Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Effects of a Youth Diabetes Prevention Program on Health-Related Outcomes in Overweight Male Adolescents
*Corresponding author: Chiung-Jung (Jo) Wu, School of Nursing, Midwifery and Paramedicine, University of the Sunshine Coast. 1 Moreton Parade, Petrie, Qld 4502, Australia, Email: cwu@usc.edu.au
Received: March 09, 2020; Published: March 17, 2020
DOI: 10.34297/AJBSR.2020.08.001254
Abstract
Background: The prevalence of overweight and obesity among adolescents increases risks of developing type 2 diabetes. A diabetes education program based on dieting, exercise and psychosocial supporting is effective for weight reductions. However, little information is found about the effect of such intervention program specifically designed for adolescents.
Purpose: To evaluate youth diabetes prevention program in improving health-related outcomes in overweight male adolescents.
Methods: A quasi-experimental research design was used. A total of 50 participants aged 16-18 years with body mass index (BMI) ≥ 24 were recruited into either the intervention group (n = 25) or control group (n = 25). Intervention group received program included school general exercise training program plus youth diabetes prevention program for 8 weeks. Control group received school general exercise training program. The primary health-related outcomes included mean body weight (kilograms), BMI (kg/m2), percentage of body fat (%), visceral fat (%), waist circumference (centimeters) and secondary outcome was cardio-respiratory endurance test (minutes). Data were collected two group at baseline (T1), four weeks (T2), and eight weeks (T3). Independent t-tests were used to summarize demographic data and measure group differences in T1. The generalized estimating equations (GEEs) statistical test were used for analyzing interval outcome variables between groups overtime.
Results: There were 45 out of 50 participants completed the study. Significant interaction effects between three time points and two different groups in body fat (Waldχ2 = 16.99), visceral fat scores (Waldχ2 = 216.60), waist circumference (Waldχ2 = 969.72), and cardio-respiratory endurance (Waldχ2 = 492.79) were found. However, no significant results found in the body weight and BMI.
Conclusions: Results provided evidence to support the efficacy of the youth diabetes prevention Program in weight reductions. The findings suggested future implications could consider such programs using face-to-face, dietary modification, peer support and aerobic plus resistance exercise to assist adolescents in managing their health-related outcomes.
Keywords: Youth Diabetes Prevention Program, Overweight, Obese, Adolescents
Abbreviations: BMI: Body Max Index, GEEs: Generalized Estimating Equations
Introduction
The prevalence of overweight and obesity rise dramatically globally, with 39% accounted for being overweight and 13% being obese [1]. Childhood obesity is associated with premature death, disability, and increased risks of diabetes, cardiovascular disease, hypertension and several types of cancer in adulthood [2]. The prevalence of overweight in age 5-19 was 18% of girls and 19% of boys, and 6% of girls and 8% of boys were obese [2]. Among Asian populations, Taiwan has the highest prevalence of overweight and obesity with 26.7% in elementary school, 25.2% in junior high school (33.3% for boys; 25.2% for girls) and 26.7% are in high school [4, 51, 52].
Overweight is defined as the Body Max Index (BMI) range of 24-27kg/m2; and > 27 kg/m2 as obesity [3]. In Taiwan, almost half of adults (45.4%) are either overweight or obese [4 , 51, 52] which is accounted for approximately 32.4% of the adult population compared with other areas in Asia and the Pacific regions. Children with overweight or obesity are the primary predictors to become obesity in adolescents [5,6]. These adolescents are at risks of developing type 2 diabetes [7,8]. Therefore, there is an urgent need to prevent overweight or obesity-induced diseases [9,10].
Overweight is a complex issue resulting from the interactions of multiple genetic, metabolic, social, behavioral and cultural factors [11,12]. Contributing factors include increased use of devices, such as a smart phone, tablet, declined regular exercise and vigorous activity, as well as increasing consumption of fatty food and high sugar contents drinks [13,14]
Lifestyle modifications have been proven to reduce risks of type 2 diabetes in adulthood [15]. A systematic review on obesity prevention and intervention programs for adolescents with weight issues showed no conclusive evidence in a specific approach [16]. It is however recommended the needs of extreme precautions on using dangerous weight control medications or behaviors, such as diet pills, self-induced vomiting, laxatives, diuretics, or combinations [17]. Safe and effective interventions to address adolescent overweight and obesity should embed diet modification and incorporated physical exercise into creative activities and group social interactions [11,18].
Adolescents often value the importance of social interactions with peers, and food is an important part of the interactions [19,20]. However social interactions were diminished by obesity- associated low self-esteem, negative self-evaluation, decreased self-image, interpersonal problems, social discrimination, and depression [21,22]. In some cultures, including Taiwan, overweight adolescents are stigmatized by their peers, especially as they mature [23]. Because social networks are important to adolescents, prevention and treatment programs should have taken account of family and peer group, as well as considering the program in the schools for accessing necessary support [20]. Exercise with a peer group is more effective has been reported to have more uptake than traditional exercise programs [24-26] as it is perceived to be more fun, hence promoting adherence to exercise regimes and improving physical and psychosocial health in adolescents [25-29].
Traditional high school physical exercise programs have limited time to address diet and exercise activity, adolescents often feel bored and frustrated during these programs [30,31]. Literature showed that these programs has limited effects on behavior changes, and suggested understanding uncooperative problems [16,32]. Aerobic plus resistance training is effective for weight reductions, aiming in increasing lean body mass, muscle strength and physical fitness components [32,33].
Aim
The aim was to evaluate the effects of a youth diabetes prevention program for male adolescents.
Materials and Methods
Study design
A quasi-experimental research design was used due to absence of the randomization. Participants in the intervention group received youth diabetes prevention program that included aerobic plus resistance exercise for male, modify dieting and peer support for 8 weeks in additional to standard school general exercise training weight reduction program (control group). The standard program included 30-minute (5-minute warm-up, 20- minute jogging, and 5-minute cooldown) exercise three times a week, delivered by the school’s physical teacher [30]. The primary outcome included body weight, body mass index, body fat, visceral fat, waist circumference. Secondary outcome was cardio-respiratory endurance.
Participants
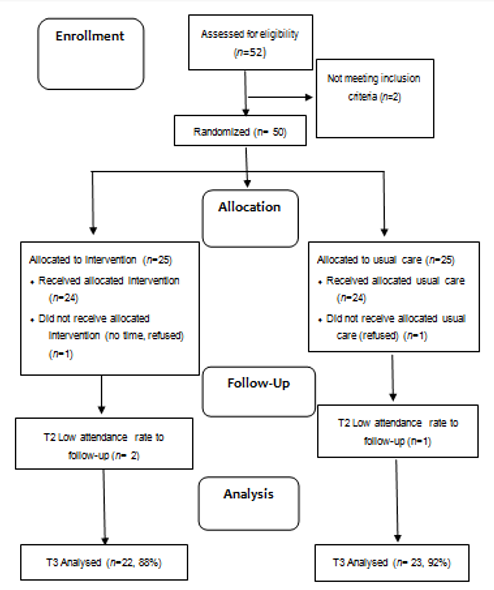
A total of 50 students who met the inclusion criteria from participating male senior high school in Southeastern Taiwan were recruited. Fifty students were randomly allocated to either the experimental group (n = 25) or the control group (n = 25) using the random numbers. Five adolescent students had withdrawn from the study due to personal time commitments, leaving 22 participants in the experimental group and 23 participants in the control group. There were no significant differences in baseline characteristics between withdrawn and completed participants (Figure 1).
Inclusion criteria were adolescents aged 16 to 18 years, BMI ≥ 24 kg/m2. Exclusion criteria were adolescents have already had a pre-existing disease, any orthopedic or joint problems restricting physical exercise, and on weight loss medications (Figure 1).
Sample size calculations
The sample size using the Statistical Software Sample Power 2.0 was calculated based on previously reported in weight changes and BMI in male adolescents [32]. With an effect size of 0.80 (power = 0.95; alpha = 0.05), at least 21 adolescents in each group were required to detect any statistically significant difference. An additional 20% attrition rates were anticipated, therefore 50 adolescents for two groups were needed.
Intervention – youth diabetes prevention program
The youth diabetes prevention program delivered by certified diabetes educator, consisted three key components: 1) one-hour structured face-to-face dietary modification sessions, 2) 20-minute peer support activity after the education, and 3) three 10-minute daily aerobic plus resistance exercise for eight weeks.
Face-to-face dietary modification session: The one-hour face-to-face session focused on dietary modification, was delivered by a certified diabetes educator and peer discussion. In the weekly dietary modification session, the educator provided behavior strategies and a food diary to participants, as well as introducing a new dietary modification topic daily. The dietary modification topic included less caloric and fat food selections, for example, more fruit and vegetable consumptions, choosing healthy beverage and snacks. The dietary also included demonstration of healthy home meals and highlighting the relationships between health and nutrition. Additional topics included managing junk food temptation through cognitive restructuring and problem-solving skills. All sessions were accompanied by approximately 20-minute peer support group discussions. During the peer discussion, the adolescents shared their own experience in challenges and success of food diaries, aerobic plus resistance exercise, issues relating to food choices and exercise regimes.
Aerobic plus resistance exercise: The exercise component consisted of three 10-minutes of concurrent aerobic plus resistance training for body composition program [33]. The aerobic plus resistance exercise included four minutes of vigorous body movement, three minutes of stretching and upper and lower muscle strength using isotonic and isometric exercises, two minutes of strengthening visceral muscles using 10-second intervals of holding different positions, and one minute of cooldown. Rock music with a strong beat accompanied exercise. A notebook was provided to individual student for recording participant’s own journey involving all program activities.
Measures and data collection
The health related outcomes included primary outcomes of mean body weight (kilograms), BMI (kg/m2), percentage of body fat (%), visceral fat (%), waist circumference (centimeters) were collected at baseline (T1), four weeks (T2), and eight weeks (T3) for intervention and control groups. The secondary outcome of completion time for the 1600-meter cardio-respiratory endurance test (minutes) was also collected at T1, T2 and T3. Data collection was undertaken by a trained research assistant who is blinded to the study protocol.
Body weight was measured. Height was measured in bare feet and without hair ornaments to the nearest 0.5cm using a HW-3050 stadiometer (Super-View Medical Co.). Waist circumference was measured to the nearest 0.1cm.the BMI was calculated by dividing weight (kg) by height squared (cm2). An HBF-370 meter (Omron Healthcare Co., Ltd.) measured visceral fat and body fat percentage. A digital stopwatch timer (Marathon Adanac 3000) measured in minutes and seconds the 1600-meter cardio-respiratory endurance as a physical fitness test. The physical education teacher told the adolescents to run as fast as they could around the school’s field track.
The activities for both the intervention and controls groups began approximately after collecting baseline measures. To ensure consistency and accuracy of the research protocol, one research assistant with a clinical background recorded data for the three time periods. If the attendance rate at any one session was≤ 50% (n=3), it was deleted from the study.
Data analysis
Data were analyzed using IBM®SPSS® version 22 statistical software. Descriptive statistics and Independent t-tests were used to summarize demographic data and measure group differences in T1. The generalized estimating equations (GEEs) statistical test was used for analyzing interval outcome variables such as weight, BMI, body fat, visceral fat, waist circumference, and cardio- respiratory endurance, correcting within-subject correlations, and conducting repeated measurement analysis. The GEEs detected body weight, BMI, body fat, visceral fat, waist circumference, and cardio- respiratory endurance on which time and group had interaction effects. For those variables on which time and group had interaction effects, GEEs were performed to analyze the differences among three time points within each group, and two groups at T2 and T3 controlling for T1. A p-value <.05 was set for a statistical significance.
Ethical considerations
Full ethics approval from University Hospital Institutional Review Board (IRB) of the human research ethics committees (approval number: 102056) and agreement from the participating school were obtained. Informed consent was acquired from individual adolescent’s guardian that explained the study’s purposes including the adolescents’ involvement in general activities related to exercise and education sessions about diet and assessment of physical measures. They were also told potential risks and benefits. Adolescents signed assent to participate. Privacy, confidentiality, and voluntary to participation were ensured in both of parents and adolescents. Data were kept in a secured university drive, protected by password, and only authorized research team member has access to the data.
Results and Discussion
Results
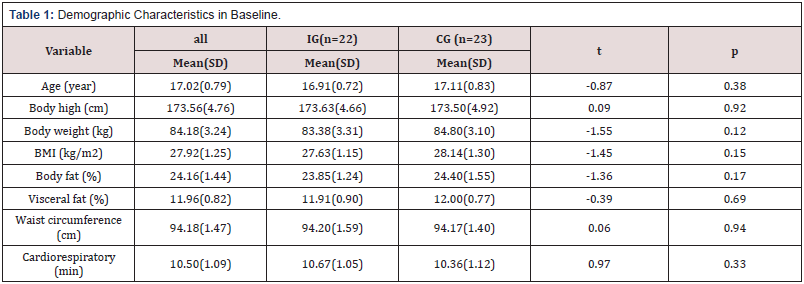
Demographical profiles: A total of 45 subjects completed the study, experiment (n = 22) and control (n = 23). The average age for this sample of adolescents was 16.91years (SD= 0.72) in experimental group and was 17.11 years (SD=0.83) in control group. All of them was male and study in senior high school. The mean body high of the experimental group was 173.63 cm (SD=4.66) and that of the control group was 173.50 cm (SD= 4.92). All the demographic profiles of the participants were no significant differences between experimental and control group on age, body high, body weight, BMI, percentage of body fat, visceral fat, waist circumference, and cardio-respiratory endurance test in baseline (Table 1).
Interaction Effects of Health-Related Outcomes Between Different Time Points and Different Groups: There were significant interaction effects between three time points and two different groups in the body fat score (Waldχ2 = 16.99, p < 0.01), visceral fat score (Waldχ2 = 216.60, p < 0.01), waist circumference (Waldχ2 = 969.72, p < 0.01), cardio-respiratory endurance (Waldχ2 = 492.79, p < 0.01). However, there were not significant in the body weight and BMI.
The Differences of Health-Related Outcomes Between the Two Groups at Each Posttest: Controlling for baseline measure, two-group differences in each posttest indicated that intervention and control groups had significant differences in body weight scores (T2 mean: IG = 81.50, CG = 83.07) and also in T3(IG = 79.90, CG = 81.51); body fat scores (T3mean: IG = 23.50, CG = 24.37) but it was not significant in T2. Visceral fat scores had significant differences after 4 weeks (T2 mean: IG = 11.15, CG =11.96) and 8 weeks (T3 mean: IG= 10.14, CG = 11.95) of the study. There also had significant differences in waist circumference scores after 4 weeks (T2 mean: IG = 91.45, CG =94.35) and 8 weeks (T3 mean: IG= 88.50, CG = 94.16); cardio respiratory endurance after4 weeks (T2 mean: IG = 9.30, CG =10.33) and 8 weeks (T3 mean: IG= 8.57, CG = 10.35) of the study. The body weight scores of participants in the intervention group were significantly lowered than those in the control group at T3 (Waldχ2 = 5.39, p<0.05); body fat scores at T3 (Waldχ2 = 7.44, p<0.05). Body fat scores of participants in the intervention group were also significantly lowered than those in the control group at T3 tests (Waldχ2 = 7.44, p < 0.05); visceral fat scores at T2 (Waldχ2 = 146.57, p < 0.01) and T3 tests (Waldχ2 = 195.87, p<0.01); waist circumference scores at T2(Waldχ2 =38.88, p<0.01) and T3 tests (Waldχ2 = 341.81, p<0.01); cardio respiratory endurance at T2(Waldχ2 = 419.21, p<0.01) and T3 tests (Waldχ2 = 528.65, p<0.01), respectively. There were not significant in BMI at T2 and T3 (p > 0.05).
The Difference Among Three Time Points Within Each Group: Results indicated that body weight scores among three time points were statistically significant in the intervention group (Waldχ2 = 253.72, p<0.01); BMI (Waldχ2 = 286.06, p<0.01); body fat (Waldχ2 = 30.25, p < 0.05); visceral fat (Waldχ2 = 313.64, p < 0.01); waist circumference (Waldχ2 = 2357.12, p<0.01); cardio respiratory endurance (Waldχ2 = 617.64, p<0.01). There also significant in the control group in body weight (Waldχ2 = 296.75, p<0.01); BMI (Waldχ2 = 209.57, p<0.01). The scores in the posttests were all smaller than the pre-test scores (Table 2). The results were found in the control group, the body fat mean scores decreased at T2 (24.35±1.60) but increased slightly at T3 (24.37±1.59). Similar in cardio-respiratory endurance, the mean scores decreased at T2 (10.33±1.18) but increased slightly at T3 (10.35±1.18). However, the control group participants showed no significant differences in body fat scores across three waves of time (Waldχ2 = 1.78, p > 0.05); visceral fat (Waldχ2 = 1.83, p > 0.05);waist circumference (Waldχ2 = 2.50, p > 0.05);cardio respiratory endurance (Waldχ2 = 1.21, p > 0.05) (Table 2).
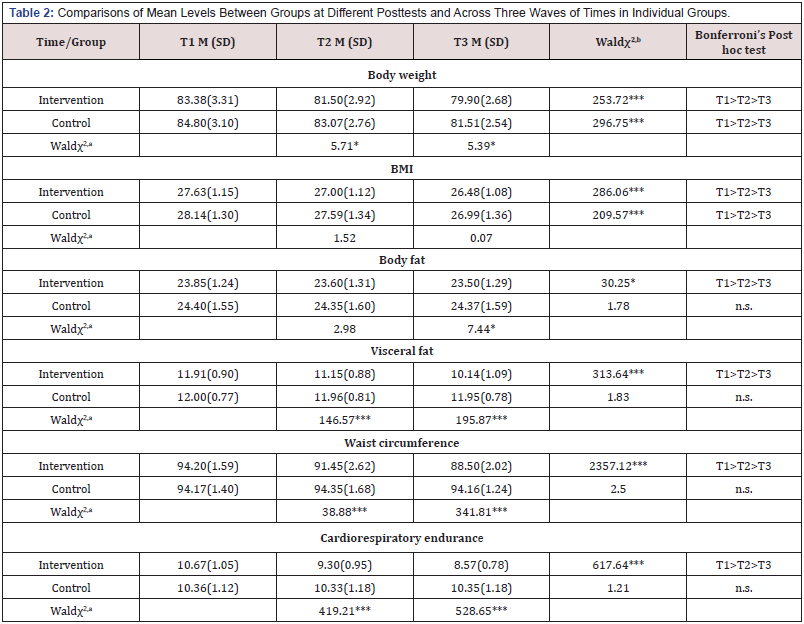
Table 2: Comparisons of Mean Levels Between Groups at Different Posttests and Across Three Waves of Times in Individual Groups.
T1: baseline test, T2: 4-week test, T3: 8-week test
*p < .05, **p <.01, ***p < .001; n.s.: non-significant (p > .05)
aGEE of the differences between the two group at each posttest (controlling for baseline)
bGEE of the difference among four time points within each group
Discussion
The results show that the program is an effective approach for improving health-related outcomes in adolescent males who are overweight and /or obese. Participants’ body fat, visceral fat, waist circumference, and cardio-respiratory endurance had significant improvements at Week 4 which were sustained throughout the 8-week study. This study provides evidence that a youth diabetes prevention program is feasible and can substantially improve diabetes and cardiovascular risk factors of greater BMI, body fat, visceral fat, waist circumference and poor cardio-respiratory endurance. The results are similar to previous literature indicating that diet modification with physical exercise incorporated into creative activities and group social interactions were important for adolescents to manage their weight [11,29,31,34]. The risk factor reductions have shown great value in reducing risks of obesity-related disease such as type 2 diabetes, metabolic complications and dyslipidemia. Changes in body fat, visceral fat, waist circumference, cardio-respiratory endurance in adolescents are predictors of changes in risk for obesity-related disease at adulthood [7,8 , 9, 10]. Specifically, changes in waist circumference lead to better body shape and body image.
Further, the weight reduction program consisted of aerobic plus resistance exercise, dietary modification and incorporating peer support discussion demonstrated great benefits in loosing weight. Weight reduction may be attributed by physical activity levels among aerobic plus resistance exercise and jogging lessons. Additionally, participants who were more physically competent at aerobic plus resistance exercise may have been more motivated to take part or have exerted more effort, which may have resulted in expending more energy and subsequent decreased waist circumference. Group cohesion in the aerobic plus resistance exercise intervention may also have supported and fostered overweight adolescents who rarely engage in traditional sports due to weight criticism [15]. Peer support groups promote social cohesion and have been known to be effective for weight reduction due to social reinforcement. Dietary modifications however are more associated with family support [19-40].
Traditional aerobic exercise has been reported to reduce body weight, visceral fat, waist circumference in some but not all studies [36-50]. The aerobic plus resistance program in this study was specifically designed to accommodate reduced body flexibility experienced by adolescents. Through the gradual progression of arranging static physical postures, and stretching to improve joint flexibility and muscular strength , participants reported decreased body weight, visceral fat and waist circumference [51-70].
Limitations: The intervention was designed for male adolescents, which could mean that different results would be found for female adolescents. Thus, the generalizability of the results is limited. The lack of correlations between attendance and weight reduction suggests that future investigation on the dose-effect of the intervention is needed.
Conclusions
This study revealed the effect of the youth diabetes prevention program on visceral fat, waist circumference, and the cardio-respiratory endurance. It is recommended that the program should take account for gender differences of adolescents’ needs.
Acknowledgements
The authors acknowledge the support by the School Principal at the participating school.
Conflict of Interest
None of the authors have any conflicts of interests with regards to this research.
Author Contributions
Concept develop and study design: SMC, WCL, HSL, C-JW; data collection and analysis: SMC, WCL, HSL; manuscript preparation: SMC, HSL C-JW; manuscript appraisal and editing: SMC, C-JW; All revisions: SMC, C-JW; Final approval: SMC, WCL, HSL, C-JW.
References
- (2016) World Health Organization. Obesity and Overweight, Fact sheet.
- (2018) World Health Organization. Obesity and Overweight, Fact sheet.
- Chang HC, Yang HC, Chang HY, Yeh CJ, Chen HH, et al. (2017) Morbid obesity in Taiwan: Prevalence, trends, associated social demographics, and lifestyle factors. PLoS One 12(2).
- Chen W, Chang MH (2010) New Growth Charts for Taiwanese children and adolescents based on World Health Organization standards and health-related physical fitness. Pediatr Neonatol 51(2): 69-79.
- Goldhaber-Fiebert JD, Rubinfeld RE, Bhattacharya J, Robinson TN, Wise PH (2013) The Utility of Childhood and Adolescent Obesity Assessment in Relation to Adult Health. Med Decis Making 33(2): 163-175.
- Muhammad F, Mustapha Kabir Musa, ABM Alauddin Chhowdhury, Moniruddin Chowdhury, SifatRokhsana Hasin (2016) Risk Factors of Childhood Obesity and Overweight in Young Children and Adolescents Aged Between 5 to 15 Years in Urban Bangladesh: A Scoping Review. Mal J Nutr 22(3): 455-459.
- Chen CM, Lou MF, Gau BS (2014) Prevalence of impaired fasting glucose and analysis of related factors in Taiwanese adolescents. Pediatric Diabetes 15(3): 220-228.
- Gungor KN (2014) Overweight and obesity in children and adolescents. J Clin Res Pediatr Endocrinol 6(3): 129-143.
- Yu JX, Tao Y, Tao Y, Yang S, Yu Y, et al. (2016) Optimal cut-off of obesity indices to predict cardiovascular disease risk factors and metabolic syndrome among adults in Northeast China. BMC Public Health 16(1): 1079.
- Gurnani M, Birken C, Hamilton J (2015) Childhood obesity: Causes, consequences, and management. Pediatr Clin North Am 62 (4): 821-840.
- Hisar F, Toruner E (2014) Adolescents’ perceptions about their weight and practices to lose weight. Australian Journal of Advanced Nursing 31(2): 23-30.
- Mühlig Y, Antel J, Focker M, Hebebrand J (2016) Are bidirectional associations of obesity and depression already apparent in childhood and adolescence as based on high-quality studies? A systematic review. Obesity Reviews 17(13): 235- 249.
- Cleobury L, Tapper K (2014) Reasons for eating ‘unhealthy’ snacks in overweight and obese males and females. J Hum Nutr Diet. 27(4): 333-341.
- Murphy LA, Blackstock SJ (2018) The influence of technology on obesity in children and adolescents’ threats to and opportunities for health in our digital world. Arch Dis Child 103(1): A1- A212.
- Lien SY, Lee JT, Wu MY, Jiang YD, Yen HR, et al. (2017) A Systematic Review and Meta-Analysis of the Effect of Lifestyle Modification on Metabolic Control in Overweight Children. Evid Based Complement Alternat Med 27 1-12.
- Kornet-van der Aa DA, Altenburg TM, van Randeraad-van der Zee CH, Chinapaw M M (2017) The effectiveness and promising strategies of obesity prevention and treatment programmes among adolescents from disadvantaged backgrounds: a systematic review. Obes Rev 18(5): 581- 593.
- Kennedy AK, Schneiderman JU, Ramseyer WV (2019) Association of body weight perception and unhealthy weight control behaviors in adolescence. Children & Youth Services Review 96: 250-254.
- Murray M, Pearson JL, Dordevic AL, Bonham MP (2019) The impact of multicomponent weight management interventions on quality of life in adolescents affected by overweight or obesity: a meta-analysis of randomized controlled trials. Obesity Reviews 20(2): 278- 289.
- Haidar M, Ranjit A, Saxton D, Hoelscher DM (2019) Perceived Parental and Peer Social Support Is Associated with Healthier Diets in Adolescents. J Nutr Educ Behav 51(1): 23-31.
- Salvy SJ, Miles JNV, Shih RA, Tucker JS, D'Amico EJ (2017) Neighbourhood, Family and Peer-Level Predictors of Obesity-Related Health Behaviors Among Young Adolescents. Journal of Pediatric Psychology 42(2): 153-161.
- Hou Y, Kim S Y, Wang Y, Shen Y, Orozco-Lapray D (2015) Longitudinal Reciprocal Relationships Between Discrimination and Ethnic Affect or Depressive Symptoms Among Chinese American Adolescents. J Youth Adolesc 44(11): 2110- 2121.
- Hsu YW, Liou TH, Liou YM, Chen HJ, Chien LY (2016) Measurements and profiles of body weight misperceptions among Taiwanese teenagers: a national survey. Asia Pac J ClinNutr 25(1): 108-117.
- Wu YK, Liu Y (2015) Weight-related stigmatization and binge eating among overweight adults in Southern Taiwan. Asia Pac J Clin Nutr 24(1): 118-127.
- Tiwana A (2003) Affinity to infinity in Peer-to-Peer knowledge platforms. Communications of the ACM 46(5): 77-80.
- Staiano AE, Abraham AA, Calvert SL (2013) Adolescent Exergame Play for weight loss and psychosocial improvement: A controlled physical activity intervention. Obesity 21(3): 598-601.
- Kulik NL, Fisher EB, Ward DS, Ennett ST, Bowling JM, et al. (2014) Peer Support Enhanced Social Support in Adolescent Females During Weight Loss. Am J Health Behav 38(5): 789-800.
- Cunha DB, Junior EV, Paravidino VB, Araujo MC, Mediano MF, et al. (2017) Design of a school randomized trial for nudging students towards healthy diet and physical activity to prevent obesity PAAPAS Nudge study protocol. Medicine 96(50): 50-55.
- Kolodziejczyk JK, Norman GJ, Rock CL, Arredondo EM, Madanat H (2014) Strategies that Predict Weight Loss among Overweight/Obese Young Adults. Am J Health Behav 38(6): 871-880.
- Goldfield GS, Adamo KB, Rutherford J, Murray M (2012) The Effects of Aerobic Exercise on Psychosocial Functioning of Adolescents Who Are Overweight or Obese. J Pediatr Psychol 37(10): 1136-1147.
- (2009) Ministry of Education, Taiwan, ROC. The Happy Program.
- Thivel D, Masurierm J, Baquet G, Timmons BW, Pereira B, et al. (2019) High-intensity interval training in overweight and obese children and adolescents: systematic review and meta-analysis. Journal of Sports Medicine & Physical Fitness 59(2): 310-324.
- Campos RM, De Mello MT, Silva PL, Masquio DC, De Piano A (2014) Aerobic plus resistance training improves bone metabolism and inflammation in adolescents who are obese. Journal Strength Condition Research 28(3): 758-766.
- García-Hermoso A, Ramírez-Vélez R, Ramírez-Campillo R, Peterson MD, Martínez-Vizcaíno V (2018) Concurrent aerobic plus resistance exercise versus aerobic exercise alone to improve health outcomes in pediatric obesity: a systematic review and meta-analysis. Br J Sports Med 52(3): 161-166.
- Douris PC, Mc Donald B, Vespi F, Kelley NC, Herman L (2012) Comparison between Nintendo WII FIT aerobics and traditional aerobic exercise in sedentary young adults. Journal of Strength and Conditioning Research 26(4): 1052-1057.
- Harrington DM, Staiano AE, Broyles ST, Gupta AK, Katzmarzyk PT (2013) BMI percentiles for the identification of abdominal obesity and metabolic risk in children and adolescents: evidence in support of the CDC 95th percentile. Eur J Clin Nutr 67(2): 218- 222.
- Andersen JR, Natvig GK, Aadland E, Moe VF, Kolotkin RL, et al. (2017) Associations between health-related quality of life, cardiorespiratory fitness, muscle strength, physical activity and waist circumference in 10-year-old children: the ASK study. Qual Life Res 26: 3421-3428.
- Baer TE, Scherer EA, Richmond TK, Fleegler EW, Areej Hassan A (2018) Food Insecurity, Weight Status, and Perceived Nutritional and Exercise Barriers in an Urban Youth Population. Clinical Pediatrics 57(2): 152-160.
- Bravender T, Lyna P, Coffman CJ, Bodner ME, Ostbye T et al. (2018) Physician Weight-Related Counseling Is Unrelated to Extreme Weight Loss Behaviors Among Overweight and Obese Adolescents. Clinical Pediatrics 57(8): 954-957.
- Brown BJ, Hermann JR, (2005) Cooking classes increase fruit and vegetable intake and food safety behaviors in youth and adults. Journal of Netrition Education & Behavior 37(2): 104-105.
- Centers for Disease Control. Health, United States.
- Chansukree P, Rungjindarat N (2017) Social Cognitive Determinants of Healthy Eating Behaviors in Late Adolescents: A Gender Perspective. Journal of Nutrition Education and Behavior 49(3): 204-210.
- Charlot K, Chapelot D (2013) Energy compensation after an aerobic exercise session in high-fat/low-fit and low-fat/high-fit young male subjects. British Journal of Nutrition 110: 1133-1142.
- Chen CM, Lou MF, Gau BS (2016) Parental Body Mass Index Is Associated with Adolescent Obesity in Taiwan. Research in Nursing & Health 39(6): 399-405.
- Chiang CL, Lin CL (2016) The effect of six weeks equal volume of alternative and continuous resistance combined aerobic training on muscle performance and hemodynamics. Chung Yuan Christian University Athletic Report 9: 109-119.
- Chou YC, Pei1 JS (2010) Risk factors of adolescent obesity in Taiwan and its association with physical activity, blood Pressure and waist circumference. Asian Journal of Sports Medicine 1(4): 214-222.
- De Miguel-Etayo P, Muro C, Santabarbara J, Lopez-Anton R, Morande G (2016) Behavioral predictors of attrition in adolescents participating in a multidisciplinary obesity treatment program: EVASYON study. International Journal of Obesity 40: 84-87.
- Denney-Wilson E, Hardy LL, Dobbins T, Okely AD, Louise A, et al. (2008) Body Mass Index, Waist Circumference, and Chronic Disease Risk Factors in Australian Adolescents. Arch Pediatr Adolesc Med 162(6): 566-573.
- Friedland RP, Fritsch T, Smyth KA, Koss E, Lerner AJ, et al. (2001) Patients with Alzheimer's disease have reduced activities in midlife compared with healthy control-group members. Proceedings of the National Acadermy of Sciences 98(6): 3440-3445.
- Gellar L, Druker S, Osganian SK, LaPelle GN, Pbert L, et al. (2012) Exploratory Research to Design a School Nurse-Delivered Intervention to Treat Adolescent Overweight and Obesity. J Nutr Educ Behav 44(1): 46-54.
- Harrington J, Perry IJ, Lutomski J, Fitzgerald AP, Shiely F, et al. (2010) Living longer and feeling better: healthy lifestyle, self-rated health, obesity and depression in Ireland. Eur J Public Health 20(1): 91-95.
- (2016) Health Promotion Administration, Ministry of Health and Welfare, Taiwan, R.O.C. Overweight and obesity prevalence of Taiwan.
- (2018) Health Promotion Administration, Ministry of Health and Welfare, Taiwan, R.O.C. Annual Report- Obesity Prevention.
- Huang YC, MALINA RM (2007) BMI and Health-Related Physical Fitness in Taiwanese Youth 9- 18 Years. Med Sci Sports Exerc 39(4): 701-708.
- Kraemer WJ, Volek JS, Clark KL, Gordon SE, Puhl SM, et al. (1999) Influence of exercise training on physiological and performance changes with weight loss in men. Med Sci Sports Exerc 31(9): 1320-1329.
- Lowry R, Lee SM, McKenna ML, Galuska DA, Kann LK (2008) Weight management and fruit and vegetable intake among US high school students. Journal of School Health 78(8): 417-424.
- Maffeis C (2000) Etiology of overweight and obesity in childrenand adolescents. European Journal of Pediatric 59(1): 35-44.
- Ozcelik O, Dogan H, Celik H, Ayar A, Serhatlioglu S, et al. (2005) Effects of different weight loss protocols on serum leptin levels in obese females. Physiologisy Reaserch 54(3): 271-277.
- Reichkendler MH, Rosenkilde M, Auerbach PL, Agerschou J, Nielsen MB, et al. (2014) Only Minor Additional Metabolic Health Benefits of High As Opposed to Moderate Dose Physical Exercise in Young. Moderately Overweight Men Obesity 22(5): 1220-1232
- Salvadori A, Fanari P, Marzullo P, Codecasa F, Tovaglieri I, et al. (2014) Short bouts of anaerobic exercise increase non-esterified fatty acids release in obesity. Eur J Nutr 53(1): 243-249.
- Santos AP, Marinho DA, Costa AM, Izquierdo M, Marques MC (2012) The effects of concurrent resistance and endurance training follow a detraining period in elementary school students. Journal of Strength & Conditioning Research 26(6): 1708-1716.
- Shih KC, Kwok CF (2018) Exercise reduces body fat and improves insulin sensitivity and pancreatic β-cell function in overweight and obese male Taiwanese adolescents. BMC Pediatrics 18(1): 80-88.
- Small L, McClain DB, Melnyk B, Vaughan L, Gannon AM (2014) The Preliminary Effects of a Primary Care- Based Randomized Treatment Trial With Overweight and Obese Young Children and Their Parents Journal of Pediatric Health Care 28(3): 198-207.
- Soltero EG, Olson ML, Williams AN, Konopken YP, Castro FG, et al. (2018) C Obesity. 26(12): 1856-1865.
- (2019) Sports Administration, Ministry of Education, Taiwan, R.O.C. Physical fitness test and the male standard for ages 6-18.
- Piercy KL, Troiano RP, Ballard RM, Carlson SA, Fulton JE, et al. (2018) Physical Activity Guidelines for Americans. JAMA 320(19): 2020-2028.
- Vangeepuram N, Townsend K, Arniella G, Goytia C, Horowitx CR (2016) Recruitment in clinical versus community-based sites for a pilot youth diabetes prevention program, New York, 2011-2012. Preventing Chronic Disease 13: 1-8.
- Vereecken CA, Inchley J, Subramanian SV, Hublet A, Maes L (2005) The relative influence of individual and contextual socio-economic status on consumption of fruit and soft drinks among adolescents in Europe. European Journal of Public Health 15(3): 224-232.
- Wang Y, Lobstein T (2006) Worldwide trends in childhood overweight and obesity. International journal of pediatric obesity 1(1): 11-25.
- Weiss EP, Albert SG, Reeds DN, Kress KS, Jennifer L McDaniel JL, et al. (2016) Effects of matched weight loss from calorie restriction, exercise, or both on cardiovascular disease risk factors: a randomized intervention trial. Am J Clin Nutr 104(3): 576-586.
- (2014) World Health Organization. Health Education and Promotion: Prevention and Control of childhood Obesity. WHA 66th Geneva, Switzerland.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.