Review Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Intermediated Actions of Apoprotein E In VLDL Lipoprotein Lipolysis
*Corresponding author: Tania Leme da Rocha Martinez, Nephrology Department, BP-A Beneficência Portuguesa de São Paulo, Brazil.
Received: April 10, 2024; Published: May 02, 2024
DOI: 10.34297/AJBSR.2024.22.002956
Abstract
Very Low Density Lipoprotein (VLDL) is the main triglyceride carrier thus characterized in the lipid metabolic profile. The others, chylomicrons and Intermediate Lipoproteins (IDL), also rich in triglycerides, are ephemeral, undosed, undosed, undetected in fasting patients. IDLs have an intermediate lipid composition between VLDL and LDL lipoproteins (Low-Density Lipoproteins). It is worth mentioning that chylomicrons are formed from food, an exogenous cycle, while VLDL is formed by the liver, an endogenous cycle. Dysbetalipoproteinemia also called type III hyperlipoproteinemia is clinically characterized by the presence of corneal arch, xanthelasma, tuberoeruptive xanthoma and palmar xanthomas. Serum cholesterol and triglycerides are elevated. Atherosclerosis is frequent with about 50% of those affected developing coronary heart disease. Low Density Lipoprotein-Cholesterol (LDL-c) is normal or reduced because there is a lower conversion of Intermediate Density Lipoprotein-Cholesterol (IDL-c) to LDL-c. Dysbetalipoproteinemia results from mutations involving the gene that conditions the formation of apolipoprotein E (Apo E), which has several allelic forms, E3 being the most common. It is believed that other forms originated from mutations that occurred in E3: a substitution of arginine for cysteine at position 112 of the amino acid sequence differentiates E4 from E3, and the same substitution at position 158 gives rise to E2. The test for the prevention of heart disease, through the detection by PCR-RFLP (polymerase chain reaction - restriction fragment length polymorphism) of the genotypes of the Apo E gene, is indicated for the following cases: people with a history of coronary heart disease; people who have proven risk factors for coronary heart disease and those with type III dyslipidemia, in addition to the lipid profile. This test is performed only once in life, at any age, including prenatal care, because the information studied comes from the individual’s genetic code.
Keywords: VLDL, Metabolism, Apoprotein E, Genetics, Dyslipidemia, Lipase
Abbreviations: APO E: Apolipoprotein E; IDL: Intermediate Density Lipoprotein; IDL-c: Intermediate Density Lipoprotein- Cholesterol; LDL: Low Density Lipoprotein; LDL-c: Low Density Lipoprotein-Cholesterol; PCR: Polymerase Chain Reaction; VLDL: Very Low-Density Lipoprotein
Introduction
Very Low-Density Lipoprotein (VLDL) is the main triglyceride carrier thus characterized in the lipid metabolic profile. The others, chylomicrons and Intermediate Lipoproteins (IDL), also rich in triglycerides, are ephemeral, undosed, undetected in fasting patients. IDL have an intermediate lipid composition between VLDL and Low Density Lipoproteins (LDL) lipoproteins. It is worth mentioning that chylomicrons are formed from food, an exogenous cycle, while VLDL is formed by the liver, an endogenous cycle.
Dysbetalipoproteinemia also called type III hyperlipoproteinemia, is clinically characterized by the presence of corneal arch, xanthelasma, tuberoeruptive xanthoma and palmar xanthomas [1]. Serum cholesterol and triglycerides are elevated. Atherosclerosis is frequent with about 50% of those affected developing coronary heart disease. Low Density Lipoprotein-Cholesterol (LDL-c) is normal or reduced because there is a lower conversion of Intermediate Density Lipoprotein-Cholesterol (IDL-c) to LDL-c [2]. Dysbetalipoproteinemia results from mutations involving the gene that conditions the formation of apolipoprotein E (Apo E). Apo E has several allelic forms, of which E3 is the most common and it is believed that the other forms (E2 and E4) originated from mutations that occurred in E3: a substitution of arginine for cysteine at position 112 of the amino acid sequence differentiates E4 from E3, and the same substitution at position 158 gives rise to E2. In adult white populations, the estimated frequencies of occurrence of E2, E3 and E4 are, respectively, 8%, 78% and 14% [3]. In vitro studies have shown that the receptor binds with high affinity to lipoproteins containing both Apo E3 and Apo E4, but particles containing Apo E2 show practically no binding with the receptor [2]. Individuals with dysbetalipoproteinemia type III are mostly homozygous for the arg 158cis mutation, which is therefore of autosomal recessive inheritance.
The need for cofactors for the development of hyperlipidemia is evident when comparing the frequency of the E2E2 genotype, which is 1/100 in most populations, and the frequency of hyperlipidemia, which is 1 in 5,000 [1,4-6]. Several other variants of Apo E, with different ability to bind to the receptor, have been discovered, some of them presenting a dominant inheritance pattern. The identification of the type of mutation is therefore important for the genetic counseling of individuals [7-9]. Apo E genetics showed that in a normal population, the E2 allele was being linked to lower plasma concentrations of cholesterol and LDL-c than in people with the E3 allele. It has also been revealed that people with the E4 allele have higher cholesterol than those homozygous for the E3 allele [10].
There is an association between the Apo E-E4 allele and coronary heart disease, especially when patients have aggravating risk factors such as smoking, obesity, and dyslipidemia. It is now known that those who have the E4 allele are three to five times more likely to have coronary heart disease compared to those who have the E3 allele. The Apo E E2 isoform has a reduced affinity for the LDL receptor when compared to the other forms and its presence may lead to the accumulation of lipoproteins containing Apo E. Approximately 90% of patients with type III hyperlipoproteinemia are homozygous for Apo E E2, however less than 10% of these develop the alteration, which suggests that another factor(s) is (are) necessary for the expression of the disease. The Apo E E4 isoform is more frequent in type V hyperlipoproteinemia, which is characterized by hypercholesterolemia due to the accumulation of chylomicrons and VLDL [11].
For better understanding of Apo E mechanisms in patients it is important that the methodology of its assay be known and whenever possible be done: isolation of genomic DNA from leukocytes, followed by Polymerase Chain Reaction (PCR) amplification of the specific region of the Apo E gene and digestion and electrophoresis. Sample collection and processing: to perform the test, it is necessary to collect 5.0 ml of peripheral blood in a vacuum collection tube with anticoagulant Ethylenediamine Tetraacetic Acid (EDTA).
Interpretation of the diagnosis: through the technique of PCR associated with enzyme restriction, we were able to characterize the patients according to the alleles visualized: the reports are characterized by being explanatory, giving greater security in the interpretation of the result for both the physician and the patient. Once the specific details on Apo E have been mentioned and having in sight the until now practical laboratory method to determine Apos E concentration, the idea is to have them measured always. This finding helps if added to the lipid profile (Figure 1).
Due to the importance of Apo E, as reported in the literature, its dosage is necessary due to its interference in lipase activation. Apo E is a constituent of VLDL, High-Density Lipoprotein (HDL), and chylomicron lipoproteins and plays a key role in the transport and metabolism of cholesterol and triglycerides. This protein is additionally related to immunoregulation and neurobiological pathways (neuronal repair, remodeling, and protection). Three main variants of Apo E are found in the human population resulting from the change of a single amino acid. The alleles encoding these variants are named Apo E E2, Apo E E3, and Apo E E4 and their frequencies in the Caucasian population are 8%, 78%, and 14%, respectively.
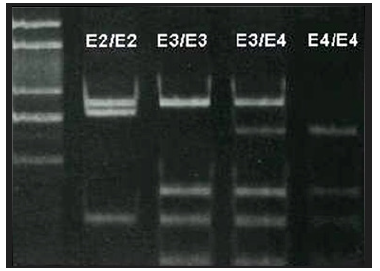
Figure 1: Genotyping for apolipoprotein E visualized on 2% agarose gel stained with etidium bromide.
It is worth reiterating that the alleles of Apo E (E2 and E4) may represent genetic markers for the identification of individuals at high risk for the development of coronary heart disease. Individuals with genotype E4E4 and E4E3 have higher levels of LDL-c and total cholesterol than individuals with E3E3, and are particularly susceptible to the early development of coronary heart disease. Van Bockxmeer, et al. [12] described a 16-fold higher prevalence of the E4E4 genotype among men under 40 years of age who were referred for angioplasty, and Lenzen, et al. [13] reported that the E3E4 genotype seems to be associated with the earlier age of individuals with myocardial infarction. The E2E2 genotype determines lower LDL-c levels than those observed for the other two phenotypes. The mechanism by which the E2 allele would be related to low LDL-c levels seems to be the weak binding that E2 establishes with the receptor protein, which decreases and/or delays the removal of chylomicrons and VLDL-c [14,15]. Decreased rates of coronary heart disease were not observed in individuals carrying the E2 allele, and it has been suggested that the lack of protection is due to the hypertriglyceridemia associated with it [16]. In the study by Wilson, et al. [17], triglyceride levels were moderately high in women and very high in men, both with the E3 allele and with the E4 allele, but the risks in both sexes for the development of coronary heart disease were significant only for E4. In this study, 15% of the prevalence of coronary heart disease (11% in men and 19% in women) was attributed to this allele. Confirming the results of several other studies, total cholesterol and LDL-c levels were lower for the E2 allele and higher for the E4 allele [18-22].
In a study that evaluated the occurrence of the E4 phenotype in 113 individuals with hypertension, Kesäniemi, et al. [23] did not observe differences in the frequency of this gene between hypertensive and control patients, but hypertensive patients with E4 had higher levels of VLDL-c and triglycerides than controls of the same genotype. The lipid levels observed were particularly high in E4 individuals using diuretics and beta-blockers, which, according to the authors, is suggestive that hypertensive individuals with E4 may develop severe dyslipidemias, particularly when submitted to these medications. In another study [24], the same group evaluated whether the risk of developing coronary heart disease in individuals with non-insulin-dependent diabetes mellitus would be related to the phenotypic pattern of Apo E. The results obtained showed that the presence of E4 increased the risk, but the plasma lipid levels of diabetics with this gene were not different from those observed in diabetics without E4. The E4 allele also seems to be associated with a type of hypercholesterolemia, determined by a polygenic genetic mechanism, in which those affected have LDL-c levels above 190mg/dl and do not have xanthomas. Those affected are most often homo genotype or heterozygous for this allele [25-27].
The heart disease prevention test, through PCR-RFLP (restriction fragment length polymorphism) detection of Apo E gene genotypes, is indicated for the following cases: people with a history of coronary heart disease; people who have proven risk factors for coronary heart disease and those with type III dyslipidemia, in addition to the lipid profile. This test is performed only once in life, at any age, including prenatal care, because the information studied comes from the individual's genetic code.
In conclusion, in pathological cases in which IDL lipoproteins are present, there is always need of consideration of the complete lipid profile to determine the therapeutic intervention.
Acknowledgments
None.
Conflict of Interest
None.
References
- Thompson GR (1990) Primary hyperlipidemia. Br Med Bull 46(4): 986-1004.
- Mahley RW, Innerarity TL, Rall SC Jr, Weisgraber KH (1984) Plasma lipoproteins: apolipoprotein structure and function. J Lipid Res 25(12): 1277-1294.
- Davignon J, Gregg RE, Sing CF (1988) Apolipoprotein E polymorphism and atherosclerosis. Arteriosclerosis 8(1): 1-21.
- Brown MS, Goldstein JL, Fredrickson DS (1983) Familial type 3 hyperlipoproteinemia (dysbetalipoproteinemia). In: Stanbury JB, Wyngaarden JB, Fredrickson DS, Goldstein JL, Brown MS (eds) The metabolic basis of inherited disease, 5th McGraw-Hill, New York, pp. 655-671.
- Innerarity TL, Weisgraber KH, Arnold KS, Rall SC Jr, Mahley RW (1984) Normalization of receptor binding of apolipoprotein E2. Evidence for modulation of the binding site conformation. J Biol Chem 259(11): 7261-7267.
- Innerarity TL, Hui DY, Bersot TP, Mahley RW (1986) Type III hyperlipoproteinemia: a focus on lipoprotein receptor-apolipoprotein E2 interactions. Adv Exp Med Biol 201: 273-288.
- Martínez Martínez AB, Torres Perez E, Devanney N, Del Moral R, Johnson LA, et al (2020) Beyond the CNS: The many peripheral roles of APOE. Neurobiol Dis 138: 104809.
- Sacks FM (2015) The crucial roles of apolipoproteins E and C-III in apoB lipoprotein metabolism in normolipidemia and hypertriglyceridemia. Curr Opin Lipidol 26(1): 56-63.
- Morton AM, Koch M, Mendivil CO, Furtado JD, Tjønneland A, et al (2018) Apolipoproteins E and CIII interact to regulate HDL metabolism and coronary heart disease risk. JCI Insight 3(4): e98045.
- Cumming AM, Robertson FW (1982) Genetics of the apolipoprotein-E isoprotein system in man. J Med Genet 19(6): 417-423.
- Martinez TLR (2003) Manual de Condutas Clínicas em Dislipidemias [Manual of Clinical Conduct in Dyslipidemia]. MedLine Publisher, Rio de Janeiro, Brazil p. 392.
- Van Bockxmeer FM, Mamotte CD (1992) Apolipoprotein epsilon 4 homozygosity in young men with coronary heart disease. Lancet 340(8824): 879-880.
- Lenzen HJ, Assmann G, Buchwalsky R, Schulte H (1986) Association of apolipoprotein E polymorphism, low-density lipoprotein cholesterol, and coronary artery disease. Clin Chem 32(5): 778-781.
- Weisgraber KH, Innerarity TL, Mahley RW (1982) Abnormal lipoprotein receptor-binding activity of the human E apoprotein due to cysteine-arginine interchange at a single site. J Biol Chem 257(5): 2518-2521.
- Mahley RW, Weisgraber KH, Innerarity TL, Rall SC (1991) Genetic defects in lipoprotein metabolism: elevation of atherogenic lipoproteins caused by impaired catabolism. JAMA 265(1): 78-83.
- Dallongeville J, Lussier Cacan S, Davignon J (1992) Modulation of plasma triglyceride levels by apoE phenotype: a meta-analysis. J Lipid Res 33(4): 447-454.
- Wilson PW, Myers RH, Larson MG, Ordovas JM, Wolf PA, et al (1994) Apolipoprotein E alleles, dyslipidemia, and coronary heart disease. The Framingham Offspring Study. JAMA 272(21): 1666-1671.
- Bates SR, Coughlin BA, Mazzone T, Borensztajn J, Getz GS (1987) Apoprotein E mediates the interaction of beta-VLDL with macrophages. J Lipid Res 28(7): 787-797.
- Alagarsamy J, Jaeschke A, Hui DY (2022) Apolipoprotein E in cardiometabolic and neurological health and diseases. Int J Mol Sci 23(17): 9892.
- Weisgraber KH, Innerarity TL, Rall SC Jr, Mahley RW (1990) Atherogenic lipoproteins resulting from genetic defects of apolipoproteins B and E. Ann N Y Acad Sci 598: 37-48.
- Topriceanu CC, Shah M, Webber M, Chan F, Shiwani H, et al (2024) APOE ε4 carriage associates with improved myocardial performance from adolescence to older age. BMC Cardiovasc Disord 24(1): 172.
- Chen W, Li B, Wang H, Wei G, Chen K, et al (2024) Apolipoprotein E E3/E4 genotype is associated with an increased risk of type 2 diabetes mellitus complicated with coronary artery disease. BMC Cardiovasc Disord 24(1): 160.
- Kesäniemi YA, Lilja M, Kerviren K, Rantala A (1992) Multiple metabolic syndrome: aspects of genetic epidemiology and molecular genetics. Ann Med 24(6): 461-464.
- Ukkola O, Savolainen MJ, Salmelaa PI, von Dickhoff K, Kesäniemi YA, et al. (1995) DNA polymorphisms at the lipoprotein lipase gene are associated with macroangiopathy in type 2 (non-insulin-dependent) diabetes mellitus. Atherosclerosis 115(1): 99-105.
- Sing CF, Davignon J (1985) Role of the apolipoprotein E polymorphism in determining normal plasma lipid and lipoprotein variation. Am J Hum Genet 37(2): 268-285.
- Ordovas JM, Litwack Klein L, Wilson PW, Schaefer MM, Schaefer EJ (1987) Apolipoprotein E isoform phenotyping methodology and population frequency with identification of apoE1 and apoE5 isoforms. J Lipid Res 28(4): 371-380.
- Utermann G (1988) Apolipoprotein polymorphism and multifactorial hyperlipidaemia. J Inherit Metab Dis 11(Suppl 1): 74-86.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.