Opinion 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Time for a Change: The End of the Pharmacracy
*Corresponding author: Rodney R Dietert, Professor Emeritus of Immunotoxicology, Cornell University, Mailing address: c/o 10035 E. Tristan Dr., Hereford, AZ 85615 USA, Tel: 6072209848.
Received: September 21, 2023; Published: October 09, 2023
DOI: 10.34297/AJBSR.2023.20.002692
Abstract
Recent and ongoing experiences with the SARS-CoV-2 pandemic have put on full display the spider web of Pharma-linked bureaucratic institutions that adhere to, promote, and even enforce the mantra: “Pharma Living is the Life for Me”. The problem is, as will be illustrated in this opinion article, we have not been living better with a Pharma-filled life. From pregnancy to birth, through childhood and beyond, our illness-filled lives are driven by the “unintended consequences” of drugs that rarely if ever cure the target disease. Adverse effects become new medically coded diseases that require additional drug treatments which, in turn, result in multimorbidity and polypharmacy earlier and earlier in life.
Many prescription drugs (e.g., statins) are designed for life-long consumption. The childhood appearance of what used to be considered adult-onset chronic diseases has reduced the healthspan even as most infants begin a vaccine- and drug-dominated life shortly after birth. All of this happened while Pharma along with its co-partners (the Pharmacracy) spent at least a half-century working to cure chronic diseases. That effort failed. It is time for change. As this opinion article points out, there are better, more personalized and holistic alternatives. As individuals and human holobionts, we need the freedom and institutional support to pursue the alternatives.
Keywords: Pharmacracy, Pharma-Institutional Complex, Chronic diseases, Multimordbidity, Polypharmacy, Adverse effects, Safety regulation, Human holobiont, Healthspan
Abbreviations: PIC: Pharma-Institutional Complex; AMA: American Medical Association; FDA: Food and Drug Administration; WHO: World Health Organization; CDC: Centers for Disease Control and Prevention
Introduction
The Pharmacracy, the pharmaceutical industry and its many public and private connections was introduced in a recent article illustrating the benefits of dietary approaches as a pharma alternative to prevent and/or treat chronic diseases and polypharmacy [1]. The reach of the Pharmacracy is extensive. Its global growth over the past several decades has been impressive. But regrettably, its long-term impact on human health has been beyond problematic. For this reason, it is time to focus on the long-standing promises of the Pharmacracy, the abject failure of its effort to better human health, and the need to change our system to facilitate the well-being and survival of humanity.
In this opinion article, I:
a) further delineate the nature of the Pharmacracy,
b) describe its impact on human civilization, and
c) argue that Pharmacracy must end if we are to follow a path of human wholeness, wellness, and freedom.
Figure 1 illustrates the Pharmacracy in a depiction of nine circles of Pharma’s operation, connections, and influence. It is so prevalent that it is not surprising that alternatives to a Pharma-driven life have had an uphill fight to break through the matrix of western medicine, medical education, and public health administration. There is a clear pharma-institutional complex (PIC) in place. Pharma has a long history of generosity in financially supporting various research and educational programs as well as sponsoring meetings, continuing medical education and conferences that are part of its vast and varied connections [2-5]. It has also utilized a fleet of representatives that routinely visit doctors’ offices. These visits have impact but not all of them are positive for the patient [6]. With this in mind, it is important to recognize the range of the Pharmacracy and the scope of its business model. At least part of the business model involves the flow of professionals among the public and private sectors including a larger group of contractor companies and individual and group consultants. As might be expected, the issue of revolving doors and potential conflict of interest is ever present (Figure 1).
Revolving Doors
One of the concerning issues that has come to the forefront is the revolving door that appears to exist between Pharma, the business, and the Food and Drug and Administration (FDA), the US agency charged with regulating that business. This problem has been raised by numerous authors [7-9]. The problem with appropriate, unbiased drug evaluation for safety and efficacy is not only an issue in the US but also in other countries. One of the regulatory examples from the UK involves the drug Vioxx [10], which also had repercussions in the US. In this case, regulatory oversight to ensure safety was thrown out the window and many deaths resulted from cardiovascular events [11,12]. As part of the Pharmacracy, public health institutions have also had their share of failures as was recently documented [13].
Chronic Diseases as a Growth Industry
Chronic diseases are by far and away the leading cause of global death [14] and are a true blight on human society. These diseases shift us from a life course of wellness and wholeness onto a track of accumulating diseases and disabilities [15]. Early-life onset diseases such as asthma and obesity have a highly predictable elevated risk of specific comorbid chronic diseases [16]. The main job of the Pharmacracy was to cure these diseases and reverse the chronic disease epidemic. In this prime directive, it has stunningly failed.
A point emphasized in Dietert [1] is that pharma-directed medicine has a poor track record when it comes to the prevention and/ or treatment of chronic diseases (previously known as noncommunicable diseases). During the decades-long period when pharmaceuticals have been the most prevalent approach to addressing chronic diseases, there have been few cures and, in fact, an expansion in the numbers and prevalence of chronic diseases [17-19]. As Dieppe [20] pointed out, a medical focus on targeting symptoms rather than causes of chronic diseases is a significant problem relative to “cures.” Menditto et al. describe the disturbing relationship between drugs and multimorbidity plus polypharmacy in chronic diseases [21]. In effect, chronic diseases beget more chronic diseases with many pharmaceutical treatments doing little to prevent the disease propagation that occurs across the lifespan. Adverse drug interactions become more likely as polypharmacy occurs [22].
Does Safety Include the Microbiome?
By several criteria, the human holobiont is mainly microbial rather than mammalian. In addition, the human microbiome directs both the maturation and function of our physiological systems [23], and the status of the human microbiome is important in determining health vs. disease [24]. With this in mind, one of the interesting questions regarding drug safety concerns the human microbiome. Numerous studies have shown that the status of the microbiome and in particular, the human gut microbiome, significantly affects the risk of chronic diseases [16,25,26]. This becomes even more significant when one considers that protection for the microbiome from toxic xenobiotics (e.g., environmental chemicals, food additives and drugs) is a recent concern [27]. Numerous food additives/ chemicals and drugs have been shown to damage the microbiome [28-31]. Yet, these microbial toxicants have yet to be dealt with by regulatory agencies such as the FDA, and consumers/patients are generally not aware of the dangers.
One Health: The Upside and the Downside
The concept of One Health has been an easy idea to support. The concept that there should be better flow of health information across species such that breakthroughs in human health can eventually benefit animal health and the reverse as well. Because the author spent most of his career in the College of Veterinary Medicine (Cornell University), One Health seemed like a logical and highly beneficial concept. What is now apparent is that One Health strongly supports Pharmacracy. The reason for this is that several major human Pharma companies either directly own or have a stake in (spinoffs) the major animal health/drug companies. Examples would be Pfizer spinning off Zoetis, Eli Lilly spinning off Elanco, while Boehringer, Merck and Bayer have direct animal health divisions.
But the control of animals is not just health. It can lead to the fundamental breeding stock. In this way Pharma can design the animal used for producing food, develop all the vaccines and drugs used to manage food and companion animal health, then produce the drugs to treat humans following consumption of pharma-originated, pharma- tailored food. That might be called an integrated business model. Is it easy to predict human illness and future required drugs and vaccines if one also breeds and guides production of the food consumed? It is also possible for the Pharmacracy to easily transfer the application of herd management strategies from production animals to humans. The only requirements for the onesize- fits-all herd approach for Covid 19 is that public health officials ignore the much-touted significance of personalized medicine and also forsake the mantra that children are not simply small adults.
How Fear Mongering Pays Off
Disease mongering to sell drugs is not necessarily a new thing. Wolinsky covered the topic more than a decade ago [32]. But with SARSCoV-2 (Covid 19) there was what has been termed a “Pandemic Panic” [33]. The recent Covid 19 pandemic was filled with lockdowns and mandates for the healthy that more resembled a 21st century form of Lysenkoism than state-of-the-art science [34]. Support for natural immunity and the human microimmunosome, the combination of the microbiome, the gut barrier, plus adjacent immune system [35], was virtually ignored and compliance was the watchword for the day for the myriad of public health mandates.
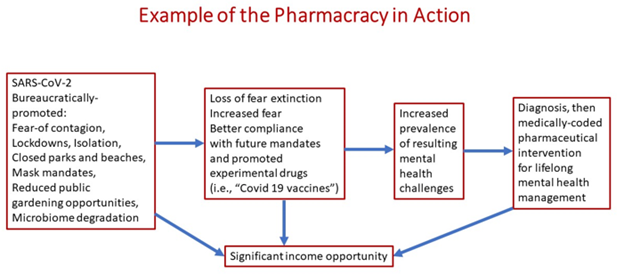
To ensure compliance, fear-of-contagion was promoted though a variety of media. One of the factors that was important in achieving a herd-like compliance among many was the loss of balanced fear. Part of the concern about mandates was damage to the microbiome [36]. The author was among those reviewing the fact that microbiome erosion results in an unbalanced and pervasive fear because the gut microbiome controls fear extinction [37]. Loss of fear extinction results not only in greater compliance but can also lead to a predictable cadre of mental health challenges [38-42]. Figure 2 depicts a diagram of the path from fear-of-contagion through mandate compliance to mental health disease and pharmacologic- based therapy.
In the case of the Covid 19 pandemic, persistent public health fear mongering not only increased herd-like compliance but also increased the prevalence of additional chronic diseases and conditions and accompanying drug treatment. It is a Lysenkoism redux where government bureaucrats promote questionable science resulting in unneeded death. The remaining question at present is whether fear-of-contagion marketing and promotion will produce the same negative outcomes with the 2023 version of Covid 19 as was seen during the original pandemic.
Conclusions
Pharma has had more than a half-century in which to reduce the prevalence of chronic diseases and the need for drugs to treat these conditions. By all measures of these diseases including multimorbidity and polypharmacy it has failed. This failure has come despite the able assistance of virtually every Western health-oriented institution. The best chance imaginable produced the poorest outcome possible short of population extinction. Admittedly, major success by Pharma across much of the 20th century and all of the 21st century would have led to severely reduced demand for their products. Additionally, it would likely have reduced demand for a broad range of health services. It is understandable that the continuing growth of Pharma requires the continued growth of chronic diseases.
But now it is time for the Pharmacracy to step aside and allow medical doctors to return to the Hippocratic Oath rather than an operational replacement for some: the Pharmacratic Oath. The Pharmacracy void can be filled with both ancient and completely new approaches to health designed to recapture personalized and holistic health care. The patient is a multi-species holobiont. There is no single species to herd toward Pharma’s experimental drugs.
Conflict Of Interest
The author declares that there is no conflict of interest. There was no financial support for the preparation or content of this paper.
References
- Dietert RR (2023) Dietary Approaches from Moms, Farms, and Nature to Overcome Chronic Diseases and the Pharmacracy. Nutrients 15(18): 3965.
- Barton L (1994) Ethics, Profit and Patients. J Hospital Market 8(1): 71-82.
- Komesaroff PA, Kerridge IH (2002) Ethical issues concerning the relationships between medical practitioners and the pharmaceutical industry. Med J Australia 176(3): 118-121.
- Rogers WA, Mansfield PR, Braunack‐Mayer A J, Jureidini JN (2004) The ethics of pharmaceutical industry relationships with medical students. Med J Australia 180(8): 411-414.
- Brody H (2009) Pharmaceutical industry financial support for medical education: benefit, or undue influence? J Law Med Ethics 37(3): 451-460.
- Mintzes B, Lexchin J, Sutherland JM, Beaulieu MD, Wilkes MS, et al. (2013) Pharmaceutical Sales Representatives and Patient Safety: A Comparative Prospective Study of Information Quality in Canada, France and the United States. J Gen Intern Med 28(10): 1368-1375.
- Karas L (2023) FDA’s revolving door: reckoning and reform. Stanford Law & Policy Rev 34(1): 1-66.
- Demasi, M (2022) From FDA to MHRA: are drug regulators for hire? BMJ 377.
- Aaron D (2023) The Fall of FDA Review, Yale J. Health Policy, Law, and Ethics, Forthcoming 2023, University of Utah College of Law Research 545.
- Heim E, Moxon S (2023) Mechanisms of regulatory capture: Testing claims of industry influence in the case of Vioxx. Regulat. Govern. Early View 1-19.
- Horton R (2004) Vioxx, the implosion of Merck, and aftershocks at the FDA. The Lancet 364(9450): 1995-1996.
- Krumholz HM, Ross JS, Presler AH, Egilman DS (2007) What have we learnt from Vioxx?. BMJ 334(7585): 120-123.
- Dietert RR (2021) Microbiome First Approaches to Rescue Public Health and Reduce Human Suffering. Biomedicines 9(11): 1581.
- World Health Organization (2023) Fact Sheets: Noncommunicable Diseases.
- Dietert RR, DeWitt JC, Germolec DR, Zelikoff JT (2010) Breaking patterns of environmentally influenced disease for health risk reduction: immune perspectives. Environ Health Perspect 118(8): 1091-1099.
- Dietert RR (2021) Microbiome first medicine in health and safety. Biomedicines 9(9): 1099.
- Horton R (2005) The neglected epidemic of chronic disease. The Lancet 366(9496): 1514.
- Holman HR (2020) The relation of the chronic disease epidemic to the health care crisis. ACR Open Rheumatol 2(3): 167-173.
- Piovani D, Nikolopoulos GK, Bonovas S (2022) Non-Communicable Diseases: The Invisible Epidemic. J Clin Med 11(19): 5939.
- Dieppe P (2000) To cure or not to cure, that is not the question. J Royal Soc Med 93(12): 611-613.
- Menditto E, Gimeno Miguel A, Moreno Juste A, Poblador Plou B, Aza Pascual-Salcedo M, et al. (2019) Patterns of multimorbidity and polypharmacy in young and adult population: Systematic associations among chronic diseases and drugs using factor analysis. PLoS ONE 14: e0210701.
- Sheikh-Taha M, Asmar M (2021) Polypharmacy and severe potential drug-drug interactions among older adults with cardiovascular disease in the United States. BMC Geriatr 21(1): 233.
- Robertson RC, Manges AR, Finlay BB, Prendergast AJ (2019) The human microbiome and child growth-first 1000 days and beyond. Trends Microbiol. 27(2): 131-147.
- Wang B, Yao M, Lv L, Ling Z, Li L, et al. (2017) The human microbiota in health and disease. Engineering 3(1): 71-82.
- Hills RD, Pontefract BA, Mishcon HR, Black CA, Sutton SC, et al. (2019) Gut microbiome: profound implications for diet and disease. Nutrients 11(7): 1613.
- Haran JP, Mc Cormick BA (2021) Aging, frailty, and the microbiome—how dysbiosis influences human aging and disease. Gastroenterology 160(2): 507-523.
- Dietert RR, Silbergeld EK (2015) Biomarkers for the 21st century: listening to the microbiome. Toxicol Sci 144(2): 208-216.
- Maier L, Pruteanu M, Kuhn M, Zeller G, Telzerow A, et al. (2018) Extensive impact of non-antibiotic drugs on human gut bacteria. Nature 555(7698): 623-628.
- Spanogiannopoulos P, Turnbaugh PJ (2018) Broad collateral damage of drugs against the gut microbiome. Nat Rev Gastroenterol Hepatol 15(8): 457-458.
- Bjarnason I, Rainsford KD (2021) NSAID-enteropathy and intestinal microbes. Inflammopharmacol 29(1): 1-4.
- Bancil AS, Sandall AM, Rossi M, Chassaing B, Lindsay JO, et al. (2021) Food additive emulsifiers and their impact on gut microbiome, permeability, and inflammation: mechanistic insights in inflammatory bowel disease. J Crohn's Colitis 15(6): 1068-1079.
- Wolinsky H (2005) Disease mongering and drug marketing. EMBO Reports 6(7): 612-614.
- Mertens G, Lodder P, Smeets T, Duijndam S (2023) Pandemic panic? Results of a 14-month longitudinal study on fear of COVID-19. J. Affect. Disord 322: 15-23.
- Dietert RR (2021) The microbiological basis of human superorganism freedom. Am J Biomed Sci Res 13(6): 653-662.
- Dietert RR (2017) The microbiome-immune-host defense barrier complex (microimmunosome) and developmental programming of noncommunicable diseases. Reprod. Toxicol 68: 49-58.
- Finlay BB, Amato KR, Azad M, Blaser MJ, Bosch TC, et al. (2021) The hygiene hypothesis, the COVID pandemic, and consequences for the human microbiome. Proc Nat Acad Sci USA 118(6): e2010217118.
- Dietert RR, Dietert JM (2023) The Human Superorganism: Using Microbes for Freedom vs. Fear. Appl Microbiol 3(3): 883-905.
- Beckers T, Hermans D, Lange I, Luyten L, Scheveneels S, et al. (2023) Understanding clinical fear and anxiety through the lens of human fear conditioning. Nat Rev Psychol 2(4): 233-245.
- Baldi E, Savastano S (2021) Fear of Contagion: One of the Most Devious Enemies to Fight during the COVID-19 Pandemic. Disaster Med. Public Health. Prep 15: e8-e9.
- Chu C, Murdock MH, Jing D, Won TH, Chung H, et al. (2019) The microbiota regulate neuronal function and fear extinction learning. Nature 574: 543-548.
- Luijten MA, Van Muilekom MM, Teela L, Polderman TJ, Terwee CB, et al. (2021) The impact of lockdown during the COVID-19 pandemic on mental and social health of children and adolescents. Qual. Life Res 30(10: 2795-2804.
- Wilson DR, Binford L, Hickson S (2023) The Gut Microbiome and Mental Health. J Holist Nurs.




 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.