Clinical Image 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Emphysematous Gastritis
*Corresponding author:Luis Enrique Nunez Moscoso, Department of Emergency Internal Medicine, Hospital Nacional “Carlos Alberto Seguin Escobedo” EsSalud, Arequipa, Peru.
Received:April 03, 2023; Published:April 19, 2023
DOI: 10.34297/AJBSR.2023.18.002492
Introduction
An 80-year-old female patient presents to the emergency department with an illness time of three days characterized by abdominal pain and distension, nausea, bilious vomiting, and diarrhea, after which she presents respiratory distress.
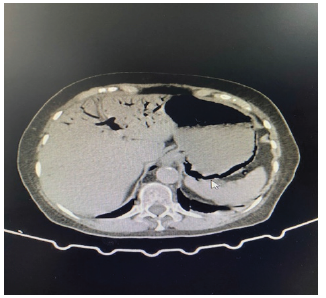
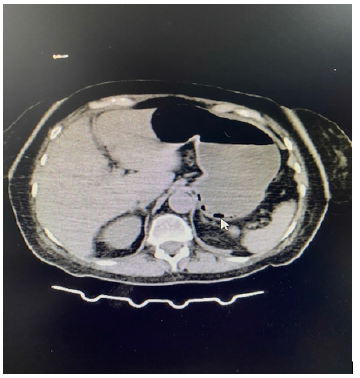
On physical examination, the chest was mobile with breathing and decreased vesicular murmur in the bases. Saturation 92% at FiO2 0.28. Globular and slightly depressed abdomen, painful on diffuse palpation and decreased air-fluid sounds. Laboratory tests showed 5760 leukocytes with 30% bands, creatinine 1.51 mg/dl, PH 7.39, PO2 76 mmHg, PCO2 26 mmHg, HCO3 16 mmol/L, and lactate 3.3 mmol/L. An abdominal tomography without contrast was performed, which showed massive pneumatosis in the liver, the gastric wall, and some areas of the lower segment (Figure 1). Emphysematous gastritis was diagnosed, and support treatment started in addition to intravenous antibiotics: meropenem 1 g every 8 hours and metronidazole 500 mg every 8 hours. On the third day of treatment, an improvement could be observed from the clinical and laboratory point of view. An abdominal tomography without control contrast was taken, which shows a substantial improvement compared to the first (Figure 2). Emphysematous gastritis is a rare form of phlegmonous gastritis associated with the invasion of the gastric wall by gas-forming bacteria. Gastric mucosal injury from alcoholism, trauma, peptic ulcer, or gastric intervention may predispose to bacterial invasion. The treatment of choice is antibiotics and surgery. Due to the lack of typical symptoms, the diagnosis is frequently delayed, which, associated with a rapid evolution to peritonitis, frequently gives a lethal result.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.