Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
HIV Positive Adults and Kaposi Sarcoma Cases Prevalence in Namibia
*Corresponding author: Sheehama J, University of Namibia, Namibia.
Received: April 08, 2021; Published: April 26, 2021
DOI: 10.34297/AJBSR.2021.12.001780
Abstract
HIV/AIDS is a global pandemic. The annual number of new HIV infections has steadily declined and due to the significant increase in people receiving antiretroviral therapy, the number of AIDS-related deaths has also declined. Namibia is one of the worst affected countries by HIV/AIDS in the world. Kaposi sarcoma is an opportunistic malignancy that occurs in HIV positive patients, the epidemic of AIDS-related type. Even though Kaposi sarcoma incidence has declined during the late 1990s with the advent of highly active antiretroviral therapy (HAART) against HIV, Namibia must invest more in the screening and treatment of this condition.
This is a quantitative study that enumerated the number of KS cases found within a HIV/AIDS population in Namibia. It was a case series that quantified retrospectively, the number of cases of Kaposi sarcoma recorded over a period of 1 year at the Windhoek Central Oncology Clinic using convenience sampling method. The data collected was recorded and entered an Epi-info 7 document project for data analysis. Data was used to calculate the prevalence and relevant frequencies.
During the study, 93 cases of KS were reviewed. Prevalence of KS is HIV positive adults in Namibia was 0.03%. The frequency in males (63.44%) was more than female counterparts (36.56%). The ages of patients ranged between 21 and 75 years. The mean age was 41.5 years. Similarly, the mode and median age distribution of KS in HIV positive adults in Namibia was 41 years. The frequency of KS was highest in the age group of 38-47 years of age. Histologically diagnosis (81.72%) predominated over clinical diagnosis (18.28%). The highest frequency of KS lesion location was found in the legs, specifically left leg, and right leg, 15.05% and 13.98% respectively.
Overall, the prevalence of KS in HIV positive adults in Namibia is relatively low according to ratios but 93 cases were reported over a period of one year which is a significant number independently.
Keywords: Infection, Cancer, Patient
Introduction and Background
Human immunodeficiency virus (HIV) is an incurable and very potent virus that lowers the immunity and allows for a variety of diseases to flourish in the body. This state of severe immunosuppression and attack by the opportunistic infections is a stage of the viral infection known as AIDS (acquired immunodeficiency syndrome) [1-3].
HIV/AIDS has been in existence for at least two decades now since its initial description in the 1980s. The overall growth of the epidemic has stabilized in recent years [4,5]. The annual number of new HIV infections has steadily declined and due to the significant increase in people receiving antiretroviral therapy, the number of AIDS-related deaths has also declined. With around 68 percent of all people living with HIV residing in sub-Saharan Africa, the region carries the greatest burden of the epidemic.
Namibia is one of the worst affected countries by HIV/AIDS in the world. According to the latest world HIV/AIDS rankings, 2009, Namibia falls in the 7th position. In its population of about 2 million, at least 200 000 people are living with HIV/AIDS (UNAIDS, 2010) [6-11]. One of the opportunistic diseases that attack the body due to immune suppression is a form of cancer known as Kaposi Sarcoma. KSHV is now thought to be largely transmitted by saliva. Although associated with sexual risk factors, these may just be a surrogate for close contact. Heterosexual risk factors largely do not play a role here. Transmission by blood or blood products can occur but use of leukopoor stored blood is likely to significantly reduce this risk. Transmission of KSHV may occur during solid organ donation, but it does not appear to affect clinical outcome in terms of survival or graft loss [12]. There may be an increase of incidence of KS in patients in solid organ recipients that are seropositive versus those that seronegative (Medscape, 2014).
Problem Statement and Study Justification
Before the AIDS pandemic, KS rarely occurred, however, there had been a rise in the incidence of this type of cancer with rise of the HIV/AIDS pandemic in the 1990s. But with new treatment for AIDS, KS has become less common in the United States, with about 6 cases per million people each year. Regardless, HHV8 is still commonly found in HIV infected people than in the general population. It is estimated that an HIV-infected person has 20,000 times increased risk of developing KS compared with people without HIV (American cancer association, 2010) [13,14]. There are no publications on this topic in Namibia therefore this study would be significant step in acquisition more knowledge about the disease than is already known in this country. This study may also trigger a more extensive research on the subject apart from creating awareness to the MoHSS.
Methodology
This is a quantitative study that enumerated the number of KS cases found within a HIV/AIDS population in Namibia.
Study Population
The study was carried out at Windhoek central hospital. Windhoek Central Hospital and Katutura Hospital together called the Windhoek State Hospital Complex (WSHC) form the national referral hospital. The WSHC has a capacity of 1383 beds. This is the last point in the referral system. Services which are rendered and departments by the national referral hospitals are as follows: Specialists such as pediatricians, physicians, obstetricians and gynecologists, general surgeons and oncologists; services of cardiothoracic surgeons, neurosurgeons and plastic surgeons should be provided on a visiting basis. In addition, intensive care, operating theatres, medical laboratory services, radiological services, nuclear medicine, pharmaceutical services, and rehabilitation services are all departments and facilities available.
The oncology clinic, formally known as the Chris Bernard oncology clinic, is the main oncology clinic in Namibia and it receives cancer patient referrals from all the regions. It receives or treats approximately 3000 cancer patients (2012). The center is rich with information on all types of cancers found in Namibia. All the Kaposi sarcoma cases are sent here for treatment [15-17]. The Kaposi sarcoma patients have files allocated to them and as they enter the center, they are recorded in registries that are specific for a type of cancer as all the other types of cancers. The data was collected from the 1st of August to 12th of September 2014.
Sample Size Determination
Sampling was done according to the number of HIV positive patients who developed Kaposi sarcoma and received treatment at the Windhoek oncology clinic. The sampling method that was employed in this study was convenience sampling, meaning every individual that had presented/referred to the oncology clinic with Kaposi sarcoma between June 2013 and June 2014, which was the study period. The sample size estimation will entirely depend on the number of subjects that presented with the cancer.
Study Design
A case series study was employed in this study which is a descriptive study. A case series (also known as a clinical series) is a medical research descriptive study that tracks patients with a known exposure given similar treatment or examines their medical records for exposure and outcome. It can be retrospective or prospective and usually involves a smaller number of patients. Case series may be consecutive or non-consecutive, depending on whether all cases presenting to the reporting authors over a period were included, or only a selection.
The cases series retrospective study used existing data that has been recorded for reasons other than this research. This study looked backward in time using medical records of patients who are already known to have Kaposi sarcoma during the study period. Existing medical records/patient files in the oncology clinic were reviewed for Kaposi sarcoma cases using the data collection tool i.e., data collection sheet, from 1st June 2013 to 1st June 2014, thus a period of 1 year of the most recent data recorded.
Data Collection
Data was collected from an oncology center, meaning that data was collected from a population of cancer patients. The population of focus was all the Kaposi sarcoma cases. The main objective of the study was to determine the prevalence of Kaposi sarcoma in HIV positive adults in Namibia; therefore, the focus was further narrowed down to HIV positive patients only. The overall study population is HIV positive adults in Namibia which was used to calculate the prevalence of KS.
The clinic had different registries allocated to different cancers treated at there that had patients’ records as they became patients there. A Kaposi sarcoma registry was thus also available which made the data collection process tolerable. The Kaposi sarcoma patients’ registry contained the name of the patients, the patients’ date of birth, patients’ sex, and the location of the lesions on the patients’ bodies and whether the diagnosis was made clinically or histologically. The histologic component contained the patients’ lab numbers. Furthermore, the Kaposi sarcoma patient files were filed together in alphabetical order in a clinic cabinet.
The pages with patients admitted during the study period were determined and the information was recorded in the data collection sheet that excluded the patients’ names. With each patient recorded in the KS registry, their file was located from the cabinet where more details needed for the study were reviewed. From the patient files, their HIV status was collected and entered in the data collection sheet. The data was then entered in an Epi-Info project document where data analysis and graphical representations on the information would be done during the formulation of the final paper.
Data Management and Statistical Analysis Strategy
Data collected was double checked for completeness. The data was then entered into an Epi-info 7 document project for data cleaning, management, analysis, and correlations. The data was then further exported to Microsoft excel and word (Microsoft Corporation, Redmond, Washington) for descriptive analysis and graphing.
Ethical Considerations and Approval
Endorsement of the research work was sought and granted by the University of Namibia’s School of Medicine’s Community Medicine Department as well as the Ministry of Health and Social Services. MoHSS granted an approval letter which was given to the Medical superintend of Windhoek central hospital and the nurses and doctors at the oncology clinic were informed about the research being carried out. Respondent’s names were not recorded, their data was saved with codes and their information was confidentially managed. Only I had access to the data collected; the information was kept private, and persons not involved in the study did not have access to it.
Study Limitations
This study was not without its limitations. The study was initially planned to be carried out in the northern part of Namibia which is one of the main regions affected by HIV/AIDS but I was told that all the records regarding Kaposi sarcoma was in Windhoek as all their Kaposi sarcoma patients were referred there for treatment. Therefore, the study could no longer be carried out at the CDC clinic in Oshakati intermediate hospital because better records were guaranteed at the Windhoek central hospital oncology clinic. This also led to the change in the study area. Initially, the area of focus was specifically Oshakati hospital, but the oncology clinic had records of patients with Kaposi sarcoma from all over the country.
Results
Prevalence of Kaposi Sarcoma in HIV Positive Adults in Namibia
The prevalence of HIV in adult Namibians as of 2012, being the latest statistic found, amounted to a population of 292 387 HIV positive adults from a total population of 2.1 million Namibians. The number of KS cases reviewed over a period of one year (June 2014 to June 2014) was 93 cases. This number of KS cases weighed over the total population of HIV positive adults is rather a small number hence the prevalence of KS calculated is 0.03%. In Bower et al. study titled ‘AIDS-related malignancies: changing epidemiology and the impact of highly active antiretroviral therapy’ (2006) found out that the incidence of Kaposi’s sarcoma has declined in the era of highly active antiretroviral therapy and the outcome of both tumors has improved [18]. HAART is free in Namibia and most HIV positive people can be started on treatment once they mean the WHO criteria. Hence it is not surprising to find that the prevalence of KS is low. Although HIV-infected patients are at increased risk of developing cancer, particularly in the later stages of acquired immune deficiency syndrome (AIDS) (Cheung et al, 2005), with the availability and free access of HAART, the prevalence is Namibia is low, 0.03% [19]. This means that the distribution of ARV’s is almost efficient and that the patients are adherent to their medication, preventing them from going into the 4th stage of the disease. This could also be attributed to the fact that; KS is not as infectious as the highly infectious Tuberculosis and therefore not as prevalent [20].
Gender Frequencies
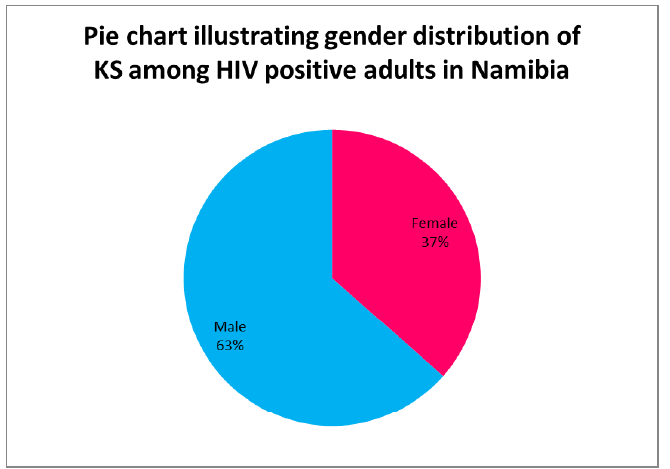
According to the Table 1, from the total number of 93 cases reviewed in this study, 34 cases were females (36.56%), and 59 cases were males (63.44%). This means that KS was more common in adult HIV positive males (Table 1).
a) Female 26.81% 47.19%
b) Male 52.81% 73.19%
The 95% confidence interval (CI) of females lay between 26.81% and 47.19%; whereas in males, the 95% CI lay between 52.81% and 73.19%. Phipps et al, 2010, found that in a cohort (in Uganda) that consisted of 197 adults with HIV and KS: 55% (108/197) were women [21]. This does not coincide with the results of this study. This could possibly imply that women in Namibia are less at risk of getting KS because they are more likely to be on treatment and have better adherence than men (Figure 1).
Age Frequency
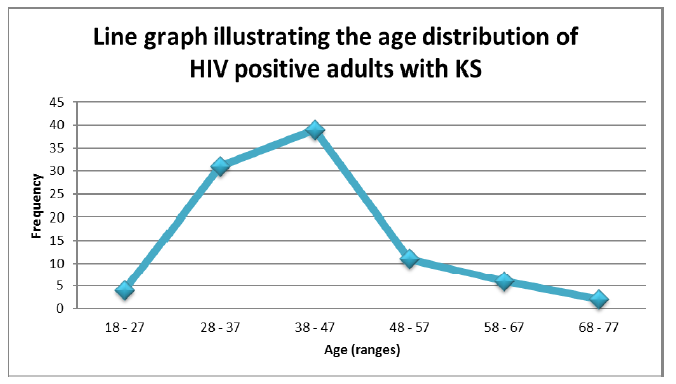
According to Table 2, the youngest patient in the study was 21 years old; the oldest patient was 75 years old. The mean age of HIV positive adults affected by KS is 41.5 years with a standard deviation of 9.97 years. The median and mode of the age range is 41 years old. According to Table 2, the age range of 38-47 years had the highest frequency of adults with KS of 39 adults (41.94%) followed by the younger age range of 28-37 years with a frequency of 31 (33.33%). The third highest age range with a frequency of 11 (11.83%) was an older age range of 48-57 years (Table 2).
The youngest age range (18-27 years) only had 4 cases out 93 cases of KS; whereas the oldest age range (68-77 years) only had 2 cases out of a total of 93 KS cases reviewed. This means that the prevalence of KS was highest among the age of 30- to 50-year-old as deduced from Figure 2.
While the incidence of KS decreased with age, older HIV-infected persons who do not receive HAART are still at increased risk of KS. As KS remains an important malignancy among HIV-infected persons, earlier HIV diagnoses and HAART initiation, particularly in older HIV-infected persons is warranted. According to the study by Luu et al. similary, the frequency of KS decreased with advanced age in Namibia. With no other former data to compare with, the frequency of KS in Namibia also decreased in younger patients [22]. The reason could be because the age range of 30-50 may have the highest prevalence of HIV in Namibia therefore is at risk of getting KS (Figure 2 & Table 3).
Diagnosis Frequency
Kaposi sarcoma is often found when a person goes to the doctor because of signs or symptoms they are having. Sometimes KS may be found during a routine physical exam. If KS is suspected, further tests will be needed to confirm the diagnosis. Depending on where the lesions are found, the following diagnostic test can be carried out: a medical history (e.g., HIV positive), physical examination (examination of KS lesions), biopsy of the suspicious lesions, chest x-ray or pulmonary lesions, bronchoscopy for lesions in the airway and gastrointestinal endoscopy for lesions in the gastrointestinal tract. The test of choice depends on the clinical presentation of the patients and the high index of suspicion of the treating doctor. According to Table 3, there were only two diagnostic ways found among the cases reviewed i.e., clinically, or histologically. 81.72% of the cases were diagnosed histologically [95% CI: 11.02-27.65] (Table 4).
95% Conf Limits
a) Clinically 11.02% 27.65%
b) Histologically 72.35% 88.98%
Meaning biopsy samples of the lesions were taken to the lab and tested to confirm the diagnosis of KS. Sometimes the clinical suspicion of KS is very high and to curb the cost of lab diagnosis, clinical diagnosis can be made. The results showed that 18.28% of the cases reviewed in this study were clinically diagnosed [95% CI: 72.35-88.98].
Most of the lesions, as illustrated by the Table 4, are found on the skin. It can either be one of two possibilities, its either cutaneous manifestation of KS is the most common in Namibia or that interior manifestations are poorly diagnosed: low index of suspicion of the doctors.
Location of Kaposi Sarcoma Lesions
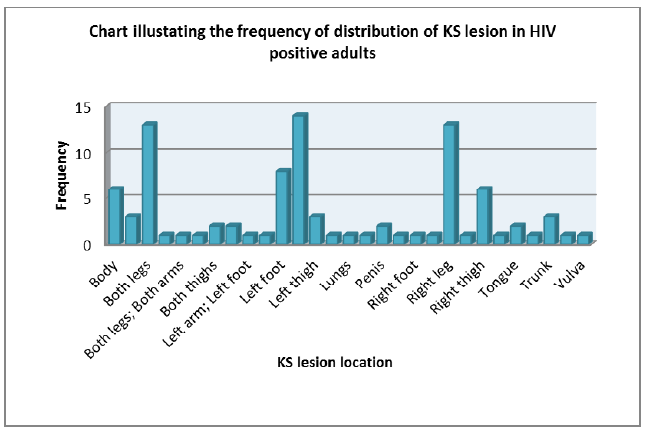
The highest frequencies of lesions were found on the left leg (14), both legs (13), right leg (13) and left foot (8). The bulk of the lesions were found in the lower extremities than in the upper extremities. A different variety of lesions were found as well although in lesser frequencies e.g., 1 case of pulmonary KS, 2 cases of hard palate KS lesions, 2 cases of penile KS lesions, 2 cases of tongue KS, 1 case of tonsillar KS lesion and 1 case of vulvar lesion (Figure 3).
Most of the lesions are cutaneous manifestations according to Table 4 and as mentioned before, the reason could be that Namibians are mostly prone to cutaneous KS or the is poor diagnosis of KS elsewhere in the body. Unfortunately, studies related to this could not be found for comparison.
Conclusions and Recommendations
Namibia is one of the worst affected countries by HIV/AIDS in the world. According to the latest world HIV/AIDS rankings, 2009, Namibia falls in the 7th position. In its population of about 2 million, at least 200 000 people are living with HIV/AIDS (UNAIDS, 2010).
One of the opportunistic diseases that attack the body due to immune suppression is a form of cancer known as Kaposi Sarcoma. Kaposi sarcoma cases have increased with the HIV/AIDS pandemic. But Kaposi’s sarcoma has declined in the era of highly active antiretroviral therapy and the cancer has improved [8].
This study aimed at determining the prevalence of Kaposi sarcoma, as an AIDS defining illness, in the adult HIV population of Namibia to assess whether HIV positive patients in Namibia nonetheless enter stage 4 of the disease in an era of free HAART. The prevalence of KS is HIV positive adults was 0.03% over oneyear duration. Male HIV positive patients were found to suffer more from KS (63.44%) than female counterparts (36.56%).
The youngest patient found to have KS from the study was 21 years old and the oldest was 75 years. The mean age was 41.5 years. Similarly, the mode and median age distribution of KS in HIV positive adults in Namibia was 41 years old. The frequency of KS was highest in the age group of 38-47 years of age. Most of the cases were diagnosed histologically (81.72%) in comparison with clinical diagnosis (18.28%).
Locations of KS lesions found include lesions all over the body, feet, legs, arms, thigh, hard palate, elbow, lumbar area, lungs, nose, penis, big toe, groin, parotid, tongue, tonsils, trunk, and vulva. The highest frequency was found in the legs, specifically left leg, and right leg, 15.05% and 13.98% respectively.
References
- Hogg RS, Yip B, Chan KJ, E Wood, K J Craib, et al. (2001) Rates of disease progression by baseline CD4 cell count and viral load after initiating triple-drug therapy. JAMA 286(20): 2568-2577.
- Palella FJ, Deloria Knoll M, Chmiel JS, Anne C Moorman, Kathleen C Wood, et al. (2003) Survival benefit of initiating antiretroviral therapy in HIV-infected persons in different CD4+ cell strata. Ann Intern Med 138(8): 620-626.
- Schacker TW, Hughes JP, Shea T, R W Coombs, L Corey (1998) Biological and virologic characteristics of primary HIV infection. Ann Intern Med 128(8): 613-620.
- Sepkowitz KA (2001) AIDS--the first 20 years. N Engl J Med 344(23): 1764-1772.
- Weiss RA (1993) How does HIV cause AIDS?. Science 260(5112): 1273-129.
- Cecil, Russell (1988) Textbook of Medicine. Philadelphia: Saunders. Pp. 1523-1799.
- (2003) HIV and Its Transmission. Centers for Disease Control and Prevention.
- (2006) How HIV is spread. San Francisco AIDS Foundation.
- Kallings LO (2008) The first postmodern pandemic: 25 years of HIV/AIDS. J Intern Med 263(3): 218-243.
- (2011) AIDS epidemic update. World Health Organization.
- (2007) 2007 AIDS epidemic update. UNAIDS, WHO.
- Centers for Disease Control (CDC) (1982) Persistent, generalized lymphadenopathy among homosexual males. MMWR Morb Mortal Wkly Rep 31(19): 249-251.
- Barré Sinoussi F, Chermann JC, Rey F, M T Nugeyre, S Chamaret, et al. (1983) Isolation of a T-lymphotropic retrovirus from a patient at risk for acquired immune deficiency syndrome (AIDS). Science 220(4599): 868-871.
- Gao F, D L Robertson, C D Carruthers, Y Li, E Bailes, et al. (1998) An Isolate of Human Immunodeficiency Virus Type 1 Originally Classified as Subtype I Represents a Complex Mosaic Comprising Three Different Group M Subtypes (A, G, and I). J Vir 72(12): 10234-10241.
- Fox J, Hannah Castro, Steve Kaye, Myra McClure, Jonathan N Weber, et al. (2010) Epidemiology of non-B clade forms of HIV-1 in men who have sex with men in the UK. AIDS 24(15): 2397-2401.
- Bobkov AF, Elena V Kazennova, Ludmila M Selimova, Tatyana A Khanina, Grigory S Ryabov, et al. (2004) Temporal trends in the HIV-1 epidemic in Russia: predominance of subtype A. J Med Virol 74(2): 191-196.
- Le Vu S, Yann Le Strat, Francis Barin, Josiane Pillonel, Françoise Cazein, et al. (2010) Population-based HIV-1 incidence in France, 2003-08: a modelling analysis. The Lancet 10(10): 682-687.
- Chalmet K, Delfien Staelens, Stijn Blot, Sylvie Dinakis, Jolanda Pelgrom, et al. (2010) Epidemiological study of phylogenetic transmission clusters in a local HIV-1 epidemic reveals distinct differences between subtype B and non-B infections. BMC Infect Dis 10: 262.
- Laeyendecker O, Li X, Arroyo M, McCutchan F (2006) The Effect of HIV Subtype on Rapid Disease Progression in Rakai, Uganda. 13th Conference on Retroviruses and Opportunistic Infections.
- Kanki PJ, D J Hamel, J L Sankalé, C c Hsieh, I Thior, et al. (1999) Human Immunodeficiency Virus Type 1 Subtypes Differ in Disease Progression. J Infect Dis 179(1): 68-73.
- Murray MC, J E Embree, S G Ramdahin, A O Anzala, S Njenga, et al. (2000) Effect of human immunodeficiency virus (HIV) type 1 viral genotype on mother-to-child transmission of HIV-1. J Infect Dis 181(2): 746-749.
- Tranchat C, P Van de Perre, A Simonon Sorel, E Karita, M Benchaïb, et al. (1999) Maternal humoral factors associated with perinatal human immunodeficiency virus type-1 transmission in a cohort from Kigali, Rwanda, 1988-1994. J Infect 39(3): 213-220.







 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.