Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Differences Between Night and Day Porters in Heart Rate Variability as A Measure of Cardiovascular Health
*Corresponding author: Lu G, Department of Military Biomedical Engineering, Fourth Military Medical University, Xi’ an, 710032, PR China.
Received: November 09, 2021; Published: November 15, 2021
DOI: 10.34297/AJBSR.2021.14.002036
Abstract
Purpose: To find the evidence of an association between night shift work and an increased incidence of health problems, in particular cardiovascular disease.
Methods: This study used heart rate variability (HRV) as a measure of cardiovascular health and resilience along with detailed questioning on general health, lifestyle and shift patterns, to draw comparisons between night porters and their day-working counterparts.
Results: Significant differences were found in aspects of cardiovascular response to heart rate and high frequency power in heart rate variability between the night porters and day porters, which could reflect disruption to autonomic control.
Conclusion: This study presents the evidence for HRV differences between day and night workers doing the same job following imposed autonomic challenge.
Keywords: Cardiovascular disease, Heart rate variability, High frequency power
Introduction
It has long been thought that there is some association between shift work and myocardial infarction (MI). Study shows that Consecutive night shifts have effect on the health problems of the porters in cortisol, melatonin and heart rate variability (HRV) [1]. The Hulsegge et al study shows that shift work is associated with reduced heart rate variability among men but not women [2]. The Knutsson et al study shows a relative risk ratio for MI in shift workers of 1.6 in men and 3.0 in middle aged women [3]. HRV is as a predictor of CVD morbidity and mortality [4]. Decreased HRV has also been associated with higher work stress and shift work [5,6]. HRV is the beat-to-beat variation in heart rate usually derived from analysis of R-R intervals in ECG recordings. It is thought that HRV is an important factor in physiological resiliency and behavioural flexibility, in that a higher frequency HRV reflects higher autonomic sensitivity, and greater ‘health’ due to the individual’s ability to adapt effectively to stress or environmental changes. There has been some success in using HRV measurements prognostically to predict outcome in congestive heart failure, development of ventricular dilatation post MI, and for identifying diabetic patients with autonomic neuropathy, though its greatest value is also thought to be for post MI prediction of mortality, with a reduced HRV seen to be an adverse marker. In addition, HRV has been shown to hold prognostic significance for CVD in healthy subjects [7]. The Greiser study discusses the association between reduced HRV and psychosocial factors, suggesting HRV to be a mediator linking stressful events with CVD events, so could therefore be an important factor linking increased job stress in shift workers, perhaps due to circadian disruption to the increased risk of development of CVD. The ratio between the low and high frequency bands has been claimed to represent the relative contributions of the two branches of the autonomic nervous system in the regulation of cardiac function which lead to an otherwise ambiguous end-organ response, and can therefore be used diagnostically for CVD. There is considerable evidence against that LF power as an adequate reflection of sympathetic modulation of heart rate includes that neither β-blockade nor direct sympathetic blockade via epidural abolish LF power, and that atropine which blocks the vagal parasympathetic of heart rate reduces LF power, showing that both the sympathetic and parasympathetic systems contribute to the LF band. Despite this evidence to the contrary, LF:HF ratio has been shown to represent a measure of sympathovagal modulation of sino-atrial node pacemaker activity in healthy subjects, though less useful in a clinical setting with cardiac patients, and despite incomplete understanding of the relative contributions to LF and HF power, Lombardi concludes in his 2002 review, that the methodology is useful for evaluating autonomic control mechanisms and identifying patients with an increased cardiac mortality [8]. Increased sympathetic tone and decreased parasympathetic function result in increased strain on the heart and a lower threshold for ventricular fibrillation, while increased parasympathetic activity protects the heart [9]. In 1992, Bigger et al suggested that it is in fact the ULF band that is the strongest predictor of mortality [10], but estimation of ULF power requires 24 hour ECG recording which requires high subject compliance, and is costly and time consuming, so not always feasible. Our study aims at determining tilt-table testing as a means of autonomic challenge could be used in place of prolonged-ambulatory recording, this would therefore be preferable.
Materials and Methods
Participants
Questionnaires were designed to collect data on general health; any current or past conditions or medications, in particular sleep disorders and sleep aids; nicotine, alcohol and tea usage; and shift patterns including a 24 hour sleep diary in order to determine whether each subject could be defined as a night worker or day worker, and to allow us to assess environmental light exposure and differences in job requirements. These questionnaires were distributed to porters and the returns assessed with suitable candidates invited to attend an appointment to the laboratory for recording ECG. 60 initial replies were received including 28 day porters and 32 night porters. Appointments were kept with 58 porters, 56 of them had usable ECG traces, therein 29 night porters and 27 day porters. Blood pressure and heart rate readings for all of them could be analysed. Of these porters, hypertension, defined in line with the Knutsson study as having a systolic BP >160mmHg, a diastolic BP >90mmHg was found in one of the day porters, and controlled hypertension with medication in three of the night porters. Finally there were 25 day porters and 25 night porters available to analyse the data.
Study Protocol
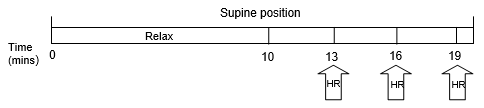
A 3 lead ECG was carried out using disposable, self-adhesive electrodes (Red Dot™ -2330; 3M Company, MN, USA) attached to the left and right forearms and right wrist, along with recording of ECG (TLC 9803; Kangtai Company, Beijing, China) for each subject for 20 minutes in the supine position. The measurements were recorded on a PC for offline analysis. The subject was given 10 minutes to relax before heart rate readings were made (M10-IT; Omron, Kyoto, Japan) at minutes 13, 16, and 19.
ECG artefacts such as misattribution of ‘R peak’ to another part of the signal leading to an ‘extra beat’ and an illegitimately short interval, or failure to detect an R peak leading to a ‘missed beat’ and an equally invalid long interval have a considerable impact on HRV estimation. Artefacts should therefore be edited out of the raw data accordingly. Ventilation was measured so that it could be taken into account in the HRV analysis if necessary in order to eliminate the confounding effects of any changes in breathing depth and rate in assessment of autonomic control of circulation. Mean heart rates were calculated for each subject in the supine position.
Candidates were also asked to complete Morningness- Eveningness questionnaires for us to identify any subjects who were clearly not well adapted to their working regime either by reporting a ‘feeling best’ time at a time when they should be sleeping according to their work schedule, (Figure 1) or excessive tiredness during waking periods. Age, sleeping time, shift work years, smoking and current drink could be acquired from the questionnaires, and BMI was calculated from reported height and weight.
Analysis of Heart Rate Variability (HRV)
Detrending the HRV
The detrending method was based on the ‘Smoothness Priors’ approach and operates like a time-varying finite-impulse response high-pass filter. This was performed to detrend the HRV before analysing the power spectrum. In this study, the cut-off frequency was 0.022 Hz.
Parameters of HRV in Time domain
Three parameters were calculated from the time domain HRV recordings: the mean interpulse interval (mean NN), the standard deviation of the interpulse intervals (SDNN), the square root of the mean squared differences of successive interpulse intervals (RMSSD).
Power spectrum analysis for HRV
Spectral power analyses were calculated in accordance with previously published standards (20), yielding the three frequency domain measures: very low frequency (VLF) power at 0-0.04 Hz , low frequency (LF) power at 0.04-0.15 Hz and high frequency (HF) power at 0.15-0.4 Hz in the HRV. Power frequency (Hz) was converted to s2 by Welch’s periodogram analysis employing 1024 points window width and window overlap of 512 points, using in-house software. The power of the low and high frequency components was computed as the integral of the bands. The ratio of the logarithm of the LF to HF power was also calculated.
Statistical Analysis
Analysis was carried out using a statistics package (SPSS 13.0, IL, USA). Variables on HRV during supine within each shift were compared by paired-t test. For convenience, all data are presented as means ± SD. Two-tailed P-values of less than 0.05 were regarded as significant.
Results
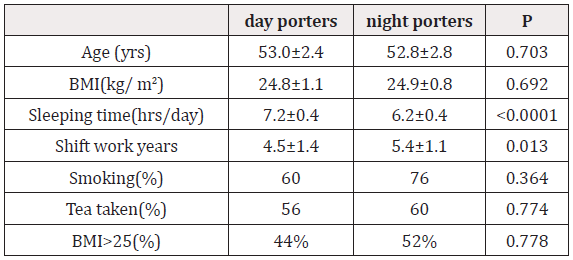
The characteristics of porters was described in (Table1). Referring to (Table1), there was no statistically significant difference between groups for nicotine or alcohol consumption, but tea intake was statistically higher (P<0.001) in the night porters based on questionnaire results. There was also no significant difference in mean age and BMI between the night and day groups, and though the mean age in the night porter group was found to be significantly higher based on the results of the pilot questionnaire (P<0.035), this was also not the case in the sample tested.
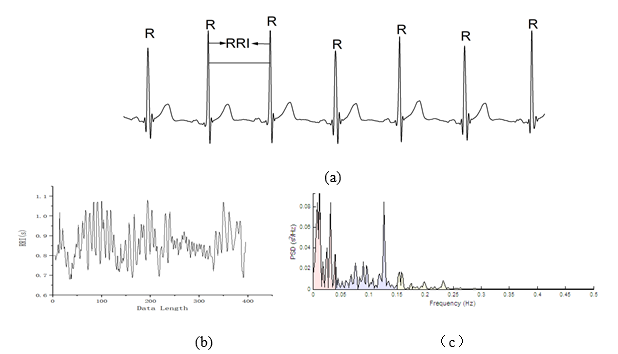
Waveforms of 5- minute segments of ECG signals from a representative subject were shown in (Figure 2(a)). The line is the ECG signal and RRI is the interval of the successive R waves. The RRI signals were shown in (Figure 2(b)), and its power spectrum density (PSD) were shown in (Figure 2(c)). The line in peach is the PSD of the VLF, the line in blue is the PSD of LF and the line in yellow is the PSD of HF.
There was a significant difference between the mean reaction of night porters and day porters with respect to heart rate (P<0.037), and high frequency power in HRV (P<0.043). The night porters on average showed a smaller increase in heart rate, and a greater reduction in HF power compared with the day porters.
Sleep disorders were reported in 2 day porters, but this was found to be in one porter who had until recently worked nights still working 2 nights per month, and in one day porter who became a caretaker on call during the night and though he is rarely woken says that he feels like he is “waiting for something to happen”, both complications only revealed through our methods asking for details of shifts worked presently and previously, that would not have been found in the previous studies (Figure 3). Sleep disorders were also reported in 7-night porters. Sleeping aids were reportedly used by the same 2-day porters, and 4 of the night porters. Based on answers to the Morningness-Eveningness questionnaire, one night porter reported a ‘feeling best’ time of 3am and the time that he feel most tired and in need of sleep as 10 am implying adaptation to the night shift. The other 2 night porters seemed more suited to day work though described themselves as ‘evening types’ as opposed to ‘morning types’.
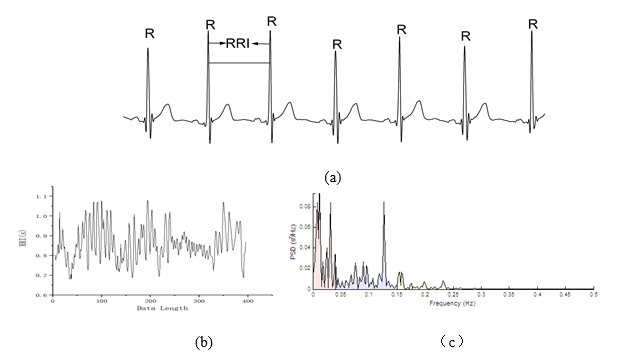
Figure 3: Boxplots for changes in a) heart rate and b) HF power following with night porter data displayed on the left and day porter data on the right in each example.
Other common symptoms were dry skin, hair or dandruff in 8 of the night porters, and just one-day porter. Hypertension or use of antihypertensive medication was reported in 4 night porters and one day porter, while one night porter reported a 1983 heart bypass, and another, type II diabetes and pancreatic failure.
Conclusions
We expected that if a night worker is adapted to night work, the normal LF: HF rhythms should be reversed. They will have an increased LF: HF ratio during the night when they are on shift, and so a decreased ratio during daytime testing. If the porters are not adapted to night work, an increased LF: HF ratio could still be observed due to stress and increased sympathetic drive. We observed no significant difference in LF: HF ratio between the night and day porters. We saw night-day group differences in heart rate and HF power, which could reflect autonomic dysregulation due to circadian disruption. The night porters responded less strongly with respect to heart rate, showing a significantly smaller increase on average, which could reflect a reduced responsiveness of the system imposed changes, which can be considered a sign of ‘poorer health’ or ‘lesser resilience’ due to an impaired ability to adapt to the environment, an idea across much of the literature linking reduced heart rate variability to increased risk of cardiovascular incidents. Finally the night group showed a greater mean reduction in high frequency power than the day porters, implying a greater mean reduction in parasympathetic input. Reduced parasympathetic drive is sometimes considered pathological due to the protective influence of the parasympathetic system on the heart. No significant differences were found between the night and day porter groups for LF:HF despite the difference found in HF power, and no significant differences in LF power were found in parallel to the HF differences to explain the lack of change in the ratio. This could be explained by the small parasympathetic contributions to LF power, an argument against LF as a good indicator of sympathetic drive. These findings could have prognostic significance in identifying asymptomatic patients thought to be at risk of CVD in order to offer advice regarding lifestyle changes including weight loss, smoking cessation, nutrition, exercise, or prophylactic aspirin use. There could also be value in the results providing information on an individual’s suitability for night work.
As far as not seeing any difference in LF:HF, it could be that our hypothesis was incorrect and that night shift work doesn’t affect LF:HF, or there may have been other reasons for not seeing a difference between groups including incomplete adaptation to night shift, stress or other confounding factors that we failed to pick up on including socioeconomic status, social background and previous employment, or differences in the demands of the porters in various colleges. HRV has also been seen to be affected by age, sex, smoking and exercise in healthy subjects, with reduced variability in the elderly and smokers, improving on smoking cessation, and increased variation in individuals who exercise, so in addition to our collection of data on current smoking habits, previous nicotine use and current and previous exercise could be valuable data. Our methods for defining night work and day work allowed us to see the great inter-group variability with respect to the length of time the night porters had been working nights or whether the day porters had ever worked nights, and if so the length of time since they stopped. With a larger sample size, groups could either have more strict inclusion criteria ie. day porters to have never worked nights; or more groups could be investigated to look at the extent of effects with respect to period of time working nights, and whether risks are reduced and to what extent when someone stops working nights in the same way they are reported to worsen in those who switch from days to nights [11]. It could also be interesting to compare results across colleges, particularly central colleges versus those which are located further from town; or female versus male-dominated colleges on the basis of differences in noise levels, number of visitors to the lodge, or number of disruptions. Additionally, our sample did not show significant differences in smoking or BMI between the day and night groups which contradicts previous findings, so it’s possible that either our small sample was an inadequate representation of the porter population, or that the Oxford college porter population is significantly different to those that have taken part in previous studies. Additionally, BMI was calculated from self reported height and weight which may have been inaccurate approximations, so in future it may be better to weigh and measure subjects ourselves to avoid bias.
Exposure to light at night, something seemingly inevitable for night workers, is known to alter melatonin secretion, which follows a circadian rhythm controlled by the SCN, so profiling via blood, urine or salivary assays could aid investigation into whether the night porters are adapted to their shift pattern. It is also thought to play a role in modulation of autonomic activity with administration of endogenous melatonin having been shown to decrease heart rate pre-election period (PEP), PEP being a measure of cardiac sympathetic activity. Relatively recent research also dispels previous thinking that melatonin receptors are only present in the brain and retina with autoradiographic studies in birds showing their presence in the heart, and similar studies in humans showing the MT2 subtype to be located in the left ventricle, aorta and coronary arteries, so melatonin could well cause physiological effects directly in the cardiovascular system, and disruption to its circadian rhythms of secretion could in turn disrupt control in the cardiovascular system. We expected to see an increased LF:HF ratio, which is seen to represent increased sympathetic drive, or reduced parasympathetic drive, and may therefore increase strain on the heart, so efforts to reduce the effect are important. It may therefore be useful to avoid photo-entrainment as demonstrated by several groups who provided dark glasses to night workers to block out morning light, though they have been argued as being incompatible with driving. Sasseville et al showed that orange-lens blue blocker glasses could impede the capacity of bright light to suppress melatonin production [12], so wearing these on the journey home from a night shift could be a means to allow night workers to adapt to their working rhythms so that they can get better quality sleep at the appropriate time and be more alert and presumably less stressed during working hours. It’s possible that a small intervention such as this could have the potential to make a difference in closing the gap between the incidence of cardiovascular disease in night workers and day workers, so a possible future direction for this study would be to test night porters and assess their risk for cardiovascular disease, introduce the blue-blockers as an intervention with a control group wearing blue-lens glasses and then reassess risk with the hope of finding improvements. Additional measures could also be used to assess risk of cardiovascular disease including ECG assessment to identify abnormalities, perimetry or capimetry, assays of risk biomarkers, and greater emphasis on reported risk factor analysis, using an algorithm such as QRISK, the Framingham Risk Score, or ASSIGN, scoring methods used to identify those at high risk of CVD [13]. Other measures of the extent to which the porters are adapted to the night shift could also be useful, from the previously mentioned melatonin profiling, to actigraphy along with more long-term circadian rhythm diaries and self-reports of sleep quality.
HRV is commonly measured over 5 minute periods in controlled laboratory conditions, and several studies have shown decreased HRV as measured over short time scales to act as a predictor for morbidity and mortality [14]. In normal subjects, an increased LF:HF ratio is seen during the day due to increased sympathetic drive, and this is reversed in the night.
The circadian clock, or suprachiasmatic nucleus (SCN) receives input from melanopsin containing- intrinsically photosensitive retinal ganglion cells with a peak absorption frequency of 484nm, corresponding to blue light. Porters travelling home from a night shift will likely be exposed to light at this frequency, which acts as a powerful entraining cue, therefore preventing the desirable avoidance of a ‘normal’ circadian cycle. The SCN projects to other hypothalamic nuclei, with a role in modulating autonomic output such as that to the heart, which could explain the findings that night shift work could increase heart rate and reduce heart rate variability.
We avoided a limitation of previous studies, where the definition of shift work has been the subject’s answer ‘yes’ or ‘no’ to ‘Do you have shift or weekend work?’ leading to variability in the night and day categories by obtaining details of shift times to determine those who regularly participate in night work.
In the Knutsson’s study 3, shiftwork is defined as work including hours beyond ‘daytime’ (6am-6pm), and nightwork is work that includes hours between 10pm-6am, nightwork is being a subset of shift work. In our study, a ‘night worker’ is to be defined as someone who works more than 50% of their shifts as nights, and a ‘day worker’ as someone who never works nights.
Acknowledgements
To the best of my knowledge, this study provides the first evidence for HRV differences between day and night workers doing the same job following imposed autonomic challenge. Further study is warranted to look for possible further differences using methods described above, and to test possible interventions that could reduce risk for night workers.
Authors’ Contributions
Guohua Lu contributed to the conception of the study; Juanjuan Xia performed the experiment, the data analyses and wrote the manuscript; Zhao Li contributed significantly to analysis and manuscript preparation; Tao Lei performed the analysis with constructive discussions.
Data Availability
The data used to support the findings of this study are available from the corresponding author upon request.
References
- Marie AJ, Anne HG, Jesper K, Kirsten NN, Marie H (2016) The effect of the number of consecutive night shifts on diurnal rhythms in cortisol, melatonin and heart rate variability (HRV): a systematic review of field studies. Int Arch Occup Environ Health 89(4): 531-545.
- Gerben H, Nidhi G, Karin IP, Natasja L, Wilhelmina I, et al. (2018) Shift work is associated with reduced heart rate variability among men but not women. Int J Cardiol 258: 109-114.
- Knutsson A, Hallquist J, Reuterwall C, Theorell T, Akerstedt (1999) Shift work and myocardial infarction: a case-control study. Occup Environ Med 56(1): 46-50.
- Yadav RL, Yadav PK, Yadav LK (2017) Association between obesity and heart rate variability indices: an intuition toward cardiac autonomic alteration–a risk of CVD. Diabetes Metab Syndr Obes 10: 57-64.
- Amirian I, Toftegard AL, Rosenberg J (2014) Decreased heart rate variability in surgeons during night shifts. Can J Surg 57(5): 300-304.
- Sanae O, Yukiko M, Toshio K (2017) The Influence of a 120-minute Nap on Physical Activity and Subsequent Sleep: Impact of Nighttime Napping during a simulated Night Shift. J Science Labour 93(3): 67-79.
- James BB, Melannie A, Pallavi B, Jameson S, James W, et al. (2019) Shift Work and Heart Rate Variability Coherence: Pilot Study Among Nurses. Appl Psychophysiol Biofeedback 44(1): 21-30.
- Lombardi F (2002) Clinical implications of present physiological understanding of HRV components. Cardiac Electrophysiology Rev 6(3): 245-249.
- Kleiger RE, Stein P, Bigger J T (2005) Heart rate variability: measurement and clinical utility. Ann Noninvasive Electrocardiol 10(1): 88-101.
- Bigger JT, Fleiss JL, Steinman RC, Rolnitzky LM, Kleiger RE, et al. (1992) Frequency domain measures of heart period variability and mortality after myocardial infarction. Circulation 85(1): 164-171.
- Biggi N (2008) Depression and coronary heart disease: recommendations for screening, referral, and treatment. Chron Int 25(2): 443-454.
- Sasseville A, Paquet N, Sévigny J, Marc H, (2006) Blue blocker glasses impede the capacity of bright light to suppress melatonin production. J Pineal Res 41: 73-78.
- Scott IA (2009) Evaluating cardiovascular risk assessment for asymptomatic people. BMJ 338 :a2844.
- Chen ST, Lin LY, Baker D, Peter LS, Ming FC, et al. (2008) Elevated blood pressure, decreased heart rate variability and incomplete blood pressure recovery after a 12-hour night shift work. J Occup Health 50(5): 380-386.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.