Case Report 
 Creative Commons, CC-BY
Creative Commons, CC-BY
A New Wedge-Shape Dental Implants for Narrow Bone Ridge: REX Piezoimplant, a Case Report With 12 Months of Follow-Up
*Corresponding author: Prof. Lucia Memè, Department of Clinical Sciences and Stomatology, Polytechnic University of Marche, 60126 Ancona, Italy
Received: May 19, 2022; Published: May 30, 2022
DOI: 10.34297/AJBSR.2022.16.002224
Abstract
Objective: The purpose of this study was to report the surgical protocol used in implant prosthetic rehabilitation with REX PiezoImplant type TL1.8 (Rex TL, Rex Implants, Columbus, OH, USA).
Methods: A 54-year-old patient was enrolled in the study. Clinical and radiographic examination (CBCT) showed severe bone atrophy of the maxilla. The preparation of the implant sites was performed with piezoelectric instruments and a specific sequence of inserts (SLC, W1, W2, W3, and W4). The implants were inserted with the REX IPD magnetic hammer achieving a slight bone expansion.
Results: The patient was strictly monitored monthly for up to 12 months. The final prosthesis was delivered 5 months after surgery. CBCT performed at the end of the study demonstrated good osseointegration of the implants and the absence of periimplant bone resorption.
Conclusions: The use of REX PiezoImplants can be considered a valid minimally invasive surgery technique in atrophic bone crests, which do not allow the insertion of traditional implants without bone regeneration procedures.
Keywords: Wedge Implant; Narrow Ridge; Piezosurgery; Minimally Invasive Surgery; Atrophic Bone Crest
Materials and Methods
A 54-year-old female patient was enrolled in this study. She did not suffer from systemic disease and did not smoke. The systemic exclusion criteria were: (i) existence of metabolic bone disease, (ii) history of malignancy, (iii) history of radiotherapy or chemotherapy for malignancy in the past 5 years, (iv) history of autoimmune disease, and long-term steroidal or antibiotic therapy. The patient desired to replace her upper removable total prosthesis with a fixed prosthesis on dental implants.
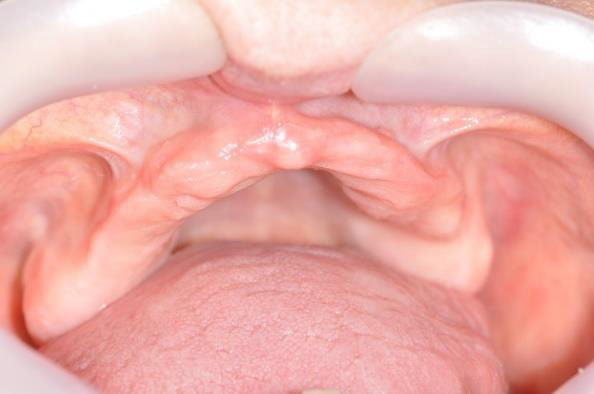
The patient was provided oral and written information regarding the surgery and the study, and written informed consent was obtained. The clinical examination showed an atrophic maxillary alveolar ridge, as expected since the patient extracted teeth and wore a total removable prosthesis for a long period of time (Figure 1).
Before the surgery, she was subjected to oral hygiene in order to lower the bacterial charge and favor the bone healing. Moreover, before starting the surgical phase, she was subjected to a Cone Beam Computer Tomography (CBCT), made by KAVO–ICAT 3D EXAM (KaVo, Biberach, Germany), to evaluate the bone width of the interested site. Images were acquired by means of Kavo software and processed by a computer, using a cutting thickness of the images of 0.8 mm. Acquisition was performed using a FOV of 23x17 mm, in order to avoid stitching [1]. During the radiographical evaluation, the patient worn her removable prosthesis in which some metallic spheres with the function of landmarks have been blocked with wax (Figure 2).
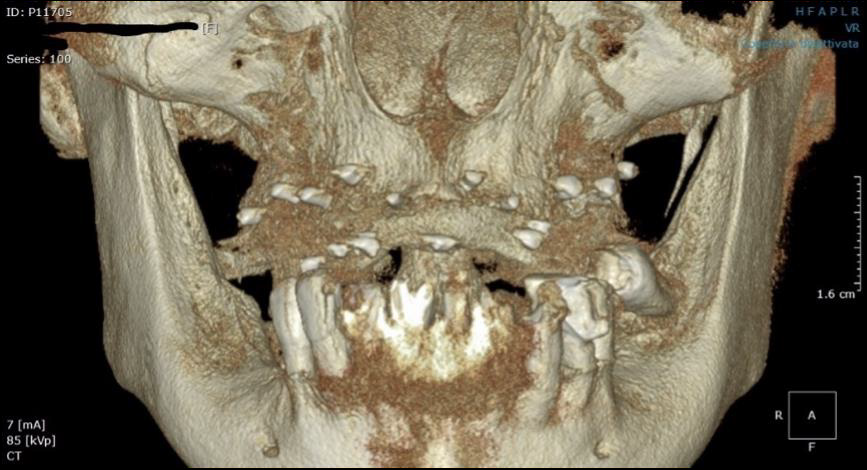
Figure 2: CBCT was carried out before the surgery, at the baseline of the study. The metallic spheres inserted into the removal prothesis were visible and used as landmarks for the implant insertion.
The CBCT analysis confirmed the clinical evaluation, highlighting a maxillary bone resorption and a horizontal bone width inconsistent with the insertion of traditional implants, without bone regeneration procedures. The width of the bone ridge was determined by measuring in perpendicular direction the distance between the buccal and lingual walls.
Using the metallic spheres as landmarks, 4 points were evaluated in the CBCT scans (Figure 3A):
a. Point 1, with a horizontal width of 2.86 mm (Figure 3B);
b. Point 2, with a horizontal width of 3.22 mm (Figure 3C);
c. Point 3, with a horizontal width of 2.66 mm (Figure 3D);
d. Point 4, with a horizontal width of 3.29 mm (Figure 3E).
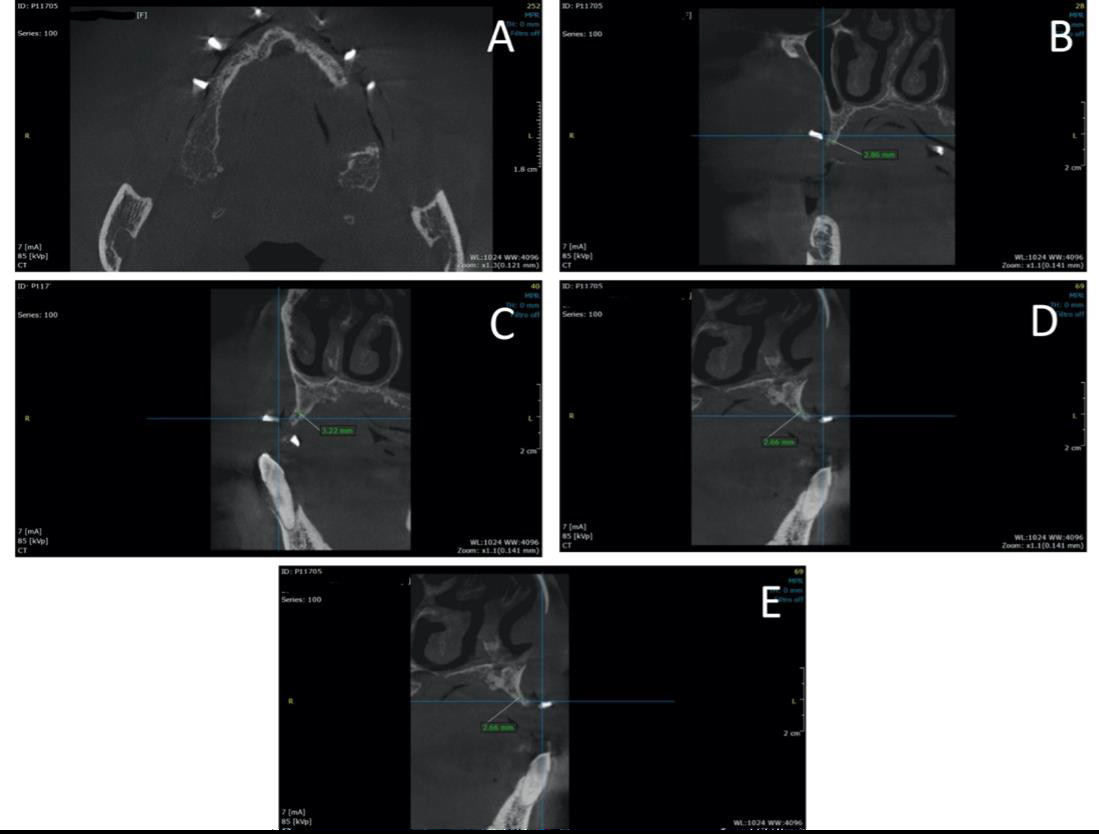
Figure 3: CBCT evaluation before the surgery highlighting 4 point were implants will be inserted. (A) Metallic spheres were inserted into the removable prosthesis as landmarks. (B) Point 1 revealed a horizontal width of 2.86 mm; (C) Point 2 and Pont 3 (D) displayed a horizontal width of 3.22 mm and 2.66 mm, respectively; (E) Point 4 showed a horizontal width of 3.29 mm.
Based on these horizontal measurements, it was decided to treat the patient with a minimally invasive implant rehabilitation, using four REX PiezoImplant TL1.8 type (Rex TL, Rex Implants, Columbus, OH, USA). One hour before surgery, patient received 2 gr of amoxicillin, and then, just before surgery, 0.2% chlorhexidine mouthwash was performed for 2 minutes. Moreover, 1 g of amoxicillin twice a day for 5 days was prescribed. The patient was subjected to local anaesthesia with Articaine, 40 mg/ml 1:100.000, administered by infiltration in the areas adjacent to the surgery.
Subsequently, a crestal incision was made from zone 2.6 to zone 2.1 and from zone 1.1 to zone 1.6. Full-thickness flaps were reflected in the vestibular and palatal sides to maximize visualization of the underlying alveolar ridge defect and to allow a good implant positioning. Four REX PiezoImplants, with a length of 9 mm and a maximum thickness of 1.8 mm, were inserted following the surgical protocol suggested to the manufacturer. Each step of preparation of implant site was performed with the piezoelectric device Piezosurgery® (Mectron S.p.A).
At first, the bone crest was made uniform through the use of the SLC insert. For each implant, initially, the pilot osteotomy was performed, with the special insert W1, performing a first perforation in the desired implant position (sites 1.3, 1.5 2.3 and 2.5), reaching a depth of 9 mm. Subsequently, the correct insertion axis, position, angulation and distance between the 4 pilot osteotomies were verified by means of the alignment pins. Then, using W1 insert, two secondary osteotomies, used as landmarks, were created for each implant: the first was made 1 mm mesial and the second 1 mm distal each initial pilot osteotomy, reaching a depth of 5mm.
Through the micro-saw burr W2 the main osteotomy was connected to the secondary osteotomies, reaching a depth of 9 mm. The walls of the osteotomy were finished using the W3 micro-file insert. By inserting the appropriate FitGauge the size and alignment of the performed osteotomies were again checked. Finally, through the micro-file insert W4, the osteotomies were widened in a mesiodistal direction, to a depth not greater than 3 mm for the type of implant selected (REX TL 1.8) (Figure 4A).
After the preparation of the implant sites, implants were inserted using the REX IPD magnetic hammer (Implant Placement Device, Mectron S.p.A) (Figure 4B). Since the patient presented a type 3 bone quality according to Misch et al. [2], the four implants were inserted with 6/8 percussions, each with an increasing power from 1 to 4 (IPD value scale), thus also obtaining a slight bone expansion.
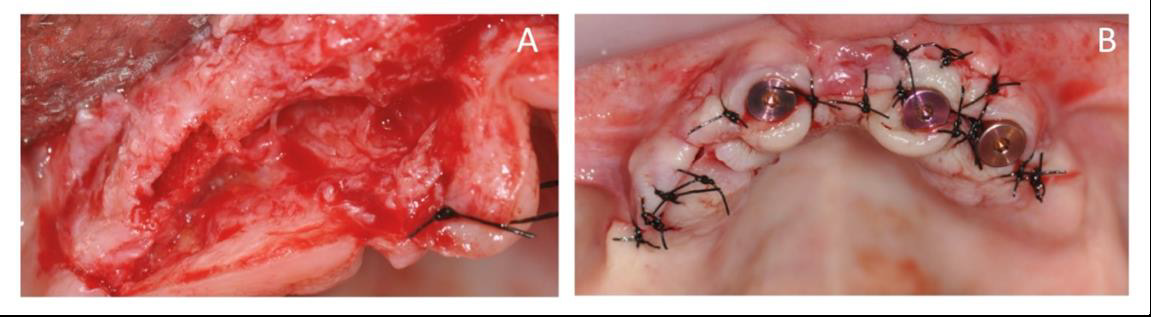
Figure 4: (A) Maxillary bone crest after the implant sites preparation with the follower burrs: W1, W2, W3 and W4. (B) Implants were inserted, and single sutures were used to close the flaps. Finally, the cover screws were located.
Once the implants were inserted, a single suture, using 4.0 Supramid (B.Braun, Milano S.p.A), were performed.
Sutures were removed after 10 days. During the healing period, the patient underwent regular monthly checks and the upper mobile prosthesis was relined with a soft acrylic resin in order to avoid soft tissue compression.
At the end of the 4 months required for the correct implant healing and osseointegration, a polyether impression was taken, and, through the use of pre-screwed transfers, the correct position of the implants was reported in the impression.
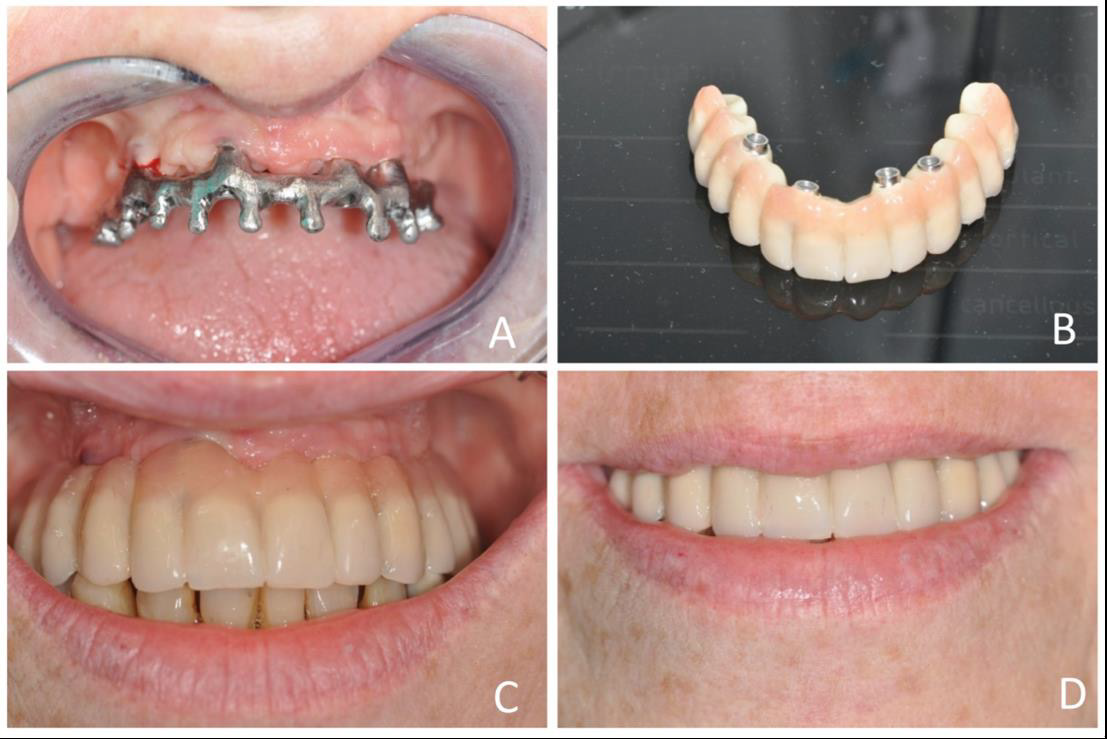
The metal connection structure was screwed to the implants by means of titanium cylinders inserted into the structure itself (Figure 5A-5D). Finally, the final prosthesis was made on the metal structure and was screwed to the implants, without soft tissue compression (Figure 5C).
Results and Discussion
Result
In this case report a 54-year-old patient was enrolled. The surgical procedures were performed successfully as planned without complications. The follow-up evaluation performed at the time of suture removal, on day 10, and after 1 month, showed uneventful healing, no signs of inflammation and soft tissue closure. The CBCT analysis, performed at 12 months of follow-up, revealed no residual radiolucency and a good osteointegration of the inserted implants (Figure 6).
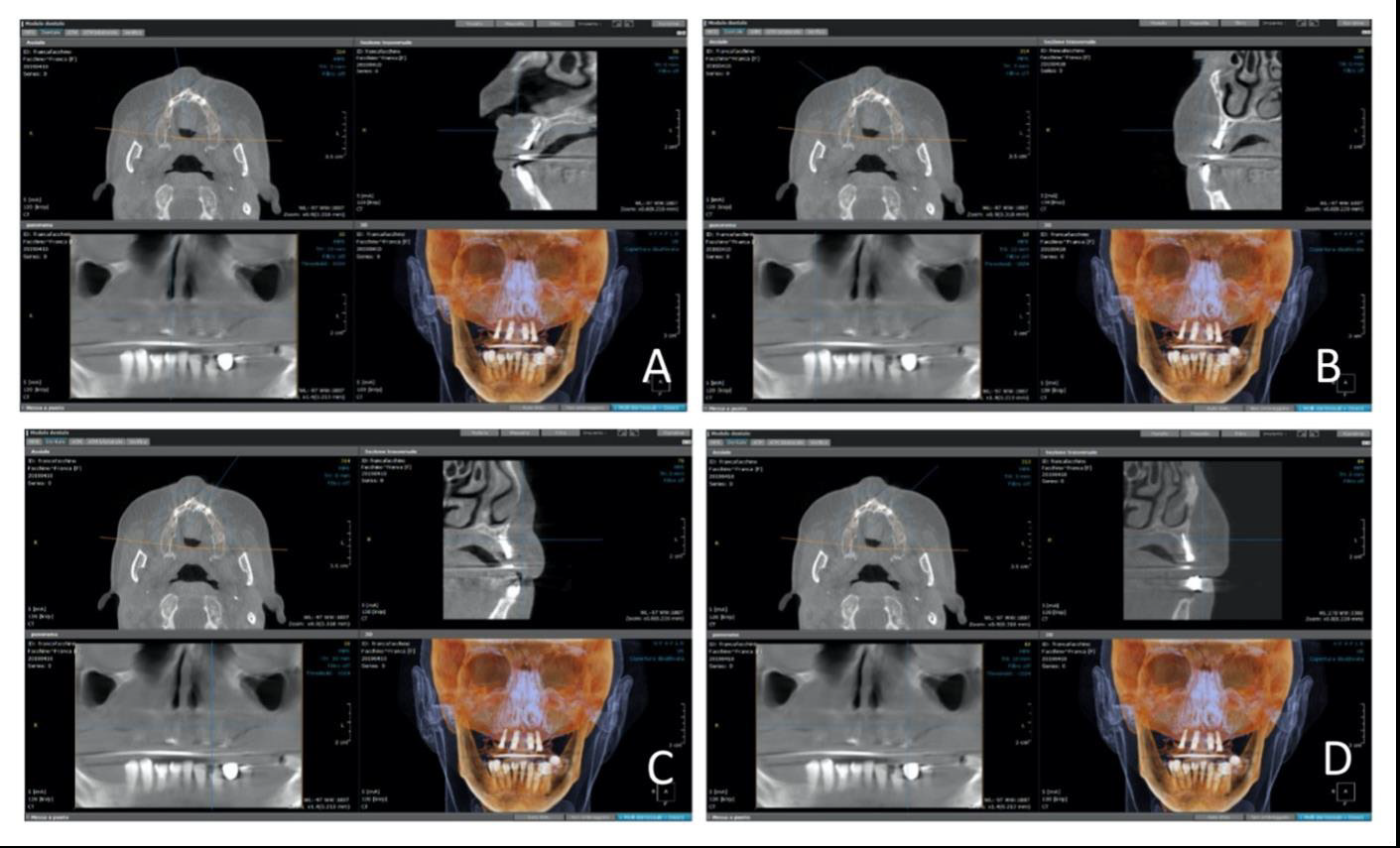
Figure 6: CBCT, performed after 12 months from the surgery, in the site 1.3 (A), 1.5 (B), 2.3 (C), 2.5 (D), revealed a good integration of the inserted implants.
Discussion
Nowadays, the use of these wedge implants can be considered as a valid minimally invasive surgery technique in atrophic bone crests, which do not allow the insertion of traditional implants without bone regeneration procedures.In particular, the REX PiezoImplant represents an interesting evolution of the Linkow blade [3]. Blade implants showed a high failure rate due to unpredictability in achieving primary stability, the type of loading protocol and postoperative complications [4]. Implant primary stability displays an important role in the osseointegration of dental implants. In the study of Vercellotti et al a good primary stability was obtained after the insertion of REX PiezoImplant in all cases and both mesiodistal and bucco-lingual ISQ values at 6-month follow-up resulted significantly higher than at 4-month follow-up [5].
Moreover, the possibility of preparing the implant site with coldcut vibrating inserts rather than with high-speed drills, reduces the heat avoiding the risk of creating bone necrosis and favoring a better osteointegration [6]. A recent meta-analysis showed that ultrasonic implant site preparation has a positive influence on early bone healing, resulting in faster development of secondary stability when compared to conventional drilling techniques [7]. In a recent study of Vercellotti et al. [8], these implants with a wedge-shape showed low morbidity and positive short-term clinical results in narrow ridges treatment [9-16]. Further researches are needed, but from the data obtained, these implants show an excellent prognosis, avoiding complications, facilitating the surgery and improving the patient’s comfort [17-26].
Conclusion
The progressive resorption of the alveolar ridge after tooth extraction may lead to maxillary or mandibular atrophy, resulting in reduced horizontal or vertical dimensions of the bone crest or in a combination of them. Insufficient bone volume could compromise the implant insertion. This case report documents the insertion of a new wedge-shape dental implant, REX PiezoImplant (Rex TL, Rex Implants, Columbus, OH, USA) in a patient with a horizontal bone width between 2.66 mm and 3.29 mm. According to our results, REX PiezoImplants displayed a good osteointegration, also demonstrated by CBCT analysis after 12 months of follow-up.
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this study. Authors confirm that the submitted work, including images, is original and the journal policies have been reviewed. There are no conflicts of interest to disclose.
References
- Fokas G, Vaughn VM, Scarfe WC, Bornstein MM (2018) Accuracy of linear measurements on CBCT images related to presurgical implant treatment planning: A systematic review. Clin Oral Implants Res 29 Suppl 16: 393-415.
- Misch CE, Judy KW (1987) Classification of partially edentulous arches for implant dentistry. Int J Oral Implantol 4: 7-13.
- Linkow LI (1968) The blade vent--a new dimension in endosseous implantology. Dent Concepts 11(2): 3-12.
- Sendyk DI, de Oliveira NK, Pannuti CM, da Graça Naclério-Homem M, Wennerberg A, et al. (2018) Conventional Drilling Versus Piezosurgery for Implant Site Preparation: A Meta-Analysis. J Oral Implantol 44: 400-405.
- Chiapasco M, Zaniboni M, Boisco M (2006) Augmentation procedures for the rehabilitation of deficient edentulous ridges with oral implants. Clin Oral Implants Res 17(Suppl 2): 136-159.
- Stacchi C, Bassi F, Troiano G, Rapani A, Lombardi T, et al. (2020) Piezoelectric bone surgery for implant site preparation compared with conventional drilling techniques: A systematic review, meta-analysis and trial sequential analysis. Int J Oral Implantol (Berl) 13(2): 141-158.
- Di Murro B, Gallusi G, Nardi R, Libonati A, Angotti V, et al. (2019) The relationship of tooth shade and skin tone and its influence on the smile attractiveness. Journal of Esthetic and Restorative Dentistry 32(1): 57-63.
- Vercellotti T, Troiano G, Oreglia F, Lombardi T, Gregorig G, et al. (2020) Wedge-Shaped Implants for Minimally Invasive Treatment of Narrow Ridges: A Multicenter Prospective Cohort Study. J Clin Med 9: 3301.
- Cardaropoli G, Araújo M, Lindhe J (2003) Dynamics of bone tissue formation in tooth extraction sites. An experimental study in dogs. J Clin Periodontol 30(9): 809-818.
- Van der Weijden F, Dell’Acqua F, Slot DE (2009) Alveolar bone dimensional changes of post-extraction sockets in humans: a systematic review. J Clin Periodontol 36(12): 1048-1058.
- Ten Heggeler JM, Slot DE, Van der Weijden GA (2011) Effect of socket preservation therapies following tooth extraction in non-molar regions in humans: a systematic review. Clin Oral Implants Res 22(8): 779-788.
- Tan WL, Wong TLT, Wong MCM, Lang NP (2012) A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin Oral Implants Res 23(Suppl 5): 1-21.
- Chiapasco M, Casentini P, Zaniboni M (2009) Bone augmentation procedures in implant dentistry. Int J Oral Maxillofac Implants. 24 Suppl: 237-259.
- Lento D, Piva A, Beltramini G, Mummolo S (2020) Oral rehabilitation of maxilla: technical consideration. J Biol Regul Homeost Agents 34 (1 Suppl. 1): 115-117.
- Candotto V, Gallusi G, Piva A, Baldoni M, Di Girolamo M (2020) Complications in sinus lift. J Biol Regul Homeost Agents 34(1 Suppl. 1): 139-142.
- Grassi A, Memè L, Orsini G, Licini C, Orilisi G, et al. (2020) A New Surgical Protocol For Horizontal Ridge Augmentation: Simplified Apposition Technique. Human Histologic and Radiographic Analysis After 2.5 Years of Follow-Up, A Case Report. Archives of Clinical and Medical Case Reports. Fortune Journals 4: 239-252.
- Chiapasco M, Casentini P (2018) Horizontal bone-augmentation procedures in implant dentistry: prosthetically guided regeneration. Periodontol 2000. 77: 213-240.
- Grasso G, Mummolo S, Bernardi S, Pietropaoli D, D’Ambrosio G, et al. (2020) Histological and Histomorphometric Evaluation of New Bone Formation after Maxillary Sinus Augmentation with Two Different Osteoconductive Materials: A Randomized, Parallel, Double-Blind Clinical Trial. Materials (Basel) 13(23): E5520.
- Bambini F, Orilisi G, Quaranta A, Memè L (2021) Biological Oriented Immediate Loading: A New Mathematical Implant Vertical Insertion Protocol, Five-Year Follow-Up Study. Materials (Basel) 14(2): E387.
- Mummolo S, Mancini L, Quinzi V, D’Aquino R, Marzo G, et al. (2020) Rigenera® Autologous Micrografts in Oral Regeneration: Clinical, Histological, and Radiographical Evaluations. Applied Sciences. Multidisciplinary Digital Publishing Institute 10: 5084.
- Bambini F, Greci L, Memè L, Santarelli A, Carinci F, et al. (2006) Raloxifene covalently bonded to titanium implants by interfacing with (3-aminopropyl)-triethoxysilane affects osteoblast-like cell gene expression. Int J Immunopathol Pharmacol 19: 905-914.
- Quaranta A, DʼIsidoro O, Bambini F, Putignano A (2016) Potential Bone to Implant Contact Area of Short Versus Standard Implants: An In Vitro Micro-Computed Tomography Analysis. Implant Dent 25(1): 97-102.
- Bambini F, Lo Muzio L, Procaccini M (2001) Retrospective analysis of the influence of abutment structure design on the success of implant unit. A 3-year controlled follow-up study. Clin Oral Implants Res 2: 319-324.
- Bambini F, Memè L, Procaccini M, Rossi B, Lo Muzio L (2004) Bone scintigraphy and SPECT in the evaluation of the osseointegrative response to immediate prosthetic loading of endosseous implants: a pilot study. Int J Oral Maxillofac Implants 19(1): 80-86.
- Santarelli A, Mascitti M, Orsini G, Memè L, Rocchetti R, et al. (2014) Osteopontin, osteocalcin and OB-cadherin expression in Synthetic nanohydroxyapatite vs bovine hydroxyapatite cultured Osteoblastic-like cells. J Biol Regul Homeost Agents 28: 523-529.
- Meme L, Santarelli A, Marzo G, Emanuelli M, Nocini PF, et al. (2014) Novel hydroxyapatite biomaterial covalently linked to raloxifene. Int J Immunopathol Pharmacol 27: 437-444.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.