Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Clinical Results of Oblique Lateral Interbody Fusion (OLIF) Technique Compared with Conventional Lumbar Posterior Laminar Decompression for Lumbar Spinal Stenosis
*Corresponding author: Xin Sun, Department of Orthopedics, Nanjing TCM Hospital Affiliated to Nanjing University of Traditional Chinese Medicine, China.
Received: April 11, 2022; Published:April 26, 2022
DOI: 10.34297/AJBSR.2022.16.002201
Abstract
Objective:To compare and analyze the safety and effectiveness of oblique lateral interbody fusion (OLIF) technique and conventional lumbar posterior laminar decompression for lumbar spinal stenosis (DLCS).
Methods:From October 2019 to November 2021 68 patients with lumbar spinal stenosis over 60 years of age were divided into OLIF group and traditional decompression group according to their treatment methods. There were 32 patients (14 males and 18 females) in the OLIF group, with an age distribution of 60 years or older and a mean of (69.56 ± 4.18) years, and 36 patients (15 males and 21 females) in the traditional decompression group, with an age distribution of 60 years or older and a mean of (70.32 ± 4.82) years, treated with traditional posterior decompression internal fixation of the vertebral plate. The general data, operation time, intraoperative bleeding, hospital stay, surgical complications, clinical efficacy evaluated by modified Macnab criteria, and patients’ preoperative and final postoperative pain visual analog scale scores (VAS) and Owelty dysfunction index (ODI) were statistically analyzed in both groups.
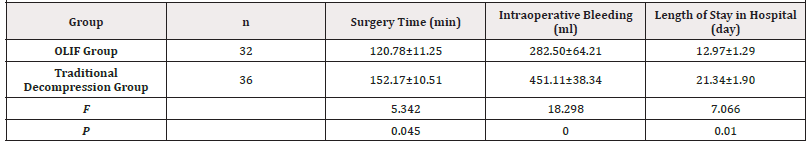
Results:There was no statistically significant difference in age, gender, BMI, disease duration, lesion segment, VAS score, and ODI index between the two groups before treatment (P>0.05). After treatment, the operation time, intraoperative bleeding, hospital stay, and surgical complications were more advantageous in the OLIF group compared with the conventional decompression group, with statistical significance between groups (P<0.05). Compared with the pre-treatment comparison, the VAS score and ODI score of patients in both groups showed significant improvement (P<0.05), and the comparison between the two groups could be found that the improvement in VSA and ODI scores at the end of postoperative period in the OLIF group was more significant than that in the traditional decompression group, with statistical difference (P<0.05). The clinical efficacy of the two groups evaluated by modified MacNab criteria at the end follow-up was 90.625% for the OLIF group and 80.55% for the conventional decompression group, respectively, with statistical differences (P < 0.05).
Conclusion:Compared with traditional decompression fusion, the use of OLIF technique can safely and effectively decompress DLCS, and has many advantages such as less trauma, less bleeding, shorter operative time, and hospital stay, and lower postoperative complications, which is worthy of clinical preference.
Keywords: Lumbar spinal stenosis; Advanced age; Spinal decompression; OLIF endoscopy
Introduction
Lumbar spinal stenosis is a common degenerative disease of the elderly, characterised by pathological spinal stenosis and compression of the spinal capsule together with nerve roots [1]. Clinical symptoms are usually low back pain, neurogenic claudication, lower limb pain and reduced walking ability. DLCS currently relies initially on conservative measures such as physiotherapy, steroid injections, and oral medication [2,3]. However, in patients with painful weakness, progressive reduction in walking distance, progression of neurological deficits and failure of conservative treatment, surgery is often recommended [3]. Numerous studies have shown that the clinical outcome of surgical treatment is superior to that of conservative treatment [3,4]. Oblique lateral interbody fusion (OLIF) reduces the risk of injury to the psoas major and lumbar plexus nerve roots when the natural gap between the retroperitoneal psoas major muscle and the abdominal aorta is used as a reference to create a surgical approach. Unlike paravertebral muscle and posterior lumbar spine surgery, OLIF does not damage the small joints [5].
Materials and methods
General Information
Sixty-eight patients with DLCS aged 60 years or older from October 2019 to November 2021 were included and divided into OLIF and conventional decompression groups according to their treatment. There were 32 patients (14 males and 18 females) in the OLIF group with a mean age of (69.56±4.18) years, and 36 patients (15 males and 21 females) in the conventional decompression group, with an age distribution of 60 years or more and a mean of (70.32±4.82) years. The general data, operation time, intraoperative bleeding, hospital stay, surgical complications, clinical efficacy evaluated by modified Macnab criteria, patients’ preoperative and final postoperative pain visual analogue scale scores (VAS) and Oswestry dysfunction index (ODI) were statistically analysed in both groups.
Inclusion Criteria
(1) Age ≥ 60 years; (2) clinical signs of neurogenic intermittent claudication with or without radiculopathy and imaging of lumbar spinal stenosis; (3) unsatisfactory relief of clinical symptoms after conservative treatment for ≥ 3 months; (4) all patients voluntarily underwent surgical treatment and regular postoperative review. Exclusion criteria: Lateral radiographs of lumbar hyperextension and hyperflexion showing lumbar instability, Cobb angle difference >15° in hyperextension and hyperflexion or displacement of more than 3 mm, requiring fusion surgery; clear-cut cases of intermittent vascular claudication, obvious lumbar disc herniation, vertebral slippage of II° or more, lumbar infection or stenosis combined with malignant tumour.
Surgical Options
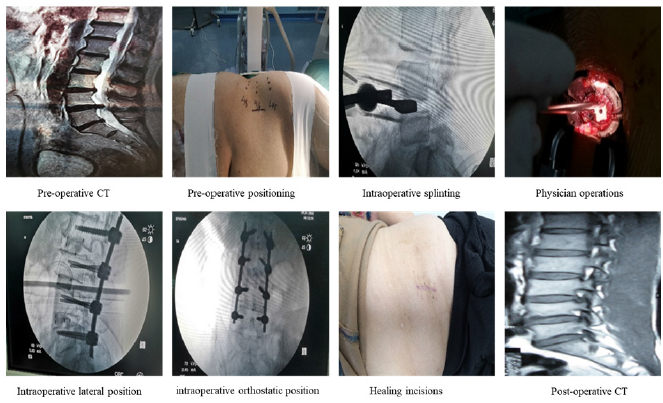
OLIF group: The patient is placed prone on the operating table after satisfactory general Anaesthesia, in the right lateral position, and the operative segment is fluoroscopically positioned and marked before surgery. The skin and deep fascia are incised sequentially with the aid of fluoroscopy, and the retroperitoneal space is reached by bluntly separating the external and internal oblique abdominal muscles and the transversus abdominis fibres, and the abdominal organs are moderately pushed forward. The target disc is exposed through the natural space between the retroperitoneal psoas major muscle and the abdominal aorta, and fluoroscopic fixation of the intervertebral space, canal dilation and removal of excess tissue is completed. The intervertebral space and intervertebral foramen are propped open to the desired height under the appropriate components, and the fusion device places the bone particles into the intervertebral space; after satisfactory results, the incision is closed layer by layer. See Figure 1 ventricular drain is inserted via the operating channel to the appropriate depth. The incision is closed with sutures. One preoperative and one postoperative dose of antibiotics was applied, and bed rest was followed by bed exercise under the protection of a lumbar girth after 3 d. (Figure 1).
Traditional decompression group:Patients in the traditional decompression group were treated with traditional laminectomy for decompression and internal fixation. The procedure was as follows: after satisfactory general Anaesthesia, a posterior median incision was made with the patient’s diseased segment as the center, the skin, subcutaneous tissue and fascia at the edge of the supraspinous ligament were incised in turn, and the sacrospinous muscles on both sides of the spinous process were separated to fully expose the decompression and fixation segment; pedicle screws were placed, the inferior edge of the superior lamina and the entire superior edge of the inferior lamina were excised, and the nerve roots were exposed and released. The nerve roots were exposed and released by subtle enlargement of the lateral saphenous fossa, after which the nerve roots and dura were pulled medially, the intervertebral disc and cartilage endplates were completely removed, an appropriate intervertebral fusion device was selected for intervertebral implant fusion, and the nail rods were linked and fixed with pressure; the incision was closed layer by layer, a wound drainage tube was placed, and the wound was dressed after surgery. The open group in this study all underwent interbody fusion to avoid postoperative instability.
Postoperative management
A drainage tube was routinely placed in the incision. Two patients with cerebrospinal fluid leakage were placed intraoperatively and connected to a drainage bag, and the drainage tube was removed 24 hours after surgery as appropriate. Post-operative antibiotics were routinely administered to prevent infection. Patients were instructed to move their lower limbs as soon as possible to prevent deep vein thrombosis in the lower limbs and to reduce bed-ridden complications. Monitor the patient’s inflammatory and biochemical indexes postoperatively. Actively control blood pressure, blood glucose and other coexisting conditions.
Statistical indicators
Patients’ age, gender, BMI, duration of disease, lesion segment, duration of surgery, intraoperative bleeding, length of hospital stay, surgical complications, modified MacNab criteria to evaluate clinical efficacy, patients’ preoperative and final postoperative pain visual analogue scale scores (VAS), and Oswestry dysfunction index (ODI) were counted.
Statistical methods
SPSS 26.0 software was used for statistical analysis. X2 test was used for counting data (gender, modified MacNab evaluation results) and independent t-test was used to compare the measurement data (operation time, intraoperative bleeding, hospital stay, operation complications, VAS score, ODI score), with P < 0.05 being considered a statistically significant difference.
Results
Analysis of Baseline Information for Both Groups
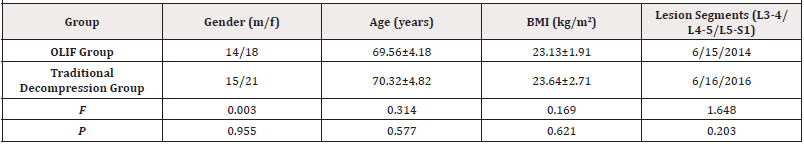
There was no statistical difference between the two groups in terms of gender, age, BMI, and lesion segment (P > 0.05), and they were comparable See (Table 1).
Groups
In the OLIF group, 32 patients had only one postoperative wound infection and no other complications; in the traditional decompression group, 36 patients had three postoperative wound infections, one cerebrospinal fluid leak and one nerve strain Injury (Table 2).
Analysis of Preoperative and Postoperative Final ODI and VSA In the Two Groups
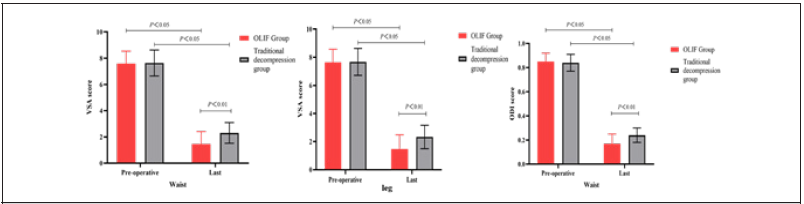
There was no statistical difference in the preoperative VSA and ODI scores between the two groups (P > 0.05); the VSA and ODI scores at the last postoperative follow-up in both groups were significantly improved compared with the preoperative scores, and there was a statistical difference in the intra-group comparison (P < 0.05); the comparison between the two groups revealed that the improvement in VSA and ODI scores at the end of the postoperative period was more obvious in the OLIF group than in the conventional decompression group, and there was a statistical difference (P < 0.05) See (Table 3) and (Figure 2).
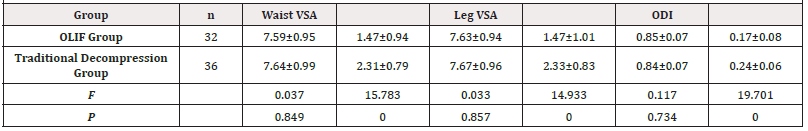
Table 3: Comparative analysis of preoperative and final postoperative VSA and DOI scores between the two groups (`X ±S).
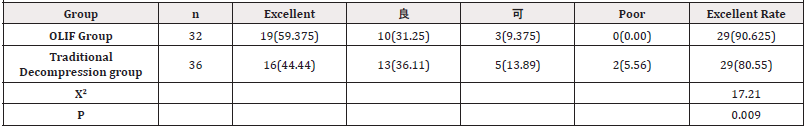
Analysis of the Results of the Evaluation of the Modified MacNab Criteria in the Two Groups
The excellent rate of the two groups was 82.85% in the UBE group and 78.94% in the conventional decompression group when the modified MacNab criteria were evaluated at the 12-month postoperative follow-up, and the UBE group was significantly better than the conventional decompression group, with statistical differences (P < 0.05) (Table 4).
Discussion
Degenerative lumbar spinal stenosis (DLCS) is the most common indication for spinal surgery in the elderly [6]. Wide laminectomy with or without concomitant fusion procedures has been considered the standard surgical procedure for decades [7,8]. This classic approach usually involves extensive soft tissue dissection, but can lead to fatty degeneration, atrophy and paravertebral muscle weakness and result in a failed low back surgery syndrome [9,10]. Randomized controlled trials have shown that fusion is not effective in decompression of degenerative DLCS [11,12]. Considering the complications of spinal fusion and internal fixation, simple but adequate decompression is a more reasonable approach for patients without an absolute indication for additional stabilization surgery [13].
For the surgical treatment of degenerative DLCS, adequate decompression is the most critical determinant. The main aim of surgical treatment is to decompress the nerve structures, thereby relieving symptoms and improving function [14]. However, traditional open surgery requires extensive dissection and traction on the paravertebral muscles, which can lead to muscle ischemia and damage to the nerves, resulting in atrophy, postoperative low back pain and low postoperative patient satisfaction [15]. Minimally invasive techniques have been developed to overcome these limitations. For over 20 years, minimally invasive (MI) spine surgery has been successfully treating patients with a variety of lumbar spine conditions [16-19].
With advances in surgical instrumentation and endoscopic techniques, MI spine surgery has gradually and rapidly evolved from a miniature open to a tubular or percutaneous endoscopic approach. In addition to the potential benefits of the MI spinal surgical approach (smaller wounds, reduced local pain, less blood loss, less postoperative wound pain, and shorter hospital stays), numerous biomechanical studies have demonstrated the importance of the posterior column, including the interspinous ligaments and small joints, in maintaining spinal stability [20,21]. Minimizing disruption to the paravertebral muscles and posterior stabilizing structures is therefore the most critical issue in the long-term developmental progress of MI spine surgery [22]. In the last decade, due to advances in minimally invasive spinal fusion techniques, OLIF surgery has emerged and is increasingly being used by spine surgeons. the benefits of the OLIF technique include preservation of the posterior lumbar structures, reduced blood loss and shorter hospital stays [23].
OLIF can reduce the posterior ligamentous complex by increasing the height of the vertebral space and promoting indirect decompression of the spinal canal. At the same time, OLIF allows reconfiguration of the vertebral sequence to enhance stability. The procedure is minimally invasive while achieving the same efficacy as conventional posterior surgery [24]. OLIF neither invades the spinal canal nor requires crossing the psoas major muscle. In contrast to posterior lumbar interbody fusion, the surgical approach to OLIF is to expose and distract the psoas major muscle by bluntly separating the internal oblique, transversus abdominis and transverse fascia through the natural gap between the psoas major muscle and the retroperitoneal vessels, i.e., revealing the guide needle for insertion into the target vertebral space and then gradually expanding to allow access to the target area [25]. Based on CT imaging data, the OLIF surgical window is divided into a vascular window, a bare window, a lumbar is major window, an ideal surgical window, and an actual surgical window. The vascular window should be avoided when establishing the surgical procedure, noting the location of the abdominal aorta and inferior vena cava, and the presence of the lumbar segmental artery on the posterior lateral aspect of the vertebral body [26].
Preoperative preparation includes adequate knowledge of the width of the gap between the psoas major muscle and the large abdominal vessels to estimate the actual size of the surgical window [27]. The psoas major muscle should not be overstretched, as this may damage the lumbar plexus nerve roots. OLIF should be performed with caution in patients with large-vessel malformations or particularly narrow gaps between the psoas major muscle and the large abdominal vessels. if the assessment indicates that the surgical window is not suitable for OLIF, other treatment options such as posterolateral interbody fusion or conventional posterior decompressive fixation may be considered. In the current study, there was a significant improvement in the clinical symptoms of degenerative DLCS treated by the OLIF technique in the postoperative period. The most significant item was the VAS score for leg pain, which improved from 7.63 to only 1.47. Patients also showed significant improvements in neurological symptoms and disability status, which was reflected in the improvement in ODI. In addition, over 90% of patients had good or excellent outcomes when assessed using the modified MacNab criteria.
References
- Hall S, Bartleson JD, Onofrio BM, HL Baker, H Okazaki, et al. (1985) Lumbar spinal stenosis. Clinical features, diagnostic procedures, and results of surgical treatment in 68 patients. Ann Intern Med 103(2): 271-275.
- Parker SL, Godil SS, Mendenhall SK, Scott LZ, David NS, et al. (2014) Two-year comprehensive medical management of degenerative lumbar spine disease (lumbar spondylolisthesis, stenosis, or disc herniation): a value analysis of cost, pain, disability, and quality of life: clinical article. J Neurosurg Spine 21(2):143-149.
- Katz JN, Harris MB. Anna NT, Emily B, Brett H, et al. (2008) Surgical versus nonsurgical therapy for lumbar spinal stenosis. N Engl J Med 358(8): 794–810.
- Mimiviral A, Sl Tis P, Heli Vaara M, Päivi S, Heikki K, et al. (2007) Surgical or nonoperative treatment for lumbar spinal stenosis? A randomized controlled trial. Spine 32(1): 1-8.
- Britt J, Jain R, Li R, (2021) Robotic radical nephroureterectomy in a patient with situs inversus totalis. Urol Case Rep 37: 101688.
- He JL, Xiao SW, Wu ZJ, Zhen CY, et al. (2016) Microendoscopic discectomy versus open discectomy for lumbar disc herniation: a meta-analysis. Eur Spine J 25(5): 1373-1381.
- Clark AJ, Safaee MM, Khan NR, Matthew TB, Kevin TF, et al. (2017) Tubular microdiscectomy: techniques, complication avoidance, and review of the literature. Neurosurg Focus 43(2): E7.
- Ding Y, Zhang JJ, Lu ZC, (2021) Study on the strategy of posterior endoscopic decompression surgery for lumbar spinal stenosis. Chinese JB and J Surg 4(14): 285-291.
- Kyung CC, June H, Jin SK, Luigi AS, Sol L, et al. (2015) Unsuccessful percutaneous endoscopic lumbar discectomy: a single-center experience of 10,228 cases. Neurosurg 76(4): 372-380.
- Wang ZP, Zhang XG, Li YZ, et al. (2020) Meta-analysis of percutaneous endoscopic lumbar discectomy for the treatment of recurrent lumbar disc herniation complications. Chinese Spinal Cord 274(1): 60-68.
- Chen HL, (2019) Comparison of the efficacy and safety of microendoscopic and microscopic lumbar discectomy for lumbar disc herniation. J Neck and B Pain 40(1): 76-78.
- Cao YW, Liu YJ, Yuan J, et al. (2020) Anatomical study and clinical significance of posterior percutaneous endoscopic cervical discectomy. Chinese J Clinical Anatomy 38(3): 9-12.
- Eum JH, Heo DH, Son SK, et al. Percutaneous biportal endoscopic decompression for lumbar spinal stenosis: a technical note and preliminary clinical results. Journal of neurosurgery. Spine :1-6.
- K Ikuta, O Tono, T Tanaka, J Arima, S Nakano, et al. (2007) Surgical complications of microendoscopic procedures for lumbar spinal stenosis. Minim Invasive Neurosurg 50(3): 145-149.
- Overdevest GM, Moojen WA, Wilco CH J, Wilco CP, Arts MP, et al. (2014) Management of lumbar spinal stenosis: a survey among Dutch spine surgeons. Acta Neurochirur 156(11): 2139-2145.
- Kim HS, Paudel B, Jang JS, Seong HO, Sol L, et al. (2017) Percutaneous Full Endoscopic Bilateral Lumbar Decompression of Spinal Stenosis Through Uniportal-Contralateral Approach: Techniques and Preliminary Results. World Neurosurg 103: 201-209.
- Ding Y, Hai C, Yang JC, et al. (2019) Effect of percutaneous endoscope-assisted transvertebral foraminal lumbar decompression and fusion for single-segment lumbar spinal stenosis on the multifidus muscle. Chinese J Spinal Cord 27(09): 60-65.
- Pao JL, Chen WC, Chen PQ (2009) Clinical outcomes of microendoscopic decompressive laminotomy for degenerative lumbar spinal stenosis. Eur Spine J 18(5): 672-678.
- Minamide A, Yoshida M, Yamada H, Yukihiro N, Hiroshi H, et al. (2015) Clinical outcomes after microendoscopic laminotomy for lumbar spinal stenosis: a 5-year follow-up study. Eur Spine J 24(2): 396-403.
- Xu Baoshan, He Jian, Ma Xinlong, et al. (2013) Anatomical study and clinical application of the translumbar foraminal approach. Chinese J Ort 33(006): 593-600.
- Li XR, Yu J, Zhang W, Gong MG, Long H, et al. (2020) Biomechanical Model Study of the Effect of Partial Facetectomy on Lumbar Stability Under Percutaneous Endoscopy - ScienceDirect. World Neurosurg 139: e255-e264.
- [22]. Bresnahan L E, Smith J S, Ogden A T, et al. (2017) Assessment of Paraspinal Muscle Cross-sectional Area After Lumbar Decompression Minimally Invasive Versus Open Approaches. Clinical Spine Surgery 30(3): E162-E168.
- Hao BC, Li LY, Sun RS (2021) Logistic regression analysis of postoperative coronal imbalance in microendoscope-assisted OLIF surgery for lumbar degenerative disease. Journal of Neck and Back Pain 42(4): 4.
- Vit K, Weerasak S, Chindarat R (2021) Neutral hip position for the oblique lumbar interbody fusion (OLIF) approach increases the retroperitoneal oblique corridor. BMC musculoskeletal disorders 21(4): 583.
- Zhang X, H Wu, Chen Y (2020) Importance of the epiphyseal ring in OLIF stand-alone surgery: a biomechanical study on cadaveric spines. European Spine Journal, 2020(Suppl 3): 1-9.
- Yang C, Zeng C, Li T (2020) Accelerated rehabilitation surgery in OLIF combined with anterior internal fixation for lumbar spinal stenosis with degenerative instability. Chinese Journal of Bone and Joint 9(1): 6.
- Liu J, Feng H (2020) Oblique Lateral Interbody Fusion (OLIF) with Supplemental Anterolateral Screw and Rod Instrumentation: A Preliminary Clinical Study - ScienceDirect. World Neurosurgery 134.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.