Case Report 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Intermittent Oscillopsia and Tinnitus: A Case of Vestibular Paroxysmia
*Corresponding author: Fabian H Rossi, Department of Neurology, Orlando VA Medical Center Professor Neurology, UCF Medical School, USA.
Received: July 29, 2024; Published: August 07, 2024
DOI: 10.34297/AJBSR.2024.23.003100
Case Report
73-year-old white male with 15-year-history of intermittent stereotype episodes of non-spinning dizziness. He describes the episodes as a sudden sensation of shaking like if he was in an earthquake followed by a significant exacerbation of his underlying right tinnitus. These spells last for 15 and 20 seconds and occur with a frequency of 60-70 per day. These episodes have no triggers. He has history of migraine headaches, but none of his headache attacks are associated with these episodes of dizziness. He denied nausea and vomiting, weakness, paresthesia, and changes in mentation. Neuro-ophthalmological and neuro-otologic examination were unremarkable. Hallpike maneuver was negative. Vestibular laboratory testing revealed a right vestibular peripheral deficit with a caloric testing weakness [functional reduction of 65%] on the right and head-shaking-induced nystagmus towards the left. Audiogram showed a moderate to severe bilateral sensory neural deficit. A cardiac evaluation with a Holter during the dizziness attacks was unremarkable. Laboratory investigations including complete metabolic panel, inflammatory markers, syphilis, and cells counts were all unremarkable. Head MRI showed normal brain parenchyma and ventricular system. An axial T2-weighted sequences of the posterior fossa showed a vascular loop compressing the right eight cranial nerve. The MRA of his neck and head reveal no stenosis. Vestibular rehabilitation and therapy with meclizine had no effect, however he became asymptomatic with carbamazepine at the dosage of 200MG three times daily.
These findings support the diagnosis of Vestibular Paroxysmia [VP]. VP is a rare syndrome caused by neurovascular cross-compression of the vestibulocochlear nerve that present with intermittent spontaneous vertigo [1,2] (Figure 1).
The mean age of presentation is 50 years of age, when affect younger patients the vascular compression is caused by a congenital vascular anomaly, but when VP affect middle-aged patients the most common caused is an aberrant vascular anatomical abnormality such as vessel lengthening or widening from age-related atherosclerosis and/or hypertension [3]. The most likely explanation of VP is a vascular compression of the vestibular nerve by an arterial loop that led to nerve hyperactivity. The chronic external pulsatile nerve compression by the artery lead to demyelination and decreased firing threshold making the nerve more susceptible to discharge. This mechanism is called ephaptic transmission and represent the coupling of action potentials via current flow through the extracellular space between adjacent axons. The site of neurovascular compression on the vestibular nerve is located within 10 mm from the brainstem. The arteries from the cerebellar pontine angle, especially the anterior inferior cerebral artery less likely the PICA, are the most common arteries compressing this nerve, and rarely a vein [1-4].
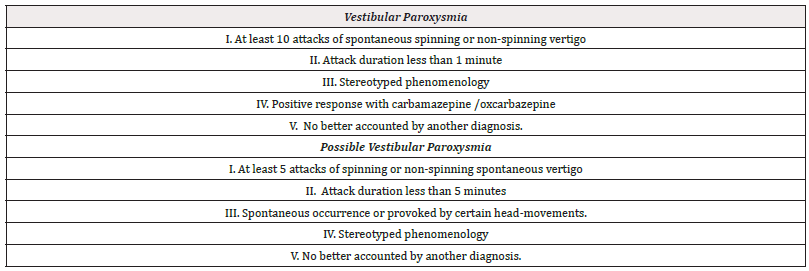
The key features of VP are brief attacks of spinning or non-spinning vertigo, binocular oscillopsia [illusory movements of the environment] and/or abrupt unsteadiness or instability of posture and gait that last less than a minute; attacks occur multiple times per day [frequencies up to 30 or more attacks per day are not uncommon], and attacks occur spontaneously, however, spells may be triggered head turning, positional changes, loud noise and hyperventilation. Attacks might or not be associated with tinnitus and hypo- or hyperacusis. Neuro-otological examination in between attack is normal, though hyperventilation while using Frenzel glasses to eliminate fixation, might trigger a nystagmus in direction to the affected ear [excitatory nystagmus] [1,3-5]. The clinical diagnostic criteria for vestibular paroxysmia defined by the Classification Committee of the Barany Society displayed in Table 1 where each point need to be present to fulfill the diagnosis or possible diagnosis of VP [5] (Table 1).
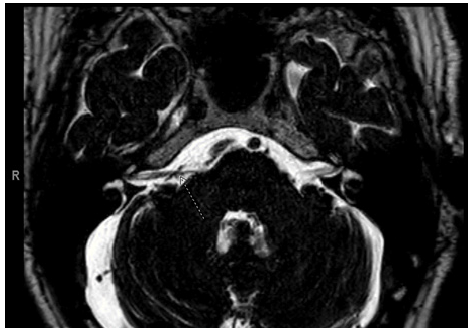
Figure 1: T2-weighted axial images of the internal auditory canal showing a right aberrant anterior inferior cerebellar artery compressing the right vestibulocochlear nerve [arrow].
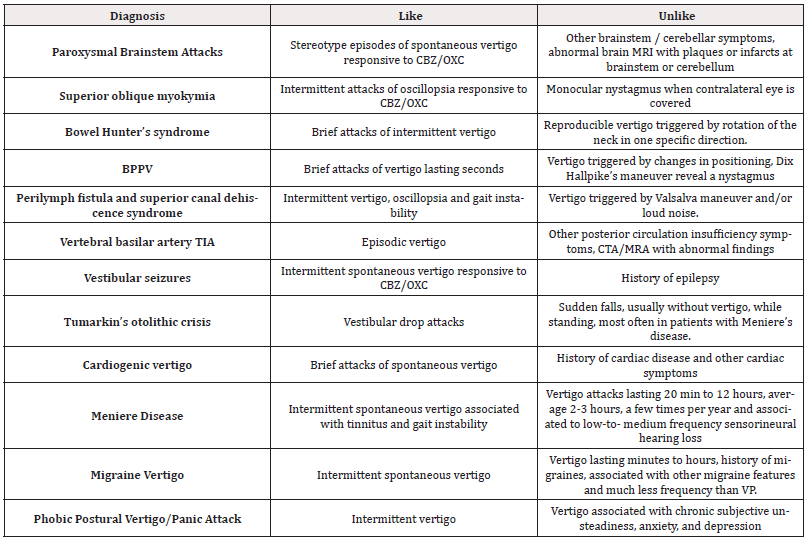
Vestibular laboratory testing may reveal signs of unilateral vestibular hypofunction during head-shaking nystagmus test, head impulse test and caloric irrigation in between the attacks in half or less of the patients [1,4,5]. MRI is the diagnostic test of choice for identification of the neurovascular compression. Constructive Interference in Steady State [CISS] and Fast Imaging Employing Steady State Acquisition [FIESTA] can display the neurovascular compression and to exclude cerebellar pontine angle lesions such as tumor, arachnoid cyst, or multiple sclerosis plaques or vascular lesions [6-8]. The diagnosis of VP is straightforward base on short duration, high frequency, and positive response to carbamazepine. However, some vertiginous conditions need to be included in the differential diagnosis of VP such as central positional nystagmus (cerebellar or brainstem lesions), benign paroxysmal positional vertigo, bowel Hunter's syndrome (vertebrobasilar insufficiency from vertebral artery occlusion during neck rotation), perilymph fistula, epileptic vertigo, and cardiogenic dizziness. In the case of possible VP, it needs to be differentiated from Meniere’s disease, migraine-vertigo syndrome, and superior canal dehiscence, refer to Table 2 [4].
Paroxysmal brainstem attacks are caused by damage of the brainstem by multiple sclerosis plaques or vascular lesions resulting in brainstem ephaptic discharges. Patients present with intermittent attacks of vertigo responding to carbamazepine, however other features such as dysarthria, paroxysmal weakness, intermittent dysesthesias, analgesia or pain, autonomic dysregulation and ataxia could be present. Brain MRI with thin sequences across the brainstem reveals the lesions [4,5,9]. Superior oblique myokymia is another neurovascular syndrome caused by compression of the trochlear nerve. It presents with frequent paroxysmal torsion of one eye with sudden monocular vertical rotatory oscillopsia that respond to carbamazepine. Eye exam reveals a rapid nystagmoid movement when contralateral eye is covered, not seen in VP [10].
Bowel Hunter's syndrome occur when the head is turned to one direction that leads to rotational occlusion of the dominant vertebral artery and vertebrobasilar insufficiency, usually from cervical spondylosis. Patients have a reproducible sharp vertigo with nystagmus and gait instability every time the head is turned in a specific direction, not seen in VP. Cerebral angiography and/or CT/MR angiogram of head and neck may reveal the vascular occlusion [11]. Cardiogenic dizziness: dizziness or vertigo lasting for second to minutes caused by cerebral hypotension from low cardiac output from a paroxysmal cardiac arrythmia, cardiomyopathy or other cardiac sources [5]. Patients have history of cardiac disease and associated cardiac symptoms. Perilymph fistula and superior canal dehiscence syndrome are two conditions presenting with loud noise induced vertigo [Tullio phenomenon] and/or changes in pressure [e.g., coughing, pressing, sneezing, or lifting] induced vertigo, oscillopsia and/or instability of posture and gait that last for seconds to days [4].
Benign Paroxysmal Positional Vertigo [BPPV] is the most common form of peripheral vestibulopathy that present with vertigo and nystagmus induced by changes of head or body position relative to gravity [e.g., standing up, rolling over-the-bed, looking up, etc.]. Its diagnosis is supported by the Dix-Hallpike test that in the case of the posterior semicircular BPPV, the most common form of BPPV, it reveals an up-beat nystagmus [12]. Vestibular seizures, a rare form of cortical seizures originated from the temporal lobe that present with a sudden sensation of vertigo, disequilibrium, mild nausea (vomiting is rare), tinnitus with or without nystagmus. These seizures last for a few seconds or minutes and affect patients often with history of seizures [13]. Tumarkin’s otolithic crisis (“vestibular drop attacks”) patients feel forcefully thrown to the ground, typically while standing, contrary to VP that occur from any position. These sudden falls are usually not accompanied by vertigo and occur in patients with history of Meniere’s disease. The frequency of the otolithic attacks is about 2-3 per year, when in VP the frequency is multiple times a day [5]. Orthostatic hypotension could present with brief vertigo when patient stand up, a down beat or horizontal nystagmus may be present. Recording of blood pressure from supine to standing confirm its diagnosis [14].
Vestibular migraines may present with spontaneous vertigo that lasts from 5 min to 72 hours in patients with history of migraines where most of the vertigo attacks are associated with other migraine symptoms. Migraine vertigo rarely lasts for seconds and does not present with multiple attacks per day like VP [15]. Meniere’s disease present with vertigo, cochlear symptoms [roaring or rushing tinnitus, aural fullness, or pressure] tinnitus and hearing loss (distorted, or muffled hearing). The duration of the attacks last 20 minutes to several hours with a frequency 4-to-6 attacks per year that declined overtime until eventually burnout. During the attacks most patients have spontaneous horizontal nystagmus that ultimately reverses direction during the attack associated with unsteadiness and motion intolerance. Patients have a low-to-medium sensorial neural hearing loss that worsen progressively over time [16]. Vertebral basilar TIA: uncommon cause of episodic vertigo that might occur a few days or weeks prior to the stroke. It could happen in isolation or associated with other posterior circulation features [e.g., dysarthria, hemi-paresthesia, diplopia [17]. Phobic postural vertigo is a neurological functional disorder where head movements might induce a sensation of body perturbation like in VP. However, symptoms occur in conjunction with chronic subjective unsteadiness associated with fear of falling without falls and with the comorbidity of anxiety and depression [4]. Panic attack consist of an abrupt onset of irrational fear and anxiety associated with dizziness, lightheadedness, chest pain, shortness of breath and unsteadiness lasting for minutes [4,5].
Vestibular paroxysmia is a treatable cause of dizziness. The treatment consists in the use of carbamazepine [200 to 800 mg a day] or oxcarbazepine [300 to 900 mg a day] which are considered the first line of therapy, usually very effective. Lacosamide [100 to 200 mg per day] could be considered when above medication is not tolerated or contraindicated. If patients fail the first line of therapy, neurosurgical intervention with microvascular decompression is warranted [18,19].
Abbreviations:
CBZ: Carbamazepine; OXC: Oxcarbazepine; SDS: Superior dehiscence syndrome, VP: Vestibular paroxysmia.
Acknowledgments
None.
Conflict of Interest
None.
References
- Michael Strupp, Jose A Lopez Escamez, Ji Soo Kim, Dominik Straumann, Joanna C Jen, et al. (2016) Vestibular Paroxysmia: Diagnostic Criteria. J Vestib Res 26(5-6): 409-415.
- Hüfner K, Barresi D, Glaser M, et al. (2008) Vestibular Paroxysmia. Neurology 71(13):1006-1014.
- Steinmetz K, Becker Bense S, Strobl R, Grill E, Seelos K, et al. (2022) Vestibular paroxysmia: clinical characteristic and long-term course. Journal of Neurology 269: 6237-6245.
- Brandt T, Strupp M, Dieterich M (2016) Vestibular Paroxysmia: A Treatable Neurovascular Cross-Compression Syndrome. J Neurol 1: 90-96.
- Eggers SDZ (2021) Episodic Spontaneous Dizziness. Continuum 27(2): 369-401.
- Karamitros A, Kalamatianos T, Stranjalis G, Anagnostou E (2021) Vestibular Paroxysmia: Clinical Features and Imaging Findings; a Literature Review. J Neuroradiol 49(2): 225-233.
- Haller S, Etienne L, Kövari E, Varoquaux AD, Urbach H, et al. (2016) Imaging of Neurovascular Compression Syndromes: Trigeminal Neuralgia, Hemifacial Spasm, Vestibular Paroxysmia, and Glossopharyngeal Neuralgia. AJNR Am Neuroradiol 37(8): 1384-1392.
- Strupp M, von Stuckrad Barre S, Brandt T, Tonn JC (2013) Teaching neuroimages: Compression of the eighth cranial nerve causes vestibular paroxysmia, Neurology 80(7): 77.
- Li Y, Zeng C, Luo T (2011) Paroxysmal dysarthria and ataxia in multiple sclerosis and corresponding magnetic resonance imaging findings, J Neurol 258(2): 273-276.
- Adamec I, Habek M (2018) Superior Oblique Myokymia. Pract Neurol 18(5): 415–416.
- Strupp M, Planck JH, Arbusow V, Steiger HJ, Bruckmann H, et al. (2000) Rotational vertebral artery occlusion syndrome with vertigo due to “labyrinthine excitation”, Neurology 54:1376-1379.
- Von Brevern M, Bertholon P, Brandt T, Fife T, Imai T, et al. (2015) Benign paroxysmal positional vertigo: Diagnostic criteria, J Vestib Res 25(3-4): 105-117.
- Tarnutzer A, Lee SH, Robinson K, Kaplan P, Newman Toker D (2015) Clinical and electrographic findings in epileptic vertigo. A systematic review. Neurology 84(15): 1595-1604.
- Choi JH, Seo JD, Kim MJ, Choi BY, Choi YR, et al. (2015) Vertigo and nystagmus in orthostatic hypotension, Eur J Neurol 22(4): 648-655.
- Lempert T, Olesen J, Furman J, Waterston J, Seemungal B, et al. (2012) Vestibular migraine: Diagnostic criteria, J Vestib Res 22(4): 167-172.
- Lopez Escamez JA, Carey J, Chung WH, Goebel JA, et al. (2015) Diagnostic criteria for Meniere’s disease, J Vestib Res 25(1): 1-7.
- Paul NL, Simoni M, Rothwell PM (2013) Transient isolated brainstem symptoms preceding posterior circulation stroke: A population-based study, Lancet Neurol 12(1): 65-71.
- Hufner K, Barresi D, Glaser M, Linn J, Adrion C, et al. (2008) Vestibular paroxysmia: Diagnostic features and medical treatment, Neurology 71(13): 1006-1014.
- Jankowska K, Pietrzak N, Rosiak O, Knopka W (2023) Literature review and two study cases of vestibular paroxysmia from an otorhinolaryngology centre. J Hear Sci 13:16-25.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.