Short Communication 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Evaluation of the Effect of Vitamin D in the Development of Deep Vein Thrombosis in those with Factor V Leiden Mutation
*Corresponding author: Gökhan Doğukan Akarsu, Department of Pharmacy Services, Yozgat Bozok University, Vocational School of Health Services, Turkey.
Received: October 11, 2022; Published:October 20, 2022
DOI: 10.34297/AJBSR.2022.17.002340
Abstract
Aim: This study was conducted to evaluate the effect of vitamin D in patients with Factor V Leiden mutation (FVL) in the development
of Deep Vein Thrombosis (DVT).
Material and Method: This prospective clinical study was conducted to evaluate vitamin D levels in 110 participants carrying FVL
with or without DVT. Patients who did not agree to participate in the study and did not come for routine controls were excluded
from the study.
Results: The mean age of the participants was 50±14.69 years, 47.3% were female, and 70% were diagnosed with DVT. The vitamin
D level of 14.56% of the participants in the study was below 20ng/ml.
Conclusion: There was no statistically significant difference in vitamin D levels between participants with and without DVT (p>0.05).
Keywords: DVT; FV; Leiden Mutation; Vit D; Thrombosis; Pulmonary Embolism; Acquired Risk Factors; Cardiovascular Disability; Oral Contraceptives; Central Venous Catheters; Thrombophilia
Introduction
Deep Vein Thrombosis (DVT) refers to the development of thrombosis in the veins of the lower extremities. DVT is likely to lead to serious complications such as pulmonary embolism [1,2]. Many hereditary and acquired risk factors contribute to the development of DVT [3]. DVT is among the largest causes of death or cardiovascular disability from embolism [4] and develops in areas where blood flow is altered, such as pockets of veins in the legs adjacent to valves [5]. It has been stated that DVT occurs not only in adults but also in infants, mostly in male genders [6]. Oral contraceptives [4], pregnancy [7,8], central venous catheters and thrombophilia [9], cancer, obesity and old age have been identified as risk factors for DVT formation. In addition, ancestral gene sequencing may also predispose to DVT. For this reason, it is possible to find a solution to the disease with studies to be conducted on patients with DVT [10]. Various inherited hematological disorders such as Protein C, Protein S and antithrombin deficiency, homocysteine and Factor V Leiden (FVL) mutation are predisposing factors for thromboembolism [11,12].
FVL is one of the most common findings in DVT and is a protein involved in the coagulation pathway and is the main procoagulant responsible for the conversion of factor X, which accelerates the conversion of prothrombin to thrombin [13]. Vitamin D (25-OH Vit D), on the other hand, is a fat-soluble vitamin that has functions in calcium and phosphorus metabolism. Vitamin D has important roles in the mineralization of our skeletal system by affecting the absorption and metabolism of these minerals [14]. Vitamin D is also considered as an important factor reducing the risk of getting sick in chronic diseases, cancer, infectious diseases and cardiovascular diseases [15]. Today, there are many methods such as venous duplex scanning, Tomography, D dimer to diagnose DVT. It is stated that some metabolites are formed in the blood with the development of DVT [16]. The aim of this study is to evaluate vitamin D levels in participants carrying FVL with or without DVT.
Material and Methods
Type and Location of the Study
This study is cross-sectional. The study was carried out in Bozok University Hospital located in the Central Anatolia region of Turkey.
Sample Selection
One hundred and ten participants carrying FVL with or without DVT were enrolled in the study. Patients who smoked, refused to participate in the study and could not attend their routine controls were excluded from the study. During the study period, 77 patients with DVT met the specified criteria and agreed to participate in the study. In addition, a control group was formed with 33 volunteers who were not diagnosed with DVT but were FVL carriers. The study was completed with a total of 110 participants.
Data Collection
Data were collected through the patient information form. In addition, vitamin D values were obtained from the files of the patients and recorded in the data collection form.
Analysis of the Data
The data of the study were evaluated using IBM SPSS (25.0) in a computer environment. The conformity of the data to the normal distribution was evaluated by Shapiro Wilk. T Test and One Way Anova were used in the analysis of data with normal distribution. And p values less than 0.05 were considered significant. Etichal statetment: Our research was approved by the local ethics committee and consent was obtained from each participant.
Result
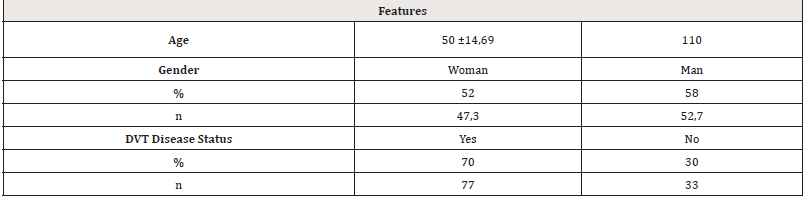
The mean age of the participants was 50 ±14.69 years. The ages of both the experimental and control group participants were in a normal distribution and there was no statistical difference between the groups. 52.7% of the participants in the study were male. The data are given in Table 1.
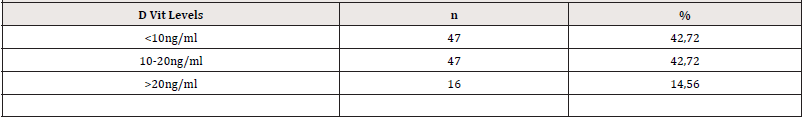
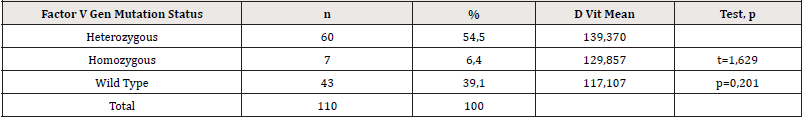
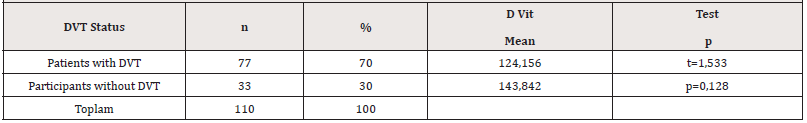
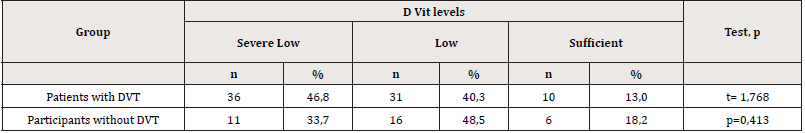
Vitamin D levels were grouped. 0-10ng/ml severe low vitamin D, 10.01-20 ng/ml low level vitamin D, 20.01 and above ng/ml adequate vitamin D level. Table 2 shows the distribution of vitamin D levels by groups (Table 2). The averages of vitamin D according to the factor V gene mutation status are given in Table 3. There was no statistically significant difference between the two groups in terms of vitamin D levels (p<0.05). The mean distribution of DVT patients with factor V gene mutations and those without DVT according to their vitamin D levels is given in Table 4. It was found that the difference between vitamin D levels of patients with and without DVT was not statistically significant (p<0.05). There was no statistically significant difference between the groups in the chisquare analysis performed according to the vitamin D levels of the participants carrying FVL with and without DVT (p>0.05) (Table 5).
Discussion

Factor V is the necessary cofactor for prothrombinase activity. In the presence of Ca+2 with vascular damage, it combines with Xa on the membrane surface and converts prothrombin to thrombin [17,18]. Factor V Leiden mutation (FVL) is one of the most common mutation types, especially in northern Europe and the Middle East. It refers to the replacement of Guanine with Adenine in the nucleotide at position 1691 of the gene in the Leiden mutation. It causes the replacement of arginine with glutamine in the factor V protein, making it difficult to perform its function [19]. FVL mutation predisposes to thrombosis. The mean age of the participants with Factor V mutation, who constituted our study group, was 50 ±14.69 years. Khademvatani, et al. [20] average age 47 years in their study, Wu and He [21] average age 68 years in their study. Since our study is in the middle-aged upper group, it is close to the young old age, which is the frequent occurrence of the disease [20,21]. Vitamin D has an important place in human life. In addition to its role in bone health, there are various studies investigating its effectiveness in various cardiovascular and cancer cases [22-24]. Values of 25-hydroxyvitamin D (25(OH)D) in plasma below ≤20ng/mL are considered vitamin D deficiency.
Vitamin D deficiency is common worldwide. In our study, vitamin D level of 10ng/ml and below was considered as severe deficiency, between 10,001-20ng/ml as moderate deficiency, and 20ng/ml and above as adequate level. It was determined that 14.56% of the participants in our study had sufficient level of vitamin D in their plasma. However, there was no statistically significant difference in vitamin D levels between those with and without a diagnosis of DVT. Lindqvist, et al. [7], Tangpricha, et al. [25] and Brot, et al. [26] stated in their studies that high vitamin D levels can prevent thrombosis. The limited amount of data in our study and the fact that it was conducted in a specific region may be the reason why there was no statistically significant result between vitamin D and DVT [27-29]. On the other hand, it has been stated that early vitamin D supplementation is associated with a long and healthy lifespan due to the increase in diseases with advancing age [29].
Conclusion
Studies reveal that vitamin D is not only related to bone development, but also has new effects in studies. In our study, no statistical correlation could be established between vitamin D and DVT among participants with FVT mutations. However, the role of vitamin D between prothrombin and thrombin is known. It is still being evaluated that this effect will be positive in DVT patients. It is only because the study was conducted in one region and a small number of patients were evaluated. It will be useful to reveal the relationship between the disease and vitamin D with studies to be conducted in many different regions.
Acknowledgement
None.
Conflict of Interest
No Conflict of Interest.
References
- Kyrle PA, Eichinger S (2005) Deep vein thrombosis. Lancet 365(9465): 1163-1174.
- Di Nisio M, Van Es N, Büller HR (2016) Deep vein thrombosis and pulmonary embolism. Lancet 388(10063): 3060-3073.
- Lensing AW, Prandoni P, Prins MH,Büller HR (1999) Deep-vein thrombosis. Lancet 353(9151): 479-485.
- Jerjes Sanchez C, Martinez Sanchez C, Borrayo Sanchez G, Carrillo Calvillo J, Ursulo Juarez Herrera, et al. (2015) Third national registry of acute coronary syndromes (RENASICA III). Arch Cardiol Mex 85(3): 207-214.
- Aird WC (2007) Vascular bed‐specific thrombosis. J Thrombosis Haemost 5(1): 283-291.
- Raffini, L, Huang YS, Witmer C, Feudtner C (2009) Dramatic increase in venous thromboembolism in children's hospitals in the United States from 2001 to 2007. Pediatrics 124(4): 1001-1008.
- Lindqvist P, Dahlbäck B, Marŝál K (1999) Thrombotic risk during pregnancy: a population study. Obstet Gynecol 94(4): 595-599.
- Jaffray J, Young G (2018) Deep vein thrombosis in pediatric patients. Pediatr Blood Cancer 65(3).
- Silverstein MD, Heit JA, Mohr DN, Petterson TM, O Fallon WM, et al. (1998) Trends in the incidence of deep vein thrombosis and pulmonary embolism: a 25-year population-based study. Arch Intern Med 158(6): 585-593.
- Şahin Ş, Benli İ, Aydoğan L (2012) Distribution of prothrombin G20210A, factor V Leiden, and MTHFR C677T mutations in the middle Black Sea area (Tokat) of Turkey. Turk J Med Sci 42(6): 1093-1097.
- Simone B, De Stefano V, Leoncini E, Zacho J, Martinelli I, et al. (2013) Risk of venous thromboembolism associated with single and combined effects of Factor V Leiden, Prothrombin 20210A and Methylenetethraydrofolate reductase CG77T: a meta-analysis involving over 11,000 cases and 21,000 controls. Eur J Epidemiol 28(8): 621-647.
- Castañeda Gaxiola R, Munive Lima MR, Meillón García LA, Rish Fein L, Sigler Morales L, et al. (2017) Trombosis venosa asociada a trombofilias. Revisión y reporte de casos. Rev Mex Angiol 45(2): 73-79.
- Slusher KB (2010) Factor V Leiden A case study and review. Dimens Crit Care Nurs 29(1): 6-10.
- Genç A, Sevim DG, Özen AT, Yilmaz G (2015) D vitamininin çeşitli hastalıklardaki nadir kullanım alanları. Ankara Tıp Üniversitesi Fakültesi Mecmuası 68(2): 55-60.
- Holick MF (2007) Vitamin D deficiency. N Engl J Med 357(3): 266-281.
- Maekawa K, Sugita C, Yamashita A, Moriguchi Goto S, Furukoji E, et al. (2019) Higher lactate and purine metabolite levels in erythrocyte-rich fresh venous thrombus: Potential markers for early deep vein thrombosis. Thromb Res 177: 136-144.
- Mann KG, Kalafatis M (2003) Factor v: A combination of dr jekyll and mr hyde. Blood 101(1): 20-30.
- Kalafatis M, Egan JO, van't Veer C, Cawthern KM, Mann KG (1997) The regulation of clotting factors. Crit Rev Eukaryot Gene Expr 7(3): 241-280.
- El Mouatassim S, Couprie N (2000) Diagnostic moléculaire des anomalies congénitales prédisposant aux thromboses veineuses: Biologie molé Spectra biologie 19(113): 49-52.
- Khademvatani K, Seyyed Mohammadzad MH, Akbari M, Rezaei Y, Eskandari R, et al. (2014) The relationship between vitamin D status and idiopathic lower-extremity deep vein thrombosis. Int J Gen Med 7: 303-309.
- Wu WX, He DR (2018) Low vitamin D levels are associated with the development of deep venous thromboembolic events in patients with ischemic stroke. Clin Appl Thromb Hemost 24(9_suppl): 69S-75S.
- Norman PE, Powell JT (2014) Vitamin D and cardiovascular disease. Circulation research 114(2): 379-393.
- Elamin MB, Abu Elnour NO, Elamin KB, Fatourechi MM, Alkatib AA, et al. (2011) Vitamin D and cardiovascular outcomes: a systematic review and meta-analysis. J Clin Endocrinol Metab 96(7): 1931-1942.
- Ebeling PR (2022) Does vitamin D supplementation reduce cardiovascular events and cancer?. The American Journal of Clinical Nutrition 115(5): 1255-1256.
- Tangpricha V, Turner A, Spina C, Decastro S, Chen TC, et al. (2004) Tanning is associated with optimal vitamin D status (serum 25-hydroxyvitamin D concentration) and higher bone mineral density. Am J Clin Nutr 80(6): 1645-1649.
- Brot C, Vestergaard P, Kolthoff N, Gram J, Hermann AP, et al. (2001) Vitamin D status and its adequacy in healthy Danish perimenopausal women: relationships to dietary intake, sun exposure and serum parathyroid hormone. Br J Nutr 86(S1): S97-S103.
- Lindqvist PG, Epstein E, Olsson H (2009) Does an active sun exposure habit lower the risk of venous thrombotic events? AD‐lightful hypothesis. J Thromb Haemost 7(4): 605-610.
- Mózsik G, Rumi G, Dömötör A, Figler M, Papp E, et al. (2005) Involvement of serum retinoids and Leiden mutation in patients with esophageal, gastric, liver, pancreatic, and colorectal cancers in Hungary. World J Gastroenterol 11(48): 7646-7650.
- Noordam R, De Craen AJ, Pedram P, Maier AB, Mooijaart SP, et al. (2012) Levels of 25-hydroxyvitamin D in familial longevity: the Leiden Longevity Study. Cmaj 184(18): E963-E968.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.