Research article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
The Efficacies and Safety of Probiotics of Lactobacillus Rhamnosus GR-1 and Lactobacillus Reuteri RC-14 in Female Vaginal Infections Without Anti-Biotics: A Clinical Trial
*Corresponding author: Dan Cheng, Ph.D., R&D Center, Shanghai Lithy One Health Group, Shanghai, China.
Received: July 04, 2022; Published: July 19, 2022
DOI: 10.34297/AJBSR.2022.16.002277
Abstract
It is urgent and imperative to find an alternative treatment for vaginal infections due to large population of female individuals susceptible of vaginal infections and low efficacies of traditional antibacterial medication and cleansing gels. There have already been clinical studies for applying probiotics in treating vaginal infections. Our trial is the first large scale investigation of 348 female individuals with vaginitis on treatment of probiotics including Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14 in female vaginal infections without antibiotics. After orally supplementation of two strains for 28 days, over 90% female individuals were satisfied with the treatment regarding the improvement in ten symptoms. The trial provided a valuable target for treating vaginitis especially for vulnerable female subjects with the application of GR-1 and RC-14 alone while no safety issues occurred.
Introduction
Female individuals frequently suffer from vaginal infections, leading to reduced quality of life such as unpleasant feeling of private burning and dysuria [1]. Bacterial vaginosis (BV) and vulvovaginal candidiasis (VVC) are two main types of vaginitis. BV, usually with the presence of a fishy odor from vaginal discharge, is the most common cause of vaginal infections worldwide [2]. VVC, with symptoms of white vaginal discharge and vulvar itching, can be considered another critical cause of vaginal infections, afflicting approximately 75% of sexually active women at least once in their lives [3]. Also, 5-50% patients develop more than one episode within a year, making a successful treatment difficult to realize [4]. Traditional treatments of vaginal infections usually include oral and intravaginal agents as antibiotics, costing over 3.1 billion in 2014; however, patients not only suffer from adverse side effects such as altered palate and diarrhea but also high recurrence of the diseases, resulting from antibiotic resistance and eradication of beneficial bacteria inhabiting vaginal canal [5-8].
Like gut microbiota that can either benefit or harm host physiology and health by gut-X axis, vaginal canal, consisting of over 80 varieties of bacteria, can also crucially impact on female private health [9]. A healthy vaginal micro-ecosystem is prevailed by lactobacillus and a commensal flora, which can fundamentally protect female individuals from vaginal infections through directly competing with pathogenic bacteria, keeping vaginal pH below 4.5 and secretion of anti-bacteria H2O2 and bacteriocins [10]. Imbalanced vaginal microflora means overgrowth of pathogenic bacteria such as E. coli and Gardnerella Vaginalis and reduced abundance of probiotic as lactobacillus, which are caused by alterations in lifestyle and physiological conditions such as menstrual cycle, sex life and gut disease. Instead of applying antibiotics that invariably eradicate vaginal microbiota and resulting in an unsuccessful treatment, the restoration of a healthy vaginal micro-ecosystem should be more effective and sustainable.
There have been quite a few solid scientific studies demonstrating the clinical benefits of probiotics in curing vaginitis [11-12]. In a randomized, double-blinded, placebo-controlled trial of 125 premenopausal women diagnosed with BV, the curing rate of BV was much higher by orally administration of Lactobacillus rhamnusus GR-1 and Lactobacillus reuteri RC-14 with antimicrobial metronidazole for 30 days, compared to that of orally taking antibiotics alone [2]. However, probiotics have been playing a role of cooperating with antibiotics in order to improve the curing rate and reduce the side effects while there is little information about the efficacy and safety of using probiotics alone in vaginitis treatment.
In our study, we aim to test the efficacies of Lactobacillus
rhamnusus GR-1 and Lactobacillus reuteri RC-14 in treating vaginal
infections without applying any antibiotics. This experiment was
conducted based on the following considerations:
a) The high occurrence and prevalence of vaginal infections
in Chinese women who are not well educated for probiotic
treatment
b) There is little evidence-based information about probiotics
treatment alone for vaginal infections for Chinese women.
Materials and Methods
Probiotic Strains
L. rhamnosus GR-1 and L. reuteri RC-14 were provided by Chr Hansen, Denmark. The specification of total cell count is no less than 15 billion/g. The probiotics are formulated with inulin and cranberry juice powder in a sachet of 2 g. Each sachet contains no less than 7.5 billion viable cells of both strains.
Subjects and Recruitment
A sample size of 380 Chinese female subjects, from 18 to 65
years old originated from 26 different provinces and districts in
China, was enrolled from January to February in 2022.
The entry criteria include:
a) Had symptoms of vaginal infections
b) Diagnosed by a physician as BV or VVC. Our clinical
research did not exclude individuals who were pregnant, and HPV
positive considering GR-1 and RC-14 showed efficacies and safety
in such cohorts from previous research [13-14].
Intervention
Before the trial, all the subjects have a one-month wash-out period during when antibiotics or probiotics were prohibited to use. In this self-controlled trial of 28 days, each female individual orally took two sachets of probiotics per day. No other probiotics or antibiotics were allowed to be used. The individuals were recommended to take the products at least one hour after meal to reduce the inactivation of probiotics by gastric acid. 32 subjects dropped the trial due to personal reasons while 348 subjects completed the whole trial. All the female individuals signed the consent agreement as they clearly understood the benefits and risks from this trial.
Outcome Measures
After the trial completed at day 28, all the subjects were asked to finish an online questionnaire regarding ten aspects in the improvement and alleviation of their vaginal infections: peculiar leucorrhea smell, excessive leucorrhea, purulent and stinky leucorrhea, foamy leucorrhea, yellow and white-grey leucorrhea, pruritus vulvae, dry and painful vulva, excessive secretion at the end of menstruation, itchy when padded with tampons, pudendal inflammation, swelling and pain. They were also asked to give an overall rate on the efficiency of the product treatment. During the whole trial, they were requested to report to a clinician or the principal investigator immediately if any adverse event happened.
Results
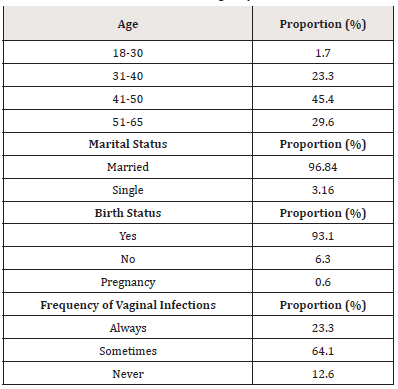
The fundamental information including age, marital status and birth status of the 348 female individuals who completed the research are shown in Table 1. Most of the individuals were older than 30 years old, married and have given birth to at least a child. The individuals from 51- 65 years old were also included, as they might also suffer from vaginal infections led by scarcity of estrogens and thus imbalanced micro-flora in vaginas during menopause period. There were over 87% of the female individuals who were at least sometimes encountering the afflictions of vaginal infections.
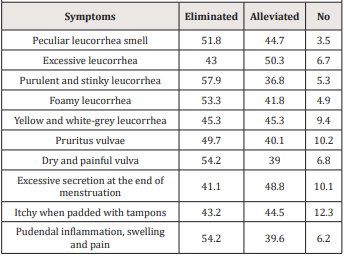
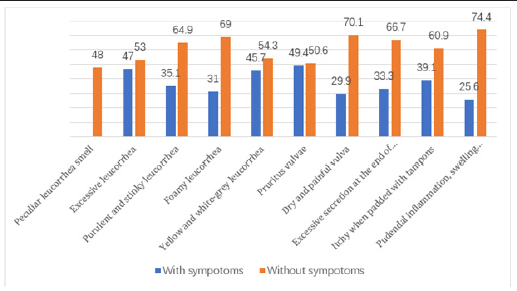
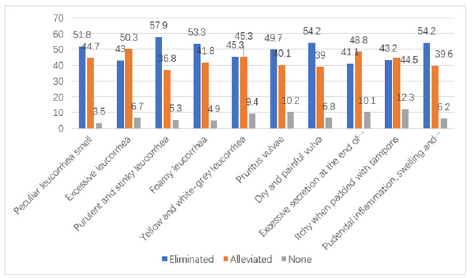
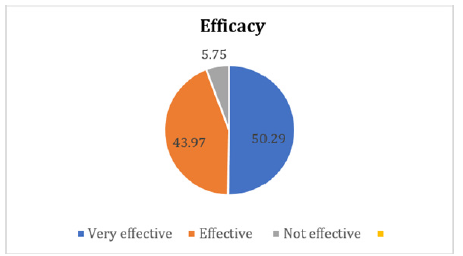
The proportions of each symptom for vaginal infections in the 348 individuals are shown in Figure 1. At least 30% of the female individuals in our trial had one of the ten symptoms. The proportions of female individuals with peculiar leucorrhea smell and pruritus vulvae were 52% and 49.4% respectively. The improvement regarding ten symptoms of vaginitis is shown in Table 2 and Figure 2. Only less than 10% subjects had no feeling of improvement regarding those symptoms. The total satisfaction rates of symptoms improvement regarding both elimination and alleviation were nearly over 90% for most of the symptoms. Almost over 40% of the female individuals reported total elimination of those symptoms. The overall efficacy of this product is shown in Figure 3. The proportions of subjects reporting “very effective” and “effective” were 50.29% and 43.97% respectively while only 5.75% individuals indicated “not effective”.
Discussion
Vaginal infections are strikingly prevalent among female individuals. Our trial included 348 female individuals and over 87% had at least sometimes afflicted by vaginal infections. Traditional therapies of antibiotics eliminate the symptoms quickly, but the high rate of recurrence would be a headache for patients. In the past decades, gut microbiota has been testified to have a bidirectional relationship with host physiology and health. Intervention and generation of health benefits are realized through gut-X axis. Vaginal health, heavily relying on its microbial community, also provides a significant target for potential treatment with improved efficacies and reduce side effects.
The female individuals, who were older than 30 years old, were susceptible to vaginal infections, because they were sexually active. The environment of vagina is mild acid due to prevalence of lactobacillus while active sexual life is inclined to neutralizing and compromising the mild acid environment by semen and thus lead to vaginal infections. Specially, the proportions of married female individuals and those who were from 30 to 50 years old in our trial were 96. 84% and over 68% respectively. Menopaused female individuals are another vulnerable group of subjects with vaginal infection. It is estrogen secretion that facilitates the polysaccharides synthesis in vagina and boosts the abundance of lactobacillus. Due to a sudden drop of estrogen synthesis for menopaused women, they might have insufficient growth of vaginal lactobacillus.
We summarized the symptoms from all the female individuals and subcategorized into 10 aspects including peculiar leucorrhea smell, excessive leucorrhea, purulent and stinky leucorrhea, foamy leucorrhea, Yellow and white-grey leucorrhea, pruritus vulvae, dry and painful vulva, excessive secretion at the end of menstruation, itchy when padded with tampons, pudendal inflammation, swelling and pain. Peculiar leucorrhea smell and pruritus vulvae are the most prevalent symptoms among the individuals. There is still little information on whether applying probiotics alone have a beneficial effect for vaginal infections. Our research can be considered the first large scale interventional study, investigating the efficacy and safety of oral administration of probiotics alone on women with vaginitis for 28 days. The overall satisfaction and efficacy rate of such a treatment is over 94%, regarding 10 relieved symptoms. Amazingly, the symptoms were totally eliminated and relieved for at least 41% and 40% of the female individuals respectively. Only less than 10% of the female individuals did not report improvement after the trial completed. The inefficacy might not result from the product itself but from lack of compliance and inappropriate usage.
Regarding safety, no adverse event was reported during the trial. There was no harm to use GR-1 and RC-14 in our trial even for pregnant women. It is extremely important to treat vaginitis for pregnant women by probiotics. Vaginal infections such as Group B Streptococcus (GBS) could cause inflammation of placenta and premature delivery [15]. A great proportion of pregnant women 3 to 4 weeks before delivery is diagnosed as GBS infected and treated by antibiotics; however, the probiotics that should be passed on to infants during vaginal delivery would be sabotaged. The utilization of probiotics in vaginitis treatment for pregnant women is absolutely beneficial for both mothers and babies.
Vaginal cleansing gel is a popular product for treating vaginitis, which in the long run compromise vaginal probiotics and lead to recurrence of such pathogenic conditions. Undoubtedly treatment targeting microbial conditions would be both beneficial and sustainable. Our trial is valuable because it demonstrated female individuals can possibly replace traditionally used antibiotics and cleansing gel by probiotics while having a comfortable and sustainable feeling during and after the intervention. In the futuristic research, a stricter design of randomized, double-blinded and placebo-controlled trial would be highly appreciated.
Conflicts of Interest
The authors declared that they have no conflicts of interest to this work.
References
- Buggio L, Somigliana E, Borghi A, Vercellini P (2019) Probiotics and vaginal microecology: fact or fancy? BMC women's health, 19(1): 25.
- Anukam K, Osazuwa E, Ahonkhai I, Ngwu M, Osemene G, et al. (2006) Augmentation of antimicrobial metronidazole therapy of bacterial vaginosis with oral probiotic Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14: randomized, double-blind, placebo-controlled trial. Microbes and infect 8(6): 1450-1454.
- Ferrer J (2000) Vaginal candidosis: epidemiological and etiological factors. Int J Gynaecol Obstet 71 Suppl 1: S21-S27.
- Paulitsch A, Weger W, Ginter-Hanselmayer G, Marth E, Buzina W, et al. (2006) A 5-year (2000-2004) epidemiological survey of Candida and non-Candida yeast species causing vulvovaginal candidiasis in Graz, Austria. Mycoses 49(6): 471-475.
- Foxman B, Barlow R, D'Arcy H, Gillespie B, Sobel JD, et al. (2000) Candida vaginitis: self-reported incidence and associated costs. Sexually transmitted diseases 27(4): 230-235.
- Martinez RC, Franceschini SA, Patta MC, Quintana SM, Candido RC, et al. (2009) Improved treatment of vulvovaginal candidiasis with fluconazole plus probiotic Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14. Letters in applied microbiology 48(3): 269-274.
- Pawlaczyk M, Friebe Z, Pawlaczyk MT, Sowinska-Przepiera E, Wlosinska J, et al. (2006) The effect of treatment for vaginal yeast infection on the prevalence of bacterial vaginosis in early pregnancy. Acta dermatovenerologica Croatica 14(1): 26-29.
- Bauters TG, Dhont MA, Temmerman MI, Nelis HJ (2002) Prevalence of vulvovaginal candidiasis and susceptibility to fluconazole in women. American journal of obstetrics and gynecology 187(3): 569-574.
- Cheng D, Song J, Xie M, Song D (2019) The bidirectional relationship between host physiology and microbiota and health benefits of probiotics: A review. Trends in Food Science & Technology 91: 426-435.
- Reid G, Charbonneau D, Erb J, Kochanowski B, Beuerman D, et al. (2003) Oral use of Lactobacillus rhamnosus GR-1 and L. fermentum RC-14 significantly alters vaginal flora: randomized, placebo-controlled trial in 64 healthy women. FEMS immunology and medical microbiology 35(2): 131-134.
- Reid G, Bruce AW, Fraser N, Heinemann C, Owen J, et al. (2001) Oral probiotics can resolve urogenital infections. FEMS Immunol Med Microbiol 30(1): 49-52.
- Anukam KC, Osazuwa E, Osemene GI, Ehigiagbe F, Bruce AW, et al. (2006) Clinical study comparing probiotic Lactobacillus GR-1 and RC-14 with metronidazole vaginal gel to treat symptomatic bacterial vaginosis. Microbes and infection 8(12-13): 2772-2776.
- Gille C, Böer B, Marschal M, Urschitz MS, Heinecke V, et al. (2016) Effect of probiotics on vaginal health in pregnancy. EFFPRO, a randomized controlled trial. American journal of obstetrics and gynecology 215(5): 608.e1-608.e7.
- Ou YC, Fu HC, Tseng CW, Wu C H, Tsai CC, et al. (2019) The influence of probiotics on genital high-risk human papilloma virus clearance and quality of cervical smear: a randomized placebo-controlled trial. BMC women's health 19(1): 103.
- Verani JR, Mc Gee L, Schrag SJ (2010) Division of Bacterial Diseases, National Center for Immunization and Respiratory Diseases, Centers for Disease Control and Prevention (CDC) (2010) Prevention of perinatal group B streptococcal disease--revised guidelines from CDC, 2010. MMWR 59(RR-10): 1-36.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.