Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Using Grassroots Community Education Campaigns to Promote Understanding of Recent Changes to the North Carolina Medicaid Program
*Corresponding author: Anthony U Emekalam, Department of Health and Human Studies, Elizabeth City State University, North Carolina.
Received: February 20, 2024; Published: April 12, 2024
DOI: 10.34297/AJBSR.2024.22.002918
Abstract
Over 200,000 Medicaid beneficiaries in 21 counties of northeastern North Carolina were among the 1.6 million beneficiaries who started receiving state Medicaid services under managed care delivery protocol from July 1, 2021. However, post implementation studies indicate that beneficiaries were unclear about several important elements of the managed care delivery system even after it was launched. This study evaluated impacts of culturally appropriate grassroots education as a tool for addressing this concern among predominantly African American communities in the northeastern region of the state. 157 state Medicaid recipients and caregivers attended 14 grassroots education events across 10 rural underserved counties in the region. Pre-/post intervention evaluations which were used to measure the impact of grassroots education on knowledge of North Carolina Medicaid reforms showed that participants improved their knowledge of Medicaid managed care reforms by 12.5% after attending the grassroots education events. This finding suggests strongly that culturally appropriate grassroots education contributed to increased understanding of Medicaid managed care reforms in this population of rural underserved residents and is significant because proper understanding of recent managed care reforms is key to accessing managed care benefits successfully and achieving core goals of North Carolina Medicaid managed care reforms.
Introduction
The North Carolina General Assembly enacted session Law 2015-245 in 2015 directing the North Carolina (NC) Department of Health and Human Services (NCDHHS) to transition state Medicaid from a fee-for-service to a managed care model [1]. Consequently, on July 1, 2021, most NC Medicaid beneficiaries including most of over 200,000 residents of 21 rural underserved counties of northeastern NC within the service region of the Elizabeth City State University started receiving Medicaid services under the managed care system which is argued to be more intentional in addressing and meeting health and health-related needs of beneficiaries in comparison to fee-for-service model [2-4]. Prior to July 1, 2021, NCDHHS worked with key stakeholders such as health plans, providers, community-based organizations, and beneficiaries to ensure smooth transitioning and install provisions that are critical to meeting key objectives of the transformation [5]. These efforts included Medicaid transformation information outreaches to beneficiaries by mail, on NCDHHS’ website and through several social service and advocacy organizations [6]. However, despite these good faith efforts, post implementation studies by Allen et al. and Zimmer et al. showed that due to limitations that were exacerbated by the global pandemic of 2020, most beneficiaries had significant deficiency in outcome-impacting knowledge about NC Medicaid reforms [7-9]. This current study therefore explored use of culturally sensitive education as means of closing perceived knowledge gaps of NC Medicaid managed care reforms among African American beneficiaries in rural underserved counties of northeastern North Carolina.
Methods
Approach
Study intervention was delivered using a community-engaged participatory approach that was modelled after evidence-based community outreach programs targeting African Americans such as Mayo Clinic’s Wellness Rx and Fostering African American Improvement in Total Health (FAITH) programs. The implementation strategy also included guidelines from Akintobi, et al. and contents from an American Medical Association publication on improving health of African Americans [10-12]. A Community Medicaid Advisory Board consisting of community leaders and residents some of whom were either NC Medicaid recipients themselves or direct caregivers of beneficiaries was convened to facilitate implementation of education activities. Board members identified venues for education outreach events, facilitated event scheduling, and coordinated every aspect of grassroots organizing that are valuable to successful implementation of community outreach programs [13-15]. Board membership included two representatives that were selected from each of the counties in the study region. The study protocol and instruments were approved by the Institutional Review Boad of the Elizabeth City State University.
Education Curriculum
The education curriculum emphasized specific information on NC Medicaid managed care reforms that were viewed as relevant to achieving optimal health outcomes under the new delivery system. Contents included information on core differences between the new NC Medicaid managed health care delivery approach and the previous traditional fee-for-service method and core differences among the 5NC Medicaid managed care standard plans that most of the beneficiaries were enrolled in. The curriculum also highlighted differences between NC Medicaid transformation and NC Medicaid expansion Table 1. Curriculum contents were adapted from information and materials available on NCHHS website [16-18].

Table 1: Key questions addressed in education sessions and respective NC managed care knowledge areas that they assessed.
Study Participants
Participants were self-validated adult (>18 years) North Carolina Medicaid recipients or direct caregivers of North Carolina Medicaid beneficiaries who were either members of the local church organization that hosted an education outreach event or invited community residents. Every participant participated in a consenting discussion that preceded each event. This plenary segment provided detailed information about the study and explained voluntary participation to potential participants.
Intervention
Educational Outreach Events
In-person education outreach events on NC Medicaid transition from pay for service to managed health care delivery models was the main intervention used in this study. Education sessions focused mainly on areas of the new managed care model that are relevant to proper utilization of managed care resources that are crucial for potential health outcomes of participants under the new delivery method Table 1. The events were informal and non-traditional and were tailored to reflect culturally acceptable expectations of participants. Discussions included specific areas of difference between the traditional fee-for-service and managed care delivery models including health care benefits (standard and extra health care benefits), availability of the 5NC managed care standard plans across Medicaid regions of North Carolina and guidelines for changing enrollment from one standard health plan to another.
Event Venues and Scheduling Process
Events were held in the auditoriums or meeting rooms of local and predominantly African American churches. African American churches were chosen as the most culturally appropriate venue for these events because of the historical significance of the of the African American church as a place of education and empowerment of African Americans [19-24]. Events were scheduled in advance and on days and times that were convenient for potential participants by community advisory board members in coordination with local church pastors. Consequently, most of the events were conducted in the evenings of weekdays however, a few (21.4%) were in the afternoon and weekends. The average timeframe between event scheduling and event implementation was 14 days and the average event period was one and half hours. All 14 events were conducted between Junes 10th and September 14, 2023.
Event Facilitators
Education sessions were facilitated by a diverse team from the department of health and human Studies at the Elizabeth City State University and community members from the region. The team of 10 members consisted of a professor/licensed pharmacist/minority health researcher, 3 student researchers, a university program associate, and 5 Community Medicaid Advisory Board members of the Elizabeth City State University’s Medicaid Transition Evaluation for eastern North Carolina (ECSU MEDITEEN) program. 90% of the facilitators identified as Black/African American and 10% as white. Facilitators were 40% male and 60% female.
Evaluation
Knowledge Assessment Questionnaire
A 5 item pre-/post knowledge assessment questionnaire which was not pre-validated was used to directly measure impacts of education outreach events on participants’ knowledge and understanding of areas of NC Medicaid managed care reforms that were measured in this study Table 1. The questionnaire was created by the research team to measure understanding of contents and materials discussed during education outreach events and was created with due consideration to implementation variables that may limit study evaluation such as time and program delivery constraints [25,26]. Furthermore, the short questionnaire with true/false responses made knowledge assessments relatively easy for participants and was a quick and reliable means of measuring a participant’s surface level and higher order knowledge of NC Medicaid managed care reforms before and after an educational intervention [27,28]. Study protocol including the knowledge assessment questionnaire was approved by the Institutional Review Board of the Elizabeth City State University.
Procedure and Data Collection
A pre-/post assessment method was used to track changes in participants knowledge and understanding of the NC Medicaid managed care reforms that were attributable to education outreach events. To this end, participants received a pretest prior to education outreach sessions and a posttest thereafter. Differences in pre- and post-assessment measurements were used to measure impact of education outreach events on the 5 knowledge areas of NC Medicaid managed care reforms that were measured in the study [29]. Data was documented only for participants who completed pretests, participated in the education outreach sessions, and completed posttests.
Data Analysis
Data from the knowledge assessment questionnaire were analyzed individually for each of the 5 knowledge areas assessed Table 1 and cumulatively for all 5 areas using descriptive and inferential statistics. Data was documented as frequencies, means, ranges and percentages. Differences in mean percentage pre-and posttest data were tested for significance by Student’s t test.
Results
Educational Outreach Events
14 educational outreach events focusing on specific elements of NC Medicaid managed care reforms were conducted across 7 rural underserved counties in northeastern North Carolina. 5/14 (35.7%) of the events were held in Tyrrell County which also has the highest percentage of Medicaid enrollees among the 7 counties studied. 2021 African American population data and total number of Medicaid enrollees in the 7 counties are summarized in Table 2 [30].

Table 2: African American NC Medicaid enrollment/population Data in the 7 northeastern North Carolina counties where education outreaches on NC Medicaid managed care reforms were conducted and number of events and participants per county.
Study Participants
The study included 157 adults (>18 years) NC Medicaid beneficiaries and direct caregivers. 96% of participants identified as Blacks/African Americans and 82% as females. The mean participant age was 51 years. The highest number of participants were from Tyrrell County and the lowest number from Washington County Table 2. The average number of participants per event was 11 with a standard deviation of 4.2 and a range of 17.
Study Impacts
Questions and Concerns about NC Medicaid Transition
Feedback from study participants during education session debriefs showed that participants received helpful answers and clarification to questions, doubts, and concerns about NC Medicaid transition after participating in the educational sessions. Participants commented on how the sessions helped relieve anxiety about potential loss in quality of care or Medicaid coverage because of the transition. They also demonstrated notable excitement after learning of extra benefits that are available through different standard health plans and were very relieved to know that they could change their plans if they needed to. Feedback also indicated a lessened sense of suspicion of government intensions regarding the transition and sense of empowerment and acceptance of the new delivery model. Furthermore, the educational sessions fostered a sense of community as participants became aware of their shared concerns and confusions about the new managed care delivery model.
General Understanding of NC Managed Care Reforms
Mean posttest knowledge assessment scores on NC Medicaid managed care reforms were significantly higher (p<0.05) than mean pretest scores in 13/14 (93%) of the events. These results suggest that the educational outreach events helped to improve participants overall knowledge/understanding of NC Medicaid managed care reforms. This outcome was highly significant (P<0.0001, CI=95%) when the mean pretest and posttest scores for all 14 events were analyzed together (Figure 1) (Table 1).
Understanding of Specific Areas of NC Medicaid Managed Care Reforms
Cumulative analysis of mean pretest and posttest scores on the 5 specific knowledge areas showed that education outreach had variable impacts on each of the 5 managed care knowledge areas assessed by the study. Although cumulative values of mean posttest scores were quantitatively higher than respective pretest scores in all areas, quantitative differences were statistically insignificant (p>0.05) in some areas (Figure 2) (Table 2). Analyzed data showed that knowledge and understanding of general differences between the new NC Medicaid managed care and the previous fee-for-service delivery models improved highly significantly (p<0.0001) after participants attended education outreach events. Furthermore, Participants achieved significant knowledge improvement (p<0.05) on diverse ancillary health care benefits such as receiving assistance with paying monthly phone bills, smartphone offers, and assistance with purchase of health-related over the counter items that were generally available through all standard Medicaid managed care plans or exclusively with enrollment in specific standard plans. The same was also true of pretest and posttest outcomes for the study area that measured understanding of managed care guidelines for switching from one standard plan to another suggesting that participants’ understanding of this study area also improved significantly because of the intervention [31,32]. However, data that assessed participants’ understanding of universal and restricted availability of the 5 standard NC Medicaid managed care health plans across different Medicaid regions of the state, and distinguishing between NC Medicaid transition and NC Medicaid expansion showed that participants’ understanding of these areas did not improve significantly (p > 0.05) after attending the education outreach events (Figure 2) (Table 2).

Figure 1: Pre and post knowledge-assessment percentage scores by event. Values are expressed as means ± standard error of the mean scores of each event. Pre -/post score differences was highly significant (p<0.0001) in 9 events, significant (p<0.05) in 4 events and not significant (p>0.5) in 1 event.
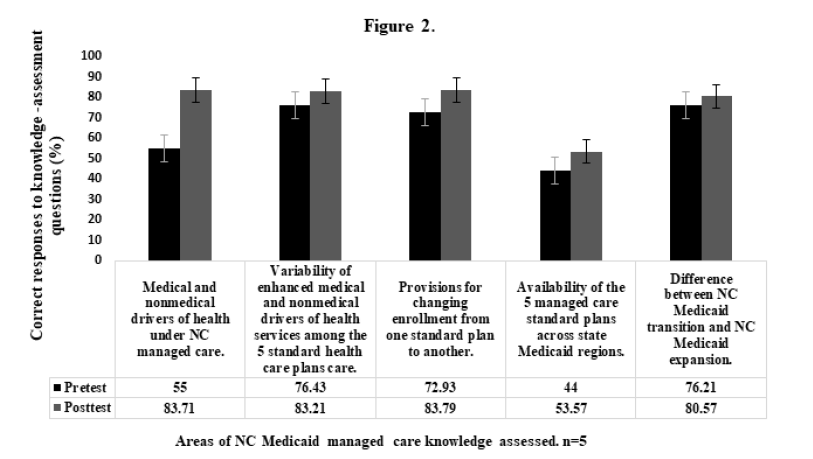
Figure 2: Pre and post knowledge-assessment percentage scores of NC managed care. Values are expressed as means ± standard error of the mean scores of each knowledge area. Cumulative pre-/post score difference was highly significant (p<0.0001), significant (p<0.05) in 3 knowledge areas but not significant (p>0.5) in 2 areas.
Discussion
This study investigated value of culturally acceptable education outreach in advancing basic knowledge of NC managed care reforms among rural underserved African Americans. On July 1, 2021, the state of North Carolina transitioned close to 1.6 million of its Medicaid beneficiaries out of fee-for-service care delivery model to managed care-a care delivery paradigm that provides basic Medicaid health benefits and additional health services through networks of providers known as managed care organizations [33]. Under this new way of receiving care, most of eligible participants now receive NC Medicaid services through a network of doctors and other providers that belong to a health plan that they qualified to enrolled in. The July 1, 2021, start date was for individuals who enrolled in 1 of 5 standard NC Medicaid managed care plans [34]. To ensure a smooth transition from the traditional fee-for-service model and to prepare affected beneficiaries adequately, the state’s department of Health and Human Services organized several prelaunch activities that included educating beneficiaries on key provisions of the new delivery method. Unfortunately, impacts of pre-launch activities were hindered by several factors that were compounded by the global pandemic of 2020. Consequently, post-implementation studies showed that beneficiaries were unclear about several elements of the managed care delivery system even after it launched [35].
Researched findings indicated that many participants had no clarity of extra benefits and enhanced services that were available through enrollment in specific standard plans and how to access those benefits [36]. A potential implication of this finding is that beneficiaries could lose important health benefits that are available through the new managed care system. Furthermore, contrary to the implementation protocol that allowed eligible beneficiaries to self-enroll in standard plans of their choice, most beneficiaries were auto enrolled into various health plans as implementation deadline approached. Consequently, many were unable to compare extra benefits across the 5 standard plans to determine if the health plan that they were enrolled in was the most adequate for their health needs [37]. The potential consequences of this concerns on overall health outcomes of NC Medicaid beneficiaries particularly for African Americans could be significant because of the number of African Americans that receive health care through NC Medicaid. For instance, in the state of North Carolina, the average Medicaid percent coverage at the time of birth was 65.1% for individuals who identified as blacks/African American [37]. These concerns may also increase current disparities in health access that is experienced by African Americans due to several reasons including long-standing mistrust of the health care system [38-40]. The intervention implemented in this study was purposed to narrow the perceived knowledge gap of the new NC Medicaid managed care reforms so African American Medicaid beneficiaries residing in rural underserved counties in northeastern North Carolina can maximize their health outcomes under the system.
Increase in knowledge of NC Medicaid Managed Care Reform
Study findings showed program participants achieved measurable gains in knowledge of NC Medicaid managed care reforms. Knowledge improvement was highly significant for major differences between the old fee-for-service and the new managed care delivery methods. This outcome suggests that confusions, misconceptions, and attending concerns about managed care reforms were significantly assuaged through improved understanding of purpose, value and how to access health care services under the new managed care delivery method. Education outreach also contributed significantly to improved understanding of different extra benefits that were offered by the 5 NC Medicaid managed care standard health plans and how to switch from one health plan to another. These findings imply that education outreach improved the ability of participants to make meaningful value-based comparisons that are relevant to their individual health outcomes. Additionally, through better understanding of managed care provisions for changing standard plan enrollment, participants can make changes that support their health goals, needs and other concerns. They were relieved to know that they may not be trapped permanently in a plan that is not the most suitable for their individual health needs which also helped to relieve concerns and confusions about the new managed care option. These findings were not altogether surprising due to plethora of scientific evidence that validates effectiveness of culturally sensitive education activities in advancing understanding and knowledge of African Americans in several health areas [41-44]. Improvements in knowledge of statewide availability of standard Medicaid managed care health plans and differentiating between Medicaid transition and Medicaid expansion were not statistically significant. This finding may be attributed to several factors that may include complexity of subject area, content delivery, or interest of participants in these subject areas. However, the marginal improvement in knowledge that was recorded (Δ=9.57%and Δ=4.36% respectively) adds to the credibility of effectiveness of the education outreach efforts.
Conclusion
Medicaid beneficiaries in the state expressed concerns and had several questions about the recent transition of NC Medicaid from a fee-for-service to a managed care delivery model. This study offers an effective approach for addressing these concerns among African Americans residing in rural communities where resources are typically insufficient for addressing these concerns adequately. It validates importance of adequate cultural balance of information campaigns that target African American communities and highlights the African American church as an incredible resource for reaching African Americans especially those residing in rural areas with important health-related messages. Policy makers should strongly consider engaging faith-based leaders of African American communities when thinking of effective ways of reaching rural-dwelling African Americans with critical messages about issues as important as changing the delivery method for Medicaid.
Study Limitations
The study has some notable limitations. Firstly, the 5-item questionnaire that served as the primary study assessment instrument was not pre-tested. Secondly, assessment of participant understanding of the five knowledge areas that were studied was based solely on dichotomous responses to survey questions suggesting that interpretations of outcomes may have been understated or overstated. Thirdly, although the study targeted African Americans, a few participants (<1% of total participants) were of other races.
Funding Support
This study is funded by the Kate B. Reynolds Charitable Trust.
Acknowledgement
The authors acknowledge the immense support and contributions of members of the Community Medicaid Advisory Board of the Elizabeth City State University Medicaid Transition Evaluation of Eastern North Carolina (ECSUMEDITEEN) program – Rev Roy G. McPherson (Chairperson), Pastor Robert Lee, Sandra Jordan, Pastor Vickie Joyner, and Shirley Brown.
Conflict of Interest Statement
None.
References
- (2023) General Assembly of North Carolina. Session 2015. Session Law 2015-245, House Bill 372: An Act to Transform and Reorganize North Carolina’s Medicaid and NC Choice Programs.
- (2021) NC Medicaid Managed Care. North Carolina Department of Health and Human Services.
- Keast SL, Skrepnek G, Nesser N (2016) State Medicaid Programs Bring Managed Care Tenets to Fee for Service. J Manag Care Spec Pharm 22(2):145-148.
- (2023) NC Medicaid Enrollment Reports. North Carolina Department of Health and Human Services.
- Allen EH, Johnston EM, Courtot B, Caraveo CA, Gonzalez D, et al. (2022) North Carolina Medicaid’s Transition to Risk-Based Managed Care. Urban Institute.
- Aijaz M, Song PH, Winslow HC, Jackson J, Lewis VA, et al. (2022) Continuity through Disruption: Beneficiary Engagement Strategies during the Transition to Medicaid Managed Care in North Carolina. Academy Health Annual Research Meeting.
- Allen EH, Johnston EM, Courtot B, Caraveo CA, Gonzalez D, et al. (2022) North Carolina Medicaid’s Transition to Risk-Based Managed Care. Urban Institute.
- Zimmer RP, Hanchate AD, Palakshappa D, Sheena McNeill, Charlotte I. Crotts, et al. (2023) Perceptions of North Carolina’s Medicaid Transformation: A Qualitative Study. North Carolina Medical Journal 85(6).
- Katella K (2021) Our pandemic Year-A COVID-19 Timeline. Yale Medicine.
- (2024) Mayo Clinic. Engaging Black and African American Populations.
- Henry Akintobi T, Jacobs T, Sabbs D, Holden K, Braithwaite R, et al. (2020) Community Engagement of African Americans in the Era of COVID-19: Considerations, Challenges, Implications, and Recommendations for Public Health. Prev Chronic Dis 17: E83.
- Berg S (2020) 7 ways to improve Black health-in mind and body.
- Cramer ME, Lazoritz S, Shaffer K, Palm D, Ford AL (2018) Community Advisory Board Members’ Perspectives Regarding Opportunities and Challenges of Research Collaboration. West J Nurs Res 40(7): 1032-1048.
- Newman SD, Andrews JO, Magwood GS, Jenkins C, Cox MJ, et al. (2011) Community advisory boards in community-based participatory research: a synthesis of best processes. Prev Chronic Dis 8(3): A70.
- Wilson C (2018) Grassroots Community outreach and engagement.
- (2024) North Carolina's Transformation to Medicaid Managed Care. North Carolina Department of Health and Human Services.
- (2023) View health plans. North Carolina Department of Health and Human Services.
- (2023) Questions and Answers about Medicaid Expansion. North Carolina Department of Health and Human Services.
- Mbe KA (2017) Culturally Competent Health Education in African Americans’ Faith-based Communities for Better Health Outcomes: A Literature Review. McNair Research Journal SJSU 13.
- Linnan LA, Ferguson YO (2007) Beauty Salons. A Promising Health Promotion Setting for Reaching and Promoting Health Among African American Women. Health Educ Behav 34(3): 517-530.
- Brewer LC, Williams DR (2019) We've Come This Far by Faith: The Role of the Black Church in Public Health. Am J Public Health. 109(3): 385-386.
- Hays K, Aranda MP (2016) Faith-based mental health interventions with African Americans: A review. Research on Social Work Practice 26(7): 777-789.
- Markens S, Fox SA, Taub B, Gilbert ML (2002) Role of Black churches in health promotion programs: lessons from the Los Angeles Mammography Promotion in Churches Program. Am J Public Health. 92(5): 805-810.
- Moore T (1991) The African American church: A source of empowerment, mutual help, and social change. Prevention in Human Services, 10(1): 147-167.
- Pratt CC, McGuigan WM, Katzev AR (2000) Measuring program outcomes: Using retrospective pretest methodology. American Journal of Evaluation 21(3): 341-349.
- Gouldthorpe O Leary JL, Israel GD (2013) Capturing Change: Comparing Pretest-Posttest and Retrospective Evaluation Methods. 2013(1).
- Dalumpines L (2011) Objective types of test: Guidelines for writing completion questions and true-false questions.
- Treser M (2015) True/False Questions: Getting Them Right. Elearning Industry.
- Davis GC, Baral R, Strayer T, Serrano EL (2018) Using pre-and post-survey instruments in interventions: determining the random response benchmark and its implications for measuring effectiveness. Public Health Nutr 21(6): 1043-1047.
- (2024) The definitive place to explore US public data. DATA USA.
- (2023) Questions and Answers about Medicaid Expansion. North Carolina Department of Health and Human Services.
- (2023) When Can I Switch Health Plans. NC Medicaid Ombudsman.
- (2023) Managed Care. Medicare.gov.
- (2023) NC Medicaid Managed Care FAQs. UNC Health.
- Engel Smith L (2021) NC Medicaid managed care information blitz did not reach all enrollees. North Carolina Health News.
- Zimmer RP, Hanchate AD, Palakshappa D, et al. (2023) Perceptions of North Carolina’s Medicaid Transformation: A Qualitative Study. North Carolina Medical Journal. 84(6).
- (2021) As NC’s Medicaid managed care transition draws near, consumers express concerns and confusion. NC Health News.
- (2020) North Carolina Data. March of Dimes Peristats.
- Volpe VV, Schorpp KM, Cacace SC, Benson GP, Banos NC (2021) State- and Provider-Level Racism and Health Care in the U.S. Am J Prev Med 61(3): 338-347.
- Kennedy BR, Mathis CC, Woods AK (2007) African Americans and their distrust of the health care system: healthcare for diverse populations. J Cult Divers 14(2): 56-60.
- (2020) New Nationwide Poll by the Kaiser Family Foundation and The Undefeated Reveals Distrust of the Health Care System Among Black Americans. Kaiser Family Foundation.
- Okoro ON, Nelson CS, Witherspoon SP, Witherspoon SF, Simmons GE Jr (2020) Culturally Responsive Health Promotion to Address Health Disparities in African American Men: A Program Impact Evaluation. Am J Mens Health 14(4):1557988320951321.
- Daniels EC, Powe BD, Metoyer T, McCray G, Baltrus P, et al. (2012) Increasing knowledge of cardiovascular risk factors among African Americans by use of community health workers: The ABCD community intervention pilot project. J Natl Med Assoc104(3-4): 179-185.
- Peña Purcell NC, Jiang L, Ory MG, Hollingsworth R (2015) Translating an evidence-based diabetes education approach into rural African American communities: The “wisdom, power, control” program. Diabetes Spectrum 28(2): 106-115.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.