Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Prevalence of Intestinal Parasites among Patients Accessing care in Secondary and Tertiary Healthcare Institutions in Edo State, Nigeria
*Corresponding author:Elemuwa CO, Pharmacovigilance Directorate, National Primary Health Care Development Agency, Abuja, Nigeria
Received:March 09, 2023 Published:March 30, 2023
DOI: 10.34297/AJBSR.2023.18.002467
Abstract
Intestinal parasitic infections are prevalent in developing countries and are of great public health concern. This study aims to compare the prevalence of intestinal parasitic infections among patients seeking care in secondary and tertiary healthcare facilities in Edo State, Nigeria. A total of 576 patients with gastrointestinal complaints and accessing healthcare in secondary (420) and tertiary healthcare (156) facilities in Edo State, Nigeria were recruited for this study. Stool specimens were collected and processed using formol-ether concentration method. Although intestinal parasitic infections were only detected among patients seeking care in the secondary health facility, there was no significant difference in the prevalence of intestinal parasitic infections among patients seeking care in secondary and tertiary healthcare facilities (1.90% vs 0.00%; p=0.7203). Age, gender and whether the patients had diarrhoea had no significant impact on the prevalence of intestinal parasitic infections (p> 0.05). Entamoeba histolytica, Ascaris lumbricoides and hookworm were the parasites detected with hookworm been the most prevalent. Overall, a prevalence of 1.39% of intestinal parasitic infections was observed in this study and the parasites were only recovered from patients accessing care in a secondary healthcare facility.
Introduction
Among the most common illnesses in humans in underdeveloped nations are parasitic infections brought on by intestinal helminths and protozoan parasites [1]. Over 2 billion people, or about onethird of the world’s population, are infected, with children making up the vast majority [2,3]. These illnesses are linked to bad hygiene practices, a lack of access to clean water, and poor sanitary habits, therefore they occur wherever there is poverty [4]. Intestinal parasites impact the poorest and most destitute places in tropical and subtropical regions of the world, where they are found in variable degrees of prevalence [5,6]. Nigeria has a high prevalence of intestinal parasites, mostly as a result of poor personal and environmental hygiene, tainted food, and water contamination from improperly disposed of human waste [7].
In Nigeria, the health care system is divided into 3 tiers – primary, secondary and tertiary. There is paucity of data comparing the prevalence of intestinal parasitic infections among the various tiers of healthcare. Against this background, this study aims to determine the prevalence of intestinal parasitic infections among patients accessing care in some secondary and tertiary healthcare facilities in Edo State, Nigeria.
Materials and Methods
Study locations
The study was carried out in three hospitals in Edo State, Nigeria. The hospitals were University of Benin Teaching Hospital (UBTH), Benin City (Egor local government area), located on latitude 6.39040N and longitude 5.61180E, Central Hospital, Benin City (Oredo local government area), located on latitude 6.32980N and longitude 5.62250E, and Irrua Specialist Teaching Hospital (ISTH), Irrua (Esan Central local government area), located on latitude 6.73310N and longitude 6.19050E, all in Edo Sate, Nigeria. UBTH and ISTH are tertiary hospitals while Central Hospital is a secondary hospital. According to the National Population Commission [8], Egor local government area has a population of 340,287; Esan Central local government area, 105,242, while Oredo local government area has a population of 374,515.
Study population
A total of 576 patients consisting of 145 from University of Benin Teaching Hospital, Benin City, 420 from Central Hospital, Benin City and 11 from Irrua Specialist Teaching Hospital, Irrua, with gastrointestinal complaints were recruited for this study. Informed consent was obtained from all subjects or their parents/ guardians in case of children prior to specimen collection. Approval for the study was given by the Ethical Committee of Irrua Specialist Teaching Hospital, Irrua, and that of the Edo State Ministry of Health, Benin City.
Collection and processing of specimen
Stool specimens were collected from each patient into sterile universal container and sent to the laboratory within one hour of collection. The stool specimens were processed to detect intestinal parasites using the formol-ether concentration method as described by Akinbo et al. [9]. Briefly, about 1g of formed stool or about 1ml of watery stool was suspended in 4ml of formol saline and mixed. The mixture was sieved and to the filtrate and 4ml of diethyl ether was added and agitated. The mixture was centrifuged at 3000 rpm for 1min. The faecal debris on the side of the tube was detached using an applicator and the supernatant was discarded. From the deposit, saline and iodine preparations were made and examined microscopically for the presence of parasites using x10 and x40 objectives.
Statistical Analysis
The data obtained were analyzed with Chi square (X2) test and odd ratio analysis using the statistical software INSTAT® (GraphPad Software Inc, San Diego, CA, USA).
Results
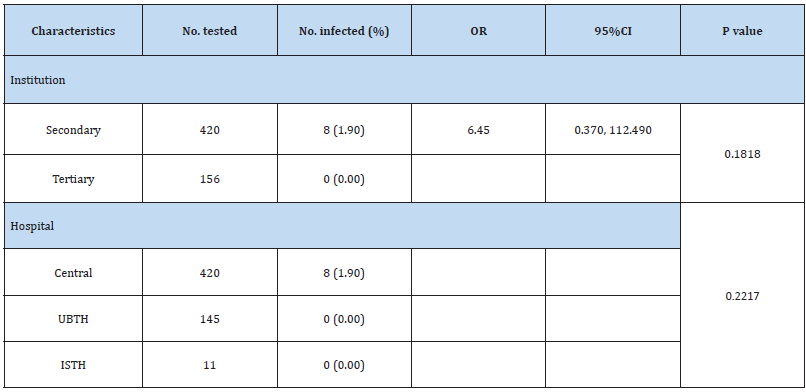
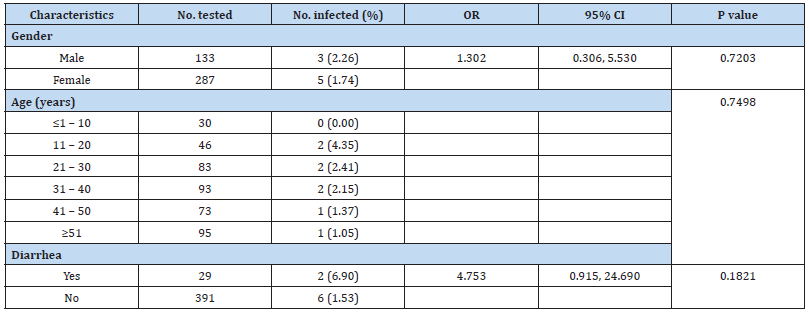
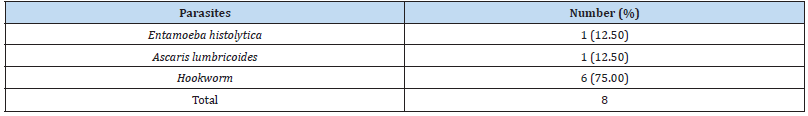
A total of 8 (1.39%) out of the 576 patients with gastrointestinal complaints had parasitic infections. Although intestinal parasites were recovered only from patients accessing care at Central Hospital, Benin City (secondary healthcare facility), location of hospital has no significant (p> 0.05) relationship with the prevalence of intestinal parasitic infections (Table 1). Similarly, gender, age and whether the patient had diarrhoea did not significantly (p> 0.05) affect the prevalence of intestinal parasitic infection (Table 2). Entamoeba histolytica, Ascaris lumbricoides and hookworm were the intestinal parasites recovered in this study with hookworm (75%) being the most prevalent (Table 3).
UBTH: University of Benin Teaching Hospital; ISTH: Irrua Specialist Teaching Hospital
Discussion
A total of 8 (1.39%) out of the 576-stool specimens examined had intestinal parasites, and all were recovered from patients with gastrointestinal complaints accessing care in Central Hospital (secondary health care institution), Benin City. This is lower than the 8.86% previously reported from the same location [10]. Among children with diarrhoea, prevalence of infection varies with geographical locations, regions within the same country, and even over time in the same location and population [11]. This may explain the difference in the prevalence obtained in this study and that of Isibor et al. [10]. A prevalence of 40% intestinal parasitic infection among non-HIV persons was reported in ISTH [12] which is not consistent with the findings in this study. The finding of no intestinal parasites from patients attending University of Benin Teaching Hospital agrees with previous reports [13,14]. Although the patients used in the Imade & Eghafona [13,14] were children, only Cryptosporidium species and Cyclospora species (parasites) were found in the stool. In this study, methods to detect Cryptosporidium and Cyclospora ova were not used. A prevalence of 3.9% of intestinal parasitic infection had earlier been reported among patients of all age groups in UBTH [15]. It may appear that the prevalence of intestinal parasites in UBTH has dropped from 3.9% in 2011 in the Akinbo et al. [15] study to 0% in 2015 in Imade and Eghafona [13] & Imade and Eghafona [14] studies as well as in this study. It is also important to note that the patients accessing care at the tertiary hospitals (UBTH and ISTH) may have been treated at the primary and secondary healthcare levels before being referred to the tertiary hospitals. This may explain the zeroprevalence observed among patients from UBTH and ISTH in this study. However, the type of hospital did not significantly (p=0.2217) affect the prevalence of intestinal parasites.
The finding that gender did not affect the prevalence of intestinal parasitic infection in this study agrees with previous reports among non-HIV patients [9,15-17]. Conflicting reports exists on the effect on age on the prevalence of intestinal parasitic infection. Some studies found higher prevalence within the age group of ≤1 – 10 years [15,19] while other reported increasing prevalence with increasing age [20,21]. In this study, age had no significant (p=0.7479) effect on the prevalence of intestinal parasitic infection. The small number of positive cases may be responsible for this. Although higher prevalence of intestinal parasitic infection was observed among patients with diarrhoea, diarrhoea did not significantly affect the prevalence of intestinal parasitic infection (p=0.1821). This agrees with a previous report [22].
Of the 8 parasites recovered, hookworm (75%) predominated, and this agrees with a previous report [10]. Previous reports from UBTH, ISTH and another tertiary hospital in a rural community of Edo State among HIV and non-HIV subjects indicated that Ascaris lumbricoides was the most prevalent intestinal parasites [12,15- 19,23]. Only one study among diabetic patients reported hookworm as the most prevalent intestinal parasites [9]. The HIV and diabetic statuses of the patients used in this study were not determined. It has been reported that infection with intestinal parasites such as Ascaris lumbricoides and hookworm increases an individual’s risk of developing gastrointestinal disorders [24]. This may indicate that these patients are at increased risk of developing gastrointestinal disorders and may be responsible for the gastrointestinal complaints that brought them to the hospital. Urgent treatment is warranted to prevent further associated sequelae.
Conclusion
In conclusion, a prevalence of 1.39% of intestinal parasitic infections was observed in this study and the parasites were only recovered from patients accessing care in a secondary healthcare facility.
References
- Funso-Aina OI, Chineke HN, Adogu PO (2020) A review of prevalence and pattern of intestinal parasites in Nigeria (2006-2015). European Journal of Medical and Health Sciences 2(1): 1-6.
- World Health Organization (2007) Partners for parasite control: geographical distribution and useful facts and stats. WHO, Geneva, Switzerland.
- Hotez PJ, Fenwick A, Savioli L, Molyneux DH (2009) Rescuing the bottom billion through control of neglected tropical diseases. Lancet 373(9674): 1570e5.
- Steketee RW (2003) Pregnancy, nutrition and parasitic diseases. Journal of Nutrition 133 (5 Suppl 2): 1661S-1667S.
- Speich B, Croll D, Furst T, Utzinger J, Keiser J (2016) Effect of sanitation and water treatment on intestinal protozoa infection: a systematic review and meta-analysis. Lancet Infect Dis 16(1): 87-99.
- Faria CP, Zanini GM, Dias GS, da Silva S, de Freitas MB, et al. (2017) Geospatial distribution of intestinal parasitic infections in Rio de Janeiro (Brazil) and its association with social determinants. PLoS Negl Trop Dis 11(3): e0005445.
- Uzairue LI, Ugbor CI, Ezeah GAC, Eze NO, Nwadike IG (2013) Gastrodiscoides hominis infestation on vegetables (cabbages) sold in Ekpoma markets, Edo State, Southern Nigeria- a case report. IJBAIR 2(2): 37-39.
- National Population Commission (2006) Population and housing census of the Federal Republic of Nigeria.
- Akinbo FO, Olujobi SO, Omoregie R, Egbe CA (2013) Intestinal parasitic infections among diabetes mellitus patients. Biomarkers and Genomic Medicine 5(1-2): 44-47.
- Isibor JO, Ayanlere MK, Eyaufe A (2007) Intestinal parasitic infections in patients attending a government hospital in Benin City, Nigeria. Journal of Parasitic Diseases 31(2): 137-140.
- Petri WA, Miller M, Brinder HJ, Levine MM, Dillingham R, et al. (2008) Enteric infections, diarrhea, and their impact on function and development. Journal of Clinical Investigation 118(4):1277-1290.
- Iyevhobu KO, Obodo BN (2020) Prevalence of parasitic infections in relation to CD4+ and antiretroviral (ART) usage of HIV sero-positive patients attending Irrua Specialist Teaching Hospital (ISTH) Irrua, Edo State, Nigeria. International Journal of Innovative Research and Advanced Studies 7(6): 205-211.
- Imade PE, Eghafona NO (2015a) Microbiological Assessment of Stool Specimens of Children with Diarrhoea in Benin City, Nigeria. British Microbiology Research Journal 9(3): 1-8.
- Imade PE, Eghafona NO (2015b) Microbial agents and associated factors of persistent diarrhoea in children less than 5 years of age in Edo State, Nigeria. British Journal of Medicine and Medical Research 9(4): 1-6.
- Akinbo FO, Omoregie R, Eromwon R, Igbarumah IO, Airueghiomon UE (2011b) Prevalence of intestinal parasites among patients of a tertiary hospital in Benin City, Nigeria. N Am J Med Sci 3(10): 462-464.
- Akinbo FO, Okaka CE, Omoregie R (2010b) Prevalence of intestinal parasitic infections among HIV patients in Benin City, Nigeria. Libyan J Med 5: 5506.
- Akinbo FO, Okaka CE, Omoregie R (2011a) Seasonal variations of intestinal parasitic infections among HIV-positive patients in Benin City, Nigeria. Ethiopian Journal of Health Sciences 21(3): 191-194.
- Akinbo FO, Okaka C, Omoregie R (2012) Plasmodium falciparum and intestinal parasitic co-infection in HIV-infected patients in Benin City, Edo State, Nigeria. Journal of Infections in Developing Countries 6(5): 430-435.
- Oladeinde BH, Omoregie R, Olley M, Anunibe JA, Odia I (2014) Intestinal parasitic infections in rural community of Okada, Edo State, Nigeria: a four-year retrospective study. Healthcare in Low-resource Setting 2(1): 35-37.
- Jamaiah I, Rohela M (2005) Prevalence of intestinal parasites among members of the public in Kuala Lumpur, Malaysia. Southeast Asian J Trop Med Public Health 36(1): 68-71.
- Nduka FO, Nwaugo VO, Nwachukwu NC (2006) Human intestinal parasite infections in Ishiagu, a leading mining Area of Abia State. Animal Research International 3(3): 505-507.
- Huruy K, Kassu A, Mulu A, Worku N, Fetene T, et al. (2011) Intestinal parasitosis and shigellosis among diarrheal patients in Gondar Teaching Hospital, Northwest Ethiopia. BMC Research Notes 4: 472.
- Akinbo FO, Okaka CE, Machado RLD, Omoregie R, Onunu AN (2010a) Cryptosporidiosis among HIV-infected patients with diarrhea in Edo State, Midwestern Nigeria. Malaysian Journal of Microbiology 6(1): 99-101.
- Blitz J, Riddle MS, Porter CK (2018) The risk of chronic gastrointestinal disorders following acute infection with intestinal parasites. Frontiers in Microbiology 9: 17.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.