Short Communication 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Prevention of Broncho Pulmonary Dysplasia: Accuracy of Surfactant Dosage for Preterm Infants at Birth Based on Their Average Weights
*Corresponding author: Naveen K Athiraman, Royal Victoria Infirmary, Newcastle upon Tyne, NE1 4LP, UK
Received: April 29, 2020;Published: May 15, 2020
DOI: 10.34297/AJBSR.2020.08.001329
Abstract
Introduction: Bronchopulmonary dysplasia (BPD) is defined as oxygen dependence at 36 weeks. Some pharmacological strategies used to decrease rates BPD include antenatal steroids, surfactant at birth and use of caffeine. In many neonatal units, surfactant is administered at birth in the delivery room in order to improve compliance of lungs and minimise lung injury as well as optimise ventilation. Knowledge on average weights at different gestational ages would be useful to deliver closer to accurate dose of surfactant, at birth.
Aim: To identify the average weights at all gestational ages from 22 weeks onwards and to calculate the average surfactant (curosurf) dose at every gestation.
Methodology: All newborn infants born and admitted to the regional neonatal unit were identified from Badgernet database, over a period of 10 years from January 2009 to November 2018. The data collection included gestational age (GA), birth weight and gender for all of the newborn infants admitted to the unit.
Results: A total of 7387 neonatal admissions were analysed during the 10-year period. The overall average weights at different gestational ages from 22 to 42 weeks were identified which was 505gms to 3728gms, respectively.
Conclusion: On attending delivery room for extreme premature infants, 120mg curosurf seems appropriate until 25 weeks GA, 240mg for preterm infants until 30 weeks GA, 360mg and 480mg for borderline premature infants until 34 weeks and 36 weeks GA respectively.
Keywords: Preterm infants, Bronchopulmonary dysplasia, Chronic lung disease of newborn, surfactant, Average weights, Accurate dose
Abbreviations: Bronchopulmonary dysplasia- BPD; Gestational age- GA
Introduction
Bronchopulmonary dysplasia (BPD), otherwise known as chronic lung disease of the newborn affects mostly preterm infants due to their premature lungsand prolonged need of respiratory support [1]. This group of infants have surfactant deficiency at birthresulting in surfactant deficient lung disease, and the severity varies with degree of prematurity and other associated factors such as infection, meconium aspiration and pulmonary haemorrhage can further decrease or inhibit surfactant production temporarily [2]. As a routine, neonatal unit practices are to deliver surfactant at birth to all intubated premature infants to ensure maximum benefits in improving lung compliance and oxygenation as well as prevent BPD [3]. In our unit, all premature infants who require intubation at birth for respiratory distress receives surfactant soon after intubation in the delivery room. The literature suggests a surfactant dose (in case of curosurf) of 200mg/kg at birth and follow-on dose of 100mg/kg, if still ventilated at around 12 hrs of age [4]. Currently, initial surfactant dose is an estimate based on the gestational age. Neonatal team takes a surfactant vial, either 120mg or 240mg, to the delivery room and the infant receives the full vial, which can result in either higher or lower the required dose. Curosurf is the commonly used exogenous surfactant in UK.
The aim of this study is to identify the average weights at all gestational ages from 22 weeks onwards and the average curosurf dose at every gestation.
Methods
All newborn infants born and admitted to the regional neonatal unit were identified from Badgernet database, over a period of 10 years from January 2009 to November 2018. The data collection included gestational age (GA), birth weight and gender for all of the newborn infants admitted to the unit. The data was collected on an excel sheet and weights were calculated as an average for individual gestational ages. The same analysis was then used with male and female gender to identify the difference in average weights for gestational ages.
Results
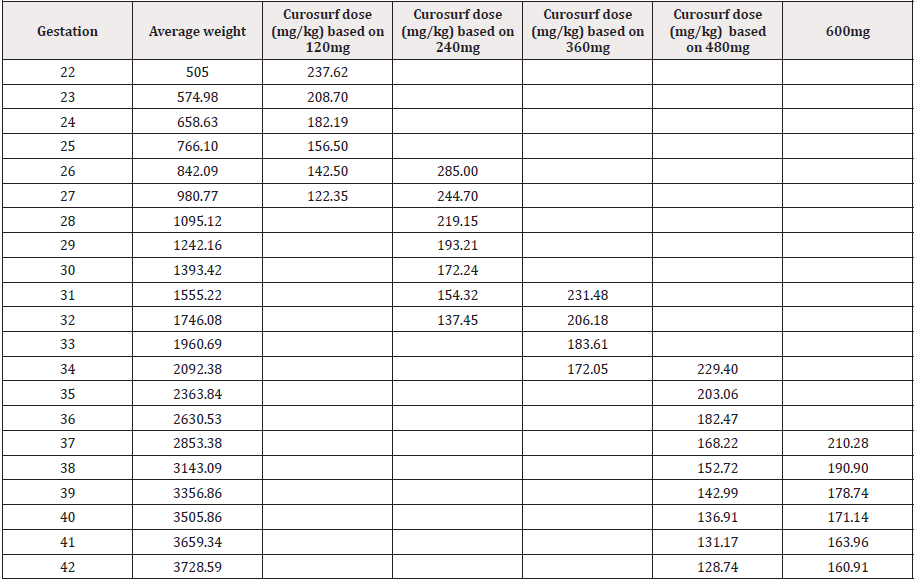
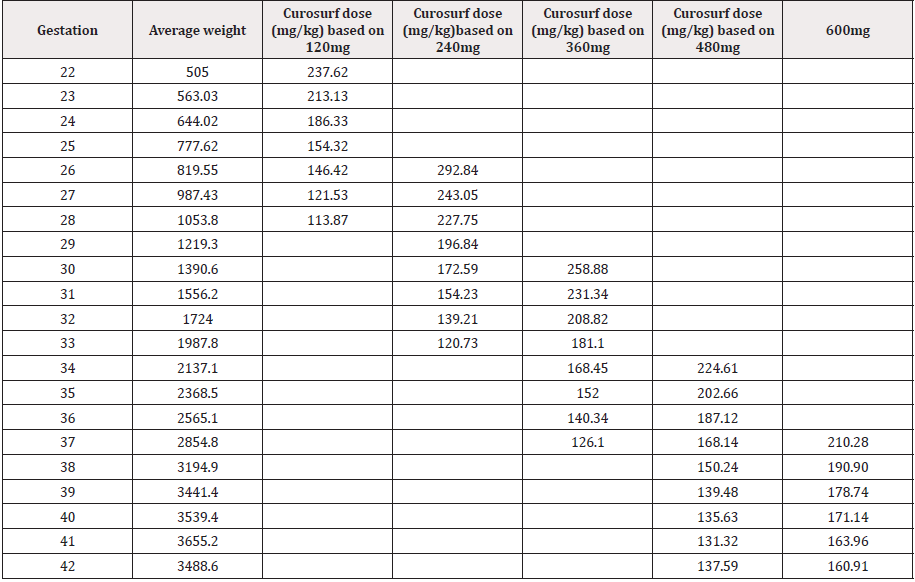
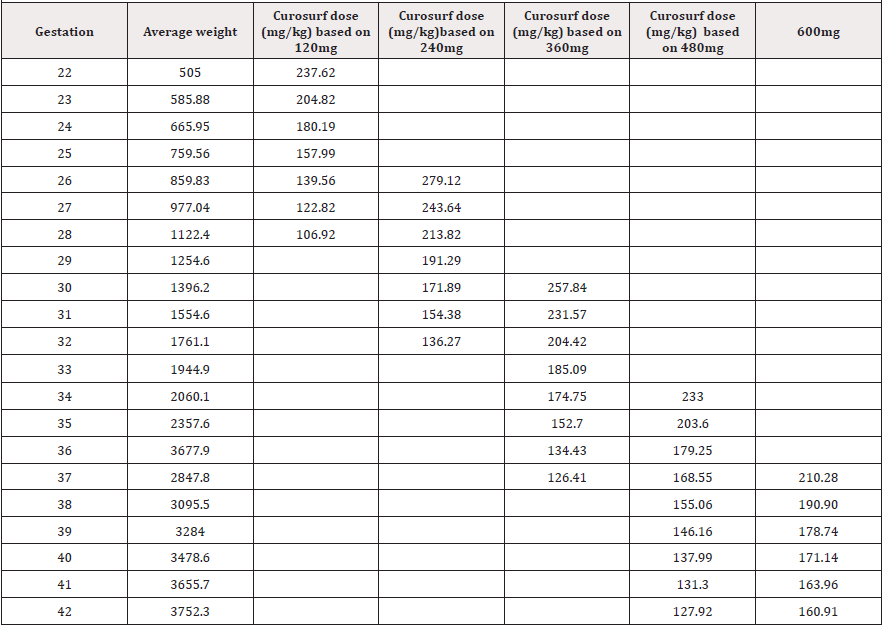
A total of 7387 neonatal admissions were analysed during the 10-year period, 3221were females and 4159 males, 5 indeterminate and 2 unknown. The overall average weights at different gestational ages from 22 to 42 weeks are shown in Table 1 and average weights for female and male gender at various gestational ages are shown in Table 2 and 3 respectively.
Average surfactant dosage at 22 weeks gestational age is 238mg/kg, when 120mg vial is used. At 26 weeks GA 240 mg vial is required to give a 285mg/kg dose, 31 weeks GA required 360mg vial to give 231mg/kg, 35 weeks GA required 480mg to give 203mg/ kg and 37 weeks GA required 600mg to give 210mg/kg (Table 1).
In females, average surfactant dosage at 22 weeks GA is 238mg/ kg, when 120mg vial is used. At 27 weeks GA 240mg vial is required to give a 243mg/kg dose, 32 weeks GA required 360mg vial to give 208mg/kg and 35 weeks GA required 480mg to give 202mg/kg (Table 2).
In males, average surfactant dosage at 22 weeks GA is 238mg/ kg, when 120mg vial is used. At 26 weeks GA 260mg vial is required to give a 279mg/kg dose, 32 weeks GA required 360mg vial to give 204mg/kg and at 35 weeks GA required 480mg to give 203mg/kg (Table 3).
Discussion
A 120mg surfactant vial gives around 237mg/kg to 156mg/ kg for 22 weeks to 25 weeks GA respectively. At 26 weeks, 240mg surfactant vial would provide 285mg/kg and would be appropriate to use until 30 weeks GA. From 31 weeks GA infants will require 360mg vial to provide 231mg/kg until 34 weeks providing 172mg/ kg. A 480mg vial will be appropriate for 35 and 36 weeks gestation giving 203mg/kg and 180mg/kg. In infants born 37 weeks and above would benefit from 600mg vials to provide surfactant dose of 210mg/kg until 42 weeks. This dosage is based on the aim to deliver 200mg/kg or closer to this dose.
Many neonatal units aim to deliver surfactant at birth to provide adequate respiratory support from birth. Premature infants are surfactant deficient and giving surfactant improves compliance and minimises the respiratory support. However, the surfactant dose is an estimate as the infant is mostly not weighed in the delivery room or theatre.
Currently, there is minimal literature available on the weights of premature infants based on gestational age and gender. Here, we looked at admissions over a 10-year period to the tertiary neonatal unit in north east of England. This information will guide the neonatal teams to estimate the surfactant dose for different gestational ages and take the right vial to the delivery room or delivery theatre, specifically when attending a preterm delivery. This information will also help managing a sick term infant such as meconium aspiration syndrome where there may be a need for surfactant delivery at birth.
Conclusion
On attending delivery room for extreme premature infants, 120mg curosurf seems appropriate until 25 weeks GA, 240mg for preterm infants until 30 weeks GA, 360mg and 480mg for borderline premature infants until 34 weeks and 36 weeks GA respectively. Term infants requiring curosurf, a 600mg vial would be an appropriate dose. There is not a large difference in dosage between male and female gender.
Acknowledgment
Neonatal team for their support and hard work.
Conflict of interest
None
References
- Kinsella JP, Greenough A, Abman SH (2006) Bronchopulmonary dysplasia. Lancet 29367(9520): 1421-1431.
- Nkadi PO, Merritt TA, Pillers DM (2009) An overview of Pulmonary Surfactant in the neonate: Genetics, metabolism, and the role of surfactant in Health and disease. Mol Genet Metab 97(2): 95-101.
- Schmidt B, Roberts R, Davis P, Doyle L, Barrington K, et al. (2006) Caffeine Therapy for Apnea of Prematurity. N Engl J Med 354: 2112-2121.
- Cogo PE, Facco M, Simonato M, Verlato G, Rondina C, et al. (2009) Dosing of Porcine Surfactant Effect on Kinetics and Gas-Exchange in Respiratory Distress Syndrome. Pediatrics 124(5): e950-e957.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.