Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Overview On Effectiveness of Abdominal Posterior Mesh Rectopexy Incomplete Rectal Prolapse
*Corresponding author: Muslihudin, Department of General and Laparoscopic Surgery, Saidu Group of Teaching Hospitals Swat, Pakistan.
Received: January 18, 2021; Published: February 14, 2022
DOI: 10.34297/AJBSR.2022.15.002121
Abstract
Objective: This study was conducted to gauge the clinical outcome of abdominal mesh rectopexy in Khyber Teaching Hospital, Peshawar, Pakistan.
Study design: an observational study.
Place and Duration of study: The present study was conducted in Surgical Department, Khyber Teaching Hospital, Peshawar from September 2019 to August 2021.
Methodology: A total of 17 patients, 11 male, and 6 females with complete rectal prolapse were included in this prospective study. Pre-operative assessment of the patients included history taking, thorough physical examination, DRE with a meticulous assessment of the sphincter tone, and colonoscopy. Abdominal Posterior mesh rectopexy was done in all patients using synthetic polypropylene mesh.
Results: Out of the total 17 patients, 5 presented with incontinence and 7 with chronic constipation. Incontinence improved over time in all 5(100%) patients while 1(5.88%) patient with preexisting constipation complained of aggravation and 3 patients (17.64%) developed new-onset constipation postoperatively. Bleeding was noted in 2(11.7%) of patients. Surgical site infection occurred in 1(5.88%) patient. No recurrence was found after 2 years of follow-up.
Conclusion: Abdominal posterior mesh rectopexy can be a safe and effective procedure for complete body part prolapse of the rectum particularly in patients with incontinence. It improves incontinence with a marginal risk of accelerating constipation.
Keywords: Rectal Prolapse; Abdominal Rectopexy; Mesh Rectopexy
Introduction
Complete rectal prolapse is the protrusion of the circumferential full-thickness body part wall through the anal canal. It is a debilitating condition that affects patients of almost all age groups. It’s often related to feculent incontinence. Description of body part prolapse dates back to the time of yore and is delineated in Ebers papyrus in 1500 BC [1]. The exact pathologic process is not clear with a large number of proposed causation theories. Moschcowits suggests that the pathologic process of body part prolapse starts with the anterior aspect of the wall herniating through the defect within the girdle fascia [2]. Broden and Snellman by using cine defecography found that body part prolapse is owing to the circumferential intussusception of the body part through the anal canal [3]. Over a hundred procedures are delineated to treat body part prolapse with an imperfect understanding of the disorder and the absence of a perfect procedure to treat this condition. The procedures for body part prolapse can be divided into two classes i.e., Abdominal and Perineal [4]. Perineal procedures are related to less morbidity and mortality, however, there is an increased rate of recurrence as compared to abdominal procedures. Perineal procedures are reserved only for elderly and high-risk patients. They can also be used in young because it is often performed under regional anesthesia [5]. This study is geared towards evaluating the results of abdominal posterior mesh rectopexy.
Methodology
This prospective observational study was conducted at the surgical department of Khyber Teaching Hospital, Peshawar from 1st September 2019 to 31st August 2021 after taking approval from the institution’s ethical committee. Total no of 17 patients were included with 11(64.7%) male and 6(35.29%) female. An age group from (21- 69 years) was selected with a mean age of 45 ± 6 years. Patients of all ages and gender with complete rectal prolapse were part of the study. Patients with Recurrent prolapse operated outside the aforementioned institution and admitted with complications or unfit for surgery are excluded from the study. Informed consent was taken from all of the patients. Baseline investigations and bowel preparation was performed in all patients preoperatively. All patients underwent abdominal posterior mesh rectopexy by a single surgeon and were assessed for any complication postoperatively. A follow-up at 6 weeks, 3 months, 6 months, 1 year, and 2 years was done.
Surgical Technique
Abdominal Posterior Mesh Rectopexy: Patient is placed in Lloyd-Davis position and on table catheterization is performed. The rectum is mobilized posteriorly up to the pelvic floor preserving nerves and ureter. Lateral ligaments are preserved in all patients. A pre-formed polypropylene mesh is applied in the presacral space and stitched to the sacrum posteriorly with the help of a nonabsorbable Prolene 2/0 suture. The mesh is placed in such a way to encircle the 3/4th circumference of the rectum and fixed with 2/0 Prolene in a seromuscular fashion.
Results
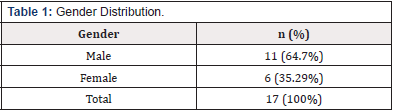
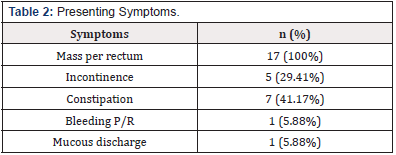
A total of 17 patients, 11(64.7%) male and 6(35.29%) female with age group from 21 to 69 years and a mean age of 46-7 years were included (Table 1). A sensation of mass per rectum was the most common presenting symptom among all 17(100%) patients. Constipation in 7(41.17%) and Incontinence in 5(29.41%) was the next common presenting complaint (Table 2).
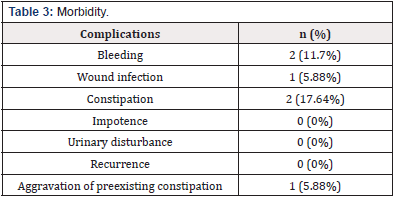
No recurrence was found after two years of follow-up in all the cases. Incontinence recovered after surgery in all the 5(100%) cases presented, while only 3(17.64%) patients developed newonset constipation postoperatively and only 1(5.88%) patient with preexisting constipation had aggravation of the symptom (Table 3). No mortality was noted during the study.
Discussion
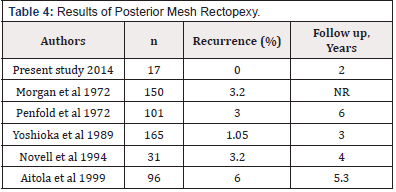
The range of surgical options available to treat rectal prolapse poses the question about the best procedure. However abdominal rectopexy retains the best reputation among Surgeons [6]. Rectal prolapse is said to be a disease of elderly females in western literature [7]. We noted a male predominance in our study 11/17(64.7%), male patients, as compared to 6/17(35.29%) female. The primary outcome measure in this study was a recurrence of full-thickness rectal prolapse which is clinically the most relevant measure. Recurrence was outlined because of the circular protrusion of body part i.e. mucous membrane through the anal canal and is evaluated by history, clinical examination [8]. Secondary outcomes were morbidity, mortality, length of initial hospital stays, constipation, and fecal incontinence. Traditionally rate of recurrence is the most significant factor to decide the procedure to be performed. Recurrence of 0-12% has been noted in different studies after posterior abdominal mesh rectopexy. In this study, we found no recurrence after two years of follow-up. A comparison of different studies in terms of recurrence is given in (Table 4).
Other minor complications noted in this study include minor bleeding 2(11.7%) which was due to the stitches taken while fixing the mesh to the sacrum and was controlled by gentle compression for a few minutes. Constipation is the most common complication after abdominal rectopexy [9]. It may occur as new-onset constipation post-surgery or it may aggravate an already existing constipation postoperatively [10]. We noted 3(17.64) new-onset constipation post-surgery which were treated with laxatives to the patient satisfaction. While out of 7(41.17%) patients presented with constipation preoperatively, only 1(5.88%) patient developed aggravated constipation post rectopexy. Incontinence was the initial presentation apart from rectal prolapse in 5 patients and all of them got cured after abdominal rectopexy. No patient developed impotence and urinary disturbance in this study after abdominal rectopexy. No mortality was noted in this study.
Conclusion
Abdominal posterior mesh rectopexy is a safe procedure in patients who can tolerate laparotomy. It has the lowest or no recurrence rate especially in patients presenting with fecal incontinence. Patients improved after surgery regarding incontinence, with a slight risk of constipation postoperatively.
Limitations
Rectal prolapse is not a very common condition hence the size of this non-randomized study was small with a short period of follow-up. A larger randomized study with a longer duration of follow-up is required to get conclusive evidence.
Ethical Approval
Ethical approval was granted before the execution of the study.
Patients’ Consent
Oral consent was obtained before the participation in the study.
Conflict Of Authors
No conflict of authors.
Authors’ Contribution
Muslihuddin: write the initial draft and conceptualized the study; Shahzeb Khan: Methodology part; Zarka Ahmad: Data analysis; Fazal Rabbi and Tawseef Ahmad: Revise and editing, Syed Mujahid Shah: Project administration.
References
- Ballantyne GH (1991) The Historical evolution of anatomic concepts of rectal prolapsed Semin Colon Rectal Surg. 2:170-179.
- Moschowitz AV (1912) The pathogenesis anatomy and cure of prolapse of the rectum. Surg Gynecol Obstet 15: 7-21.
- Broden B, Snellman B (1968) Procidentia of the rectum studied with cineradiography. A contribution to the discussion of causative mechanism. Dis Colon Rectum 11(15): 330-347.
- Iqbal Z, Nasir IU, Iftikhar M, Ullah A, Ahmad S, et al. (2014) ABDOMINAL MESH RECTOPEXY: OUR EXPERIENCE AT HAYATABAD MEDICAL COMPLEX PESHAWAR. KJMS 7(2): 325.
- Akira Tsunoda, Naokuni Yasuda, Noboru Yokoyama, Goichi Kamiyama, Mitsuo Kusano (2003) Delorme’s procedure for rectal prolapsed: clinical and physiological analysis. Dis Colon rectum 46(9):1260-1265.
- K Azimuddin, I T Khubchandani, L Rosen, J J Stasik, R D Riether, et al. (2001) Rectal prolapsed: a search for the “best” operation. Am Surg 67(7): 622-627.
- Bashar S, Anthony MV (2008) Abdominal approaches for rectal prolapsed. Clin Colon Rectal Surg 21(2): 94-99.
- Y Kariv, C P Delaney, S Casillas, J Hammel, J Nocero, et al. (2006) Long term outcomes after laparoscopic and open surgery for rectal prolapsed. Surg Endosc 20(1): 35-42.
- Bashar Safar, Anthony M Vernava (2008) Abdominal approaches for rectal prolapse. Clinics in Colon and rectal surgery 21(2): 94-99.
- A J Brown, J H Anderson, R F McKee, I G Finlay (2004) Strategy for selection of type of operation for rectal prolapsed based on clinical criteria. Dis colon Rectum 47(1): 103-107.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.