Review article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Rocky Mountain Spotted Fever: A Review and Clinical Applications Amid Case Incidences in Southern California
*Corresponding author:Leonard Ranasinghe, Professor of Emergency medicine and M4 Director, California North state University College of Medicine, Elk Grove, California 95757.
Received: February 04, 2024; Published: February 09, 2024
DOI: 10.34297/AJBSR.2024.21.002855
Abstract
Rocky Mountain Spotted Fever (RMSF) is a bacterial infection of human cells, primarily endothelial, which can result in extensive tissue and organ damage. The etiologic agent of RMSF is the bacteria Rickettsia rickettsii, which spreads to humans through the bite of an infected tick. An identifying symptom is a cutaneous rash. Characterized by pink macules, the rash can spread over the extremities, and be a hallmark feature of the infection. RMSF often presents non-specifically in the first couple few days, with a fever and body aches, posing a diagnostic challenge to clinicians when a rash is non-existent. Previous epidemiologic reports located RMSF cases to specific regions of the Rocky Mountains, the Southwestern United States, and Northern Mexico. Northern Mexico faced an epidemiologic crisis in 2015 due to RMSF, which should concern to United States residents. A recent set of RMSF cases in Southern California has been attributed to travel between Southern California and Tecate, Mexico. The CDC (Center for Disease Control) is concerned about the porous nature of the US Mexico Border and the potential public health crisis that could result through transborder movement. An overview of RMSF and its potential to spread will be analyzed through clinical reports from the National Library of Medicine (NIH) across multiple age and geographic profiles.
Keywords: Rocky mountain spotted fever, Rickettsia rickettsii, Bacterial infection
Introduction
Rocky Mountain Spotted Fever (RMSF) is a bacterial infection of animal cells, primarily endothelial. The bacteria Rickettsia rickettsii is the source of this infection as it invades the human immune system and can cause severe illness and death if specific antibiotics are not administered in a given window. Rickettsia rickettsii, as an obligate intracellular species, accesses host eukaryotic cells and can damage major organs: heart, kidneys, brain, and gastrointestinal. Clinical impacts of host endothelial invasion and damage to vascular tissue by the bacteria are notable. RMSF notably has a mortality rate of up to twenty-five percent if not diagnosed and appropriately treated with antibiotics. The infection results when tick vectors such as the Rocky Mountain Wood Tick and Brown Dog Tick, transmit the bacteria. As infection spreads, patients often present non-specifically with fevers, headaches, and gastrointestinal symptoms. A distinct cutaneous rash, characterized by a spotted red pattern, may result due to Rickettsia’s invasion of endothelial cells and blood vasculature. This condition is challenging to diagnose without a rash in combination with other symptoms. Furthermore, the challenge persists if the patient does not report exposure to a tick or geographic region such as the Rocky Mountains [1]. In December 2023, five individuals from Southern California were infected with RMSF, warranting a public health concern by CDC officials when three of the patients died as a result [2]. The patients noted travel to or being in Tecate, Mexico, only a few weeks before symptom onset. It is critical to understand the origins of RMSF, which typically does not originate in California. Recent cases in Southern California facilitate a discussion about the origins of Rickettsia, its structural characteristics, clinical presentation, and treatment options. Reviewing Rocky Mountain Spotted Fever is inherent as the CDC mounts concern for more cases to emerge in Southern California, considering transborder movement from Mexico (Figure 1).
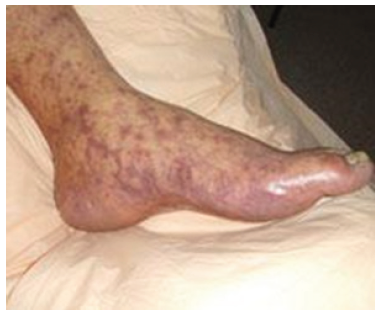
Figure 1: Center for Disease Control 2024, Image depicts characteristic RMSF rash. Rash extends from the lower extremities upwards. Red and purple macules characterize the rash. https://www.cdc.gov/rmsf/symptoms/index.html.
Rickettsia rickettsii, as an obligate intracellular anaerobe, poses significant health risks to humans. The ability of this bacterium to survive depends on access to a host cell's nutrients. Ticks are an optimal transmission vector for diseases because they are hematophagous. Their search for host blood as a nutrition source forces them to contact human skin, where they use blade-like structures to puncture the epidermis. Next, they employ their salivary glands to secrete a thick substance, which has two benefits. The salivary secretion of ticks allows them to attach to hosts and induce hemorrhage [3]. As the tick feeds on host blood, the bacterium Rickettsia uses its outer membrane proteins to recognize host cell receptors. A vital characteristic of Rickettsia's infection mechanism is its identity as a gram-negative bacterium. Bacterial cells can be either gram-positive or gram-negative, concerning their structural characteristics. Gram-negative species are characterized by an OM (outer membrane), which aids in both protection and recognition of host cells. Using an outer membrane protein romp A, Rickettsia can adhere to the cell and be endocytosed into a host. Following endocytosis, Rickettsia populations within host cells soon increase due to bacterial cell replication [4]. Eventually, bacterial cell populations are too massive to be contained, and host cell lysis occurs. As a result, the bacteria gain access to the human bloodstream and can potentially infect organ systems. The impact of endothelial invasion and blood vessel deterioration may result in a cutaneous rash in patients. About one-half of patients will present with a hemorrhagic rash, which is beneficial for physicians who witness the rash in combination with other symptoms [5].
History
Rocky Mountain Spotted Fever (RMSF) was initially known as the Idaho spotted fever. Patients in late 1800’s Idaho, were presenting with fevers and spotted rashes, initially on their lower extremities which then spread over their bodies. In the early 20th century, wood ticks were implicated as transmission vectors of RMSF through a review of over one hundred cases of the illness. Howard T Ricketts would distinguish the wood tick from the pathogenic bacteria, noting the transmission potential to humans through the tick. Due to his isolation of the bacterium, the bacterial disease was named Rickettsia. Into the early 1920s, the infection mechanism of Rickettsia rickettsii was further understood, as it was classified as an obligate, intracellular anaerobe [6].
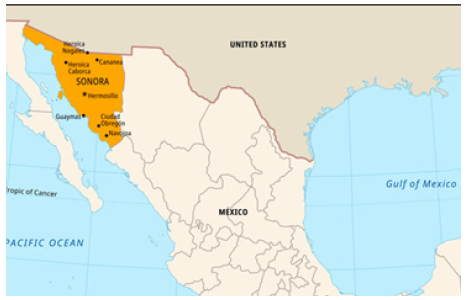
Wood ticks are a part of the family Ixodidae, characterized as hard ticks. Within this family, the genus Dermacentor includes the American dog tick (D. variabilis), Rocky Mountain wood tick (D. Andersoni) and brown dog tick under the Rhipicephalus genus (R. sanguineus), which are all capable of carrying the bacterium Rickettsia and transmitting it to humans. The variability of wood tick species implies that RMSF may not be isolated to a particular region. While the Rocky Mountain regions of states like Idaho, Utah, and Colorado are primary locations for Rocky Mountain wood ticks, other areas like the Southwestern United States and Northern Mexico house the brown dog tick. The brown dog tick is considered the primary transmission source in Mexico, and it is imperative to highlight this tick in the wake of the recent cases of RMSF in Southern California [6]. In December of 2023, five cases of RMSF arose in this region, with three out of five cases resulting in fatalities. Furthermore, all of the patients had traveled to Tecate, Mexico. The implications of cross-border travel from northern Mexico states, including Tecate and Sonora, where the brown dog tick lives, and the potential for more RMSF cases prompt further review [2] (Figure 2).
Case Review
A 52-year-old woman experiencing diarrhea, vomiting, nausea, and a fever went to a Southern California emergency department in May 2014. The woman noted the presence of symptoms for three days and had begun taking ampicillin, believing it would resolve her infection. The antibiotic, ampicillin, had been prescribed to the woman for a previous infection. The patient did not report any recent travel in the month leading to her illness but mentioned her other relatives often visited Mexico and brought their dogs back and forth across the border. Upon admission, doctors noted a red and purple spotting rash across the patient's extremities. Urosepsis was an initial diagnosis in which the patient's fever and nausea were considered. A course of broad-spectrum antibiotics, including levofloxacin and cefepime, was ordered.
Laboratory tests showed elevated enzymes-hepatic transaminases and higher than average blood clotting time (compared to a baseline ratio) The patient was admitted to a San Diego care facility where her chart documented DIC (disseminated intravascular coagulation). No other tests were run except a serum specimen on both day 7 and day 24 of illness [7]. Serologic tests are employed to evaluate antibody levels, which are produced in response to specific antigens. IgM titers measure the levels of immunoglobulin M, an antibody first made when a new infection begins, while IgG (Immunoglobulin G) is produced later on to file a memory of infection [8]. The patient's earlier serum test reported an IgG titer <64 and an IgM titer of 160. Day 24 results indicated an IgG >1024 and >160. The normal range of values for IgM is between 45-150mg/dL, while the normal range for IgG is between 800-1500mg/dL [9]. The woman's results are consistent with the rise of IgG over time, as her day 7 levels were minimal, while on day 24, both her levels indicated the presence of antibodies. Later, the California Department of Public Health conducted an immunofluorescence antibody assay, which revealed her serologic titers were reactive with the bacterial species Rickettsia. The chart notes that no fibrogen or D-dimer results were reported.
The patient's condition worsened when she arrived at the San Diego facility. The report notes the woman was intubated and began to decline. Acute renal failure, encephalopathy, and cardiomyopathy are recorded. The patient was given hemodialysis amid acute renal failure, and another course of antibiotics was started via intravenous measures. Both vancomycin and metronidazole were administered, yet the patient died twenty-eight days following her initial symptoms. The cause of death was linked to complications of DIC (disseminated intravascular coagulation) leading to multistage organ failure, including the kidneys (bilateral pyelonephritis), pancreas, lungs (pneumonia), and other abdominal organs (ascites). Later, an epidemiological review of the patient's home revealed an infestation of the brown dog tick. Over thirty ticks were discovered in the patient's yard and on the dog itself. Through laboratory polymerase chain reaction (PCR) techniques, the ticks' DNA was studied, and one of the ticks contained DNA strands from the bacteria Rickettsia. This was cross-referenced with a skin biopsy after the patient died, in which PCR was used to confirm the presence of a Rickettsia species [7].
A second case involves an 18-year-old female presenting with fever, headache, generalized fatigue, and joint pain. Her symptoms persisted, and she sought care on three distinct occasions in Nogales, Mexico. Her symptoms were seen as a nonspecific viral or bacterial infection, and she was prescribed the broad-spectrum antibiotic cephalexin. Following each visit to the emergency room, the woman received no confirmative diagnosis. Like the previous patient, lab testing revealed elevated enzymes, both hepatic transaminases and pancreatic enzymes. The patient's white cell count was elevated, and symptoms persisted. During transfer to a different medical center in the United States, the patient went into cardiac arrest and died. A later autopsy revealed a widespread rash on the patient's extremities as well as internal bleeding in the lung pleural space and the heart. Inflammation of various organs, including the liver and heart, was documented. Synonymous with the previous case, PCR techniques were employed and confirmed the presence of RMSF [7].
A final case for review from 2021 is a 20-year-old male from North Texas presenting with a persistent fever. At the hospital, his fever was 103°F, and during intake, the patient noted a persistent sore throat and cough. His history was unremarkable, with no recent travel out of the country. Amid his symptoms, his labs were within normal parameters, including his white cells and metabolic enzyme panel. The cough and sore throat were interpreted as COVID-19 symptoms, and physicians ordered a test. Although the COVID-19 test returned negative, the patient was sent home with instructions to take Tylenol for the pain. He returned five days later after his fever had climbed to 104.2. The patient presented with abdominal pain, nausea, and diarrhea. Labs revealed decreases in Hemoglobin concentrations-11.4g/dL, platelets-50x10^9 L, and Sodium-129 mEq/L. Normal ranges for Hemoglobin in males are 14-18g/dL, Sodium levels are 136-145 mEq/L, and th normal platelet count is 150 to 450 billion per liter [9]. Additionally, liver enzymes were elevated: aminotransferases (AST; 240U/L), alanine aminotransferase (ALT; 247 U/L), and elevated bilirubin-7.2 mg/dL [10]. Typical range values are as follows: Aminotransferases AST and ALT with values of 10-40 U/L and bilirubin between 0.3-1.0mg/dL [9]. The patient's persistent abdominal pain prompted an abdominal computed tomography scan (CT). The scan revealed evident inflammation of the liver, spleen, gallbladder, and appendix, as well as ascites. Surgery was consulted to check for appendicitis, which was eventually disregarded as a diagnosis. In the meantime, the patient was administered vancomycin and piperacillin-tazobactam antibiotics. After an additional three days, symptoms persisted, and liver enzymes remained elevated. An infectious workup tested for multiple diseases. The workup tested for Epstein Barr, hepatitis A-E, HIV, and C. diff (Clostridium difficile), which were all negative. A test for RMSF IgM antibodies was eventually run on the fourth day, returning positive.
The normal range for Immunoglobulin M is between 45-150mg/dL, with greater concentrations indicating a positive antibody test. The patient's antibiotics were exchanged for doxycycline, and symptoms quickly improved. After twenty-four hours, the patient's fever broke, and no GI (gastrointestinal) symptoms persisted. The patient did not present with any complications and following a classic 10-day course of antibiotics, the patient's lab values were back to ordinary, including his Sodium-136-145mEq/L, platelet count-150-450 billion/L, and Hemoglobin-14-18g/dL. Previously, low platelet count and Hemoglobin concentrations had indicated Thrombocytopenia, placing him at risk for blood clotting and severe complications. The patient's liver enzymes were no longer elevated with AST and ALT in the normal range-10-40U/L and his bilirubin with 0.3-1.0 mg/dL. The two-week follow-up noted no further symptoms, which, combined with typical lab values, point to a complete recovery.
Discussion
Rocky Mountain Spotted Fever presents a clinical dilemma. Symptoms are relatively nonspecific if a distinct spotted rash does not form. Apparently, a rash was observed in cases one and two, yet this rash was not indicated in their initial visit to the emergency room. This makes sense if we consider how an RMSF rash presents in only 3% of initial cases in the first three days of infection. Additionally, a fever can precede a rash by up to five days, and from the cases outlined above, patients made multiple trips to the emergency room. On their initial visits, in which patients presented with nonspecific symptoms, including fever and headache, RMSF was not on the differential as the identifying triad (fever, headache, rash) was not evident.
In the first two cases described, both patients died due to organ damage and the invasive nature of the bacteria Rickettsia. While neither patient reported a tick bite, both patients' histories indicate the potential for RMSF to be considered. Patient One noted her relatives often travel to Mexico and bring their dogs back and forth over the border. Although the woman herself had not traveled, ecological reports showed a positive DNA match for the bacterium. In the second case of the 18-year-old female, no contact with a tick or ownership of a dog was mentioned, the female's residence in Nogales, Mexico, should be considered. Etiological reports highlight northern Mexico as an optimal location for the brown dog tick (R. sanguineus) to reside. In fact, the state of Sonora, in which the 18-year-old female lived, has a fatality rate of 18% for RMSF [7]. The etiological nature of wood ticks can be applied in the third case, in which the patient's residence in northern Texas makes it probable that he could encounter this tick. It seems that the rash is an identifying marker for RMSF, and the implications of misdiagnosis due to nonspecific symptoms are grave. Considering the potential for RMSF to cross into new geographic regions such as Southern California, makes etiology an even more significant factor. Comprehension that Sonora is a prime location for the brown dog tick is critical for clinicians and individuals traveling to it. Furthermore, although humans cannot transmit RMSF to one another as Rickettsia utilizes ticks as a vector, animals such as dogs are prime transmission vehicles. There is concern that not only will people's migration across the United States-Mexican border have clinical implications, but the migration of stray dogs across the border could be equally or even more problematic.
With the potential for new cases of RMSF to emerge, understanding effective treatment is critical. In both case one and case two, patients died of organ complications and respiratory failure due to the invasive vascular nature of the bacterium Rickettsia. Patient one had initially been taking leftover Ampicillin and then was later prescribed broad-spectrum antibiotics levofloxacin and cefepime. Patient two was prescribed cephalexin; originally, patient three was prescribed vancomycin and piperacillin-tazobactam. Antibiotics encompass a wide range of functions and target different properties of the bacterial cell. All these antibiotics are ineffective against Rickettsia due to its structural properties noted above. Antibiotics like vancomycin and piperacillin-tazobactam target predominant structures in gram-positive bacterial cells and are unable to permeate the outer membrane in gram-negative species [11].
Additionally, IgM and IgG antibody tests may be negative initially which was evident in the case of the 18-year-old woman. It can take up to a week for antibody titers to be positive [10]. Doctors recommend that even if RMSF is suspected, patients be prescribed tetracycline-class antibiotics such as doxycycline. The mechanism of this antibiotic allows it to target both gram-negative and gram-positive bacterial cells. It targets the bacterial 30S subunit of the bacterial ribosome, which is conserved in bacteria and differs from eukaryotic ribosomal subunits. The antibiotic is characterized by lipophilicity and is able to cross through the OM (outer membrane) of gram-negative cells, making it an effective target for infections like Rocky Mountain Spotted Fever [12]. This treatment was influential in the case of patient three, who, following a course, had recovered from the infection. It is important to note that waiting for the appearance of a rash is not recommended to confirm the presence of RMSF because, in 9-12% of cases, a cutaneous rash does not present. A lack of rash is noted in older individuals and African Americans [6]. Understanding the presentation of symptoms is critical because symptoms appear at different points in time and are missing in certain patients.
Conclusion
Throughout history, Mexico has had to declare a public health emergency for RMSF. This is a strong indicator of the propensity of Rickettsia to be transmitted if a vector is available. In Mexico and regions like the Rocky Mountains of the United States, it is evident, based on epidemiological history, that this bacterial disease can be transmitted to humans when certain tick species are present. Due to the severity of the disease and the clinical implications of improper diagnosis, education on disease presentation and treatment is now more critical than ever. As warranted by the CDC (Center for Disease Control) only last month, there is a risk with the porousness of the US-Mexican border that more and more cases of RMSF begin to arise in Southern California. Although this is not the hope, understanding the structural characteristics of the bacterium Rickettsia rickettsii and the mechanism of infection is critical from an education and health prevention standpoint.
References
- Rickettsiae - Medical Microbiology - NCBI Bookshelf.
- Rudy M, Fox News (2023) Deadly rocky mountain spotted fever outbreak in California likely came from Mexico, CDC says. Fox News.
- Boulanger N, Boyer P, Talagrand Reboul E, Hansmann Y (2019) Ticks and tick-borne diseases. Médecine et Maladies Infectieuses 49(2): 87-97.
- Li H, Walker, DH (1998) Rompa is a critical protein for the adhesion of Rickettsia Rickettsiito host cells. Microbial Pathogenesis 24(5): 289-298.
- Walker DH, Rickettsiae - USAL.
- Dantas-Torres F (2007) Rocky Mountain Spotted Fever. The Lancet Infectious Diseases 7(11): 724-732.
- Drexler NA, Yaglom H, Casal M, Fierro M, Kriner P, et al. Fatal rocky mountain spotted fever along the United States-Mexico border, 2013-2016. Emerging infectious diseases.
- Immunoglobulin test: High vs low VS normal levels of (IG) antibodies.
- ABIM laboratory test reference ranges ̶ January 2024.
- MBDI (n.d.-a). Rocky Mountain spotted fever masquerading as gastroenteritis: A common but overlooked clinical presentation. Cureus.
- Silhavy TJ, Kahne D, Walker S (2010) The bacterial cell envelope. Cold Spring Harbor perspectives in biology.
- Patel RS (2023) Doxyycline hyclate. StatPearls.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.