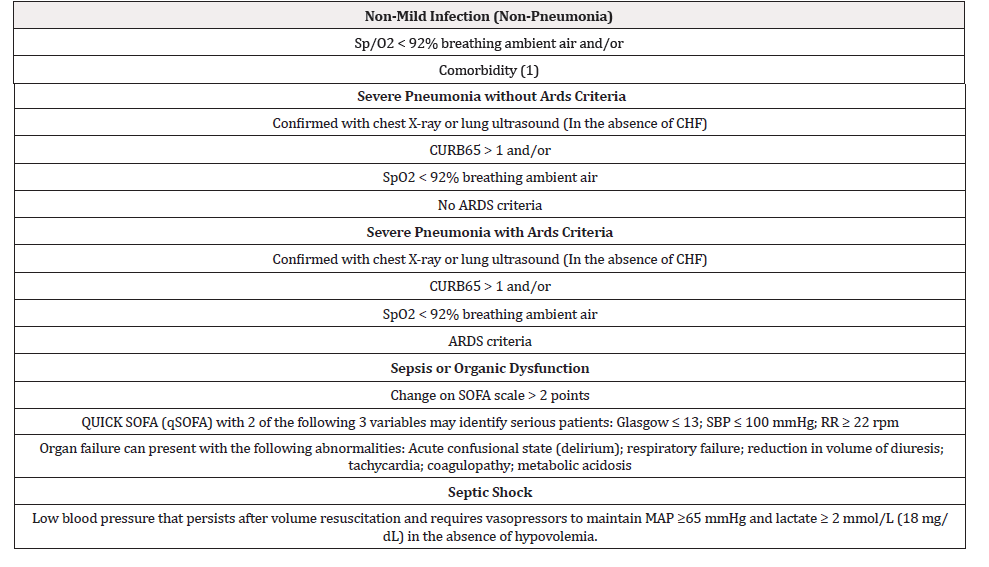
The hospital admission criteria established in the emergency department of Hospital Ramón y Cajal (Table 1), the AEP and PSI scales were used [6,7] to meet the study objectives.
(Table 1).Results
All patients admitted to the hospital through the emergency department were hospitalised correctly according to the AEP scale, and 65% were hospitalised according to the HURyC admission criteria. If we add the patients hospitalised according to the hospital admission criteria with a SCORE equal to or greater than III on the PSI scale, the percentage of patients increases to 82.5%. Of these, 9.09% were non-mild infections (non-pneumonias); 60.61% were severe cases of pneumonia without ARDS; 9.10% had sepsis, and 21.21% were cases with PSI equal to or greater than III. A total of 17.5% of the patients did not fulfil the hospital admission or PSI criteria, and all these patients had mild pneumonia.
Discussion and conclusions
There is a need for a consensus on the hospital criteria to be adopted during the current COVID-19 pandemic. This study shows a total alignment between the hospital admissions and the MAP scale, i.e. there was no incongruency. Like the studies conducted during the pre-COVID-19 period, the MAP scale was closely aligned with appropriate hospital admission [2].
When the HURyC COVID-19 hospital admission criteria were applied, it was seen that 65% of hospitalisations were appropriate, but if we included patients with Score greater than or equal to III on the PSI scale, this percentage increased to 82.5%. The discrepancy between criteria may be explained by the fact that by assessing COVID-19 hospital admission criteria alone, other dependent nondiagnostic admission criteria were not considered. The AEP scale is for independent diagnosis.
The study was conducted during the second wave of increased incidence of SARS-CoV-2 cases in the Community of Madrid. It has been carried out scrupulously according to HURyC criteria for COVID-19 case. It is based on clinical data from the hospital’s electronic medical records. However, we have not considered other factors that influence the decision to hospitalise, such as social issues, hospital pressure, among others.
References
- Gertman PM, Restuccia JD (1981) The appropriateness evaluation protocol: a technique for assessing unnecessary days of hospital care. Med Care 19(8): 855-871.
- Puig C, Carrasco G, Cid R, García M, Martí J, et al. (2004) Factors associated with inadequate admissions for emergencies in a tertiary private hospital. Healthcare Quality Magazine 19(6): 363-369.
- Rahimi H, Ostovar R, Vali L, Angha P (2019) Investigating inappropriate admissions and hospitalisations in Yasuj educational hospitals based on appropriateness evaluation protocol (AEP): A case study in the internal and surgical wards. Int J Health Plann Manage 34(2): 636-643.
- Murphy AW (1998) ‘Inappropriate’ attenders at accident and emergency departments I: definition, incidence and reasons for attendance. Fam Pract 15(1): 23-32.
- Reducing non-urgent use of the emergency department: a review of strategies and guide for future research. Health Services Utilization and Research Committee
- Kim MA, Park JS, Lee CW, Choi WI (2019) Pneumonia severity index in viral community acquired pneumonia in adults. PLoS One 14(3): e0210102.
- Aranaz Andrés JM, Martínez Nogueras R, Rodrigo Bartual V, Gómez Pajares F, Antón García P (2004) Adequacy of the demand for health care in hospital emergency services. Clinical medicine 123(16): 615-618.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.