Review Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
About One Case: Afebrile Rheumatic Fever in a Clinic in Sincelejo
*Corresponding author: Ettlingert Blas Rico Díaz, Medical Student, Universidad de Sucre, Colombia
Received:July 19, 2022; Published: August 09, 2022
DOI: 10.34297/AJBSR.2022.16.002291
Abstract
Acute rheumatic fever (RFA) is the result of an autoimmune response to pharyngitis caused by infection with group A streptococcus, with rheumatic heart disease (RHD) being one of its main complications, as well as a notable cause of morbidity and mortality in poor settings around the world. Although it has improved in the understanding of the pathogenesis of the disease in recent years, diagnostic approaches have not led to the improvement of its diagnosis being the Jones criteria introduced in 1944 and revised in 2015 still in force, on the other hand, penicillin has remained the fundamental pillar throughout the decade, and it has not been shown that another treatment is better.
Below is a case of atypical rheumatic fever in a 9-year-old female patient from Ovejas, Sucre Colombia.
Keywords: Rheumatic fever, Korea, Mitral Valve Regurgitation, Colombia
Introduction
Rheumatic fever (RFA) is a severe multifocal autoimmune sequelae of group A streptococcal infection (GAS), presenting with a combination of signs and symptoms, which are performed in the presence of 2 major criteria or 1 major and 2 minor with evidence of recent GAS infection used as part of the diagnosis according to Jones criteria, RFA leads to a disease that is characterized by various combinations of joint pain and inflammation, heart valve failure with potential for secondary heart failure (rheumatic heart disease refers to long-term heart damage caused by a single severe episode or multiple recurrent RFA episodes), chorea, cutaneous, subcutaneous manifestations and fever; Since 1944, the diagnosis of RFA has been based on the Jones criteria, which are reviewed periodically. The 2015 revision of Jones’ criteria underscores the importance of knowing the epidemiological status of his own region with up-to-date data, however, in Colombia the data are outdated [1,2].
Clinical Case
A 9-year-old female patient from Ovejas-Sucre, who was evaluated in the pediatric emergency department on February 21 in the company of the mother, she reports clinical picture that began on February 20, presented by episodes of sudden onset with arrhythmic and brief involuntary choreal movements in the left hemibody, more muscle contractions with deviation of the labial commissure to the left (Sydenham’s Korea), accompanied by a moderate mitral murmur 3/6 on the Levine-Harvey scale, without febrile episodes from the moment of admission, the mother denies that her daughter has lost consciousness and respiratory symptoms.
Background
Pathological: Denies recent pharyngotonsillitis infections.
Schoolchildren: In the fourth grade of primary school, with a slow pace of learning, difficulties in reading – mathematics.
No pathological family history.
Prenatal and Perinatal (Unknown).
Physical examination found vital signs. HR: 88 bpm FR: 18 rpm T: 36.5°C Blood pressure: 110/80 mm Hg Weight: 22 kg. SatO2: 98%, in good general condition with reactive pupils, good eye contact, preserved cranial nerves, fluid language, coherent,adequate understanding of orders, preserved trophism, nonclonus, non-babinski, plus independent gait with motor dyspraxia, paediatric Glasgow scale: 15.
As an important finding, it is highlighted that 1 month ago he presented a febrile picture, associated with soft tissue infection; current laboratory tests found elevated ESR (39 mm/h), elevated antistreptolysin (ASTO) (800 IU/mL), simple and contrasted brain MRI at normal limits, and doppler echocardiogram evidencency rheumatic mitral valve disease and moderate mitral retral regurgitation.
For the hemicorea presented, he received valproic acid with a gradual decrease in his symptoms, treatment with enalapril, furosemide and spironolactone was indicated plus treatment with penicillin and subsequent prophylaxis with amoxicillin due to the findings found in the echocardiogram.
Discussion
Rheumatic fever is a chronic systemic inflammatory disease consisting of a series of joint, cutaneous, cardiovascular and neurological conditions, resulting from an infection with Landfield group A beta hemolytic streptococcus, mainly due to encapsulated strains highly immunogenic resistant to phagocytic processes. The pathological process of the disease is based on an exaggerated immune response to the infectious agent. After a streptococcal pharyngeal infection, multiple specific bacterial epitopes are released from the germ that mimic the components of the human body, gestating an autoimmune process in the organs and systems described above [3,4].
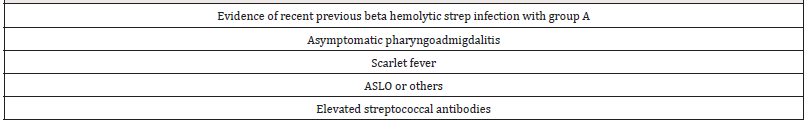
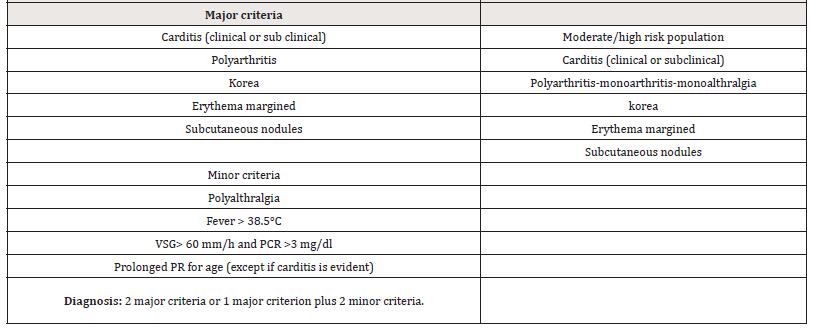
Rheumatic fever is a disease, in essence, of childhood and adolescence, occurring mainly in the population aged between 5 and 20 years, with peaks of incidence at 10 years, in 0.3-3% of patients who presented strep throat; a slight predominance has been reported in females and in patients from families and communities at high social risk. The classic presentation of the disease has the appearance 2 to 3 weeks prior of a streptococcal pharyngotonsillitis with the respective tonsillar erythema, presence or not of exudate, regional adenopathies, fever, dysphagia, petechiae on the palate, and sometimes scarlet fever. Subsequently, the disease debuts with a clinical picture consisting, initially, of fever, inflammation and joint pain, anorexia, fatigue, anemia and affectation of the general condition. Considering the multiple and non-specific clinical manifestations of the disease, for its diagnosis the Duckett Jones criteria were established (Table 1) that relate signs and symptoms with evidence of a recent streptococcal infection; however, atypical presentations are highly frequent, so the disease should be suspected in patients with high fever, accelerated erythrocyte sedimentation rate (ESR), positive C-reactive protein (CRP) and electrocardiographic alterations [4-6](Table 2).
In addition to the absence of a specific laboratory test or pathognomonic sign of the disease, another drawback in the approach to rheumatic fever is the wide repertoire of differential diagnoses, since depending on the clinical manifestations, juvenile arthritis, reactive arthritis secondary to infectious diseases, Lyme disease, should be considered. collagenosis, sarcoidosis, sickle cell disease, gout, endocarditis, myocarditis, Kawasaki disease, lupus choreas and other non-rheumatic choreas, etc. In relation to the evolution of the disease, it is cardiac involvement, especially the degree of valvular damage, which will determine the long-term prognosis, since this manifestation becomes chronic; Contrary to arthritis, erythema and chorea that are self-limiting. Mortality from rheumatic fever is uncommon and is associated with complications in the acute process [3-5].
The treatment of rheumatic fever is based on several strategies; eradication of the agent, symptomatic treatment and prophylaxis. As for the eradication of streptococcus, penicillin is the antibiotic of choice, first generation cephalosporins and macrolides have also been considered with the disadvantage of the appearance of resistance to both groups. In relation to clinical manifestations, arthritis of rheumatic fever responds excellently to salicylates, in addition corticosteroids are also used to mitigate inflammatory processes and severe heart conditions.
Primary prevention is based on timely treatment of pharyngotonsillitis; and the secondary one aims to prevent recurrent events in patients with acute rheumatic fever, usually benzathine penicillin is used [3].
Conclusion
It is important to bear in mind that rheumatic fever is a serious immunological disorder that mainly affects vulnerable populations and high social risk affecting especially children, therefore, it is up to all health personnel, not only doctors or specialists, to know the clinical presentation of this disease, given that the jones criteria provide the opportunity for a timely diagnosis which would generate an early treatment to patients, thus improving their quality of life and prognosis, at the same time as this way, seeks to avoid complications and mortality rates.
It should be noted that, the fairly broad symptomatology that usually occurs in these cases would help generate a clinical diagnosis, since there is no diagnostic test that can corroborate the pathology. Emphasizing the prevention of this disease can greatly reduce infections caused by streptococcus group A thus avoiding permanent sequelae [7].
References
- Carapetis J, Beaton A, Cunningham M, et al. (2016) Acute rheumatic fever and rheumatic heart disease. Nat Rev Dis Primers 1-24.
- Marino A, Cimaz R, Pelagatti MA, Giulia Tattesi, Andrea Biondi, et al. (2021) Acute rheumatic fever: where are we? An epidemiological study in northern Italy. Front Med (Lausanne). 8: 621668.
- Antón López J, Mosquera Angarita J (2017) Rheumatic fever and post-streptococcal reactive arthritis. Journal of Integral Pediatrics 21(3): 196-206.
- Santamaría Díaz H, Gaytán G, Quiñónez Gálvez R M, Gómez Gómez M (2006) Rheumatic fever. Is it still a problem in children? About a case. Revista Mexicana de Pediatría 73(3): 127-131.
- Ros Viladoms JB, Rheumatic fever (RF). Diagnostic and therapeutic protocols in pediatrics, undated 49-52.
- Montero Verdecia Delmis, Pompa Virelle C, Rondón Peña M, Figueredo Montero G, Álvarez Rondón (2020) Clinical-epidemiological characterization of rheumatic fever in children. Hermanos Cordové Hospital. First Virtual Congress of Basic Biomedical Sciences of Granma 1-13.
- Parra Calero AA, Ordoñez Toro AM, Castro Macías AM, Quinde Zambrano JM (2021) Rheumatic fever, particularities. Pole of Knowledge, 6(5): 836-843.




 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.