Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
The Role of Personal Protective Equipment (PPE) in Prevention of COVID-19 Novel Corona Virus and Fatalities occur due to Non-availability of the PPE
*Corresponding author: Ahsan Ali Siddiqui, Consultant Preventive Medicine and Epidemiologist, Quality Management and Patient Safety Department, Ministry of Health, Riyadh, Saudi Arabia
Received: July 06, 2020; Published: August 14, 2020
DOI: 10.34297/AJBSR.2020.09.001458
Abstract
Background and Objective: The Main Aim of the Article is to highlight the Importance of the Personal protective equipment (PPE) in prevention of COVID-19 novel corona virus. During current Pandemic of COVID-19 we found out that most of the Developed and Civilized countries lack basic availability of Personal protective equipment (PPE) for their Health care workers and Public.
Methods: The Author of this article has randomly selected 15 Articles from PUBMED and other sources on Internet with the word using “Personal protective equipment (PPE) in prevention of COVID-19”. The Author relies on Conceptual Literature Review for the Methodology of this article. Where the groups of Articles are reviewed and analyzed to find out the answer of the Question “The role of Personal protective equipment (PPE) in prevention of COVID-19”. The Table 4 is created to Analyze the 15 randomly selected Articles and the results has been presented By SPSS software diagrammatic presentation.
Results: Author of this article have presented the results by using diagrams from SPSS19 software. After studying and carefully critically reviewing the 20 Articles and other sources and randomly selecting 15 Articles for current PPE study. The Author has found out that all the 15 randomly selected articles favors the role of Personal protective equipment (PPE) in prevention of COVID-19 novel corona virus. 10 Articles has 100% agreed with the positive role of Personal protective equipment (PPE) in prevention of COVID-19 whereas 5 Articles did not.
Conclusion: COVID-19 Pandemic has taught the Global community A big lesson after losing Approximately 370,000 innocent lives and approximately Half Million people being sick of COVID-19. The lesson is that in this high-tech 21st century where countries claim to be super Developed and Civilized countries don’t have enough PPE for their health care workers and for local people. Not to take the name of the countries and governments they have ignored the Warnings of WHO in December 2019 and continue blaming the WHO for COVID-19 Pandemic. The Governments has not done their Homework to fight the Battle against COVID-19 Pandemic and people are still losing the lives due to lack of PPE’S, Not development of VACCINE, No confirmed TREATMENT available for COVID-19.
Keywords: Masks, Pandemic, Respirators, Aerosols, COVID-19, Corona, Helmet, Masks, Personal protective equipment, Protection, Suits, Surgeon, controlled air-purifying respirator, elastomeric respirator, high risk, personal protective equipment, powered air-purifying respirator,3D printing, Face shields, PPE, Safety, Sterilization.
Introduction
Airborne transmission may [21] occur if patient respiratory activity or medical procedures generate respiratory aerosols. These aerosols contain particles that may travel much longer distances and remain airborne longer but their infective potential is uncertain. Contact droplet and airborne transmission are each relevant during airway maneuvers in infected patients particularly during tracheal intubation. Personal protective equipment is an important component but only one part of a system protecting staff and other patients from corona virus disease 2019 cross-infection. Appropriate use significantly reduces risk of viral transmission. Personal protective equipment should logically be matched to the potential mode of viral transmission occurring during patient care [21] contact droplet or airborne.
Keeping healthcare [22] providers safe healthy and available to work throughout this pandemic is critical. The consistent use of appropriate personal protective equipment-PPE will help assure its availability and healthcare provider safety. The purpose of this communique is to give both anesthesiologists and other front-line healthcare providers a framework from which to understand the principles and practices surrounding PPE decision-making. We propose three types of PPE including: 1) PPE for droplet and contact precautions 2) PPE for general airborne droplet and contact precautions and 3) PPE for those performing or [22] assisting with high-risk aerosol-generating medical procedures.
[Figure 1 & 2]
[Figure 3 & 4]
PPE such as eye protection, Isolation gowns, Gloves, face masks, N95 Respirators, Powered air purifying respirators and Ventilators shortages are currently posing a tremendous challenge to the U.S. healthcare system because of the COVID-19 pandemic. Healthcare facilities are having difficulty accessing the needed PPE and are having to identify alternate ways to provide patient care. Surge capacity refers to the ability to manage a sudden unexpected increase in patient volume that would otherwise severely challenge or exceed the present capacity of a facility.
The corona virus disease-COVID-19 [23] pandemic caused by the severe acute respiratory syndrome SARS-CoV-2 virus is challenging healthcare providers across the world. Current best practices for personal protective equipment-PPE during this time are rapidly evolving and fluid due to the novel and acute nature of the pandemic and the dearth of high-level evidence. Routine infection control practices augmented by airborne precautions are paramount when treating the COVID-19positive patient. Best practices for PPE use in patients who have unknown COVID-19 status are a highly charged and emotional issue. The variables to be considered include protection of patients and healthcare providers accuracy and [23] availability of testing and responsible use of PPE resources.
Surgeons need guidance [24] regarding appropriate personal protective equipment-PPE during the COVID-19 pandemic based on scientific evidence rather than availability. A systematic review was undertaken in accordance with the PRISMA guidelines using the MEDLINE, EMBASE, & WHO COVID-19 Databases. Recommendations made by the WHO regarding the use of PPE in the COVID-19 pandemic have evolved alongside emerging evidence. Medical resources including PPE have been rapidly overwhelmed. There is a global effort to overcome this by combining the most effective use of existing PPE in combination with innovative strategies to produce more. Although there is a need to balance limited supplies with staff and patient safety [24] this should not leave surgeons treating patients with inadequate PPE.
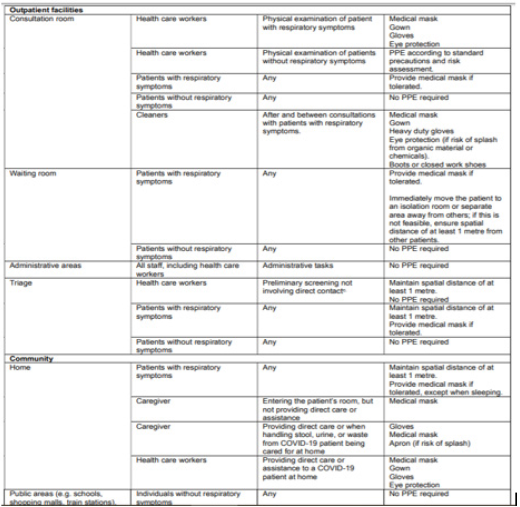
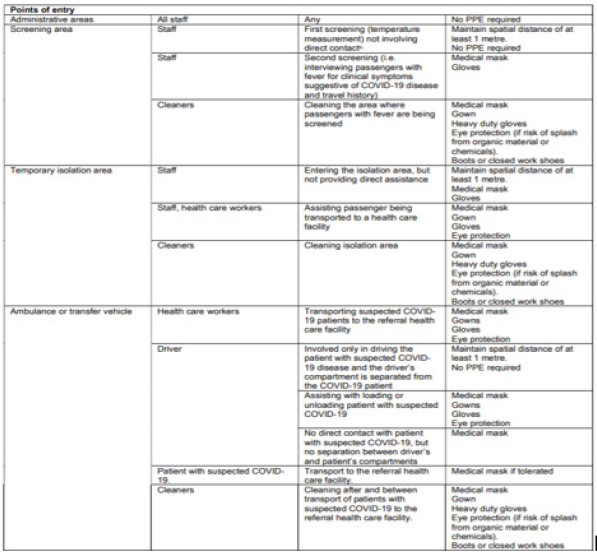
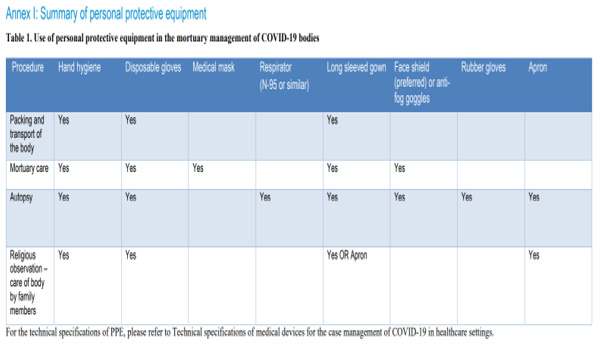
[Table 1,2 & 3]
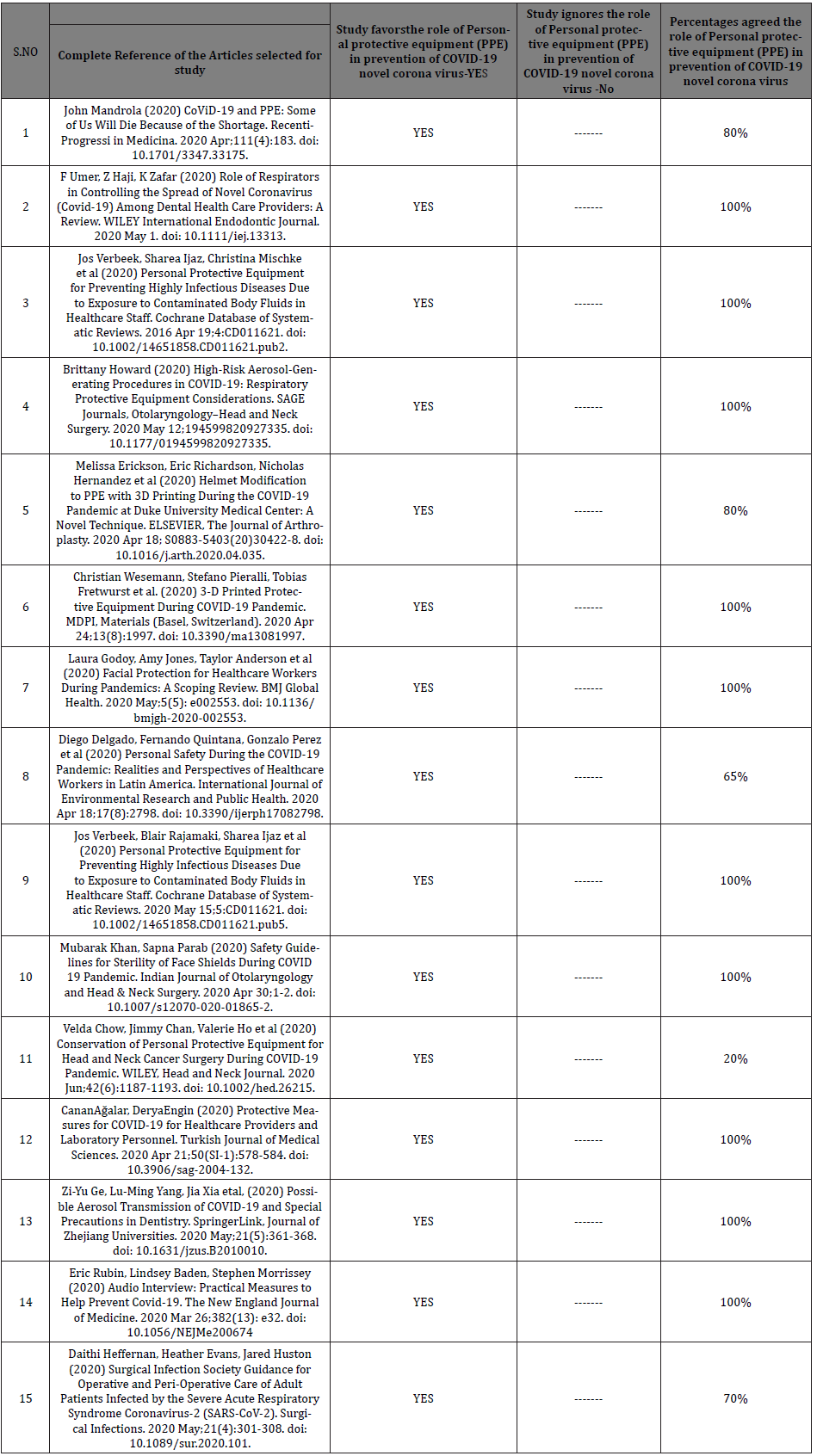
Table 4: 15Randomly selected Articles to show the role of Personal protective equipment (PPE) in prevention of COVID-19 novel corona virus and Fatalities occur due to non-availability of the PPE.
Tragically many [25] of the infections and deaths recorded in the global coronavirus disease 2019-COVID-19 pandemic have occurred in healthcare workers. Some have attributed this to inadequate provision of personal protective equipment-PPE. In the UK several organizations have voiced their concerns that the national PPE guidance issued by Public Health England is inadequate. Despite recent revisions to these guidelines concerns remain that they offer insufficient [25] protection to frontline NHS healthcare workers.
Of concern are the risks to [26] (B McGrath, N Ashby, M Birchall et al, 2020) healthcare staff of infection arising from tracheostomy insertion and subsequent management. Hospitals are also facing extraordinary demands on critical care services such that many patients who require a tracheostomy will be managed outside established intensive care or head and neck units cared for by staff with little tracheostomy experience. These concerns led NHS England and NHS Improvement to expedite the National Patient Safety Improvement Program’s Safe Tracheostomy Care work stream as part of the NHS COVID-19 response. Topics with direct relevance for frontline staff were identified. The consensus guidance includes infectivity of patients with respect to tracheostomy indications and timing aerosol-generating procedures and risks to staff insertion [26] (B McGrath, N Ashby, M Birchall et al, 2020) procedures and management following tracheostomy.
The use of medical masks [27] and respirators as personal protective equipment is pivotal to reducing the level of biological hazard to which healthcare workers are exposed during the outbreak of highly diffusible pathogens such as the recent novel corona virus SARS-CoV-2. Unfortunately, during these pandemic supplies are rapidly running out worldwide with potential consequences for the rate of occupational infections. A better understanding of SARS-CoV-2 transmission is needed together with high-quality clinical data on the use of respirators or alternative devices. Moreover, healthcare workers regardless of their level of experience should receive specific training. This review aims to summarize the available evidence on the use of medical masks and respirators in the context of viral infections [27] especially the current corona virus disease 2019-COVID-19.
Methods
The Author of this article has randomly selected 15 Articles from PUBMED and other sources on Internet with the word using “Personal protective equipment (PPE) in prevention of COVID-19”. The Author relies on Conceptual Literature Review for the Methodology of this article. Where the groups of Articles are reviewed and analyzed to find out the answer of the Question “The role of Personal protective equipment (PPE) in prevention of COVID-19”. The [Table 4] is created to Analyze the 15 randomly selected Articles and the results has been presented By SPSS software diagrammatic presentation.
Low certainty evidence [28] suggests that medical masks and N95 respirators offer similar protection against viral respiratory infection including corona virus in healthcare workers during non-aerosol-generating care. Preservation of N95 respirators for high-risk aerosol-generating procedures in this pandemic should be considered when in short supply. Four RCTs were meta-analyzed adjusting for clustering. Compared with N95 respirators the use of medical masks did not increase laboratory confirmed viral including corona viruses respiratory infection OR 1.06; 95% CI 0.90-1.25; I2 = 0% low certainty in the evidence or clinical respiratory illness OR 1.49; 95% CI: 0.98-2.28; I2 = 78% very low certainty in the evidence. Only one trial evaluated corona viruses separately and found no difference between [28] the two groups P = .49. [Table 4] [Figure 4].
Results
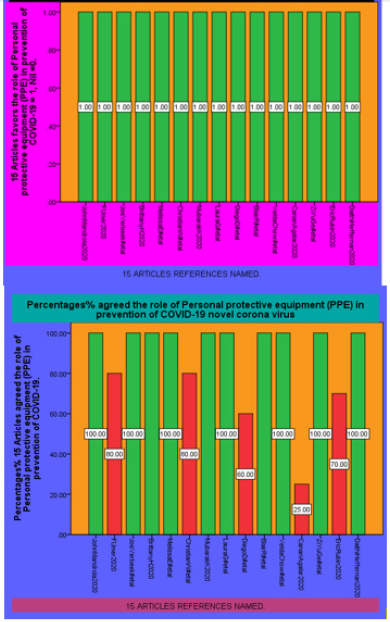
Author of this article have presented the results by using diagrams from SPSS19 software. After studying and carefully critically reviewing the 20 Articles and other sources and randomly selecting 15 Articles for current PPE study. The Author has found out that all the 15 randomly selected articles favors the role of Personal protective equipment (PPE) in prevention of COVID-19 novel corona virus. 10 Articles has 100% agreed with the positive role of Personal protective equipment (PPE) in prevention of COVID-19 whereas 5 Articles did not.
Rational use and successful reuse [29] of respirators can help in the shortage of PPE during a pandemic. Further studies testing UVGI and other decontamination techniques are an unmet need. The definitive answer to pandemic issues can be found in artificial intelligence and deep learning. Most studies on previous respiratory virus epidemics to date suggest surgical masks are not inferior compared with N95 respirators in terms of protective efficacy among healthcare workers. Therefore, the use of N95 respirators should be limited to high-risk situations. Concerning respirator reuse highly energetic short-wave ultraviolet germicidal irradiation (UVGI) at 254 nm was determined to decontaminate N95 respirators from viral respiratory agents but UVGI [29] requires careful consideration of the type of respirator and of the biologic target.
There is a critical shortage [30] of personal protective equipment-PPE around the globe. This article describes the safe collection storage and decontamination of N95 respirators using hydrogen peroxide vapor-HPV. This article is unique because it describes the HPV process in an operating room and is therefore a deployable method for many healthcare settings. Results presented [30] here offer creative solutions to the current PPE shortage.
Discussion
During global health [31] emergencies such as the current COVID-19 pandemic the decontamination of single-use personal protective equipment-PPE becomes a necessary means to keep up with the growing demand from healthcare workers and patients alike. Many unverified methods are being considered which can pose the risk of incomplete decontamination and lead to catastrophic results. Several factors come into play when determining the suitability of such methods including the quality of the decontamination technique the targeted pathogen cost ease of installation and use rate of sterilization and the surface or material to be sterilized. The germicidal properties of ultraviolet-C are well known. This review will cover the most commonly described methods for the sterilization of N95 respirators namely ultraviolet germicidal irradiation hydrogen peroxide [31] vaporization microwave-generated steaming and dry heating.
It has been shown that the [32] face rather than hands was the more frequent site of skin damage in Chinese health care workers managing COVID-19 related to pressure from face masks and goggles. Health care workers may be tempted to touch their face after removal of personal protective equipment. Given the respiratory route of transmission refraining from touching the face during facial personal protective equipment application and removal is another recommendation that should be impressed upon health [32] care workers just as strongly as preventing hand dermatitis.
Small droplets < 5 μm are [33] thought to remain suspended in the air and could theoretically be inhaled into the lungs causing infection. Loose fitting surgical masks will not prevent such inhalation and only a tight‐fitting filtering mask is adequate. Conversely larger > 5 μm particles do not remain suspended in the air 2 and can only cause infection if they are immediately inhaled. Nicas et al. is cited as evidence that 99.9% of the fluid volume ejected during a cough is in large particles. Typically, the faster the airflow the more aerosols are generated. Although we agree there is some evidence supporting tracheal intubation as an AGP in our experience very few airway procedures generate rapid airflows unless they cause coughing (e.g. at tracheal extubation). Many of the procedures which were defined as aerosol generating may in fact be a risk precisely because they generate coughing. Bronchoscopy [33] and physiotherapy would likely fit this description.
Face shields [34] are generally not used alone but in conjunction with other protective equipment like cap mask, goggle, and are therefore classified as adjunctive personal protective equipment. In the wake of scarcity of face shields during the COVID 19 Pandemic consideration of innovating newer methods of manufacturing must be considered to overcome the present-day scarcity without jeopardizing the safety of front-line Heath care workers. All initial fast innovations come with advantages and disadvantages hence we thought of putting down simple [34] guidelines for new emerged face shield use.
Public health measures to [35] achieve these goals may include quarantine which involves the restriction of movement or separation from the rest of the population of healthy persons who may have been exposed to the virus with the objective of monitoring their symptoms and ensuring early detection of cases. Many countries have the legal authority to impose quarantine. Quarantine should be implemented only as part of a comprehensive package of public health response and containment measures and in accordance with Article 3 of the International Health Regulations 2005 be fully respectful of the dignity human rights and fundamental freedoms [35] of persons.
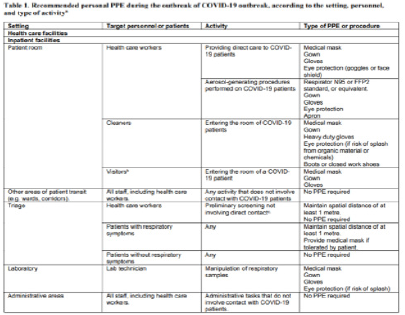
Personal protective equipment’s [36] and especially masks were among the hottest topics during this pandemic. Regardless of which mask is used performing hand hygiene frequently with an alcohol-based hand rub or with soap and water if hands are dirty is the most effective preventive measure for COVID-19. The type of mask used when caring for COVID-19 patients will vary according to the setting type of personnel/person and activity. Although the main transmission route for COVID-19 is droplets during aerosol generating procedures airborne transmission may occur. Keeping the distancing and medical masks and eye protection during close contact efficiently protects against respiratory diseases transmitted via droplets. Airborne precautions include goggles and respiratory protection with the use of an N95 or an equivalent mask respirator [36] to prevent airborne transmission.
Conclusion
COVID-19 Pandemic has taught the Global community A big lesson after losing Approximately 370,000 innocent lives and approximately Half Million people being sick of COVID-19. The lesson is that in this high-tech 21st century where countries claim to be super Developed and Civilized countries don’t have enough PPE for their health care workers and for local people. Not to take the name of the countries and governments they have ignored the Warnings of WHO in December 2019 and continue blaming the WHO for COVID-19 Pandemic. The Governments has not done their Homework to fight the Battle against COVID-19 Pandemic and people are still losing the lives due to lack of PPE’S, Not development of VACCINE, No confirmed TREATMENT available for COVID-19.
References
- John Mandrola (2020) CoViD-19 and PPE: Some of Us Will Die Because of the Shortage. Recenti Prog Med 111(4): 183.
- Health and Safety Executive (2020) Fit testing face masks to avoid transmission during the corona virus outbreak.
- Google (2020) Personal Protective Equipment Images.
- WHO (2020) Medical devices, Personal protective equipment?
- WHO Rationale use PPE (2020) Rational use of personal protective equipment (PPE) for coronavirus disease (COVID-19).
- F Umer, Z Haji, K Zafar (2020) Role of Respirators in Controlling the Spread of Novel Coronavirus (Covid-19) Among Dental Health Care Providers: A Review. Int Endod J 53(8): 1062-1067.
- Jos Verbeek, Sharea Ijaz, Christina Mischke, Riitta Sauni, Elaine Toomey, et al. (2020) Personal Protective Equipment for Preventing Highly Infectious Diseases Due to Exposure to Contaminated Body Fluids in Healthcare Staff. Cochrane Database Syst Rev 4(4): CD011621.
- Brittany Howard (2020) High-Risk Aerosol-Generating Procedures in COVID-19: Respiratory Protective Equipment Considerations. Otolaryngol Head and Neck Surg 163(1): 98-103.
- Melissa Erickson, Eric Richardson, Nicholas Hernandez, Dana W Bobbert, Ken Gall, et al. (2020) Helmet Modification to PPE with 3D Printing During the COVID-19 Pandemic at Duke University Medical Center: A Novel Technique. J Arthroplasty 35(7S): S23-S27.
- Christian Wesemann, Stefano Pieralli, Tobias Fretwurst, Julian Nold, Katja Nelson, et al. (2020) 3-D Printed Protective Equipment During COVID-19 Pandemic. Materials (Basel) 13(8): 1997.
- Laura Godoy, Amy Jones, Taylor Anderson, Cameron L Fisher, Kylie ML Seeley, et al. (2020) Facial Protection for Healthcare Workers During Pandemics: A Scoping Review. BMJ Glob Health 5(5): e002553.
- Diego Delgado, Fernando Quintana, Gonzalo Perez, et al (2020) Personal Safety During the COVID-19 Pandemic: Realities and Perspectives of Healthcare Workers in Latin America. Int J Environ Res Public Health 17(8): 2798.
- Jos Verbeek, Blair Rajamaki, Sharea Ijaz, Riitta Sauni, Elaine Toomey, et al. (2020) Personal Protective Equipment for Preventing Highly Infectious Diseases Due to Exposure to Contaminated Body Fluids in Healthcare Staff. Cochrane Database Syst Rev 4(4): CD011621.
- Velda Chow, Jimmy Chan, Valerie Ho, George chung ching Lee, Medoly Man, et al. (2020) Conservation of Personal Protective Equipment for Head and Neck Cancer Surgery During COVID-19 Pandemic. Head and Neck Journal 42(6): 1187-1193.
- WHO Infection Prevention (2020) Infection Prevention and Control for the safe management of a dead body in the context of COVID-19.
- Canan Ağalar, Derya Engin (2020) Protective Measures for COVID-19 for Healthcare Providers and Laboratory Personnel. Turk J Med Sci 50(SI-1): 578-584.
- Zi-Yu Ge, Lu-Ming Yang, Jia Xia, Xiao Hui Fu, Yan Zhen Zhang, et al. (2020) Possible Aerosol Transmission of COVID-19 and Special Precautions in Dentistry. J Zhejiang Univ Sci B 21(5): 361-368.
- Eric Rubin, Lindsey Baden, Stephen Morrissey (2020) Audio Interview: Practical Measures to Help Prevent Covid-19. N Engl J Med 382(13): e32.
- Daithi Heffernan, Heather Evans, Jared Huston, Jeffrey A Claridge, David Blake, et al. (2020) Surgical Infection Society Guidance for Operative and Peri-Operative Care of Adult Patients Infected by the Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2). Sur Infect 21(4): 301-308.
- IBM (2006) IBM SPSS Software USA.
- T M Cook (2020) Personal Protective Equipment During the Coronavirus Disease (COVID) 2019 Pandemic - A Narrative Review. Anesthesia 75(7): 920-927.
- Shannon Lockhart, Laura Duggan, Randy Wax, Stephan Saad, Hilary P Grocott (2020) Personal Protective Equipment (PPE) for Both Anesthesiologists and Other Airway Managers: Principles and Practice during the COVID-19 Pandemic. Can J Anesth 67(8): 1005-1015.
- Yale Fillingham, Matthew Grosso, Adolph Yates, Matthew S Austin (2020) Personal Protective Equipment: Current Best Practices for Orthopedic Teams. J Arthroplasty 37(7s): S19-S22.
- Zita Jessop, Thomas Dobbs, Stephen Ali, Emman Combellack, Rachel Clancy, et al. (2020) Personal Protective Equipment (PPE) for Surgeons During COVID-19 Pandemic: A Systematic Review of Availability, Usage, and Rationing. Br J Surg.
- John Thomas, Anand Srinivasan, Chandu Wickramarachchi, Parveen K Dhesi, Yat Ma Hung, et al. (2020) Evaluating the National PPE Guidance for NHS Healthcare Workers during the COVID-19 Pandemic. Clin Med (Lond) 20(3): 242-247.
- Mariachiara Ippolito, Filippo Vitale, Giuseppe Accurso, Pasquale Lozzo, Cesare Gregoretti, et al. (2020) Medical Masks and Respirators for the Protection of Healthcare Workers From SARS-CoV-2 and Other Viruses. Science Direct Pulmonology 26(4): 204-212.
- Jessica Bartoszko, Mohammed Farooqi, Waleed Alhazzani, Mark Loeb (2020) Medical Masks vs N95 Respirators for Preventing COVID-19 in Healthcare Workers: A Systematic Review and Meta-Analysis of Randomized Trials. Influenza other Respire Viruses 14(4): 365-373.
- Ivo Boškoski, Camilla Gallo, Michael B Wallace, Gudio Costamagna (2020) COVID-19 Pandemic and Personal Protective Equipment Shortage: Protective Efficacy Comparing Masks and Scientific Methods for Respirator Reuse. Gastrointest Endosc S0016-5107(20): 34247-34254.
- Douglas Perkins, Steven Villescas, Terry Wu, Timothy Muller, Steven Bradfute, et al. (2020) COVID-19 Global Pandemic Planning: Decontamination and Reuse Processes for N95 Respirators. Exp Biol Med (Maywood) 245(11): 933-939.
- Angeli Torres, Alexis Lyons, Shanthi Narla, Indermeet Kohli, Angela Parks Miller, et al. (2020) Ultraviolet-C and Other Methods of Decontamination of Filtering Facepiece N-95 Respirators During the COVID-19 Pandemic. Photochemical & Photobiological Science (6): 746-751.
- Mohit Gupta, Shari Lipner (2020) Personal Protective Equipment Recommendations Based on COVID-19 Route of Transmission. J Am Acad Dermatol 83(1): e45-e46.
- J Brown, C Pope (2020) Personal Protective Equipment and Possible Routes of Airborne Spread during the COVID-19 Pandemic. Anesthesia 75(8): 1116-1117.
- Mubarak Khan, Sapna Parab (2020) Safety Guidelines for Sterility of Face Shields During COVID 19 Pandemic. Indian J Otolaryngol Head Neck Surg 1-2.
- WHO Considerations for quarantine (2020) Considerations for quarantine of individuals in the context of containment for corona virus disease (COVID-19).
- Alpay Azap, Fatma Erdinç, (2020) Medical Mask or N95 Respirator: When and How to Use? Turk J Med Sci 50(SI-1): 633-637.






 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.