Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Minimally Invasive Cross-link: A Cadaveric Feasibility Study with a Working Prototype
*Corresponding author: Kyle McGrath, Ohio University Heritage College of Osteopathic Medicine, Columbus, Ohio, USA.
Received: March 09, 2021; Published: April 01, 2021
DOI: 10.34297/AJBSR.2021.12.001754
Abstract
Spinal fusion involving posterior instrumentation with rods and pedicle screws has been common surgical practice for many years. Traditionally, a cross-link connecting the vertical rods can be added to the construct to increase stability in multiple planes of motion. More recently however, minimally invasive spine surgery (MISS) techniques have gained traction without accompanying technology or methodology to place a cross-link. Herein we describe a novel technique of placing a cross-link percutaneously, accommodating both open and minimally invasive spine fixation. A single cadaveric feasibility study was done, demonstrating the patented technique and instrumentation used in successful deployment of a percutaneous cross-link. The cross-link was successfully deployed and secured to the posterior fixation construct using a fluoroscopy-guided posterior paramedian approach. This study demonstrates that minimally invasive cross-links can be successfully incorporated into both open and minimally invasive posterior fixation procedures, providing added stability while leaving the posterior midline anatomic structures intact.
Keywords: Cross-link, Instrumentation, Fusion, Minimally invasive spine surgery
Abbreviations: MISS: Minimally Invasive Spine Surgery; PLC: Posterior Ligamentous Complex
Introduction
Spinal instrumentation and fusion is a form of spine stabilization surgery offered to patients who are experiencing pain or neurologic deficit secondary to instability of the vertebral column. Instability warranting spinal fusion can result from a variety of sources such as degenerative disease, trauma, tumor, or infection [1]. Spinal fixation is intended to provide patients with long term stability by way of solid bony fusion and accompanying instrumentation. Traditionally, instrumentation involved in spinal fusion has involved pedicle screws connected vertically by metallic rods with or without cross-links connecting both vertical rods together across the midline (Figure 1). Spinal fixation can be done as an open procedure, in which the midline structures are exposed, or more recently, through minimally invasive technique in which the midline may remain unexposed. Cross-link placement has historically required an open approach due to necessary exposure and disruption of midline structures in order to place a rod through this plane. However, in recent decades the spine community has pushed for further research and development of minimally invasive spine surgery (MISS). MISS aims to reduce the amount of surgical invasion and tissue disruption and has been shown to result in a reduction of blood loss, hospital length of stay, and complication rate as compared to open lumbar fusions.[2] Open spine procedures, especially fusions with cross-linking, require significantly more exposure and dissection than MISS, resulting in increased “dead space” and ultimately increasing the risk of infection [3]. Despite the surge in MISS in recent history, there has not been a method of successfully introducing a cross-link in this setting until now [4]. Herein we describe a novel percutaneous technique of crosslink placement that allows for midline structures to remain intact, accompanying both open and minimally invasive spine surgery.
Materials and Methods
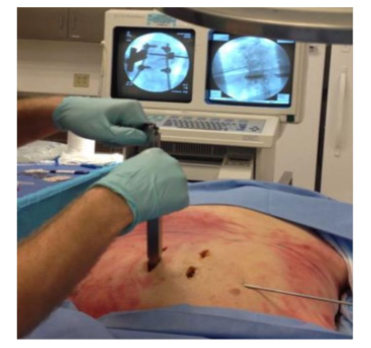
This was a single cadaveric study, and IRB/ethics committee approval was not required. The novel method described herein provides the surgeon the ability to introduce a cross-link to any construct without disturbing the posterior ligamentous complex (PLC) or removing of the spinous process (Figure 2). This cross-link method can accompany both minimally invasive and open pedicle screw and rod construct placement, which requires a posterior approach with the patient in the prone position. Following successful placement of the pedicle screw-rod construct, the crosslink acceptors are first applied to each rod using the specialized applicator (Figure 3) through the same incision(s) in which the adjacent pedicle screws were placed. Upon successful insertion of the cross-link acceptors, introduction of the cross-link was done with the cross-link driver (Figure 4) under fluoroscopic guidance through a separate stab incision via a posterior paramedian approach (Figure 5). The cross-link is equipped with a proprietary self-drilling tip, which, in our cadaveric study, allowed passage through soft tissue and bone (Figure 2). Upon successful guidance of the cross-link through both acceptors, the set screws were placed through the acceptor deployment devices, locking the acceptor, cross-link, and vertical rod construct together. Once the final crosslink construct was secured, the acceptor deployment devices were removed, and the cross-link delivery device was unscrewed and removed.
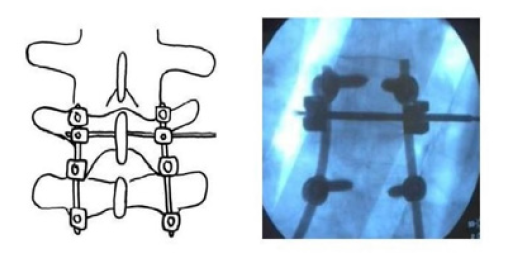
Figure 2: Illustration (Left) and anteroposterior radiograph (Right) of secured cross-link pedicle screw construct, demonstrating cross-link delivery through the base of the spinous process.

Figure 3: Model of the cross-link acceptor deployment device, demonstrating delivery of bilateral cross-link acceptors through the same incision in which the adjacent pedicle screw(s) were placed.

Figure 4: Cross-link driver for lateral delivery via a posterior paramedian approach. The proximal end of the cross-link is screwed into the end of the driver in a clockwise fassion. Upon delivery and locking of the cross-link into both acceptor devices, the driver is then unscrewed in a counterclockwise fashion and removed from the secured cross-link construct.
Results and Discussion
In this study, the cross-link was successfully deployed through the PLC and spinous process, fixated to the vertical rods of a twolevel lumbar fixation. Placement was confirmed with postoperative fluoroscopy. Post-operative examination of the cadaveric specimen revealed that no vital nervous or vascular structures were damaged, with the midline structures remaining intact. Together, postoperative fluoroscopy and dissection confirmed the feasibility of placing a minimally invasive cross-link. In spinal fusion procedures, construct stiffness and resistance to deformation are of utmost importance, as the end goal of these procedures is arthrodesis or bony fusion at the targeted segments. It has been demonstrated that insufficient mechanical stiffness of constructs leads to higher nonunion rates in these patients, supporting the need for adequate construct stability [5].
Cross-links can be used in spinal fixation in order to increase the stability of the construct in all planes of motion, particularly in axial torsion by directly preventing torsional deformation of rods about one another [3]. For this reason, cross-links are often considered in long fusion constructs involving the thoracic spine as axial rotation is a major component of thoracic spine motion [5-8]. In addition to long constructs involving the thoracolumbar spine, those requiring multi-level posterior osteotomies may also benefit significantly from cross-link addition wherein the biomechanical stability of the native spine is significantly reduced [9].
As some of the known benefits of MISS were discussed, a notable biomechanical advantage is the preservation of anatomic components that allow for stabilization in the native spine. Among these stabilizing components that can be preserved is the posterior tension band or posterior ligamentous complex. The PLC, composed of the supraspinous ligament, interspinous ligament, ligamentum flavum, and facet joint capsules is a vital component in maintaining biomechanical stability in a healthy spine by preventing excessive flexion, rotation, distraction, and translation [10]. The PLC is commonly disrupted or completely removed at specific segments during open fixation and decompression of the spine, and a major advantage of MISS is maintaining this “mechanically eloquent” [3] component of the anatomy. Potential benefit of the novel cross-link method discussed can be demonstrated in both MISS (Wiltse and percutaneous approach) and in open spinal fixation procedures when decompression is not indicated. The instrumentation described, including a cross-link equipped with a self-drilling tip allows the surgeon to place the cross-link through the base of the spinous process or lamina if deemed appropriate, which has been shown to add significant stability to a construct vs. cross-links passing between the spinous process (through soft tissue only) [11].
This study was a cadaveric feasibility study using one cadaveric specimen. Although the cross-link was successfully deployed, biomechanical testing still needs to be conducted to assess the integrity of these constructs. Surgeon experience, anatomic knowledge, and clinical reasoning should be considered in conjunction with the current literature when making the decision to implement a minimally invasive cross-link.
Conclusions
This feasibility study demonstrates a surgical method with novel instrumentation and technique that now allows the spine surgeon to introduce a cross-link through an entirely percutaneous approach allowing for preservation of the posterior midline structures. In addition to preserving more of the normal anatomy, this method of cross-link implementation may carry the added benefit of offering surgeons an avenue to incorporate MISS into their practice. Surgeons who find cross-links beneficial may be inclined to perform open fixation procedures in order to accommodate placement of a cross-link, however the minimally invasive crosslink method may allow surgeons to explore MISS procedures where they previously would not have. Looking ahead, further research is necessary in order to determine biomechanical properties and long-term outcomes associated with the use of minimally invasive cross-links.
Acknowledgements
Source of Financial Support: OhioHealth Research Institute Grant: $50,000.
Conflicts of Interest
The authors have no disclosures or conflicts of interest to report.
References
- Wang R, Li C, Yi X, Lu H, Wang Y, et al. (2020) Causes of lower extremity weaknesses after posterior lumbar spine fusion surgery and therapeutic effects of active surgical exploration. J Orthop Surg Res 15(1): 435.
- Hammad A, Wirries A, Ardeshiri A, Nikiforov O, Geiger F (2019) Open versus minimally invasive TLIF: literature review and meta-analysis. Journal Orthop Surg Res 14(1): 229.
- Benzel EC (2015) Biomechanics of Spine Stabilization. In: Biomechanics of Spine Stabilization. Thieme pp. 208-450.
- Karas C (2012) Systems, methods, and apparatuses for spinal fixation.
- Robert Hart, Werner Hettwer, Qi Liu, Shilpa (2006) Prem Mechanical Stiffness of Segmental Versus Nonsegmental Pedicle Screw Constructs: The Effect of Cross-Links. Spine 31(2): E35-E38.
- Dick JC, Zdeblick TA, Bartel BD, Kunz DN (1997) Mechanical Evaluation of Cross-Link Designs in Rigid Pedicle Screw Systems. Spine 22(4): 370-375.
- Mina Alizadeh, Mohammed Rafiq Abdul Kadir, Miskon Mohd Fadhli, Ali Fallahiarezoodar, Baharudin Azmi, et al. (2013) The use of X-shaped cross-link in posterior spinal constructs improves stability in thoracolumbar burst fracture: A finite element analysis. J Orthop Res 31(9):1447-1454.
- Dick JC, Jones MP, Zdeblick TA, Kunz DN, Horton WC (1994) A Biomechanical Comparison Evaluating the Use of Intermediate Screws and Cross-Linkage in Lumbar Pedicle Fixation. J Spinal Disorders 7(5).
- Ronald A Lehman Jr, Daniel G Kang, Scott C Wagner, Haines Paik, Mario J Cardoso, et al. (2015) Biomechanical stability of transverse connectors in the setting of a thoracic pedicle subtraction osteotomy. Spine J 15(7): 1629-1635.
- Alexander R Vaccaro, Joon Y Lee, Karl M Schweitzer Jr, Moe R Lim, Eli M Baron, et al. (2006) Assessment of injury to the posterior ligamentous complex in thoracolumbar spine trauma. Spine Journal 6(5): 524-528.
- Yasuhiro Nakajima, Masahito Hara, Daisuke Umebayashi, Shoichi Haimoto, Yu Yamamoto, et al. (2016) Biomechanical Analysis of a Pedicle Screw-Rod System with a Novel Cross-Link Configuration. Asian Spine J 10(6): 993-999.




 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.