Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Deformity Correction of Lower Extremities by Application of Ilizarov
*Corresponding author: Imran Khan and Department of Orthopedic and Trauma, Medical Teaching Institute Lady Reading Hospital Peshawar, Pakistan.
Received: June 06, 2023; Published: June 13, 2023
DOI: 10.34297/AJBSR.2023.19.002560
Abstract
Objective: The objective of this study is to evaluate the results of osteotomy and application of Ilizarov of lower limb deformities.
Material and Methods: This is a case series study on 23 patients of either sex that has been conducted in the Department of Medical Teaching Institute Hayatabad Medical Complex and Akbar Medical Center Peshawar from November 2016 to April 2021. The age of the patients was 10 and above. To reduce the bias, we have excluded patients with diabetes mellitus, patients on oral anticoagulants, tobacco addicts and those on steroid or immunocompromised patients. Preoperative deformity was calculated that how much time it will take to correct, so when the deformity is corrected double the time was required for consolidation of the callus at corticotomy site. So, some frames were removed early while others were removed late. All the data were collected with the help of a proforma and then entered SPSS version 20 for analysis [1,2].
Results: There were total 23 patients in which male 9(39.1%) and female were 14(60.9%). The mean age was 19.39 while minimum was 10 and maximum was 40 years. Both sides were involved 6(26.1%) in right while 9(39.1%) was involved in left 8(34.8%) in cases. The deformity was ankle in 4(17.4%), femur in 4(17.4%), knee in 8(34.8%) while tibia was involved in 7(30.4%) cases. Single osteotomy was done in 16(69.6%) while double osteotomy was done in 7(30.4%) cases due to the CORA calculated in two places. Ten (43.5%) cases were totally complication free while there was acceptable residual deformity in 4(17.4%), pin lessening in 2(8.7%), pin tract infection 3(13.0%), and restricted knee movement in 4(17.4%).
Conclusion: Ilizarov External fixator is best for deformity correction in all dimensions and directions if the patient and attendant are complaint otherwise.
Keywords: Deformity, Knee, Ilizarov, Tibia, Varus, Valgus
Introduction
Deformities in upper limbs are well tolerated but in lower limbs it creates a lot of problems and cannot be tolerated. Deformities in children are mostly metabolic but may occur secondary to trauma; either to growth plate or mal-united fracture. In adults the deformities are mostly traumatic that can be the result of mal-united fracture. Deformities can also occur secondary to arthritis either Rheumatoid or osteoarthritis. Deformity in the lower limb changes the mechanical axis of limb that can lead to pain and restriction of movement which ends ultimately in early osteoarthritis of the affected limb. Therefore, correction of deformity in lower limb needs urgent attention to avoid complication. There are a lot of ways to correct it. In children for juxta particular area either temporary or permanent epiphysiodesis of the affected bone can be done in single stage by stapling or plating. But the original challenges come when deformity is found in adults. In adults there are also many surgical procedures to correct the mechanical axis of the lower limb. In acute correction the surgical procedure is opening or closing wedge osteotomy with plating/nailing, but this procedure is not free of complications. Opening wedge needs bone graft and causes lengthening while closing wedge causes shortening but there is one method that neither casues shortening or lengthening or bone grafting with less complication and that is called close osteotomy and application of Ilizarov. With Ilizarov deformity can be corrected gradually without affecting the soft tissues. If there is shortening, it can elongate the bone postoperatively with gradual distraction. There is a special type of frame which is called Taylor Spatial Frame that is computer operated; all the deformity is enter into the software and that calculate how much struts must be rotated for how many days to correct the deformity, but it needs high cost. The one and single most benefit of Ilizarov is that one can correct the deformity post operatively up to his satisfaction which cannot be done with acute correction with osteotomy and plating/nailing. Therefore, the objective of this study is to evaluate the results of osteotomy and application of Ilizarov of lower limb deformities [3].
Material and Methods
This is a case series study on 23 patients of either sex that has been conducted in the Department of Medical Teaching Institute Hayatabad Medical Complex and Akbar Medical Center Peshawar from November 2016 to April 2021. The age of the patients was 10 and above. To reduce the bias, we have excluded patients with diabetes mellitus, patients on oral antiguagulants, tobacco addicts and those on steroid or immunocompromised patients. Patients were admitted from the outpatient department. All the patients that fulfilled the inclusion criterion were counseled for the procedure and written informed consent was taken. All patients have done scanogram of both lower limbs beforehand, the site and magnitude of deformity has been calculated. All the surgery was done by the same consultant. Paper tracing was done, and angle of deformity calculated. Patients were either anesthetized by spinal or general anesthesia. At the time of induction two grams of cephoprazone + sulbactum were given intravenously after test dose. Prefabricated Ilizarov frame that contains hinges, is fixed to the bone with wires and shanz pins [4]. Then 1–2-centimeter incision given over the deformity and closed corticotomy was done with the help of osteotome. The rings were loosened to check that corticotomy is complete or vice versa. The wound is closed, antiseptic dressing done and the patient shifts to orthopedic unit after full recovery. On the day of discharge from unit, patient was instructed for follow up, daily dressing and about distraction. Patient and attendant were instructed to rotate the nuts of two hinges on the concave side of deformity after two weeks of operation, half turn in morning and half turn in evening. Patients were followed up at 2 weeks, 6 weeks, 10 weeks, 14weeks, six months and ninth months while some needed one year follow up. At final follow up scanogram or x ray of the affected limb was done to check the correction Preoperative the deformity was calculated that how much time it will take to correct, so when the deformity is corrected double the time was required for consolidation of the callus at corticotomy site. So, some frames were removed early while others were removed late. All the data were collected with the help of a proforma and then entered SPSS version 20 for analysis [5-14].
Results
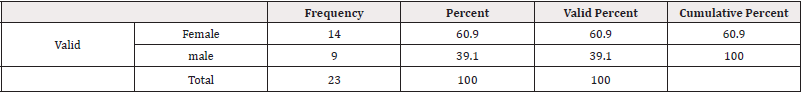
There was total 23 patients in which male 9(39.1%) and female were 14(60.9%) (Table 1).
The mean age was 19.39 while minimum was 10 and maximum was 40 years (Table 2).
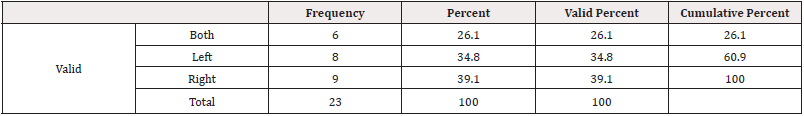
Both sides were involved 6(26.1%) in right while 9(39.1%) was involved in and left 8(34.8%) in cases (Table 3).
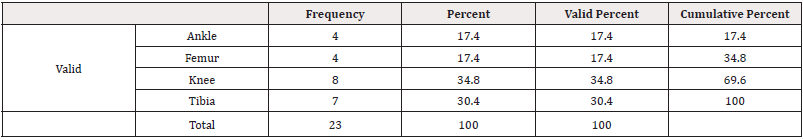
The deformity was ankle in 4(17.4%), femur in 4(17.4%), knee in 8(34.8%) while tibia was involved in 7(30.4%) cases (Table 4).
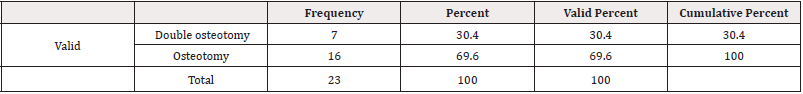
Single osteotomy was done in 16(69.6%) while double osteotomy was done in 7(30.4%) cases due to the CORA calculated in two places (Table 5).
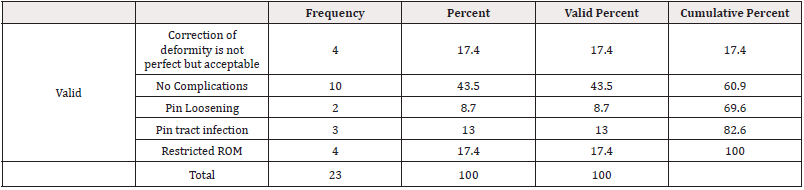
Ten (43.5%) cases were totally complication free while there was acceptable residual deformity in 4(17.4%), pin lessening in 2(8.7%), pin tract infection 3(13.0%), and restricted knee movement in 4(17.4%) (Table 6).
Discussion
Valgus/varus malalignment of the lower limbs is considered normal in kids under six years of age. After age 8 years, little correction in alignment is expected, and treatment for excessive physiological valgus may be needed [15]. There are many conditions which may be responsible for pathological genu valgum such as post traumatic, metabolic disorders (rickets), post infections, various forms of dysplasias, and secondary to tumor like conditions such as fibrous dysplasia and enchondromatosis [16]. Radiological evaluation is mandatory in children with excessive genu valgum. Valgus deformity may progress and become symptomatic. In such cases the knees may rub, child walks with awkward gate and may develop lateral patellar subluxation [17,18].
Corrective osteotomy for excessive genu valgum is appropriate when the patient presents near or after skeletal maturity. Usually, a contoured compression plate is required to achieve stability, but a blade plate is preferred [19]. Varus osteotomy has been proved as an effective treatment option if good correction is achieved [20]. By taking a wedge from the medial supracondylar area a stable construction is achieved, fixation of the osteotomy with a 90° blade plate provides intrinsic stability [21]. An ordinary 90° plate with offset, normally used in intertrocanteric osteotomies, provides the necessary extra stability for early mobilization of the patient. Tibial medial closing wedge osteotomy may be a suitable surgical choice when a small correction is required [22]. No graft is required and healing generally occurs in four weeks from surgery. This study, supported by Coventry [23]. Chambat, et al. [24] and Marti and Verhagen [25]. a joint surface tilt of 10° in the coronal plane is well tolerated.
In the current study there are a total of 23 patients with Ilizarov. All osteotomies were opening wedge followed by Ilizarov ring fixator. Hundreds of percent correction was achieved in 19 patients (82.6%) in terms of deformity correction, knee range of motion, leg length discrepancy and union at osteotomy site. Complications in our study were pin lessening in 2(8.7%), pin tract infection 3(13.0%), and restricted knee movement in 4(17.4%).
Conclusion
Ilizarov External fixator is best for deformity correction in all dimensions and directions if the patient and attendant are complaint otherwise. Physiotherapy and exercises can prevent many complications and make it a success.
Acknowledgments
None.
Conflict of Interest
None.
References
- Kirienko A, Gradov L, Malagoli E, Tacci F, Lucchesi G (2022) Correction of a Complex Foot Deformity with V and Y Osteotomy and Ilizarov Method. J Foot Ankle Surg S1067-2516(22): 00050-00053.
- Popkov A, Dučić S, Lazović M, Lascombes P, Popkov D (2019) Limb lengthening and deformity correction in children with abnormal bone. Injury 50 Suppl 1: S79-S86.
- Matsushita T, Watanabe Y, Takenaka N, Miyamoto W, Kawano H (2021) Correction of equinus deformity by means of a new unconstrained ilizarov frame system. Injury 52(7): 2006-2009.
- Patel I, Young J, Washington A, Vaidya R (2022) Malunion of the Tibia: A Systematic Review. Medicina (Kaunas) 58(3): 389.
- Sharma A, Cherian RJ, Pandey RA, Khatter H, Paul R, et al. (2022) Clinico-Radiological and Functional Outcome of Difficult Talipes Equinovarus Deformity Corrected with an Ilizarov Fixator. J Foot Ankle Surg 61(4): 719-725.
- Bakircioglu S, Caglar O, Yilmaz G (2021) Multiplanar correction of proximal tibial recurvatum deformity with tibial osteotomy and computer assisted fixator Knee 32: 159-165.
- Hou N, Zhang H, Bai M, Chen H, Song W, Wang L (2020) The Old Supracondylar Fracture of Femur Treated by Gradual Deformity Correction Using the Ilizarov Technique Followed by the Second-Stage Internal Fixation in an Elderly Patient with Osteoporosis. Geriatr Orthop Surg Rehabil 11: 2151459320931673.
- Mayer SW, Hubbard EW, Sun D, Lark RK, Fitch RD (2019) Gradual Deformity Correction in Blount Disease. J Pediatr Orthop 39(5): 257-262.
- Wen XD, Liang XJ, Zhang Y, Liang JQ, Liu PL, et al. (2021) Ilizarov Gradual Distraction Correction for Distal Tibial Severe Varus Deformity Resulting from Epiphyseal Fracture: Case Report and Literature Review. J Foot Ankle Surg 60(1): 204-208.
- Bliven EK, Greinwald M, Hackl S, Augat P (2019) External fixation of the lower extremities: Biomechanical perspective and recent innovations. Injury 50 Suppl 1: S10-S17.
- Calder PR, Faimali M, Goodier WD (2019) The role of external fixation in paediatric limb lengthening and deformity correction. Injury 50 Suppl 1: S18-S23.
- Kwon KB, Chung CY, Park MS, Lee KM, Sung KH (2021) Lengthening and deformity correction in vascularized fibular autograft for a patient with Ewing sarcoma. J Orthop Surg (Hong Kong) 29(3): 23094990211044549.
- Morasiewicz P, Burzyńska K, Orzechowski W, Dragan SŁ, Dragan SF, et al. (2018) Three-dimensional printing as a technology supporting the treatment of lower limb deformity and shortening with the Ilizarov method. Med Eng Phys 57: 69-74.
- Kirienko A, Malagoli E (2021) Ilizarov Technique in Severe Pediatric Foot Disorders. Foot Ankle Clin 26(4): 829-849.
- Stevens PM, Maguire M, Dales MD, Robins AJ (1999) Physeal stapling for idiopathic genu valgum. J Pediatr Orthop 19(5): 645-649.
- Herring JA, Tachdjian S (2002) pediatric orthopedics. 3rd ed. Philadelphia, London, New York, St Louis, Sydney, Toronto: WB Saunders Company pp. 839-890.
- Staheli LT (1990) Lower positional deformity in infants and children: a review. J Pediatr Orthop 10(4): 559-63.
- Thempson GH (2001) Angular deformities of the lower extremities in childhood. In: Chapman MR Edn. Chapman, s orthopedic surgery. 3rd Philadelphia, Baltimore, New York, London, Buenos Aires, Hong Kong, Sydney, Tokyo, Lippincott Williams & welkins pp. 4287-4335.
- Schoenecker PL, Rich MM In: Lowell and Winter’s paediatric orthopaedics. 5th Lippincott Williams and Wilkins.
- Zilber S, Larrouy M, Sedel L, Nizard R (2004) Distal femoral varus osteotomy for symptomatic genu valgum: long-term results and review of the literature [in French]. Rev Chir Orthop Reparatrice Appar Mot 90: 659-665.
- Marti RK, Schroder J, Witteveen A (2000) The closed wedge varus supracondilar osteotomy. Oper Tech Sports Med 8: 48-55.
- Puddu G, Cipolla M, Cerullo G, Franco V, Giannì E (2010) Which osteotomy for a valgus knee? Int Orthop 34(2): 239-247.
- Coventry MB (1987) Proximal tibial varus osteotomy for osteoarthritis of the lateral compartment of the knee. J Bone Jt Surg Am 69: 32-38.
- Chambat P, Ait Si Selmi T, Dejour D (2000) Varus tibial osteotomy. In: Osteotomies about the athletic knee. Oper Tech Sports Med 8: 44-47.
- Marti RK, Verhagen RAW (2001) Upper tibial osteotomy for osteoarthritis of the knee. Surg Techn Orthop Traumatol 55-530-A-10.




 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.