Case Report 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Utilization of Donor Round Ligament During Liver Transplantation
*Corresponding author: Atta Nawabi, The University of Kansas Medical Center, Department of Surgery, USA.
Received: December 14, 2023; Published: December 20, 2023
DOI: 10.34297/AJBSR.2023.20.002780
Abstract
Liver transplantation offers definitive treatment for patients with end-stage liver disease or those who meet criteria for hepatocellular carcinoma. With advancements in the medical field many common complications of liver transplantation have decreased substantially. Post-operative complications generally are categorized as biliary or vascular in nature [1]. Vascular complications remain one of the most dreaded complications following liver transplant. Hepatic artery thrombosis/dysfunction has been the most common vascular complication with a high mortality, morbidity, and graft loss. A compromised inflow via the hepatic artery not only affects hepatocyte perfusion but also progress to ischemic biliopathy and subsequent liver allograft failure. This article discusses a single center’s technique that has been utilized donor round ligament during liver transplantation to support hepatic artery in over 100 cases of liver transplantations recipients.
Keywords: Liver transplant, Hepatic artery stenosis, Hepatic artery thrombosis, Round ligament
Introduction
Orthotopic liver transplantation remains the only definitive treatment for patients with End Stage Liver Disease (ESLD) [2]. There are many complications associated with the liver transplant but hepatic artery stenosis, thrombosis, pseudoaneurysm and bleeding remain one of the most feared complications due to a high incidence of both graft loss and mortality [3]. The incidence of vascular complications varies from center to center but typically remains around 7% [3]. Diagnosing and treating of these complications remains a major challenge to ensure of the allograft function [3]. Many transplant centers utilize early surveillance of the allograft via doppler ultrasonography which allows for early detection of vascular compromise before inevitable graft failure. The most common vascular complications include hepatic artery thrombosis and portal vein thrombosis [3]. Such complications can interrupt the blood supply to the liver allograft and biliary system resulting graft loss. Treatment modalities of such complications involve surgical revascularization, percutaneous thrombolysis, percutaneous angioplasty, re transplantation, and conservative management. Thus far there has been little to no data of surgical techniques to help prevent or decrease the incidence of such dread complications specifically regarding the hepatic artery. Though the Liver retains dual blood supply via the portal vein and hepatic artery, the hepatic artery plays a vital role in supplying oxygenated blood to both the liver parenchyma and biliary trees. This paper focuses on a surgical technique to reduce hepatic artery complications.
Here at the University of Kansas Medical Center (KUMC)’s Center of Transplantation, we employed an innovative technique by utilizing the donor’s round ligament during liver transplant place it between the hepatic artery and bile duct anastomosis. This simple technique not only support and prevent hepatic artery kinking but also separate bile duct from the hepatic artery anastomosis and potentially prevent formation of pseudoaneurysm (Figure 1).
Surgical Technique
Liver transplantation is one of the most complex surgical procedures. The first step is to performed recipient hepatectomy whether with standard or piggyback techniques. The second step is to performed liver allograft transplantation with supra hepatic vena cava, portal vein, hepatic arteries and then bile ducts anastomosis.
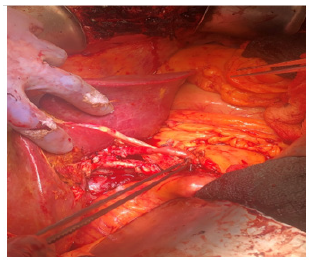
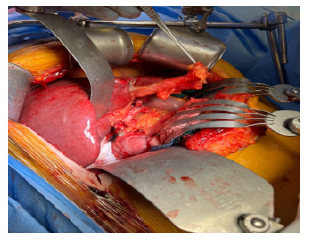
The technique that we are describing is the utilization of the donor round ligament at the time of liver Transplantation. First the donor round ligament preserved with its entire length at the time of organ procurement. After completion of liver transplantation, the donor round ligament brings without tension and place it from left to Right or Right to left between the hepatic artery and bile ducts anastomosis (Figures 2,3).
This simple technique will prevent the hepatic arterial anastomosis from kinking, reduces the risk of postoperative bleeding and hepatic artery pseudoaneurysm due to bile leak and allograft dysfunction (Figure 4).
Discussion
Hepatic arterial integrity is critical for optimal patient and liver allograft outcomes post-liver transplantation. Hepatic Artery Stenosis (HAS) is a devasting complication that occurs around 3.1- 7.4% of patients [4]. HAS is important to detect and treat early on due to the propensity to progress to hepatic artery thrombosis leading to graft dysfunction and biliary complications such as ischemic biliopathy [4]. Treatment of HAS with either surgery, angioplasty, stenting, that puts patients at increased risk for further complications. Employing our technique with the utilization of the donor round ligament allows for an effective means to reduce the risk of developing such a devastating vascular complication.
In our institution we have had success in preventing such complications with over 100 liver transplants thus far. We strongly believe our technique provides a safe, effective, and easily reproducible maneuver to potentially prevent hepatic artery complications following liver transplantation. We plan to continue to collect data to provide further evidence of the effectiveness of our technique with hope of standardizing our method across other institutions while also providing insight into other avenues to optimize organ transplantation.
Acknowledgement
None.
Conflict of Interest
None.
References
- Craig EV, Heller MT (2021) Complications of liver transplant. Abdom Radiol (NY) 46(1): 43-67.
- Sudan DL, Shaw BW (1997) The role of liver transplantation in the management of portal hypertension. Clin Liver Dis 1(1): 115-120.
- Piardi T, Lhuaire M, Bruno O, Memeo R, Pessaux P, et al. (2016) Vascular complications following liver transplantation: A literature review of advances in 2015. World J Hepatol 8(1): 36-57.
- Barahman M, Alanis L, Di Norcia J, Moriarty JM, McWilliams JP (2020) Hepatic artery stenosis angioplasty and implantation of Wingspan neurovascular stent: A case report and discussion of stenting in tortuous vessels. World J Gastroenterol 26(4): 448-455.





 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.