Case Report 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Acute Pancreatitis Caused by Cytomegalovirus: An Unusual Cause of Acute Pancreatitis in an Immunocompetent Patient
*Corresponding author: Roun Kim, Specialist in General Surgery, General Hospital of Luque, Catholic University of Nuestra Señora de la Asuncion- Faculty of Medicine and Health Sciences, Paraguay.
Received: October 18, 2024; Published: October 23, 2024
DOI: 10.34297/AJBSR.2024.24.003206
Abstract
Cytomegalovirus (CMV) is a double-stranded DNA virus that belongs to the herpes family (Herpesviridae) and infects a large portion of the adult population. In immunocompetent patients, it is usually asymptomatic or presents with mild, self- limited symptoms similar to the flu, while in immunocompromised patients, it can cause severe disease. This case is based on acute pancreatitis caused by cytomegalovirus (CMV) in a 25-year- old immunocompetent male. The diagnosis of CMV-induced pancreatitis was based on clinical presentation and the detection of IgM and IgG antibodies in the blood, ruling out other causes. The patient developed pancreatic necrosis involving less than 50%, which did not require surgical treatment (Balthazar D).
He received conservative medical treatment with good clinical and laboratory recovery, remaining asymptomatic for more than one month after the confirmation of the causative agent.
This is a rare case of CMV-induced pancreatitis in an immunocompetent patient, which highlights the need for diagnostic suspicion in cases of acute pancreatitis where common causes have been ruled out. This approach can lead to appropriate treatment and positive outcomes.
Keywords: Pancreatitis, Cytomegalovirus, Pancreatic necrosis, Immunocompetent
Clinical Case
A 25-year-old male with no underlying conditions was admitted for severe abdominal pain. He had a history of abundant liquid stools for 3 days, with no blood or mucus, accompanied by generalized weakness. Two days prior to admission, he experienced multiple episodes of nausea and vomiting with food contents. Symptoms persisted, and 24 hours before admission, he developed epigastric pain described as stabbing, moderate in intensity, radiating to both hypochondria, and progressively worsening. The patient denied any previous similar episodes. Upon admission, he was afebrile with stable vital signs. Physical examination revealed a mildly distended abdomen, tender to palpation in the epigastrium, with guarding but without signs of peritoneal irritation.
Initial lab work showed Hb of 13.8g/dL, Hct 42%, WBC 17,360/mm³ with 93% segmented neutrophils, and platelets 210,000/mm³. Urea was 25mg/dL, creatinine 0.7mg/dL, and electrolytes were within normal limits. Liver function tests revealed GOT 21U/L, GPT 12U/L, total bilirubin 1.07mg/dL with direct bilirubin 0.44mg/dL, and alkaline phosphatase 80U/L. Amylase returned at 966U/L.
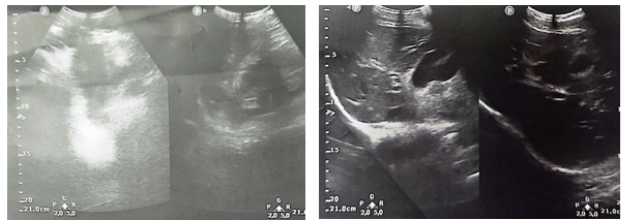
A diagnosis of mild acute pancreatitis was made based on Apache score of 0, BISAP score of 0, Marshall score of 0, and Japanese score of 0. An abdominal ultrasound and lipid profile were requested to investigate the cause of acute pancreatitis. The lipid profile returned normal with total cholesterol at 175mg/dL (HDL 74mg/dL, LDL 93mg/dL, VLDL 8mg/dL, TG 41mg/dL). The abdominal ultrasound showed a normal liver, a distended gallbladder with thin walls, no evidence of gallstones, and non-dilated intrahepatic bile ducts. The common bile duct was of normal caliber, and the pancreas appeared normal in size and echotexture. However, a small amount of fluid was noted in the right paracolic gutter, along with significant distension of intestinal loops with gaseous content in the epigastric area (Figure 1).
On the second day of hospitalization and the fifth day of illness, due to persistent abdominal pain without improvement, accompanied by a fever spike of 38.4°C and the presence of an epigastric mass on physical examination, a contrast-enhanced CT scan was ordered due to suspicion of local complications. Blood tests were repeated, including procalcitonin levels and blood cultures. In the meantime, the patient received only symptomatic treatment without antibiotics. Laboratory results returned with Hb 13.2g/dL, Hct 39%, WBC 17,270/mm³ with 82% segmented neutrophils, platelets 192,000/mm³. Creatinine was 0.7mg/dL, electrolytes were within normal limits. Liver function tests showed GOT 22U/L, GPT 11U/L, total bilirubin 0.77mg/dL with direct bilirubin 0.33mg/dL, amylase 509U/L, and lipase 312U/L. Procalcitonin was 0.3ng/mL, and no bacterial growth was observed in the blood culture. The contrast-enhanced abdominal and pelvic CT scan revealed a normal liver and gallbladder with no tomographically evident alterations. The pancreas was globally enlarged, with the head measuring 48mm in its craniocaudal diameter, and the margins were diffuse with peripancreatic fat stranding and adjacent fluid collections extending along the left paracolic gutter down to the pelvic cul-de-sac. There was homogeneous enhancement in the head and body of the pancreas, with decreased enhancement noted in the tail, suggesting a possible necrotic area involving less than 30% of the parenchyma. The main pancreatic duct was preserved caliber. These findings were consistent with acute pancreatitis with peripancreatic fluid collections, a tomographic severity index of 5 points, classified as moderate pancreatitis (Balthazar D), with probable necrosis involving less than 30% of the pancreas (Figure 2).
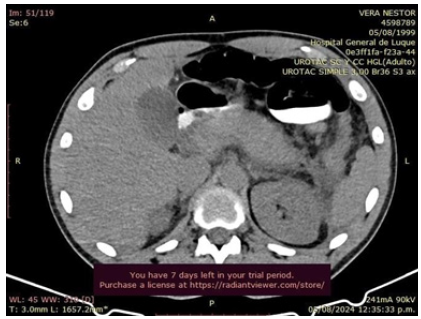
Figure 2: Contrast-Enhanced CT Abdomen. Peripancreatic fluid collections. Balthazar D, probable necrosis less than 30%.
The patient underwent imaging studies, which revealed an acalculous gallbladder, normal lipid profile, and normal calcium levels. There was no history of abdominal trauma, only occasional alcohol consumption, and no medication use that could have side effects resulting in pancreatitis. Therefore, after ruling out more common causes of acute pancreatitis [1-3] (Table 1), additional laboratory tests and an MRCP (Magnetic Resonance Cholangiopancreatography) were requested in search of a definitive diagnosis for the patient.
Laboratory results returned as follows: C3 complement 163mg/dL, C4 complement 30mg/dL, Hepatitis B surface antigen non-reactive, VDRL non-reactive, HIV antibodies non-reactive. Total Anti-Hepatitis A antibodies 0.9140 COI (COI <1.0 Positive reactive for Anti-HAV antibodies), Anti-Hepatitis C antibodies (HCV) 0.0451 COI (COI <0.9 non-reactive). Double-stranded DNA antibodies (DNAds) negative, ANA (antinuclear antibodies) total negative. Epstein-Barr virus (EBV-VCA) IgM and IgG antibodies were negative. Notably, the patient had elevated levels of Cytomegalovirus (CMV) antibodies: IgM 2.01 and IgG 14.9U/mL, both positive, which provided a conclusive diagnosis for CMV as the cause of acute pancreatitis. A follow-up procalcitonin level was 0.2ng/mL.
The MRCP report showed a well-distended gallbladder with thin, regular walls, with filling defects suggestive of stones. The cystic duct was appropriately implanted at the posterior margin of the proximal common bile duct. No bile duct dilatation was observed. Signs of pancreatitis with a peripancreatic collection were noted (Figure 3).
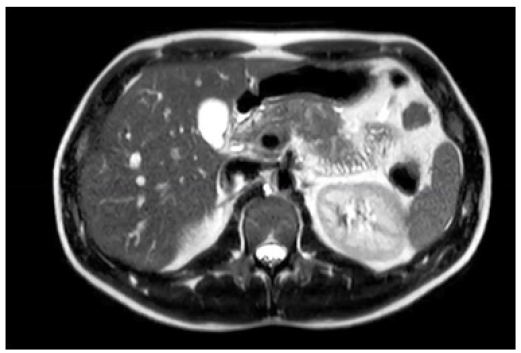
Figure 3: CRMN. Gallbladder shows absence of filling suggestive of stones. Signs of pancreatitis with peripancreatic collection.
The patient showed good clinical and laboratory progress during hospitalization with conservative medical treatment. There was clinical improvement in the pain, the patient remained afebrile, tolerated oral intake well, and maintained normal bowel function. He was discharged on the 6th day of hospitalization, the 9th day of illness, with plans to perform a follow-up CT scan with contrast in 15 days and outpatient follow-up. During his follow-up visits, the patient remained asymptomatic with good tomographic improvement of pancreatic inflammation and necrosis.
Discussion and Case Analysis
Cytomegalovirus (CMV), or human herpesvirus (HHV-5), belongs to the Herpesviridae family. CMV infection in immunocompetent individuals is usually asymptomatic, and clinically significant infection is considered rare in these patients. According to National Health and Nutrition Examination Surveys (NHANES) from 1988-2004, CMV seroprevalence in the United States ranged from 32-90%, with higher rates in females, individuals born abroad, those from lower socioeconomic backgrounds, households with high crowding, and individuals with lower education levels [4].
In immunocompetent patients, this infection generally presents as a benign, self- limiting syndrome. Conversely, in immunocompromised patients, CMV can cause significant morbidity and mortality, particularly in those with HIV, organ transplant recipients, and newborns [4,5].
Multiple organ systems can be affected by CMV infection, most commonly manifesting as colitis, gastritis, gastric ulcers, hepatitis, pancreatitis, duodenitis, or enteritis [6-10]. Other systems that can be affected include the central nervous system, hematologic system, vascular system, and lungs.
Currently, there are very few documented cases of CMV infection in immunocompetent patients. Diagnosing CMV-related pancreatitis is more challenging compared to other CMV infections in the gastrointestinal tract. In general, pancreatic biopsy is not recommended. In this case, the diagnosis was made by excluding more common causes and confirming positive results for CMV IgM and IgG antibodies. Despite the challenges in diagnosing and predicting CMV complications, patients tend to have favorable outcomes when treated.
Guidelines for immunocompromised patients recommend IV ganciclovir or oral valganciclovir. However, there are no clear guidelines on antiviral use in immunocompetent patients. In this case, the patient did not receive antiviral treatment due to his good progress and complete resolution of symptoms. In the absence of multicenter trials, initiating antiviral treatment is at the discretion of the treating physician. Literature shows better outcomes in immunocompetent patients who received treatment [2].
The patient underwent a follow-up contrast-enhanced CT scan on the 15th day of illness, which showed a pancreas that was still slightly enlarged globally with laminar fluid adjacent to it, compared to the previous CT. There was good homogeneous enhancement throughout the parenchyma, without areas of necrosis, and the main pancreatic duct remained of normal caliber. (Figure 4) Control IgM and IgG antibody levels for CMV were also tested, returning IgM as non-reactive at 0.8 (Reference value: Non- reactive < 0.9) and IgG at 308UI/mL [11,12].
Conclusion
CMV disease is typically self-limiting in immunocompetent patients. Pancreatitis and pancreatic necrosis secondary to CMV are rare; however, they should be considered in the differential diagnosis. This highlights the importance of sharing this clinical case.
Ethical Considerations
No ethical issues were identified in the management of this clinical case. Informed consent was obtained from the patient for the publication of his medical history.
Funding Sources
This study did not receive any external funding.
Author Contributions
All authors were involved in the patient’s care and contributed to the preparation of the manuscript.
Conflict of Interest
The authors declare no conflicts of interest related to this work.
References
- Leppäniemi A, Tolonen M, Tarasconi A, Segovia Lohse H, Gamberini E, et al. (2019) 2019 WSES guidelines for the management of severe acute pancreatitis. World J Emerg Surg 14: 27.
- Tenner S, Baillie J, DeWitt J, Vege SS (2013) American College of Gastroenterology guideline: Management of acute pancreatitis. Am J Gastroenterol 108(9): 1400-1415.
- Forsmark CE, Baillie J (2007) AGA institute technical review on acute pancreatitis. Gastroenterology 132(5): 2022-2044.
- Bate SL, Dollard SC, Cannon MJ (2010) Cytomegalovirus seroprevalence in the United States: National Health and Nutrition Surveys, 1988-2004. Clin Infect Dis 50(11): 1439-1447.
- Rafailidis PI, Mourtzoukou EG, Varbobitis IC, Falagas ME (2008) Severe cytomegalovirus infection in apparently immunocompetent patients: a systematic review. Virol J 5:47.
- Ebisutani C, Kawamura A, Shibata N, Nasu M, Ueno R, et al. (2012) Cytomegalovirus-associated gastric ulcer in an immunocompetent patient: diagnostic method. Case Rep Gastroenterol 6(2): 365-368.
- Krajicek E, Shivashankar R, Hansel S (2017) Cytomegalovirus and the apparently immunocompetent host: a case of perforating gastric ulcer. ACG Case Rep J 4: e27.
- Chan A, Bazerbachi F, Hanson B, Alraies MC, Duran Nelson A (2014) Cytomegalovirus hepatitis and pancreatitis in immunocompetent patients. Ochsner J 14(2): 295-299.
- Yasumoto N, Hara M, Kitamoto Y, Nakayama M, Sato T (1992) Cytomegalovirus infection associated with acute pancreatitis, rhabdomyolysis, and renal failure. Intern Med 31(3): 426-430.
- Oku T, Maeda M, Waga E, Wada Y, Nagamachi Y, et al. (2005) Cholangitis and cytomegalovirus pancreatitis in an immunocompetent patient. J Gastroenterol 40(10): 987-992.
- Sakakibara Y, Nakazuru S, Kodama Y, Mita E (2018) Acute pancreatitis caused by cytomegalovirus-associated duodenal papillitis. Ann Gastroenterol 31(1): 122.
- Eddleston M, Peacock S, Juniper M, Warrell DA (1997) Severe cytomegalovirus infection in immunocompetent patients. Clin Infect Dis 24(1): 52-56.




 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.