Research Article 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Syndrome of the lodges in the wake viperine enemasures in intensive care Chu of Bouake. Ivory coast
*Corresponding author: Koffi N’guessan R, Head of Infrastuture department, Université Alassane Ouattara de Bouaké, Côte d’Ivoire.
Received: June 27, 2019; Published: July 05, 2019
DOI: 10.34297/AJBSR.2019.03.000711
Summary
Viperine envenomation’s are serious because of the local complications they cause.
Objective: To describe the clinical and evolutionary aspects of patients with post-envenomation syndrome.
Patients and Method: Retrospective and descriptive study of cases of viperine envenomation syndrome treated in intensive care unit at the CHU of Bouaké during the period from January 1, 2012 to March 31, 2016. We identified 126 cases of envenomation including 37 viperine envenomations and noted 06 cases of compartment syndrome. The average admission time was 11.50 hours with extremes of 02 and 48 hours. There were 04 men for 02 women. Farmers were the most affected including five and a shepherd. The bite was located at the feet and ankles at 04 patients and at the hands at 02 patients. Painful tension was observed in the muscular compartments with extensive locoregional edema, and disappearance of peripheral pulses necessitated a discharge fasciotomy. Antivenom serotherapy was systematically performed with the FAV Afrique at a dose of 02 doses on average associated with amoxicillin-clavulanic acid antibiotics and multimodal analgesia (paracetamol, tramadol and / or morphine). The average duration of hospitalization was 13 days with extremes of 10 and 19 days. The evolution was favourable in all the patients without amputations with sequelae of tendinous retractions.
Conclusion: The logde syndrome post viperine envenomation is observed more and more in our context. Effective management requires surgical and antivenom treatment.
Keywords: Envenomation; Antivenom; Compartment syndromes
Introduction
Envenomations in sub-Saharan Africa are frequent and are responsible for more than 20,000 deaths per year. Viperine envenomation is the most common in the savannah zone and is the cause of clinical manifestations commonly associating an inflammation syndrome with edema, cutaneous disorders with necrosis and haemorrhagic manifestations. Indeed, venoms of viperids are rich in enzymes of varying specificities. Some destroy the tissues around the bite and cause severe necrosis. Other enzymes act on the various stages of haemostasis, in particular coagulation leading to haemostasis disorders [1,2]. Viper syndrome can progress to local (gangrenous, compartment syndrome) and systemic (CIVD, renal failure, pulmonary edema) complications. The syndrome of the lodges is characterized by a muscular ischemia consecutive to an abnormal increase of pressure in a box osteo-aponeurotic little or no extensible. The occurrence of this syndrome in the wake of a viperin envenomation remains a dreaded complication emanating from the necrotizing effect of venom on the tissues. Its treatment is surgical, but many teams reserve the surgical intervention for failures of treatment with antivenom [3,4].
Patients and Methods
This is a retrospective and descriptive study of the case of viperin syndrome syndrome treated in intensive care at the CHU Bouaké during the period from January 1, 2012 to March 31, 2016. The variables studied were the admission delay, age, sex, occupation, bite circumstances, clinical parameters, biological parameters, therapeutic modalities and evolution.
Results
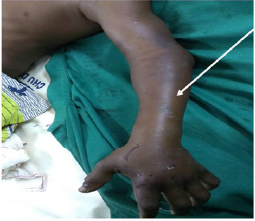
One hundred twenty-six cases of envenomation were reported during the study period with 37 viperine envenomations and 06 cases of compartment syndrome. The average age was 19 years old with extremes of 8 years and 36 years. There were 04 men and 02 women. Farmers were the most concerned (05 cases) and a shepherd. The average admission time was 11.50 hours with extremes of 02 and 48 hours. The symptomatology was dominated by a painful tension of the muscular compartments with extensive loco-regional edema, a disappearance of peripheral pulses. The bite was located in the lower limbs (feet and / or ankles) at 04 patients and in the hands at 02 patients. We noted hemorrhagic syndrome in 04 patients and respiratory distress in one patient. Haemostasis disorders were found in 04 patients with mean TP <50%; thrombocytopenia with an average platelet count of 104.56 elements per m3 (Figure 1-3).
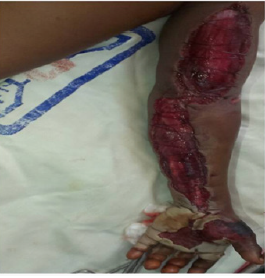
Figure 2: Patient reviewed at J 36 post discharge fasciotomy with sequelae of retractile scarring, stiffness of the left elbow, limitation of prono-supination movements of the left wrist.
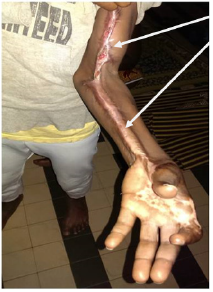
Figure 3: Patient reviewed at J 36 post discharge fasciotomy with sequelae of retractile scars, stiffness of the left elbow, limitation of wrist prono-supination movements.
The treatment received at home was scarification in 04 patients, use of tourniquet and application of decoction on the bitten limb in respectively 02 and 03 patients. A discharge aponeurotomy was initiated on average 01 to 02 days after admission, an antivenom serotherapy was performed with FAV Africa at an average of 02 doses within 24 to 48 hours. Adjuvant therapy included vascular filling in 03 patients in shock, erythrocyte concentrate transfusion in 04 patients with hemorrhagic syndrome, amoxicillin-clavulanic acid antibiotic therapy, and multimodal analgesia with (paracetamol, tramadol and/or morphine) have been prescribed in all patients. The average hospital stay was 13 days with extremes of 10 and 19 days. The evolution during the hospitalization was marked by a necrosis of the incised areas of the back of the hand in a patient with need of recovery in the operating room by the surgeons. The average length of stay in trauma was 13 days with extremes of 7 and 20 days.
Discussion
The venoms of snakes consist of an extraordinary cocktail containing: hemorrhages that cause an alteration of the vascular endothelium with edema and tissue necrosis. Proteases that play the role of platelet antiaggregant and fibrinolytic enzymes causing haemostasis disorders with haemorrhagic syndrome [2]. The severity of this condition is sometimes correlated with the rapid extension of edema and the formation of systemic manifestations, particularly hemorrhagic or local, with syndromes of lining syndrome [5]. The occurrence of a syndrome of lining following envenomation is due to the virulence of the venom, its concentration in a small volume of tissue or the use of tourniquet by some patients causing ischemia of the Member [5]. Also, the syndrome of the lodges is characterized by an increase of the pressure at the level of the muscular compartments with venous compression at the origin of a fall of the local flow. It then appears a pseudo-inflammatory aspect of the limb with painful swelling. This pressure can be measured also through para-clinical investigations in the face of any diagnostic doubt. According to some authors, the measurement of intra-compartmental pressures can help the diagnosis to be positive in the face of any uncertainty. At rest in supine position, the normal pressures of a muscular lodge are between 0 and 8mmHg. Ischemia begins as soon as the intramuscular pressure is 10 to 30 mmHg above the Whiteside diastolic blood pressure [1,4,8].
In our series the diagnosis was clinical before the painful tension of the muscular boxes with disappearance of the peripheral pulses. Once constituted, it is an absolute surgical emergency whose management consists of a discharge fasciotomy according to several authors that must be early. This was the case in our observation. This intervention is not immune to certain complications, including hemorrhagic risk in this context of bleeding disorder and infectious complications. This leads some practitioners to remain armed with expectancy and monitor the clinical course of the limb [4]. The etiological treatment remains antivenom immunotherapy. According to some authors, the antivenom can neutralize the local and systemic effects of snake venom. Its early administration at adequate doses before the 36th hour can prevent the appearance of a syndrome of lodges and even minimize the evolution if it is already constituted [3-10]. The ideal is to administer 02 ampoules of 10ml to renew in 02h then in 04h. All our patients benefited from the antivenom « FAV Africa» with a posology of 2 dosages in the 24 hours following the bite. The adequate dosages according to the referential norms have not been respected because of the high price of the antivenom serum and sometimes because of its availability in our sanitary structure.
Conclusion
The syndrome of post-envenomation viperine lodges is observed more and more in our context. The diagnosis is clinical, possibly confirmed by the measurement of intramuscular pressures. Effective management requires surgical treatment and antivenom.
References
- Bellefleur JP (2005) The Dantec P Hospital management of snake bites in Africa. Bull soc pathol exot 98 (4): 273-276.
- Mion G, Olive F, Hernandez E, Martin NY, Viellefosse A-S, et al. (2002) Action of venoms on blood coagulation: diagnosis of hemorrhagic syndromes. Bull socpathol exot 95(3): 132-138.
- Koraichi El A, Tsala G, Ahid SJ, Tadili J, Kharraz H, et al. (2011) The syndrome of the lodges in the wake of the viperine enemasions of the child. Resuscitation 20: 463-466.
- Dantec P, Hervé Y, Niang B, Chippaux J P, Bellefleur P, et al. (2004) Bite Bitis arietans in Senegal, interest in the measurement of intracompartmental pressure. Med health to 64 (2): 187-191.
- Ait Essi F, Benhima M A, Abkari I, Najeb Y, et al. (2013) Fingers amputation following snakebite: a report of three cases. Lamel surgery 32: 92-95.
- Chani M, Kassimi H, Abouzahir A, Nazi M, Mion G (2008) About three observations of severe viperine enemias in Morocco. Ann Franç Anesth Réanim 27: 330-334
- Mion G, Larréché S (2014) What an anti-venom for the envenomations by the vipers of the kind cerastes. Med Health Trop 24: 105-106.
- Berdai M A, Labib S, Harandou M (2013) Pediatric Ophidian Envenimation at the University Hospital Center of Fes (Morocco). Med Health Too 23: 427-432.
- Aissaoui Y, Kichna H, Boughalem M, Drissi Kamili N (2013) The paraspecificity of the anti-vinoins: example of a serious envenomation by the viper with horns of the Sahara (cerastes) treated by a nonspecific polyvalent anti-venom. Med Health Too 23: 100-103.
- Caens-Daudin C, Guerbet M (2001) Update on the treatment of viper bites. Pharmaceutical Lyon 52: 182-188.



 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.