Review Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Comparative Dosimetric Study using Various Applicators for Vaginal Cuff Brachytherapy; Three Ovoid Technique Proposal
*Corresponding author: Sunghyun Kim, MD, Department of Radiation Oncology, Wonju Severance Christian Hospital, Yonsei University Wonju College of Medicine, Wonju, Republic of Korea.
Received: March 28, 2023; Published: April 14, 2023
DOI: 10.34297/AJBSR.2023.18.002486
Abstract
Purpose: Vaginal-cuff brachytherapy is the adjuvant treatment in women with intermediate-high risk of endometrial or uterine cervical cancers. The most common applicators are single-channel vaginal cylinders and two-symmetric ovoid applicators according to the shape of the stump. For two-ovoid applicators, the distance between them depends on the therapist and vaginal size. A greater distance means a lower dose in the vaginal apex point. To overcome this problem, this study proposes brachytherapy plans using three-ovoid applicators to improve insufficient dose distribution.
Materials and Methods: Clinical dosimetry was calculated using HDRPlus software, and patients were treated using the BEBIG MultiSource® High Dose Rate brachytherapy treatment unit with a cobalt-60 source. In this study, three types of applicators (cylinder, two-ovoid, and three-ovoid) and three brachytherapy plans were compared for optimal dose delivery. The three-ovoid applicators used were two-ovoids and tandem with multiple holding discs. To compare the three brachytherapy plans, the prescription point, vaginal apex point, bladder, and rectal dose were evaluated.
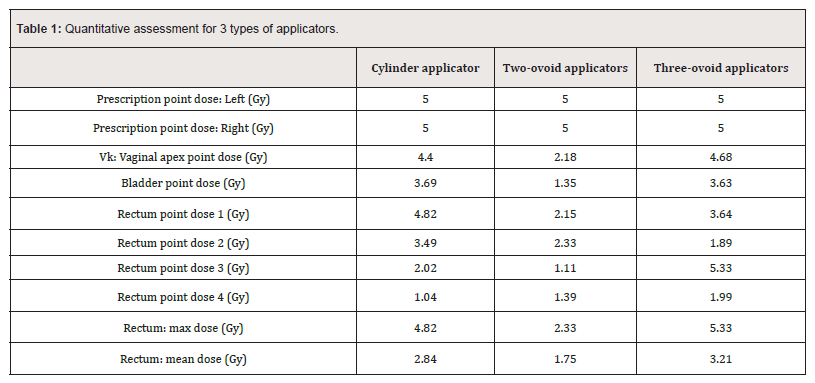
Results: In the plans using cylinder, two-ovoid, and three-ovoid applicators, the calculated values for the vaginal apex point were 4.40 Gy, 2.18 Gy, and 4.68 Gy, respectively. These values corresponded to 88%, 43.7%, and 93.7% of the prescribed dose, respectively. The bladder doses were 3.69 Gy, 1.35 Gy, and 3.63 Gy, respectively. The rectal doses ranged from 1.0-4.8 Gy, 1.1-2.3 Gy, and 1.8-5.3 Gy, respectively.
Conclusion: According to the dosimetric comparison of these applicators, vaginal-cuff brachytherapy plans using three-ovoid applicators may be a way to overcome the vaginal apex cold spot.
Keywords: Analysis of variance; F -test; Gene expression data; Multiple mean comparison.
Introduction
Since the introduction of intracavitary brachytherapy to treat gynecologic cancer patients by Margaret Cleaves in 1903 [1,2], vaginal cuff brachytherapy has been an effective way to deliver ionizing radiation in endometrial cancer and selected cervical cancer patients who are at high risk of recurrence posthysterectomy [3]. The vaginal cuff is the upper portion of the vagina that opens up into the peritoneum and is sutured after the removal of the cervix and uterus during a hysterectomy. For treatment of the vaginal cuff, the most commonly used applicator is the singlechannel cylinder and two symmetric ovoid applicators according to the shape of the vaginal stump [4]. The choice of applicator depends on the consultant and the clinical scenario. Generally, ovoids treat the upper part of the vaginal cuff, whereas vaginal cylinders allow treatment of the entire length of the vagina. Both applicators have pros and cons in clinical use and dosimetric properties. The cylinder applicator is convenient for insertion, can deliver a uniform dose distribution over the surface, and is available in various diameters to minimize the air gap between the cylinder and the vaginal wall. However, there is a slight underdosage to the “dog-ear” area of the vagina [4]. The cylinder also delivers a higher dose to the bladder and rectum compared to ovoid applicators. However, dose laterality can be modified, and the mean dose to the rectum and bladder can be lowered by using two-ovoid applicators. However, the distance between the ovoid applicators depends on the therapist and vaginal size, and the vaginal apex may be underdosed with the two-ovoid technique. To overcome the problem, we have conducted this study with three-ovoid applicators to improve insufficient dose distribution.
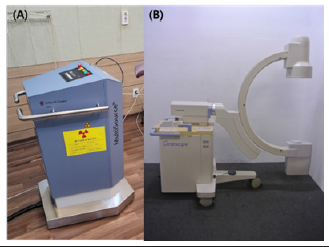
Clinical dosimetry was calculated using HDRPlus (Eckert & Ziegler, Germany) software, and patients were treated using the BEBIG MultiSource® High Dose Rate brachytherapy treatment unit with a cobalt-60 source. For a treatment plan, posterior-anterior (PA) projection and right-left (RL) lateral projection images were acquired using the c-arm fluoroscopic x-ray system (Clear scope SXT-9000A, Toshiba). The brachytherapy and c-arm system used in this study are shown in Figure 1.
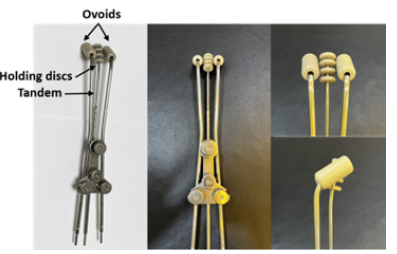
In this study, three types of applicators (cylinder, two-ovoid, and three-ovoid) were used, and three brachytherapy plans were compared for optimal dose delivery. The comparison between various brachytherapy plans to find an optimal setting was explained to the patients, and the patients agreed to be included in this study. The diameter of the cylinder was 3 cm, and the air gap between the cylinder and the vaginal wall was minimized. The two-ovoid applicators with a diameter of 1.5 cm were inserted as symmetrically as possible in accordance with the tension and size of the vagina. Ovoids are placed on the right and left outer edges and the inferior side of the cervix. As shown in Figure 2, the concept of the three-ovoid applicator was used by modifying the fletcherset applicator for the cervix. The three-ovoid applicator consists of two ovoids and a tandem with multiple holding discs. Holding discs were used to prevent perforation of the surgical site of the vaginal cuff during insertion, and the curved direction of the tandem was in the same direction as the ovoid. In accordance with American Brachytherapy Society guidelines [4], the total treatment dose was 5Gy in five separate fractions.
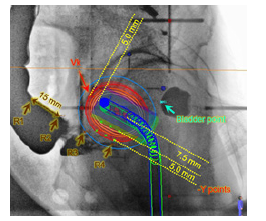
For each individualized treatment plan, dose optimization is performed from a standardized plan according to the applicator types. The aim of each plan was to provide optimal dose distributions to the prescription point, defined by a depth of 5 mm in the vaginal mucosa surrounding the applicator. A dosimetry analysis was carried out using orthogonal radiographs where point doses to critical structures were calculated according to the ICRU 38 recommendations [5]. To compare the three brachytherapy plans, the prescription point, vaginal apex point (Vk) [6], bladder, and rectal dose were evaluated. Figure 3 shows the schematic diagram of the vaginal apex point and bladder and rectal dose points. The dose at the vaginal apex point, which was defined as 5 mm above the surface of the vaginal apex corresponding to the midline of the applicator tips and perpendicular to the anteroposterior axis of the patient, was calculated. In the RL image, the point located on the back wall of the urinary balloon closest to the applicator was marked as the bladder reference point. In addition, the barium contrast agent was used to confirm the rectal wall, and the rectal reference point was marked along the rectal surface as the point closest to the applicator on the rectal wall.
Results
Figure 4 shows the treatment plans using the three types of applicators, and Table 1 shows the quantitative dose assessment results. The dose distribution was planned so that 100% of the 5Gy prescription dose could be delivered to the prescribing point. In the plan using cylinder, two-ovoid, and three-ovoid applicators, the calculated values for the vaginal apex point were 4.40 Gy, 2.18 Gy, and 4.68 Gy, respectively. These values correspond to 88%, 43.7%, and 93.7% of the prescribed dose, respectively. The treatment plan using the cylinder applicator showed a uniform dose distribution overall. As shown in Figure 4C-4D, the greater the distance of the two-ovoid applicators, the lower the dose appears in the vaginal apex point. Because of some underdosing at the center of the vagina, there is a limit to delivering the dose uniformly and conformally to the target volume. For optimal dose distribution, three-ovoid applicators are proposed to compensate for the disadvantages of a cylinder and two-ovoid applicators. As shown in Figure 4E-4F, superior dose coverage for the vaginal cuff was obtained in the brachytherapy plan using the three-ovoid applicator.
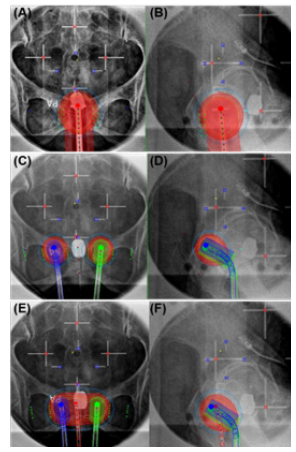
Figure 4. Brachytherapy plans and dose distribution using (A, B) the cylinder, (C, D) two-ovoid, and (D, F) three-ovoid applicators in (A, C, E) posterior-anterior (PA) projection images and (B, D, F) right-left (RL) lateral projection.
Comparing the quantitative dose evaluation of major organs, the bladder point doses were 3.69 Gy, 1.35 Gy, and 3.63 Gy, respectively. The rectal point doses ranged from 1.04–4.82 Gy, 1.11–2.33 Gy, and 1.89–5.33 Gy, respectively. The two-ovoid applicators delivered a lower dose to the bladder and rectum for a given vaginal dose compared to others. The use of a cylinder and three-ovoid applicators resulted in similar dose values to the bladder and rectum.
Discussion
In this study, three-ovoid applicators were proposed to deliver the optimal doses to the treatment region. When deciding which applicator to use for vaginal-cuff brachytherapy, if the “dog-ear” area of the vagina is not present, the cylinder applicator should be used. If there is a “dog-ear” area of the vagina, it should be simulated first with two-ovoid applicators. Currently, the greater the distance between the two ovoids, the lower the dose appears in the vaginal apex point. To overcome the severe cold spot, we devised a plan using three-ovoid applicators. In the two-ovoid technique, when a larger-sized ovoid is used, the dose distribution is slightly better, but it is not completely resolved. However, three-ovoid applicators are not necessarily superior to two-ovoid applicators. If the distance between the two ovoids is not far enough to result in a cold spot, three-ovoid applicators do not need to be applied. Also, if there is not enough space in the intravaginal cavity, it is difficult to insert an additional ovoid between the ovoids.
Figure 5 shows a brachytherapy plan and dose distribution using the two-ovoid applicators. The prescription dose is 4Gy per fraction, and the calculated value for the vaginal apex point is 3.27 Gy, which corresponds to 81.75% of the prescribed dose. The bladder point dose was 1.84 Gy, and the rectal point doses along the rectal wall ranged from 0.65–2.62 Gy, with an average dose of 1.73 Gy. In this case, we decided to use two-ovoid applicators.
The distance between the ovoids can vary depending on the therapist, as well as the size and tension of the vagina. If the therapist fixes the two ovoids with too much tension, it may cause problems with the surgical suture site, so careful consideration and experience may be required. If a severe cold spot is expected to occur due to the distance between the ovoid applicators, even at low tension, three-ovoid applicators may be considered.
The ultimate goal of brachytherapy is to achieve as low of radiation dose as possible to the surrounding normal tissue while delivering the highest homogeneous dose within the target. The main dose-limiting normal structures are the rectum and bladder, which are closer to the target in patients who have undergone hysterectomy. Therefore, rectal and bladder doses should be minimized to reduce treatment-related side effects. Two-ovoid applicators allow relatively low bladder and rectal doses because of the applicator geometry while supplying reduced normal tissue doses and preventing treatment-related side effects, such as narrow vagina and vaginal shortening. In addition, two-ovoid applicators diminish the potential rectal injury rate [6]. However, the mean doses to the rectum and bladder were found to be significantly higher when cylinders were used [7]. The geometry of the cylinder applicator does not allow the optimization of rectal dose unless shielding and multi-channel applicators [8] are used. In this study, the highest rectal dose was shown when three-ovoid applicators were used, while the most uniform dose was delivered to the target. Since the Vk point, rectum, and bladder are generally located in the midline, the doses of those points have a proportional value, although it varies depending on each applicator and the patient’s anatomy (Table 1). Because the three types of applicators have different dose characteristics for normal organs and target doses, the selection and placement of applicators should be made carefully, depending on the treatment scenario and effectiveness.
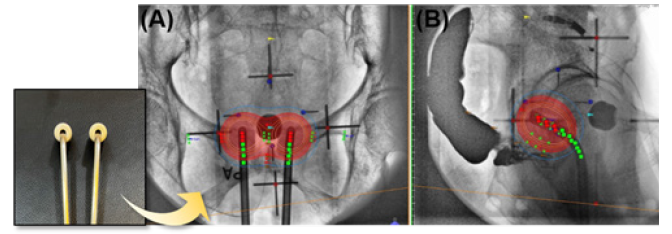
Figure 5. Brachytherapy plan and dose distribution using the two-ovoid applicator method in (A) a posterior-anterior (PA) projection image and (B) right-left (RL) lateral projection.
There are several limitations to this study. First, although the dosimetric characteristics were compared, we used a twodimensional image-based brachytherapy plan. The calculated point doses may not represent the accurate dose received by the volume of the organs. Point doses measured based on orthogonal images sometimes lead to under or overestimating results for normal organs. For that reason, volume-based dose calculation is better than point dose calculation for both target and organs at risk. The advantage of the three-dimensional image-based brachytherapy plan is the accurate quantification of doses received by various volumes of surrounding critical structures. For more accurate dose verification, we will apply three-dimensional image-based brachytherapy in the future. Next, this study only proposed the three-ovoid technique, and it is difficult to know how much the improvement in the coverage of the Vk point affects the patient’s prognosis. Therefore, we identified the feasibility of three-ovoid applicators, but more patient cases and the evaluation of oncologic outcomes and toxicities are needed in further studies. Finally, since each hospital may have different applicators, it may be difficult to broadly apply this technique. However, understanding these concepts will enable application with little modification for each applicator.
Conclusion
In conclusion, according to the results of the dosimetric comparison of three types of applicators, vaginal-cuff brachytherapy plans using three-ovoid applicators can be a way to overcome the vaginal apex cold spot. Since the three types of applicators have different dosimetric properties conferring specific advantages and disadvantages for normal organs and target doses, all applicators have good reproducibility if applicator selection and placement are carefully made.
Statement of Ethics
Ethics approval was not required for this article.
Conflict of Interest Statement
No potential conflict of interest relevant to this article was reported.
Data Availability Statement
Not applicable.
References
- Cleaves MA (1903) Radium: With a preliminary note on radium rays in the treatment of cancer. Med Rec 64: 601-606.
- Aronowitz JN, Aronowitz SV, Robison RF (2007) Classics in brachytherapy: Margaret Cleaves introduces gynecologic brachytherapy. Brachytherapy 6(4): 293-297.
- Zakem SJ, Robin TP, Smith DE, Arya Amini, William A Stokes, et al (2019) Evolving trends in the management of high-intermediate risk endometrial cancer in the United States. Gynecol Oncol 152(3): 522-527.
- Small W Jr, Beriwal S, Demanes DJ, Kathryn E Dusenbery, Patricia Eifel, et al. (2012) American Brachytherapy Society consensus guidelines for adjuvant vaginal cuff brachytherapy after hysterectomy. Brachytherapy 11(1): 58-67.
- (1992) International Commission on Radiation Units and Measurements. ICRU Report 38, Dose and Volume Specification for Reporting Intracavitary Therapy in Gynecology. Bethesda, MD: ICRU Publication.
- Tuncel N, Garipagaoglu M, Kizildag AU, Andic F, Toy A (2009) Optimisation techniques in vaginal cuff brachytherapy. Br J Radiol 82: 936-940.
- Kumar NP, Kumar A, Jayaprakash PG, Raghukumar P, James FV (2018) Dosimetric comparison of bladder, rectal, and vaginal surface doses between ovoids and cylinder-based vaginal brachytherapy in carcinoma of the endometrium. J Cancer Res Ther 14(6): 1191-1195.
- Bahadur YA, Constantinescu C, Hassouna AH, Eltaher MM, Ghassal NM, et al. (2015) Single versus multichannel applicator in high-dose-rate vaginal brachytherapy optimized by inverse treatment planning. J Contemp Brachytherapy 6(4): 362-370.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.