Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Activity of Oxidative Stress and Damage to Vascular Endothelium in Rats with Experimental Peritonitis Under Administration of NO-Syntase Inhibitors
*Corresponding author: EV Husakouskaya, Grodno State Medical University, Department of Pathophysiology named after D A Maslakov, Belarus, Grodno, Gorkogo Street, Belarus.
Received:May 11, 2022; Published:June 03, 2022
DOI: 10.34297/AJBSR.2022.16.002235
Abstract
Background: The high lethality in peritonitis and the lack of data on the role of various NO-synthase isoforms in its pathogenesis
suggests the advisability of the research to study the effects of NO-synthase (NOS) inhibitors.
Objective: The aim of the research was to study the activity of oxidative stress and state of vascular endothelium in rats with
experimental peritonitis under administration of NO-syntase inhibitors.
Material and Methods: The research was carried out on male rats (n=72), divided into 4 series which were injected
intraperitoneally with 0.6ml/100g: 1st series (control)-0,85% NaCl; 2nd series (experimental peritonitis, EP)-15% fecal suspension;
3rd series (EP+L-NAME)-15% fecal suspension with intramuscular injection of Nώ-nitro-L-arginine methyl ester, L-NAME (10mg/
kg); 4th series (EP+AG)-15% fecal suspension with intramuscular administration of aminoguanidine, AG (15mg/kg). The content of
nitrite/nitrates (NOx), malondialdehyde (MDA) and reduced glutathione (GSH) in blood plasma of rats, the quantity of circulating
endothelial cells (CEC) in blood were analyzed in half a day, 1 day and 3 days of EP.
Results: An increase in the level of NOx and MDA, a decrease in [GSH] in blood plasma, an increase in amount of CEC in the blood
of rats with EP were detected. Unidirectional changes, however, to a greater extent, were observed in EP under administration of
L-NAME. The administration of AG resulted in decrease in level of NOx and MDA, an increase in [GSH] in blood plasma, a decrease in
the amount of CEC in blood.
Conclusion: The course of acute EP was characterized by significant increase in level of NOx, development of oxidative stress
and damage to endothelium of blood vessels. The administration of non-selective NOS inhibitor, L-NAME, aggravated the severity of
changes in EP, that may be explained by inhibition of endothelial NOS with progression of microcirculatory disorders. The corrective
effect of AG in EP was manifested by a decrease in [NOx], oxidative stress activity and degree of damage to vascular endothelium,
which may be a consequence of the suppression of cytotoxic nitric oxide overproduction.
Keywords: Experimental peritonitis, Nitrite/Nitrates, Oxidative stress, Endothelium, L-NAME, Aminoguanidine
Abbreviations: NOS: NO-synthase; EP: Experimental Peritonitis; L-NAME: Nώ-Nitro-L-Arginine Methyl Ester; AG: Aminoguanidine; NOx: Nitrite/Nitrates; MDA: Malondialdehyde; GSH: Reduced Glutathione; CECc: Circulating Endothelial Cells; BP: Blood Plasma
Introduction
Diffuse peritonitis continues to be an unresolved problem of urgent surgery, which is associated with high lethality, reaching 85-90% with the development of multiple organ failure and septic shock [1], and may be due to the inferiority of pathogenetic therapy. There are literature data on the participation of various biologically active molecules in the pathogenesis of inflammation, among which is nitric monoxide (NO), formed from the amino acid L-arginine under participation of inducible and constitutive isoforms of NO synthase (NOS). The ambiguity of the NO properties: pro- and antioxidant, pro- and anti-inflammatory, pro- and antiadhesive [2] may be associated with changes in the activity of various NOS isoforms. In turn, insufficient knowledge of the role of NOS isoforms in the inflammatory process in the abdominal cavity necessitates a detailed pathogenesis of peritonitis. The purpose of the study was to research the severity of oxidative stress and the state of the vascular endothelium in rats with acute experimental peritonitis under administration of NO-synthase inhibitors.
Material and Methods
Experiments were carried out on outbred male rats, 230- 250g (n=72). An inhibitor of the inducible isoform of NOS (iNOS), aminoguanidine (AG), and a nonselective NOS inhibitor, Nω-nitro- L-arginine methyl ester (L-NAME), were used in experiment. Rats, divided into 4 series, were injected intraperitoneally, 0.6ml per 100g of body weight, with: 1st series-0.85% sodium chloride solution (control), 2-4th series-15% filtered fecal suspension (experimental peritonitis, EP) [3,4]. After intraperitoneal injection rats of all series were injected intramuscularly, 0.5ml, with: 1st (control) and 2nd (EP) series-0.85% sodium chloride solution, 3rd series (EP+L-NAME)-L-NAME at dose of 10mg/kg (Sigma, USA), series 4 (EP+AG)-AG at dose of 15mg/kg (Sigma, USA). The level of stable NO metabolites, nitrite/nitrates (NOx), was determined in blood plasma (BP) using the Griess reagent and cadmium on a SOLAR PV 1251C spectrophotometer [5]. The severity of oxidative stress was assessed by the concentration of a secondary product of lipid peroxidation (LPO)-malondialdehyde (MDA) and an indicator of antioxidant protection-reduced glutathione (GSH) in the BP of rats. The content of MDA was determined by measuring the extinction of a solution containing a pink-colored trimethyl complex of MDA with thiobarbituric acid, and the concentration of GSH was determined using trichloroacetic acid and Ellman’s reagent on a SOLAR PV 1251C spectrophotometer [6]. The study of the state of vascular endothelium was carried out by counting the number of circulating endothelial cells (CEC) of the blood in a hemocytometer [7], under light microscopy using a Micromed 3 var 3-20M microscope (China), equipped with plan achromatic lenses and a RisingCam video camera E3CMOS 20000KPB” (China). Statistical data processing was performed using the Statistica 10.0 program for Windows (StatSoft, Inc., USA) after testing for normal distribution (Shapiro-Wilk test) using the nonparametric Kruskal- Wallis test and post hoc comparisons using the Dunn test; data are presented: Me (LQ; UQ), where Me is the median, LQ and UQ are the values of the lower and upper quartiles, respectively. Differences were considered statistically significant at p<0.05.
Discussion
Current international medical literature suggests that the aerococci have been found as human path-ogens causing a wide range of infections, such as UTIs and several invasive infections (bacteremia, infective endocarditis, spondylodiscitis, hip abscess, lymphadenitis, acute pyelonephritism peritonitis) and also soft tissue infections. The prevalence of Aerococcus urinae UTIs has been reported to be 0.2-0.8%, although in a 2015 study, a 4% prevalence has been observed [4].
Aerococcus urinae ‘s association to urinary tract infections is supported by a growing number of case reports [5-12]. The case reported by Higgins and Garg [12] presents many similarities to the case we describe in this article, since they both regard elderly patients with bladder neoplasms and multiple comorbidities. The conclusions derived are strongly supported by the retrospective, observational cohort study conducted by Sahu et al. [13].
The pathogenicity mechanisms of Aerococcus urinae include biofilm formation [2,14,15], human platelet aggregation [2,15] and cytotoxicity to human urothelial cells [15]. In a mouse model described by Gilbert et al. [16], Aerococcus urinae exhibits tropism for the kidney and causes histological inflammation and neutrophil recruitment to the kidney. These findings may help understand better its potential to act as an uropathogen.
Results and Discussion
As a result of the studies, it was found that the development of EP was characterized by an increase in the content of NOx in BP after half a day-5.6 times (p<0.01), after 1 day-6.6 times (p<0.01), after 3 days-4 times (p<0.01), indicating a significant increase in the production of NO by iNOS, which, as it’s known, produces NO in micromolar concentrations after stimulation by bacterial antigens and pro-inflammatory cytokines, and reflects the high intensity of the inflammatory process course [8] (Table 1).
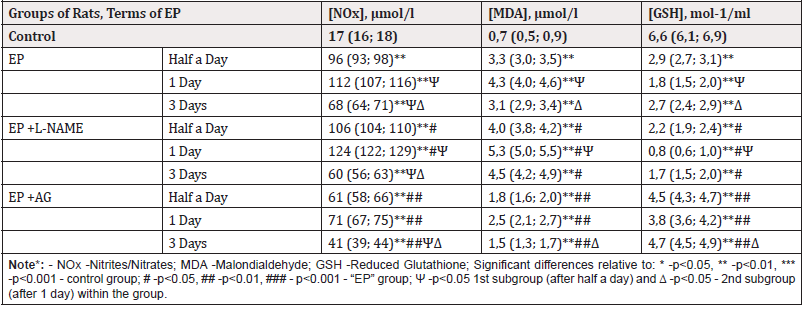
Table 1:Nitrite/nitrate concentration and parameters of prooxidant-antioxidant state in rats with experimental peritonitis (EP) and separate use of NO-synthase inhibitors - L-NAME and aminoguanidine (AG), Me (LQ; UQ).
The administration of L-NAME resulted in increase in [NOx] in the BP of rats with EP after half a day and 1 day (p˂0.05), compared with the values in EP without its use, which may be associated with the progression of microcirculation disorders and alteration under suppression of endothelial NOS and additional stimulation of iNOS by pro-inflammatory cytokines. In rats with EP and administration of AG, on the contrary, a decrease in [NOx] in BP was detected, compared with the values in EP without its administration, which may be due to inhibition of iNOS [9]. Along with an increase in the level of NOx in rats with EP, an increase in the concentration of the lipid peroxidation product-MDA in the BP was observed in half a day-4.7 times (p<0.01), in 1 day-6.1 times (p<0, 01), and in 3 days- 4.4 times (p<0.01), indicating the activation of oxidative processes in all the studied periods.
At the same time, there was a decrease in the content of GSH in BP in half a day, 1 day and 3 days-2.3 times (p<0.01), 3.7 times (p<0.01) and 2.4 times (p< 0.01), respectively, indicating a significant inhibition of antioxidant protection. Thus, the prooxidantantioxidant state in EP was characterised by the oxidative stress development. The change in the oxidative processes activity in rats with EP and administration of L-NAME in half a day, 1 day and 3 days was more significant than in EP without its use, an increase in the content of MDA-1.2 times (p˂0 .05), 1.2 times (p˂0.05) and 1.5 times (p<0.05), along with a decrease in the level of antioxidant GSH-1.3 times (p˂0.05), 2.3 times (p˂0.05) and 1.6 times (p˂0.05), respectively. An increase in the severity of lipid peroxydation and decrease in antioxidant protection under L-NAME administration indicates an enhance in the oxidative stress activity. At the same time, injection of AG led to the opposite effect-a decrease in the level of the MDA in half a day, 1 day and 3 days-1.8 times (p<0.01), 1.7 times (p <0.01) and 2.1 times (p<0.01), respectively, and to an increase in the content of GSH in BP-1.6 times (p<0.01), 2.1 times (p <0.01) and 1.7 times (p<0.01) in the corresponding terms, compared with the values in EP without its administration, indicating a decrease in the prooxidant-antioxidant imbalance. The obtained results may be due to change in the production of reactive nitrogen species under administration of the NOS inhibitors, which leads to modulation of the formation of molecules with prooxidant properties. In addition, in rats with EP, an increase in the number of CEC per unit of blood volume as an indicator of damage to vascular endothelium in half a day-up to 10.6 (10; 11.7)/μl, or 3.4 times (p<0.001), in 1 day-up to 20.6 (19.4; 21.7)/μl, or 6.6 times (p<0.001), in 3 days-up to 19.7 (19.4; 21.1)/l, or 6.4 times (p<0.001), compared with the value in the control group-3.1 (2.2; 4.2)/μl, was found, that indicates a progressive damage to endothelium with the subsequent development of its dysfunction and about the relationship between iNOS activation, changes in the prooxidant-antioxidant state, and damage to endothelium of blood vessels (Figure 1).
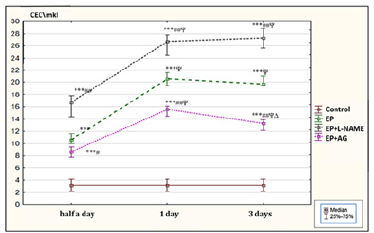
Figure 1: The content of circulating endothelial cells in the blood (CEC/μl) of rats with experimental peritonitis (EP) and administration of Nώ- nitro-L-arginine methyl ester (EP+L-NAME) and aminoguanidine (EP+AG), Me (LQ; UQ). Note*: EP-Experimental peritonitis; L-NAME-Nώ-nitro-L-arginine methyl ester; AG-aminoguanidine; significant differences relative to: * -p<0.05, ** -p<0.01, *** -p<0.001 -control group; # -p<0.05, ## -p<0.01, ### - p<0.001 - “EP” group; Ψ -p<0.05 - half a day and Δ -p<0.05 -1 day.
The administration of L-NAME contributed to an increase in morphological damage to endothelium of blood vessels in rats with EP, which was manifested by increase in the amount of CEC in their blood after half a day, 1 day and 3 days-1.6 times (p<0.01), 1.3 times (p<0.01) and 1.4 times (p<0.01), respectively, which may be due to greater severity of oxidative stress and inhibition of the endothelial NOS isoform with aggravation of microcirculatory disorders. The severity of morphological damage to endothelium of blood vessels in rats with EP and administration of AG was less pronounced, which was manifested in decrease in the amount of CEC in the blood in half a day, 1 day and 3 days 1.2 times (p<0.05), 1.3 times (p<0.01) and 1.5 times (p<0.01), respectively, compared with their number in EP without its use. It is assumed that the corrective effect of AG in relation to endothelium of blood vessels of rats with EP may be associated with a decrease in the toxic effect of NO metabolites on the vascular wall with prooxidant damage peroxynitrite, etc. [10].
Conclusion. Thus, the research of the EP course in rats revealed an increase in the content of nitrites/nitrates and lipid peroxidation product, MDA, in the blood plasma, along with a decrease in the level of the antioxidant defense marker, GSH, and pronounced desquamation of blood vessel endotheliocytes, which may indicate development of oxidative stress and endothelial dysfunction. The study of acute EP course under L-NAME administration revealed an unfavorable effect of non-selective NOS inhibition in relation to the severity of oxidative stress and damage to endothelium of blood vessels. The corrective effect of AG in EP in rats was manifested by a decrease in [NOx], oxidative stress activity and morphological damage to the endothelium of blood vessels in all the studied periods, compared with the values of indicators in rats with peritonitis without its administration, which can be a consequence of the suppression of the excess NO formation with a decrease in the production of the highly toxic peroxynitrite molecule (ONOO-).
Acknowledgment
To the Editors of the Journal.
Conflict of Interest
The authors declare no conflict of interest.
References
- Husakouskaya EV, Maksimovich N Ye (2018) Alternative choice оf an adequate method оf peritonitis modeling in the experiment. News Biomed Sci 17(2): 73-78.
- Maksimovich N Ye, Maslakov DA (2003) Aminoacid L-arginine and perspectives of its use in clinical practice. Healthcare 5: 35-37.
- Lazarenko VA, Lipatov VA, Blinkov Ju Ju, Skorikov DV (2008) Experimental model of diffuse fecal peritonitis. Man and his health 4: 128-132.
- Husakouskaya EV, Maksimovich N Ye, Pavlyukovets A Yu, Patonich IK (2019) Standardization of the infectious peritonitis modeling in the experiment. Topical issues of Physiology: Collection of materials scientific and practical conference with international participation, dedicated 60 years of the Department of Normal Physiology Grodno State Medical University. Belarus.
- Granger DL, Taintor RR, Boockvar KS (1996) Measurement of nitrate and nitrite in biological samples using nitrate reductase and Griess reaction. Methods Enzymol 268: 142-151.
- Rice Evans CA (1991) Laboratory techniques in biochemistry and molecular biology: techniques in free radical research. Elsevier pp. 291.
- Hladovec J, Rossma P (1973) Circulating endothelial cells isolated together with platelets and the experimental modification of their counts in rats. Thromb Res 3(6): 665-674.
- Cinelli MA, Do HT, Miley GP, Silverman RB (2020) Inducible nitric oxide synthase: Regulation, structure, and inhibition. Med Res Rev 40(1): 158-189.
- Proskuryakov S Ya, Konoplyannikov AG, Skvortsov VG, Mandrugin AA, Fedoseev VM (2005) NO-synthase inhibitors containing carboxamidine group and its isosteres. Advances in Chemistry 74(9): 933-952.
- Sylman J (2015) Development of vascular injury models to measure the interactions between platelets, endothelial cells and nitric oxide under physiological flow conditions. ProQuest Diss Publ Colorado School of Mines pp. 231.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.